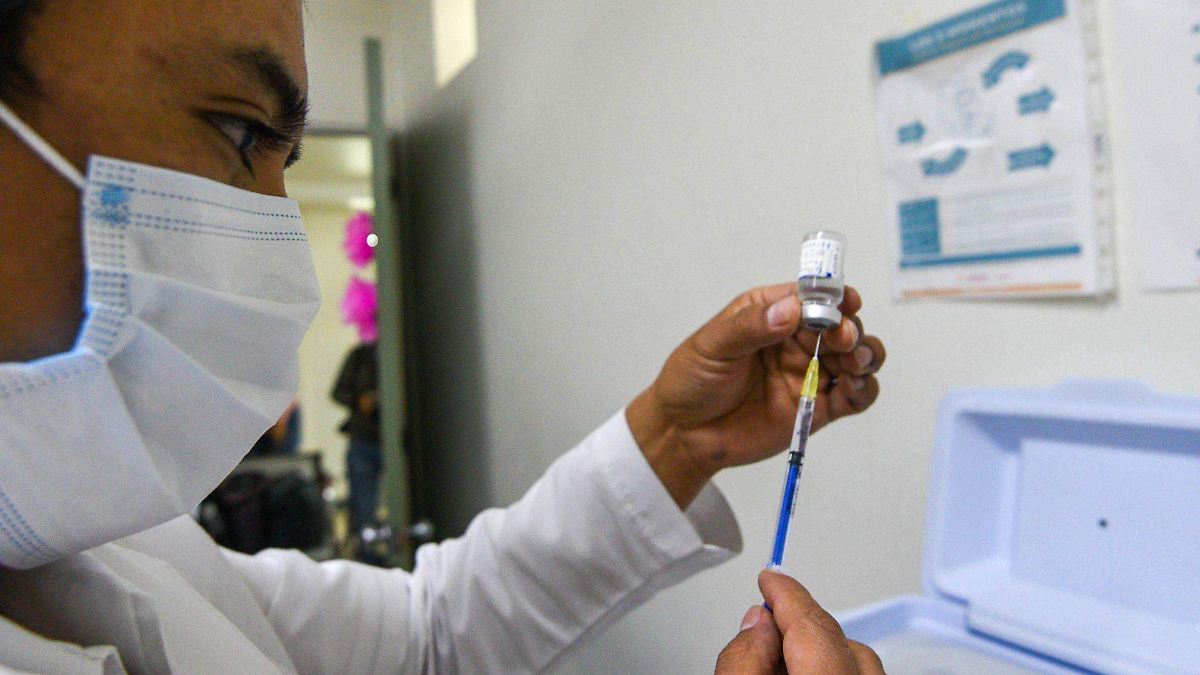
Health officials in Tamaulipas, Mexico, are initiating a landmark vaccination program this week, offering respiratory syncytial virus (RSV) immunization to pregnant individuals for the first time. This proactive measure aims to protect newborns from severe RSV-related illness during their first vulnerable months of life, a significant public health advancement given RSV’s substantial burden on infant hospitalization rates.
The decision to vaccinate pregnant individuals represents a paradigm shift in RSV prevention. Historically, managing RSV has largely focused on supportive care for infected infants and, more recently, on passive immunization with monoclonal antibodies for high-risk newborns. However, these approaches have limitations. Passive immunization provides temporary protection, while supportive care doesn’t alter the course of infection. Maternal vaccination leverages the mother’s immune system to actively produce antibodies that are then transferred to the fetus, providing crucial protection in early infancy – a period when infants are most susceptible to severe RSV disease. This strategy is particularly impactful because infants under six months old have underdeveloped immune systems and often don’t respond effectively to vaccines directly.
In Plain English: The Clinical Takeaway
- Protecting Babies: This vaccine isn’t for the pregnant person themselves, but to give the baby antibodies *before* they’re born, shielding them from a common, serious lung virus.
- RSV is Serious: RSV can cause bronchiolitis (inflammation of the small airways in the lungs) and pneumonia, especially in babies. This vaccine aims to reduce hospitalizations.
- How it Works: The mother gets the shot, her body makes antibodies and those antibodies cross the placenta to protect the baby for the first few months of life.
The Science Behind Maternal RSV Vaccination
The RSV vaccines authorized for maternal immunization utilize mRNA technology, similar to some COVID-19 vaccines. The mechanism of action involves introducing messenger RNA (mRNA) encoding for a stabilized form of the RSV fusion (F) protein. This F protein is crucial for the virus to enter and infect cells. Once inside the body, the mRNA instructs cells to produce the F protein, triggering an immune response. The immune system recognizes the F protein as foreign and generates antibodies and T cells specifically targeted against it. These antibodies, particularly immunoglobulin G (IgG), cross the placenta, providing passive immunity to the developing fetus. ( PubMed: mRNA-1345: A novel mRNA vaccine against respiratory syncytial virus). The key advantage of using a stabilized F protein is that it elicits a broader immune response, protecting against both RSV-A and RSV-B strains.

Clinical trials, including the pivotal Phase III trial (PROTECT) sponsored by Pfizer, demonstrated a vaccine efficacy of approximately 82% against severe lower respiratory tract disease (SLRTD) in infants born to vaccinated mothers. The trial, involving over 7,000 pregnant individuals, showed a statistically significant reduction in medically attended RSV-associated SLRTD through the first six months of life. Side effects were generally mild and similar to those observed with other mRNA vaccines, primarily consisting of local pain at the injection site, fatigue, and headache. ( The New England Journal of Medicine: Maternal RSV Vaccination). Funding for the PROTECT trial was provided by Pfizer, a factor that necessitates transparent interpretation of the results, though the rigorous trial design and large sample size bolster confidence in the findings.
Global Implications and Regional Healthcare Access
The rollout in Tamaulipas is part of a broader global trend. In the United States, the Food and Drug Administration (FDA) approved Abrysvo (Pfizer) and Arevyvy (GSK) for maternal RSV vaccination in August 2023. The Centers for Disease Control and Prevention (CDC) subsequently recommended the vaccine for pregnant individuals during the RSV season (typically fall and winter). The European Medicines Agency (EMA) followed suit with approvals in late 2023 and early 2024. However, access to these vaccines remains uneven globally. Lower-income countries face challenges related to vaccine procurement, cold chain infrastructure, and healthcare worker training. The Pan American Health Organization (PAHO) is working to facilitate equitable access to RSV vaccines across the Americas, but significant logistical hurdles remain.
“Maternal RSV vaccination represents a major step forward in protecting infants from a disease that has historically caused significant morbidity and mortality. The ability to proactively transfer immunity to the fetus is a game-changer,” says Dr. Jay Edwards, a leading epidemiologist at the CDC, in a recent statement.
Data on RSV Incidence and Severity
| Region | Estimated Annual RSV Hospitalizations (Infants <1 year) | RSV-Associated Mortality (Infants <1 year) |
|---|---|---|
| United States | 58,000 – 80,000 | 100 – 500 |
| Europe | 100,000 – 200,000 | 500 – 1,000 |
| Latin America & Caribbean | Data Limited, estimated 80,000+ | Data Limited, significant underreporting |
(Source: World Health Organization, CDC, and European Centre for Disease Prevention and Control – data estimates vary based on surveillance systems).
Contraindications & When to Consult a Doctor
While RSV vaccination during pregnancy is generally considered safe, certain contraindications exist. Individuals with a history of severe allergic reaction (anaphylaxis) to any component of the vaccine should not receive it. Similarly, those with a history of Guillain-Barré syndrome (GBS) within six weeks of a previous vaccine dose should consult with their physician before vaccination. It’s crucial to discuss any underlying medical conditions or allergies with a healthcare provider. Following vaccination, individuals should consult a doctor if they experience any signs of a severe allergic reaction, such as difficulty breathing, swelling of the face or throat, or hives. Any unusual symptoms or concerns should be promptly addressed by a medical professional.
The implementation of this vaccination program in Tamaulipas, and its subsequent adoption in other regions, signals a new era in RSV prevention. Continued surveillance, ongoing research into long-term immunity, and equitable access to vaccines will be crucial to maximizing the public health benefits of this innovative approach. The success of maternal RSV vaccination hinges on robust public health infrastructure, effective communication strategies, and a commitment to protecting the most vulnerable members of our society – newborns.