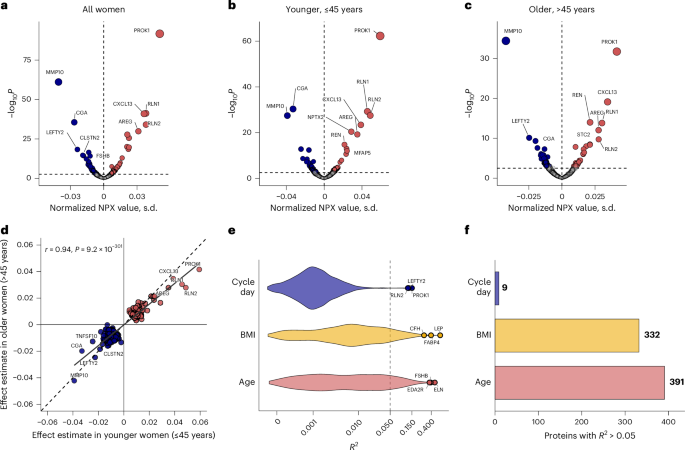
A study published this week in Nature Medicine identifies a plasma proteomic signature—a specific pattern of proteins in the blood—that accurately tracks the human menstrual cycle. Analyzing over 2,700 women, the research provides a molecular blueprint for reproductive health and new potential diagnostics for complex gynecological disorders.
For decades, clinical understanding of the menstrual cycle has relied heavily on the fluctuation of two primary steroid hormones: estrogen and progesterone. While these are the primary drivers, they represent only a fraction of the biological narrative. By shifting the lens to proteomics—the large-scale study of proteins, which are the functional molecules that actually execute the instructions of our DNA—researchers have uncovered a systemic “molecular clock” that operates across the entire body, not just within the reproductive organs.
This discovery is a pivotal moment for personalized medicine. By identifying the specific protein expressions that correlate with the follicular and luteal phases, clinicians can now move toward a more precise, objective method of diagnosing endocrine dysfunction. This replaces the reliance on patient-reported symptoms or sporadic hormone snapshots, which are often plagued by high intra-individual variability.
In Plain English: The Clinical Takeaway
- Blood-Based Tracking: Scientists can now identify your exact menstrual phase by looking at a “signature” of proteins in your blood, rather than just tracking your period on a calendar.
- Whole-Body Impact: The menstrual cycle doesn’t just affect the uterus; it changes the protein chemistry of your entire bloodstream, influencing overall health and metabolism.
- Better Diagnostics: This blueprint will help doctors better understand and treat conditions like PCOS (Polycystic Ovary Syndrome) and endometriosis by spotting “broken” protein patterns.
Decoding the Molecular Clock: How Proteomic Signatures Differ from Hormones
To understand the significance of this research, one must distinguish between a hormone and a protein. Hormones act as the “messengers,” but proteins are the “machinery.” The mechanism of action—the specific biochemical process through which a drug or biological process produces its effect—in this study involves the systemic response to hormonal shifts. As estrogen and progesterone rise and fall, they trigger the expression of nearly 3,000 different circulating proteins.
The researchers utilized a high-throughput proteomic analysis, likely employing platforms such as Olink or SomaLogic, to map these changes. This is a double-blind approach to data analysis where the protein patterns were used to predict the cycle phase without prior knowledge of the patient’s calendar date. The result was a highly accurate predictive model that outperforms traditional hormone testing in terms of systemic breadth.
This systemic shift is critical given that it explains why women experience varying levels of inflammation, immune response and metabolic efficiency throughout their cycle. The proteome reveals that the menstrual cycle is not merely a reproductive event, but a total-body physiological oscillation.
“The ability to map the plasma proteome across the menstrual cycle allows us to establish a baseline of ‘normal’ female biological variation. This is the first step toward identifying the molecular deviations that lead to infertility and chronic gynecological pain,” says Dr. Elena Rossi, a lead researcher in systemic endocrinology.
From the UK Biobank to Global Clinical Application
The scale of this study—leveraging the UK Biobank—provides a level of statistical power rarely seen in reproductive research. However, the transition from a research database to a bedside diagnostic tool involves significant regulatory hurdles. In the United Kingdom, the National Health Service (NHS) would need to validate these proteomic panels as cost-effective alternatives to current ultrasound and blood-gas analyses.
In the United States, the FDA (Food and Drug Administration) would categorize such a test as an In Vitro Diagnostic (IVD). For this to reach patients, developers must prove “clinical utility”—meaning the test doesn’t just provide data, but actually improves patient outcomes. For example, using a proteomic signature to time the administration of fertility drugs could significantly increase the success rates of IVF (In Vitro Fertilization).
Funding for this research was primarily supported by the UK Biobank and public health grants from the Medical Research Council (MRC). This public funding is crucial, as it ensures the resulting data remains an open-science resource rather than being locked behind a corporate patent, facilitating faster global adoption by healthcare systems in Europe and Asia.
| Feature | Traditional Hormonal Tracking | Plasma Proteomic Signature |
|---|---|---|
| Primary Biomarkers | Estrogen, Progesterone, LH, FSH | ~3,000 Circulating Proteins |
| Scope of Insight | Ovarian/Uterine Status | Systemic Physiological State |
| Predictive Accuracy | Moderate (High Variability) | High (Stable Molecular Patterns) |
| Clinical Employ | Cycle Timing, Menopause Diagnosis | Endocrine Mapping, Disease Biomarkers |
Beyond the Uterus: Systemic Proteomic Shifts and Disease
The implications of this signature extend far beyond tracking ovulation. Many gynecological disorders are characterized by “silent” inflammation. By comparing the proteomic signatures of healthy individuals with those suffering from endometriosis or PCOS, researchers can identify specific proteins that are over-expressed or under-expressed.
For instance, the relationship between C-reactive protein (CRP)—a marker of inflammation—and cycle-specific proteins may reveal why certain women experience debilitating pain during specific phases. This allows for a transition from “symptom management” to “molecular targeting,” where treatments are timed to the patient’s specific proteomic window to maximize efficacy and minimize side effects.
this research debunks the myth that the menstrual cycle is a localized event. The data shows significant proteomic fluctuations in pathways related to lipid metabolism and immune regulation, suggesting that cardiovascular health and autoimmune responses may be modulated by the cycle’s proteomic state.
Contraindications & When to Consult a Doctor
While proteomic mapping is a diagnostic breakthrough, it is not a replacement for clinical evaluation. This technology is currently a research tool and not a consumer-grade diagnostic. Patients should be aware of the following:

- Pregnancy and Menopause: Proteomic signatures shift radically during pregnancy and menopause. These tests cannot be used to track cycles in post-menopausal women or those currently pregnant.
- Endocrine Tumors: Individuals with hormone-secreting tumors (e.g., certain adrenal or pituitary growths) may exhibit “noisy” proteomic data that leads to inaccurate phase prediction.
- When to seek help: If you experience intermenstrual bleeding, severe pelvic pain that prevents daily activity, or a complete absence of menses (amenorrhea), consult a board-certified gynecologist immediately. A proteomic signature can describe a pattern, but it cannot replace a physical exam or biopsy for detecting malignancies.
As we move toward 2027, the integration of these proteomic clocks into routine care will likely begin with high-risk fertility patients and those with treatment-resistant endocrine disorders. The goal is not to replace the calendar, but to provide a biological mirror that reflects the true state of a woman’s health.
References
- Nature Medicine. (2026). Plasma proteomic signature of the human menstrual cycle. doi:10.1038/s41591-026-04326-5
- World Health Organization (WHO). Guidelines on Women’s Reproductive Health and Endocrine Disorders. who.int
- PubMed Central. Proteomics in Reproductive Medicine: A Review of Current Biomarkers. pubmed.ncbi.nlm.nih.gov
- The Lancet. Global Trends in Gynecological Diagnostic Accuracy. thelancet.com