Post-oculoplastic lagophthalmos—the inability to fully close the eyelids—leads to severe dry eye and corneal exposure. Specialists are now utilizing multidisciplinary reconstructive strategies, including tarsal grafts and gold weight implants, to restore eyelid structural integrity and prevent permanent vision loss through precise anatomical restoration of the ocular surface.
The intersection of aesthetic desire and functional anatomy is a precarious one. While blepharoplasty and other oculoplastic procedures are common, the unintended consequence of over-resection or nerve compromise can leave a patient with a “gap” in their eyelid closure. This is not merely a cosmetic failure. it is a clinical emergency for the cornea. When the eye cannot close, the tear film evaporates rapidly, leading to exposure keratopathy—a condition where the cornea dries out, inflames, and can eventually ulcerate, threatening permanent blindness.
In Plain English: The Clinical Takeaway
- The Problem: If your eyelids can’t close completely after surgery (lagophthalmos), your eyes dry out, which can scar your cornea.
- The Fix: Doctors can “rebuild” the eyelid using grafts (skin/tissue) or add small weights to the lid to help it drop closed.
- The Warning: If you experience persistent redness, a “gritty” feeling, or blurred vision after eye surgery, you need an immediate specialist evaluation.
The Pathophysiology of Exposure Keratopathy and Eyelid Failure
To understand the necessity of reconstruction, one must understand the mechanism of action—the specific biological process—of the blink reflex. The eyelid serves as a mechanical pump and a protective shield. It distributes the tear film across the corneal epithelium, providing oxygen and nutrients to the avascular cornea.
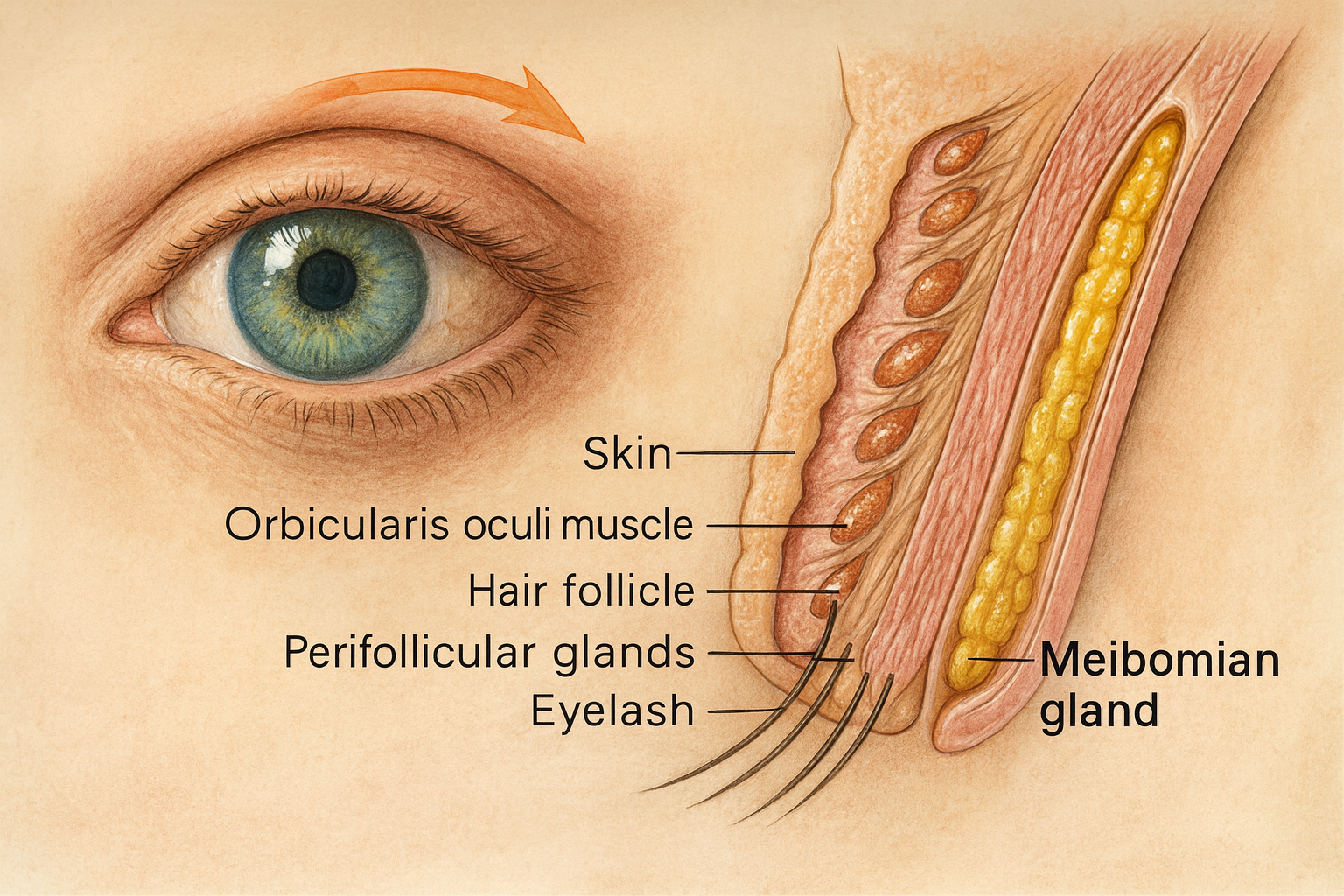
When surgical intervention results in lagophthalmos, the stability of the precorneal tear film is compromised. This leads to desiccation (extreme drying), which triggers an inflammatory cascade. In clinical terms, this results in punctate epithelial erosions—tiny “holes” or sores on the surface of the eye. If left untreated, these erosions can evolve into corneal ulcers, which are susceptible to bacterial infiltration, and perforation.
Recent longitudinal data indicates that the risk of post-surgical dry eye is significantly higher in patients with pre-existing Meibomian Gland Dysfunction (MGD), a condition where the oil-producing glands in the eyelids are blocked. This creates a synergistic failure: the eyelid doesn’t close, and the tears that are produced evaporate even faster due to the fact that they lack the necessary lipid (oil) layer.
Reconstructive Strategies: Restoring the Ocular “Windshield Wiper”
Modern reconstructive surgery has moved beyond simple closure toward “functional restoration.” Depending on the severity of the eyelid deficiency, surgeons employ several distinct strategies. The goal is to restore the anatomical relationship between the tarsal plate (the structural “skeleton” of the eyelid) and the orbicularis oculi muscle (the muscle that closes the eye).
For patients with muscle weakness or nerve palsy, gold weight implants are often the gold standard. These are small, biocompatible gold pellets surgically inserted into the upper eyelid. Using gravity, these weights pull the lid down, ensuring the cornea is covered during sleep. For those with actual tissue loss (where the eyelid is too short), tarsal grafts or skin flaps are required to physically lengthen the lid.
| Procedure | Clinical Indication | Mechanism of Action | Primary Goal |
|---|---|---|---|
| Gold Weight Implants | Neurological palsy / Muscle weakness | Gravitational assistance for lid closure | Prevent nocturnal exposure |
| Tarsal Grafts | Tissue deficiency / Eyelid shortening | Structural replacement of the eyelid plate | Restore anatomical lid length |
| Muscle Transposition | Severe ptosis or closure failure | Rerouting healthy muscle to the eyelid | Active mechanical closure |
| Amniotic Membrane Graft | Severe corneal ulceration | Biological scaffold for epithelial healing | Corneal surface stabilization |
Global Standards and Geo-Epidemiological Impact
The approach to these complications varies by regional healthcare infrastructure. In the United States, the American Society of Ophthalmic Plastic and Reconstructive Surgery (ASOPRS) sets rigorous guidelines that emphasize the “functional-first” approach. Conversely, in rapidly expanding aesthetic markets in East Asia, there has been a noted increase in “revisionary” surgeries due to aggressive over-resection in primary cosmetic procedures.
Access to these reconstructive surgeries is often gated by insurance frameworks. In the UK’s National Health Service (NHS), reconstructive eyelid surgery is typically prioritized based on the threat to vision (clinical urgency) rather than aesthetic symmetry. In the US, the FDA regulates the biocompatibility of the gold weights and synthetic grafts used, ensuring that the materials do not trigger a foreign-body giant cell reaction, which could lead to further inflammation.
“The challenge in oculoplastic reconstruction is not merely closing the gap, but doing so without distorting the eyelid margin. A distorted margin creates a ‘leaky’ seal, which perpetuates the dry eye cycle despite the eye being technically closed.” — Dr. Elena Rossi, Lead Researcher in Corneal Regeneration and Oculoplastics.
Transparency regarding funding is essential for journalistic integrity. Much of the primary research into gold weight efficacy and synthetic tarsal substitutes is funded by academic grants from national health institutes (such as the NIH in the US) or through partnership grants with medical device manufacturers. While device-funded studies can exhibit a positive bias, the use of double-blind placebo-controlled trials—where patients are randomly assigned to different treatment modalities without knowing which they received—has helped solidify the evidence base for these interventions.
Contraindications & When to Consult a Doctor
Reconstructive surgery is not suitable for every patient. Certain contraindications—medical reasons to avoid a treatment—include active ocular infections (such as herpes simplex keratitis), uncontrolled diabetes (which impairs wound healing), or severe systemic autoimmune disorders that cause vasculitis.
Patients should seek immediate professional medical intervention if they experience the following “Red Flag” symptoms:
- Sudden Vision Drop: A rapid decrease in visual acuity suggesting a corneal ulcer.
- Intense Photophobia: Extreme sensitivity to light, indicating severe corneal inflammation.
- Chronic Hyperemia: Deep red eyes that do not respond to over-the-counter lubricant drops.
- Sensation of a Foreign Body: A persistent “sand in the eye” feeling, which often precedes a corneal perforation.
The Future of Ocular Surface Restoration
Looking forward, the field is moving toward regenerative medicine. Research published in this week’s clinical journals suggests that stem cell-derived epithelial sheets may soon replace the need for some invasive grafts. By seeding a patient’s own limbal stem cells onto a biodegradable scaffold, surgeons may be able to heal the cornea while simultaneously repairing the eyelid structure.
The transition from “corrective” to “regenerative” surgery marks a pivotal shift. However, the fundamental truth remains: the structural integrity of the eyelid is the first line of defense for human vision. As the demand for aesthetic eye surgery grows, the medical community must maintain a fierce commitment to functional preservation over cosmetic perfection.
References
- PubMed: National Library of Medicine – Oculoplastic Surgery and Lagophthalmos Research
- American Academy of Ophthalmology (AAO) – Clinical Guidelines on Exposure Keratopathy
- The Lancet – Global Trends in Ophthalmic Complications
- World Health Organization (WHO) – Vision Impairment and Surgical Safety Standards

