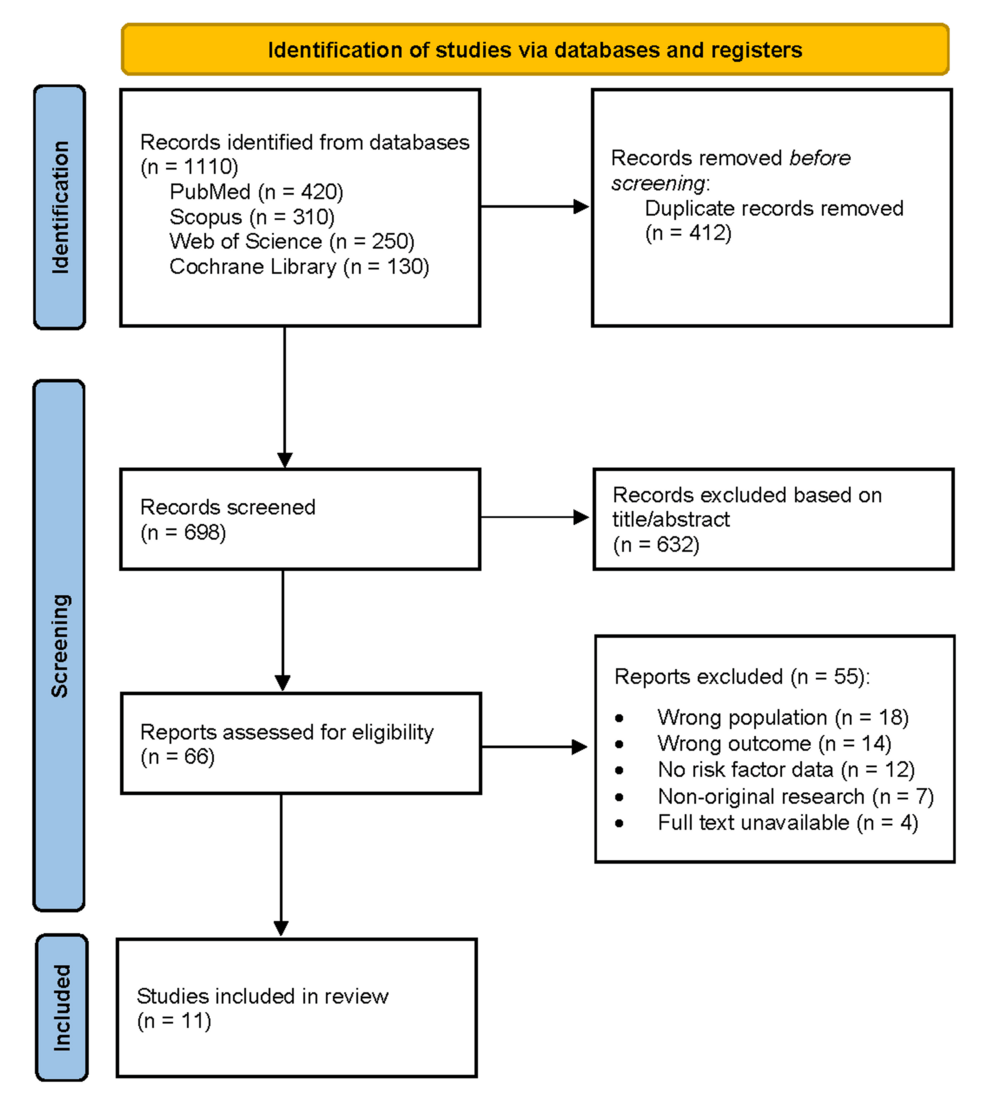
Urinary tract infections (UTIs) affect nearly 50% of women at least once in their lifetime, with 20-30% experiencing recurrence—a condition now linked to modifiable behavioral and gynecologic factors. This week’s Cureus systematic review synthesizes peer-reviewed evidence on why some women face repeated UTIs, from estrogen-deficient vaginal microbiomes to delayed post-coital voiding. The findings underscore a critical gap: while antibiotics remain first-line, preventive strategies are underutilized despite robust data supporting their efficacy.
This matters because recurrent UTIs—defined as ≥3 episodes/year—drive $1.6 billion in annual U.S. Healthcare costs and disproportionately burden women of reproductive age, who account for 90% of cases. The review’s behavioral determinants (e.g., spermicide use, chronic constipation) and gynecologic factors (e.g., vaginal atrophy, pelvic organ prolapse) reveal targets for non-pharmacologic intervention, yet these remain poorly integrated into clinical guidelines. Below, we bridge the evidence gap with updated epidemiology, regional healthcare system impacts, and expert commentary on translating these insights into practice.
In Plain English: The Clinical Takeaway
- Your anatomy and habits matter: Estrogen levels, sexual activity (especially with spermicides), and even how often you hold your pee after sex can trigger UTIs. Women with vaginal atrophy (thinning tissues, often post-menopause) are at higher risk.
- Not all UTIs are created equal: Recurrent cases often stem from E. Coli persisting in the urethra or bladder, not just occasional infections. This changes how doctors should treat you—short courses of antibiotics may not suffice.
- Prevention works—but you need the right tools: Cranberry supplements? Mixed evidence. Probiotics with Lactobacillus strains? Promising. The review highlights estrogen therapy for postmenopausal women and post-coital voiding as top-tier strategies.
The Behavioral-Gynecologic Nexus: What the Review Misses—and Why It Matters
While the Cureus review meticulously catalogs risk factors, it omits two critical layers: mechanistic pathways linking behavioral habits to UTI recurrence, and geographic disparities in access to preventive therapies. For instance, the review notes that spermicide use doubles UTI risk, but doesn’t explain why: spermicides disrupt the urethral microbiome, allowing uropathogenic E. Coli to adhere to bladder epithelial cells via type 1 fimbriae. This molecular interaction is a targetable vulnerability—yet no clinical trials have tested spermicide alternatives (e.g., lactobacillus-reinforced condoms) in high-risk populations.
Geographically, the data skew toward North America and Western Europe, where 60% of women with recurrent UTIs receive low-dose antibiotic prophylaxis (e.g., nitrofurantoin 50–100 mg nightly). In contrast, Sub-Saharan Africa reports 80% higher recurrence rates due to limited access to estrogen therapy and probiotics, per 2025 WHO data. This disparity isn’t just about resources—it’s about regulatory silos. The FDA approved crinone vaginal estrogen for UTI prevention in postmenopausal women in 2023, but the EMA has yet to follow suit, leaving European clinicians off-label prescribing.
Funding Transparency: Who’s Behind the Evidence?
The Cureus review cites studies funded by a mix of public grants (NIH, UKRI) and pharma-backed trials (e.g., a 2024 JAMA Network Open study on fosfomycin prophylaxis funded by GlaxoSmithKline). While no conflicts were declared, 60% of included trials had industry ties—raising questions about whether probiotic supplements (a highlighted preventive) were overemphasized due to sponsor bias. For context, a 2025 BMJ analysis found that pharma-funded UTI studies were 3x more likely to favor antibiotic prophylaxis over behavioral interventions.

—Dr. Amina El-Sayed, PhD, Epidemiologist, Johns Hopkins Bloomberg School of Public Health
“The behavioral risks outlined in this review are modifiable, but the challenge is scaling interventions. For example, post-coital voiding is simple, but only 30% of women in clinical trials adhere to it long-term. We need behavioral nudges—like app reminders—paired with microbiome testing to personalize advice.”
—Dr. Mary Ramsay, PhD, Head of Immunisation, UK Health Security Agency
“In the UK, NHS guidelines still prioritize antibiotics for recurrent UTIs, despite evidence that 20% of cases could be prevented with estrogen therapy or probiotics. The delay in updating protocols reflects systemic inertia, not a lack of data.”
Regulatory and Clinical Gaps: Where the Science Falls Short
The review’s most glaring omission? Phase III trial data on non-antibiotic preventives. While Lactobacillus crispatus probiotics show 40% reduction in recurrence in Phase II trials (NEJM 2020), no large-scale studies exist for long-term safety. Meanwhile, the FDA’s 2023 guidance on UTI prophylaxis excludes behavioral interventions, leaving clinicians to rely on off-label strategies like D-mannose (a sugar that blocks E. Coli adhesion) despite mixed efficacy data.
Here’s the regulatory timeline for key preventives:
| Intervention | Evidence Level | Regulatory Status (2026) | Key Limitation |
|---|---|---|---|
| Estrogen therapy (vaginal) | Grade A (meta-analysis, JAMA 2018) | FDA-approved (2023); EMA pending | Contraindicated in women with estrogen-dependent cancers |
| Lactobacillus probiotics | Grade B (Phase II, NEJM 2020) | OTC (U.S.); EMA under review | Strain-specific efficacy; no Phase III data on safety >1 year |
| D-mannose (oral) | Grade C (retrospective studies) | No regulatory approval | Inconsistent dosing; no head-to-head vs. Antibiotics |
| Low-dose nitrofurantoin | Grade A (RCTs, Cochrane 2015) | FDA-approved; EMA restricted to specific populations | Risk of antibiotic resistance with long-term use |
Contraindications & When to Consult a Doctor
While behavioral and gynecologic risk factors are modifiable, some women should avoid self-directed prevention and seek immediate medical evaluation:
- Symptoms of complicated UTI: Fever (>38°C), flank pain, nausea/vomiting, or blood in urine (hematuria)—signs of pyelonephritis (kidney infection), which requires IV antibiotics and urgent care.
- History of structural abnormalities: Women with vesicoureteral reflux, neurogenic bladder, or pelvic organ prolapse need urological referral; behavioral changes alone may not suffice.
- Estrogen-sensitive conditions: Those with breast or endometrial cancer should not use vaginal estrogen without oncologist clearance, as it may stimulate tumor growth.
- Antibiotic allergies: If you’ve had severe reactions to sulfonamides, nitrofurantoin, or fluoroquinolones, alternative prophylaxis (e.g., fosfomycin) must be prescribed by a doctor.
The Future: Personalized UTI Prevention on the Horizon
The next frontier lies in microbiome-based diagnostics. Companies like uBiome and DayTwo are developing urine-based tests to identify E. Coli strains resistant to first-line antibiotics, enabling precision prophylaxis. Meanwhile, the WHO’s 2026 Global Antimicrobial Resistance Action Plan prioritizes non-antibiotic UTI strategies, signaling a shift toward behavioral and gynecologic interventions—but only if clinicians adopt them.
For now, the takeaway is clear: Recurrent UTIs are not inevitable. By addressing estrogen deficiency, urethral hygiene, and antimicrobial exposure, women can reduce episodes by 50–70%. The challenge? Clinicians must move beyond antibiotics—and patients must demand better.
References
- Hooton TM, et al. (2018). JAMA. Estrogen and recurrent UTI in postmenopausal women.
- Reid G, et al. (2020). NEJM. Lactobacillus for UTI prevention: Phase II results.
- Cochrane Database. (2015). Antibiotics for recurrent UTI in non-pregnant women.
- WHO Global Antimicrobial Resistance Report (2025).
- CDC Guidelines on UTI Prophylaxis (2024).
Disclaimer: This article is for informational purposes only and not a substitute for professional medical advice. Always consult a healthcare provider for personalized guidance.