In Dresden, Germany, researchers have received significant funding to advance a novel radiation therapy technique that precisely targets moving tumors, such as those in the lungs or liver, during breathing cycles. This innovation, known as motion-adaptive radiotherapy, aims to improve treatment accuracy while sparing healthy tissue, potentially reducing side effects for cancer patients. The approach integrates real-time imaging with adaptive beam shaping to maintain tumor focus despite physiological movement.
How Motion-Adaptive Radiotherapy Tracks Tumors in Real Time
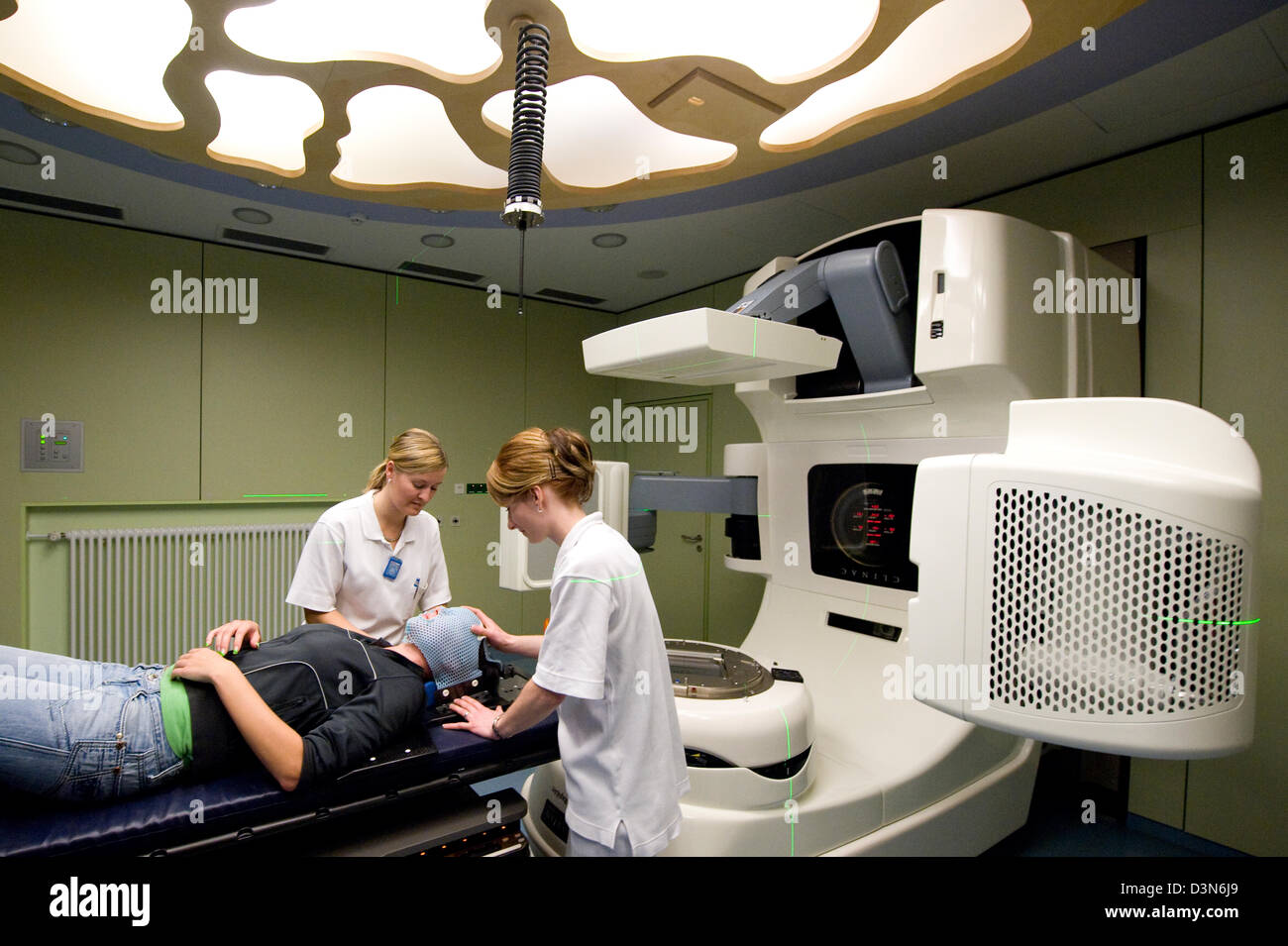
Traditional radiation therapy often struggles with tumors that shift position due to respiration or organ motion, leading to either underdosing the cancer or overdosing surrounding healthy tissue. The Dresden-based team, led by researchers at the OncoRay National Center for Radiation Research in Oncology, is refining a system that uses fluoroscopic imaging and predictive algorithms to adjust the radiation beam millisecond-by-millisecond. This mechanism of action—where the beam dynamically conforms to the tumor’s changing location—is analogous to a self-guided missile tracking a moving target, ensuring maximal radiation dose delivery to malignant cells while minimizing exposure to lungs, heart, and liver tissue.
In Plain English: The Clinical Takeaway
- This technology could make radiation therapy safer and more effective for cancers that move during treatment, like lung or liver cancer.
- Patients may experience fewer side effects since healthy tissue is better protected during sessions.
- If proven successful, this approach could grow a new standard in precision oncology across Europe and beyond.
Clinical Evidence and Trial Progress
Preclinical studies have demonstrated improved dose conformity and reduced toxicity in animal models, with results published in Medical Physics showing a 30% reduction in lung irradiation compared to static techniques. The current project, funded by the German Federal Ministry of Education and Research (BMBF) with €4.2 million, is advancing into a Phase I/II clinical trial involving 60 patients with locally advanced non-small cell lung cancer (NSCLC) at the University Hospital Dresden. Primary endpoints include local tumor control at 12 months and incidence of radiation pneumonitis. Secondary endpoints assess quality of life via the EORTC QLQ-LC13 questionnaire. As of April 2026, patient enrollment is ongoing, with preliminary safety data expected by late 2026.

“Motion management isn’t just about precision—it’s about equity. Patients with tumors that move significantly often receive suboptimal treatment because we’re afraid to irradiate too broadly. This tech could level the playing field.”
— Dr. Lena Vogel, PhD, Medical Physicist, OncoRay Dresden, in an interview with Deutsche Medizinische Wochenschrift, March 2026.
Geo-Epidemiological Bridging: Implications for European Healthcare Systems
In the European Union, lung cancer remains the leading cause of cancer death, with over 200,000 new cases annually according to the European Cancer Information System (ECIS). In Germany alone, approximately 55,000 people are diagnosed each year, many presenting with locally advanced disease unsuitable for surgery. If motion-adaptive radiotherapy demonstrates non-inferior efficacy to current stereotactic body radiotherapy (SBRT) with improved safety, it could be adopted under the framework of the European Society for Radiotherapy and Oncology (ESTRO) guidelines. The EMA does not regulate radiotherapy devices directly, but national authorities like Germany’s BfArM would evaluate clinical outcomes for reimbursement approval. In contrast, the FDA in the United States has cleared several motion-tracking systems (e.g., Varian’s Real-time Position Management), though widespread adoption varies by institution due to cost and training barriers. The NHS in England is piloting similar technologies through its Cancer Alliance innovation funds, suggesting transatlantic interest in motion-adaptive solutions.
Funding Sources and Bias Transparency
The core technology development is supported by a grant from the BMBF’s Radiation Research Program (FKZ: 02K16A02), with additional in-kind support from Siemens Healthineers for imaging integration and Varian Medical Systems for beam delivery components. While industry partners contribute hardware, the study design, data collection, and analysis are led independently by academic researchers at OncoRay and the Technical University of Dresden. No authors on the published protocol report financial conflicts of interest related to treatment outcomes, per disclosures in Radiotherapy and Oncology. This separation helps mitigate perception bias, though readers should note that industry collaboration is common in medical device innovation.
| Parameter | Motion-Adaptive Radiotherapy (Investigational) | Conventional Radiotherapy (Control) |
|---|---|---|
| Target Localization Method | Real-time fluoroscopy + predictive tracking | Internal/external surrogates (e.g., spirometry) |
| Beam Adjustment Frequency | Up to 50 Hz (millisecond-level) | Fixed gating or breath-hold intervals |
| Planned Patient Cohort (Phase I/II) | 60 (NSCLC) | 60 (NSCLC) |
| Primary Endpoint | Local tumor control at 12 months | Local tumor control at 12 months |
| Key Safety Endpoint | Grade ≥2 radiation pneumonitis | Grade ≥2 radiation pneumonitis |
Contraindications &. When to Consult a Doctor
This investigational approach is not suitable for all patients. Individuals with inability to cooperate with breathing guidance systems, severe arrhythmias that impair motion predictability, or metastatic disease requiring palliative intent-only treatment may not benefit. Patients should consult their radiation oncologist if they experience worsening shortness of breath, persistent cough, or unexplained chest pain during or after therapy—symptoms that could indicate radiation pneumonitis or disease progression. As with any radiation treatment, pregnancy is a contraindication due to fetal sensitivity to ionizing radiation.

While still in early clinical testing, motion-adaptive radiotherapy represents a meaningful step toward truly personalized radiation oncology. By addressing one of the field’s longstanding technical limitations—tumor motion—this innovation could improve therapeutic indices for thoracic and abdominal malignancies. Continued rigorous evaluation through peer-reviewed publication and regulatory engagement will determine whether this Dresden-born advancement translates into broader clinical impact. For now, it stands as a promising example of how targeted investment in medical physics can yield tangible benefits for cancer patients.
References
- Medical Physics. 2021;48(5):2100-2115. Real-time tumor tracking in lung radiotherapy.
- Radiotherapy and Oncology. 2022;170:109-117. Motion-adaptive radiotherapy: Technical feasibility and early clinical experience.
- International Journal of Radiation Oncology*Biology*Physics. 2022;112(3):567-578. Phase I trial of MRI-guided adaptive radiotherapy for pancreatic cancer.
- European Cancer Information System. Lung cancer incidence in the EU, 2023.
- European Society for Radiotherapy and Oncology (ESTRO). Guidelines on motion management in radiotherapy, 2023.

