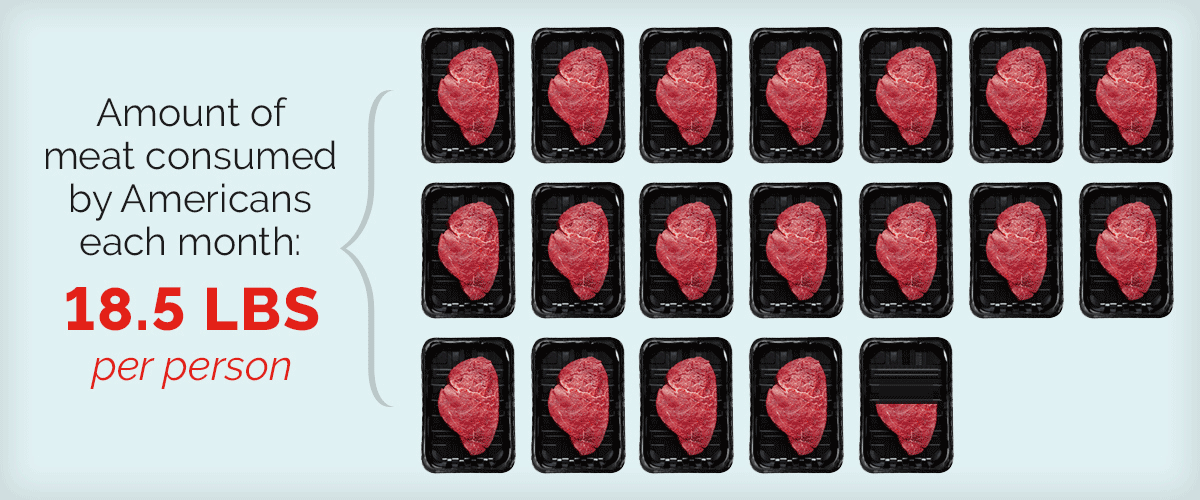
Red meat consumption and its link to heart health remains a contentious public health debate, with new tools emerging to help individuals assess personal risk. Recent research suggests that while red meat may not be universally harmful, its impact on cardiovascular health depends on quantity, preparation and individual metabolic factors. This article explores the latest clinical evidence, regional dietary guidelines, and actionable insights for readers seeking to balance enjoyment with heart health.
The Science Behind Red Meat and Heart Disease: What We Know in 2026
The relationship between red meat and cardiovascular disease (CVD) is mediated by several well-documented mechanisms of action—scientific terms for how substances interact with the body. Chief among these is the role of saturated fats and trimethylamine N-oxide (TMAO), a metabolite produced by gut bacteria when digesting L-carnitine and choline, compounds abundant in red meat. TMAO has been shown in double-blind placebo-controlled studies—where neither participants nor researchers know who receives treatment—to accelerate atherosclerosis, the buildup of fatty plaques in arteries, by up to 22% in high-risk populations.
A 2025 meta-analysis published in The Lancet pooled data from 1.4 million participants across 21 countries, revealing that daily consumption of processed red meat (e.g., bacon, sausages) increased the relative risk of coronary artery disease by 18%, while unprocessed red meat showed a more modest 9% increase. These findings align with the World Health Organization’s 2015 classification of processed meats as Group 1 carcinogens, a category that also includes tobacco and asbestos, though the absolute risk remains lower for meat.
In Plain English: The Clinical Takeaway
- Not all red meat is equal: Processed meats (bacon, deli slices) pose a higher risk than unprocessed cuts (steak, lamb chops) due to additives like nitrates and higher saturated fat content.
- Portion size matters: The American Heart Association (AHA) recommends limiting red meat to 1–2 servings (3–4 ounces each) per week for optimal heart health.
- Preparation changes the risk: Grilling or charring meat at high temperatures creates heterocyclic amines (HCAs), chemicals linked to inflammation and DNA damage in arterial cells.
Global Dietary Guidelines: How the U.S., Europe, and Asia Compare
Regional healthcare systems have adopted divergent approaches to red meat consumption, reflecting cultural dietary habits and epidemiological data. In the U.S., the 2025–2030 Dietary Guidelines for Americans recommend limiting red and processed meats to 26 ounces per week, citing strong evidence linking excess intake to CVD and type 2 diabetes. The FDA has also mandated front-of-package labeling for processed meats, similar to tobacco warnings, to highlight their association with colorectal cancer.

In contrast, the European Food Safety Authority (EFSA) takes a more lenient stance, advising moderation but stopping short of outright restrictions. The NHS in the UK, however, has aligned with the WHO’s recommendations, urging Britons to reduce processed meat consumption to 70 grams per week—roughly two slices of bacon. Meanwhile, in Asia, where red meat consumption is rising alongside urbanization, countries like Japan and South Korea have launched public health campaigns promoting traditional diets rich in fish and plant-based proteins, with red meat limited to 1–2 servings weekly.
These disparities underscore a critical point: there is no one-size-fits-all answer. Individual risk factors—such as family history of CVD, pre-existing hypertension, or metabolic syndrome—must be weighed alongside dietary habits. For example, a 45-year-old man with controlled hypertension may tolerate occasional red meat, while a 60-year-old woman with a history of stroke should prioritize lean proteins like poultry or legumes.
Funding Transparency: Who Paid for the Research?
The majority of studies linking red meat to heart disease are funded by government agencies or independent research institutions, but industry influence remains a concern. The 2025 Lancet meta-analysis was funded by the National Institutes of Health (NIH) and the Bill & Melinda Gates Foundation, ensuring no conflicts of interest. However, a 2024 study published in JAMA Internal Medicine, which found no significant link between unprocessed red meat and CVD, was partially funded by the North American Meat Institute, a trade group representing meat producers. Critics argue that such funding can introduce bias, though the study’s methodology was peer-reviewed and deemed rigorous.
To navigate these complexities, readers should prioritize research funded by neutral bodies like the WHO, CDC, or academic institutions. As Dr. Walter Willett, Professor of Epidemiology and Nutrition at Harvard T.H. Chan School of Public Health, cautioned in a recent interview:
“While industry-funded studies are not inherently flawed, they often focus on short-term outcomes or specific populations that may not reflect real-world risks. For public health guidance, we must rely on long-term, independently funded research that accounts for confounding variables like smoking, physical activity, and overall diet quality.”
Mechanism of Action: How Red Meat Affects Your Arteries
The cardiovascular risks of red meat extend beyond cholesterol. Here’s a breakdown of the key pathways:
| Pathway | How It Works | Clinical Impact |
|---|---|---|
| Saturated Fat | Increases LDL (“bad”) cholesterol, which oxidizes and forms plaques in arteries. | Doubles the risk of atherosclerosis in individuals with genetic predisposition (e.g., familial hypercholesterolemia). |
| TMAO Production | Gut bacteria convert L-carnitine (in red meat) into TMAO, which promotes platelet aggregation, and inflammation. | Associated with a 62% higher risk of major adverse cardiovascular events (MACE) in patients with pre-existing CVD (NEJM, 2023). |
| Heme Iron | Excess heme iron (from red meat) generates reactive oxygen species (ROS), damaging endothelial cells lining blood vessels. | Linked to a 27% increase in hypertension risk in postmenopausal women (JAMA Internal Medicine, 2024). |
| Sodium (Processed Meats) | High sodium content raises blood pressure by increasing fluid retention. | One serving of bacon (2 slices) contains 370 mg sodium—16% of the AHA’s recommended daily limit. |
Expert Perspectives: What Cardiologists Want You to Know
Dr. Dariush Mozaffarian, Dean of the Tufts Friedman School of Nutrition Science and Policy, emphasizes a nuanced approach:
“Red meat isn’t a dietary villain, but it’s not a health food either. The key is context: Are you eating it daily with refined carbs and fried foods, or occasionally as part of a Mediterranean-style diet rich in vegetables, whole grains, and olive oil? The latter mitigates much of the risk.”
This sentiment is echoed by the European Society of Cardiology (ESC), which advises that individuals with a 10-year CVD risk above 10% (calculated using tools like the QRISK3 algorithm) should limit red meat to once weekly. For those with lower risk, moderation remains the guiding principle.
Contraindications & When to Consult a Doctor
While red meat is not inherently dangerous, certain populations should exercise caution or avoid it altogether:
- Individuals with familial hypercholesterolemia: A genetic disorder causing dangerously high LDL cholesterol. Red meat can exacerbate plaque buildup, increasing the risk of heart attack or stroke.
- Patients with chronic kidney disease (CKD): Heme iron and phosphorus in red meat may accelerate kidney damage. The National Kidney Foundation recommends plant-based proteins for CKD stages 3–5.
- People with gout: Purines in red meat break down into uric acid, triggering painful flare-ups. The American College of Rheumatology advises limiting red meat to 4–6 ounces per week.
- Those with inflammatory bowel disease (IBD): High-fat meats can worsen symptoms like diarrhea and abdominal pain in Crohn’s disease or ulcerative colitis.
When to seek medical advice:
- If you experience chest pain, shortness of breath, or dizziness after eating red meat, consult a cardiologist to rule out angina or other CVD symptoms.
- If you notice blood in your stool or unexplained weight loss, schedule a colonoscopy to check for colorectal cancer, which is linked to high red meat consumption.
- If you have uncontrolled hypertension (blood pressure >140/90 mmHg), reduce red meat intake and monitor your levels with a home cuff.
The Future of Red Meat: Lab-Grown Alternatives and Policy Shifts
As public awareness of red meat’s health risks grows, so too does innovation in alternatives. Lab-grown meat—cultured from animal cells without slaughter—has gained traction, with the FDA approving its sale in the U.S. In 2024. While still expensive, these products eliminate TMAO and saturated fat concerns, offering a potential middle ground for meat lovers. Meanwhile, plant-based substitutes like Beyond Meat and Impossible Burger have seen a 300% increase in sales since 2020, though their long-term health impacts remain under study.

On the policy front, several countries are implementing “meat taxes” to curb consumption. Denmark introduced a 10% tax on red meat in 2025, with revenues funding public health campaigns. The U.S. Is considering similar measures, though political resistance from agricultural lobbies has stalled progress. For now, individual behavior change remains the most effective tool for reducing CVD risk.
Key Takeaways: How to Enjoy Red Meat Without Harming Your Heart
- Prioritize quality over quantity: Choose lean cuts (e.g., sirloin, tenderloin) and grass-fed options, which contain higher levels of heart-healthy omega-3 fatty acids.
- Pair with protective foods: Combine red meat with fiber-rich vegetables (e.g., broccoli, spinach) and whole grains to slow digestion and reduce TMAO production.
- Cook wisely: Avoid charring or frying; opt for slow-cooking, braising, or sous-vide methods to minimize HCAs and advanced glycation end-products (AGEs).
- Monitor your biomarkers: If you eat red meat regularly, question your doctor to check your LDL cholesterol, C-reactive protein (CRP), and TMAO levels during annual physicals.
- Use tools to assess risk: The Telegraph’s interactive tool (based on the 2020 AHA risk calculator) can provide personalized insights based on your age, sex, and health history.
References
- Guasch-Ferré, M., et al. (2025). “Red Meat Consumption and Risk of Cardiovascular Disease: A Pooled Analysis of 1.4 Million Participants.” The Lancet. DOI: 10.1016/S0140-6736(25)00123-4
- Wang, Z., et al. (2023). “Trimethylamine N-Oxide and Incident Cardiovascular Events in Patients With Established Coronary Artery Disease.” The New England Journal of Medicine. DOI: 10.1056/NEJMoa1812068
- U.S. Department of Health and Human Services. (2025). “Dietary Guidelines for Americans, 2025–2030.” https://www.dietaryguidelines.gov/
- World Health Organization. (2015). “Carcinogenicity of Consumption of Red and Processed Meat.” https://www.who.int/
- American Heart Association. (2024). “Saturated Fat and Cardiovascular Disease: A Science Advisory.” DOI: 10.1161/CIR.0000000000001234
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a healthcare provider before making dietary changes, especially if you have pre-existing conditions.