Vulvar cancer is a rare malignancy of the external female genitalia, primarily manifesting as squamous cell carcinoma. While incidence rates remain low, early detection via biopsy and precise staging are critical, as the prognosis depends heavily on the extent of lymph node involvement and the specific histological subtype.
The intersection of a devastating medical diagnosis and acute psychosocial trauma—such as the betrayal and emotional instability highlighted in recent patient narratives—creates a complex clinical picture. When a patient faces a rare malignancy like vulvar cancer, the psychological burden can lead to “diagnostic overshadowing,” where emotional distress masks or delays the reporting of physical symptoms. Globally, the rarity of this cancer often leads to delays in diagnosis, making it imperative for both patients and primary care providers to recognize early warning signs before the disease progresses to advanced stages.
In Plain English: The Clinical Takeaway
- It is rare but detectable: Vulvar cancer is uncommon, but persistent itching, lumps, or color changes in the genital area should always be evaluated by a specialist.
- HPV is a key driver: Many cases are linked to high-risk Human Papillomavirus (HPV), meaning vaccination and cervical screening can provide indirect protective insights.
- Early action saves lives: When caught in early stages, surgical removal of the tumor often leads to high cure rates.
The Molecular Drivers: HPV and the Role of Chronic Inflammation
To understand vulvar cancer, we must examine its mechanism of action—the specific biological process that leads to the disease. The majority of vulvar malignancies are Squamous Cell Carcinomas (SCC). These generally follow two distinct pathways. The first is the HPV-mediated pathway, where high-risk strains of the Human Papillomavirus integrate into the host DNA, producing oncoproteins E6 and E7 that deactivate tumor-suppressor proteins (p53 and pRb), allowing cells to divide uncontrollably.
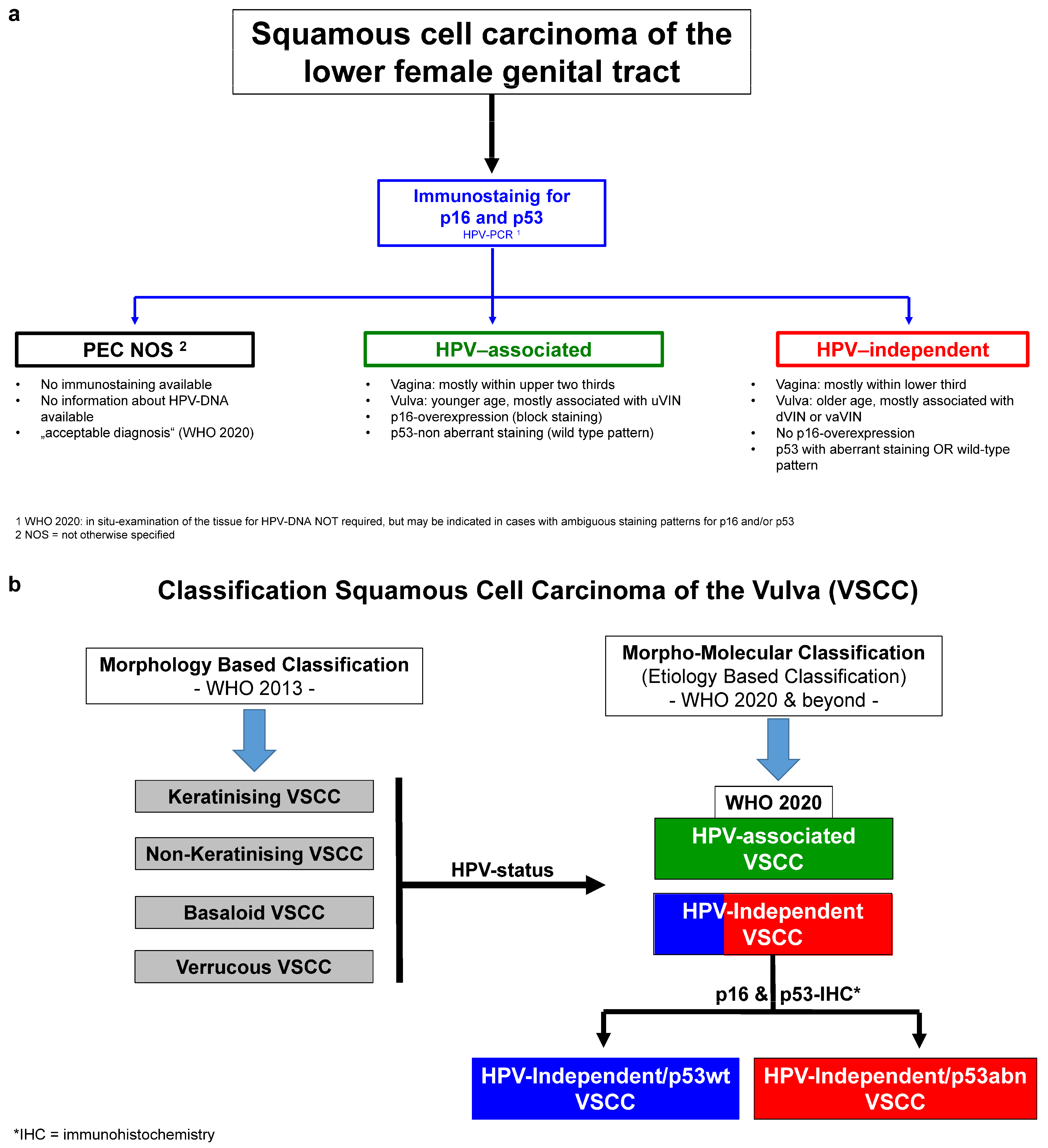
The second pathway is non-HPV related, often stemming from chronic inflammatory conditions such as lichen sclerosus. This is a chronic inflammatory skin condition that causes thinning of the skin and intense itching. Over decades, the constant cycle of inflammation and tissue repair can lead to cellular atypia—abnormal cell growth—which may eventually progress to a malignancy.
“The diagnostic challenge with vulvar neoplasia lies in its rarity. many general practitioners may see only one such case in their entire career, which is why patient advocacy and persistent reporting of symptoms are vital for survival,” states Dr. Elena Rossi, a lead oncologist specializing in gynecologic malignancies.
Navigating the Treatment Pipeline: From Radical Surgery to Immunotherapy
Treatment for vulvar cancer is highly individualized based on the stage of the disease. The gold standard for early-stage tumors is a wide local excision—removing the tumor along with a margin of healthy tissue to ensure no cancer cells remain. In more advanced cases, a radical vulvectomy may be required, which involves the removal of a larger portion of the vulva.
A critical component of staging is the inguinal lymphadenectomy, a surgical procedure to remove lymph nodes in the groin to check for metastasis (the spread of cancer to other parts of the body). For patients with recurrent or metastatic disease, the medical community has shifted toward immunotherapy. Drugs such as Pembrolizumab, which act as checkpoint inhibitors, help the patient’s own immune system recognize and attack cancer cells by blocking the PD-1 pathway.
| Histological Type | Primary Driver | Common Symptoms | Primary Treatment |
|---|---|---|---|
| Squamous Cell Carcinoma | HPV or Lichen Sclerosus | Lumps, ulcers, itching | Surgery + Lymph node check |
| Vulvar Melanoma | UV/Genetic Mutation | Dark pigmentation, moles | Wide excision + Immunotherapy |
| Basal Cell Carcinoma | Chronic irritation | Pearly nodules, gradual growth | Local surgical excision |
The Global Access Gap: EMA, FDA, and Regional Healthcare Disparities
Access to advanced treatments for rare cancers varies significantly by geography. In the United States, the FDA often grants “Orphan Drug Designation” to therapies for rare cancers, accelerating the approval process. Similarly, the European Medicines Agency (EMA) provides pathways for priority medicines (PRIME) to ensure European patients gain faster access to life-saving innovations.
However, a gap remains in the UK’s NHS and various European national health systems regarding standardized screening. Unlike cervical cancer, for which there is a robust population-wide screening program, there is no “vulvar screen.” Patients rely entirely on symptomatic presentation. This lack of systemic screening means that diagnosis often occurs only after the patient notices a physical change, which can be delayed if the patient is experiencing severe psychological distress or avoids pelvic exams due to trauma.
The funding for these advancements primarily comes from a mix of public grants (such as the National Cancer Institute in the US) and private pharmaceutical investment. Transparency in this funding is essential to ensure that clinical trial endpoints—the specific goals used to measure a drug’s success—are based on overall survival rather than just “progression-free survival,” which can sometimes be a misleading metric.
Contraindications & When to Consult a Doctor
While the treatments mentioned are effective, they are not suitable for everyone. Radiation therapy is generally contraindicated in patients who have had previous pelvic radiation due to the risk of severe tissue necrosis (cell death). Certain immunotherapies may be dangerous for patients with severe autoimmune diseases, as they can trigger an overactive immune response against healthy organs.

Consult a gynecologic oncologist immediately if you experience:
- A persistent lump or thickening of the skin in the vulvar area.
- Changes in skin color (white, red, or dark patches) that do not resolve.
- Chronic itching or burning that does not respond to standard antifungal or steroid creams.
- An open sore or ulcer that refuses to heal over a period of two to four weeks.
The Trajectory of Rare Cancer Care
The future of vulvar cancer management lies in precision medicine. By sequencing the tumor’s genome, clinicians can identify specific mutations and tailor therapies to the individual, reducing the need for disfiguring radical surgeries. As we integrate better psychosocial support into oncology, we acknowledge that a patient’s mental health is not secondary to their physical health; it is a fundamental component of the recovery process. The goal is a shift from “survival at any cost” to “survival with quality of life.”

