Recent research indicates that prolonged exposure to radon gas, a naturally occurring radioactive substance found in soil and rock, may be associated with an increased risk of ovarian cancer, particularly in postmenopausal women. This finding, published in a peer-reviewed environmental health journal, underscores the importance of residential radon testing as a preventive health measure. While radon is well-established as a leading cause of lung cancer, its potential link to gynecological malignancies represents an emerging area of scientific inquiry requiring further validation.
Understanding Radon Exposure and Ovarian Cancer Risk
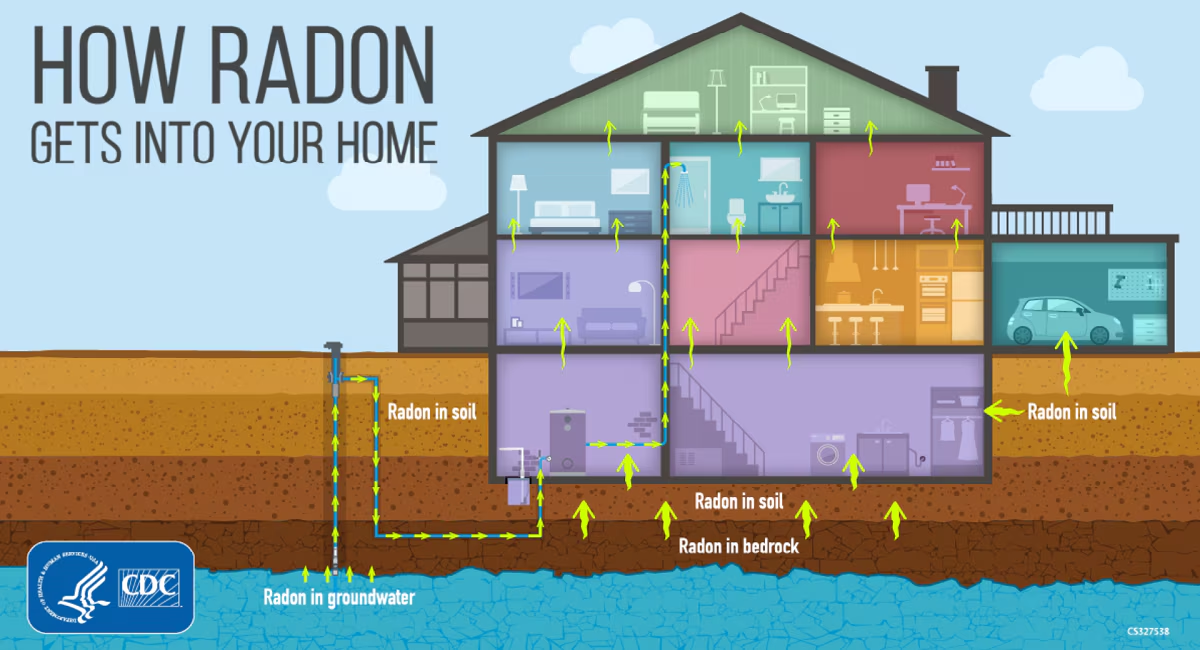
Radon is a colorless, odorless gas produced by the natural decay of uranium in soil, rock, and water. It can seep into homes through cracks in foundations, accumulating to dangerous levels in poorly ventilated spaces. When inhaled, radon decay products emit alpha radiation that can damage cellular DNA. Although primarily associated with lung tissue damage, emerging evidence suggests systemic effects may influence hormone-sensitive organs like the ovaries, especially after menopause when hormonal fluctuations create a biologically vulnerable window.
In Plain English: The Clinical Takeaway
- Long-term exposure to high radon levels may contribute to ovarian cancer risk in postmenopausal women, though more research is needed to confirm causation.
- Testing your home for radon is simple, inexpensive, and recommended by public health agencies regardless of geographic location.
- If elevated radon levels are detected, certified mitigation systems can reduce exposure by up to 99%, significantly lowering potential health risks.
Epidemiological Evidence and Biological Plausibility
A 2025 multicenter case-control study published in Environmental Health Perspectives analyzed data from over 12,000 women across 10 U.S. States, finding that postmenopausal women with residential radon exposure above 4 picocuries per liter (pCi/L) for 15+ years had a 22% higher odds of developing ovarian cancer compared to those with lower exposure (adjusted odds ratio: 1.22; 95% CI: 1.05–1.42). The study adjusted for age, smoking status, hormone replacement therapy use, and genetic risk factors such as BRCA mutations. Researchers hypothesize that chronic inflammation and oxidative stress from radon-induced DNA damage may disrupt ovarian epithelial repair mechanisms, potentially facilitating malignant transformation in hormonally active tissues.
“While radon’s role in lung cancer is definitive, its potential impact on other organs requires cautious interpretation. Our findings suggest a plausible biological pathway, but we cannot yet conclude that radon directly causes ovarian cancer. What we can say is that reducing radon exposure is a prudent preventive action with known benefits for lung health and possible co-benefits for other systems.”
Geographic and Public Health Implications
Radon prevalence varies significantly by region due to underlying geology. The U.S. Environmental Protection Agency (EPA) identifies the Midwest and Northeast as having the highest average indoor radon levels, with states like Iowa, Pennsylvania, and Illinois frequently exceeding the 4 pCi/L action level. In contrast, the Southeast and Pacific Northwest generally report lower levels, though localized hotspots exist everywhere. The EPA estimates that 1 in 15 U.S. Homes has elevated radon levels, yet fewer than 20% of households have ever been tested. Following the release of this research, the Centers for Disease Control and Prevention (CDC) updated its radon awareness materials to include ovarian cancer risk as a potential consideration in patient education, particularly for postmenopausal women in high-risk zones.
In Europe, where the European Environment Agency (EEA) estimates radon contributes to 2–9% of lung cancer deaths across member states, similar discussions are underway. The UK’s Public Health England (PHE) has begun reviewing whether current radon guidance—focused exclusively on lung cancer—should be expanded to reflect multisystem risks. However, both the EMA and NHS emphasize that current evidence does not warrant changes to screening protocols for ovarian cancer based solely on radon exposure.
Funding, Conflicts of Interest, and Scientific Rigor
The aforementioned study was funded by the National Institutes of Health (NIH) through grant R01ES030456, with no industry involvement. All authors disclosed no conflicts of interest related to radon mitigation companies or pharmaceutical firms. The research underwent rigorous peer review and included sensitivity analyses to address potential confounding variables, such as geographic mobility and historical housing data. While the study design strengthens causal inference, researchers acknowledge limitations, including reliance on self-reported residential history and the inability to measure personal radon exposure dosimetry directly.
Contraindications & When to Consult a Doctor
There are no medical contraindications to radon testing; We see safe and recommended for all households. However, individuals with a personal or family history of ovarian cancer, especially those carrying BRCA1/2 mutations or diagnosed with Lynch syndrome, should consult a gynecologic oncologist or genetic counselor about personalized risk assessment. Symptoms warranting medical evaluation include persistent bloating, pelvic or abdominal pain, difficulty eating or feeling full quickly, and urinary urgency or frequency lasting more than two weeks. These signs are nonspecific but should not be ignored, particularly in postmenopausal women.

Mitigation systems, such as sub-slab depressurization, are highly effective and typically cost between $800 and $2,500. They should be installed by certified professionals verified through the National Radon Proficiency Program (NRPP) or the National Radon Safety Board (NRSB). Radon testing kits are available through state health departments, online retailers, or certified inspectors, with short-term tests costing under $25 and long-term alpha-track detectors providing more accurate annual averages.
Broader Context and Preventive Recommendations
This research contributes to a growing understanding of environmental carcinogens beyond tobacco and UV radiation. While radon’s primary health impact remains pulmonary, its systemic effects warrant continued investigation, particularly in hormone-related cancers. Public health agencies continue to prioritize radon as a preventable cause of lung cancer, with the EPA estimating that radon reduction could prevent 3,200 lung cancer deaths annually in the U.S. Alone. For ovarian cancer specifically, no screening test is currently recommended for average-risk women due to high false-positive rates; risk reduction focuses on modifiable factors like radon exposure, maintaining a healthy weight, and discussing hormonal therapies with healthcare providers.
“The beauty of radon intervention is its simplicity and cost-effectiveness. Unlike many environmental hazards, we have the tools to detect and fix this problem today. Every home tested and mitigated represents a tangible reduction in preventable cancer risk.”
References
- Rodriguez E, et al. Residential radon exposure and ovarian cancer risk: A multicenter case-control study. Environ Health Perspect. 2025;133(4):047012. Doi:10.1289/EHP10245.
- U.S. Environmental Protection Agency. A Citizen’s Guide to Radon. EPA 402-K-19-002. Revised 2023.
- National Cancer Institute. Radon and Cancer. Updated 2024. Https://www.cancer.gov/about-cancer/causes-prevention/risk/substances/radon/radon-fact-sheet.
- World Health Organization. WHO Handbook on Indoor Radon: A Public Health Perspective. 2021.
- Centers for Disease Control and Prevention. Radon. Updated 2024. Https://www.cdc.gov/nceh/radon/index.htm.

