Dr. Wu Rui highlights the critical disparity between available medical interventions and public adherence regarding respiratory infections. By analyzing current epidemiological trends, bridging this gap through enhanced vaccination literacy and systemic air quality improvements is essential to reducing global morbidity and healthcare system strain.
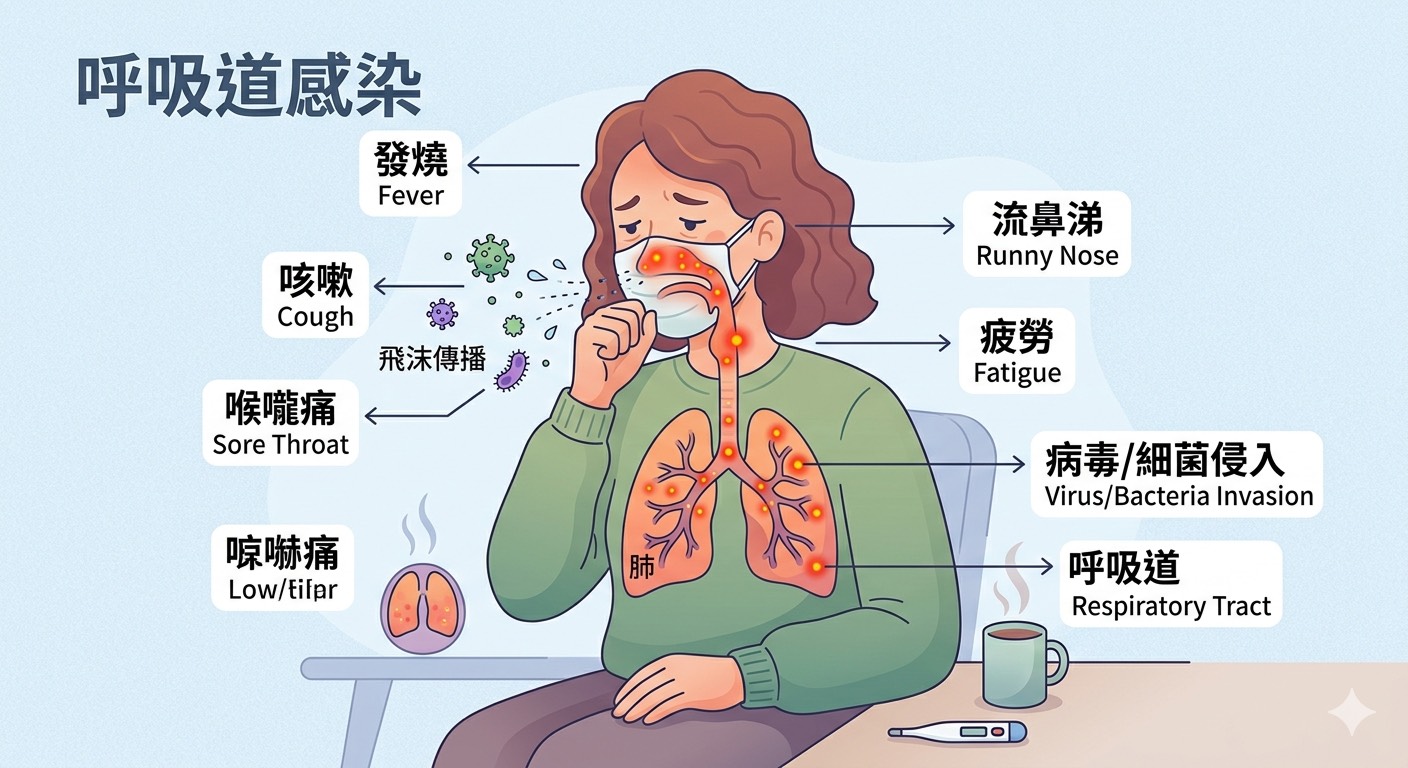
The persistence of respiratory infections—ranging from seasonal influenza and Respiratory Syncytial Virus (RSV) to evolving SARS-CoV-2 variants—represents more than a seasonal inconvenience. We see a systemic failure of preventative integration. When we discuss the “distance” between the public and respiratory health, we are discussing the lag between clinical innovation and bedside application. For the average patient, So the difference between a manageable upper respiratory infection and a life-threatening progression to viral pneumonia.
In Plain English: The Clinical Takeaway
- Vaccines are shields, not bubbles: While vaccines may not stop every mild infection, their primary goal is to prevent “severe outcomes,” meaning they retain you out of the hospital.
- Airflow is medicine: Improving ventilation (bringing in fresh air) is as clinically significant as wearing a mask in reducing the viral load you encounter.
- Timing is everything: Antiviral medications work by stopping the virus from replicating, but they must be started within the first 48-72 hours of symptoms to be effective.
The Molecular Gateway: How Respiratory Viruses Breach the Epithelial Barrier
To understand the distance between prevention and infection, we must examine the mechanism of action—the specific biochemical process through which a drug or virus produces its effect. Most respiratory pathogens target the respiratory epithelium, the thin layer of cells lining your airways.
Viruses like SARS-CoV-2 utilize the ACE2 receptor as a doorway into the cell, while influenza viruses often bind to sialic acid receptors. Once inside, the virus hijacks the cell’s ribosomal machinery to replicate its own genetic material. This process triggers a cytokine storm—an overproduction of immune cells that, while intended to fight the virus, often causes collateral damage to the lung tissue, leading to acute respiratory distress syndrome (ARDS).
Current pharmacological interventions focus on “viral entry inhibitors” or “polymerase inhibitors.” The latter, such as Molnupiravir or Remdesivir, work by introducing errors into the virus’s genetic copying process, effectively “jamming” the biological photocopier so the virus cannot multiply.
The Global Immunity Gap: From Local Outbreaks to Systemic Vulnerability
Clinicians are currently observing a phenomenon known as the “immunity gap” or “immunity debt.” This occurs when a population experiences a period of low exposure to common pathogens—due to lockdowns or strict masking—resulting in a decline in naturally acquired immunity. As we move further into 2026, we are seeing a surge in pediatric RSV and influenza cases that are more severe than pre-pandemic norms.
Here’s not merely a local issue in East Asia but a global epidemiological trend. In the United States, the CDC has noted shifted seasonality in respiratory peaks, while the World Health Organization (WHO) has expressed concern over the “syndemic” nature of these infections—where multiple viruses circulate simultaneously, complicating diagnosis and treatment.
“The challenge we face in 2026 is not a lack of vaccines, but a crisis of confidence and access. We are seeing a decoupling of clinical efficacy from public uptake, which leaves our most vulnerable populations exposed during peak transmission windows.” — Dr. Maria Van Kerkhove, Technical Lead on COVID-19, WHO.
Comparing Prophylactic Strategies: mRNA vs. Traditional Inactivated Vaccines
The debate over vaccine platforms often confuses the public. To provide clarity, we must look at the data regarding efficacy versus reactogenicity (the physical response to a vaccine, such as fever or soreness).
mRNA vaccines provide a blueprint to the body to create a spike protein, triggering a robust T-cell response. In contrast, inactivated vaccines use a “killed” version of the virus. While mRNA platforms allow for faster updates to match new variants, inactivated vaccines are often more stable for transport in regions without ultra-cold chain infrastructure, such as parts of Southeast Asia and Africa.
| Vaccine Platform | Mechanism of Action | Primary Advantage | Common Side Effects | Regulatory Path |
|---|---|---|---|---|
| mRNA | Genetic instruction for protein synthesis | Rapid adaptation to variants | Myalgia, low-grade fever | FDA/EMA Fast-Track |
| Inactivated | Introduction of killed pathogen | Higher thermal stability | Injection site soreness | Standard WHO Prequalification |
| Protein Subunit | Purified viral proteins + adjuvant | Lower reactogenicity | Mild fatigue | Traditional BLA Process |
Regulatory Landscapes and the Hurdle of Patient Access
The transition from a clinical trial to a pharmacy shelf involves rigorous regulatory hurdles. Most new antivirals undergo double-blind placebo-controlled trials—the gold standard of research where neither the patient nor the doctor knows who is receiving the drug and who is receiving a sugar pill—to eliminate bias.
However, geo-epidemiological bridging reveals a stark divide. While the European Medicines Agency (EMA) and the FDA may approve a new protease inhibitor, the actual cost and distribution networks in developing healthcare systems often mean the “distance” to the patient remains vast. Funding for these trials is predominantly driven by large pharmaceutical entities and government grants (such as the NIH), which occasionally creates a bias toward treatments that are profitable rather than those that are most accessible for global public health.
Contraindications & When to Consult a Doctor
Not every respiratory treatment is suitable for every patient. Contraindications—specific situations in which a drug or treatment should not be used because it may be harmful—are critical to review.

- mRNA Vaccines: Individuals with a documented history of severe allergic reactions (anaphylaxis) to polyethylene glycol (PEG) should consult an immunologist before administration.
- Antivirals: Certain protease inhibitors can have severe drug-drug interactions with common blood pressure medications or anticoagulants. Always provide a full medication list to your provider.
- Steroids: While used to treat severe lung inflammation, corticosteroids can suppress the immune system and should not be used in the early “viral phase” of an infection without strict medical supervision.
Seek immediate emergency care if you experience:
- Oxygen saturation (SpO2) dropping below 94% on a pulse oximeter.
- Persistent pain or pressure in the chest.
- New onset of confusion or inability to wake/stay awake.
- Bluish lips or face (cyanosis).
The “distance” Dr. Wu Rui speaks of is not a physical one, but a cognitive and systemic gap. As we refine our molecular understanding of respiratory pathogens, the focus must shift from simply creating the next “miracle drug” to ensuring that the existing arsenal of evidence-based medicine is accessible, understood and utilized by the global population. The trajectory of public health in 2026 depends not on the brilliance of our laboratories, but on the strength of our delivery systems.