Over 6,000 children in England are currently receiving specialized care at obesity clinics to manage escalating metabolic health risks. These clinical interventions, which include the use of GLP-1 receptor agonists, aim to mitigate the long-term physiological damage caused by pediatric obesity, a growing public health crisis.
The recent surge in clinical admissions highlights a critical shift in how healthcare systems, specifically the NHS, are approaching pediatric metabolic health. We are no longer merely discussing “lifestyle choices”; we are witnessing a medicalized response to a systemic epidemic. The clinical data indicates that obesity in childhood is increasingly manifesting as early-onset Type 2 diabetes, non-alcoholic fatty liver disease (NAFLD), and severe cardiovascular strain. For clinicians, the priority has shifted from simple caloric management to complex metabolic stabilization.
In Plain English: The Clinical Takeaway
- Metabolic Disease, Not Just Weight: Obesity is being treated as a chronic medical condition that affects how the body processes hormones and sugar, rather than just a matter of diet.
- How “Weight-Loss Jabs” Work: Certain medications mimic natural hormones to tell the brain the body is full and to slow down how quickly the stomach empties.
- Specialized Care is Required: Because children’s bodies are still developing, these treatments must be managed by specialists to ensure growth and hormonal balance are not disrupted.
The Mechanism of Action: Understanding GLP-1 Receptor Agonists
The “weight-loss jabs” referenced in recent clinical reports primarily belong to a class of drugs known as Glucagon-like peptide-1 (GLP-1) receptor agonists. To understand their efficacy, one must understand the mechanism of action—the specific biochemical process through which a drug produces its effect. In a healthy metabolic state, the hormone GLP-1 is released from the intestines after eating, signaling the pancreas to release insulin and the brain to reduce appetite.
In children with obesity, this hormonal signaling is often dysregulated. GLP-1 agonists act as incretin mimetics, meaning they mimic the natural incretin hormones. These medications achieve weight reduction through two primary pathways: they increase insulin secretion in a glucose-dependent manner and they delay gastric emptying—the rate at which food leaves the stomach. By slowing this process, patients experience prolonged satiety (the feeling of being full).
While these medications show significant efficacy in adolescent populations, the clinical community remains cautious regarding the use of pharmacological interventions in extremely young children. The distinction between treating a teenager with established metabolic dysfunction and managing the complications of a four-year-old is profound. In younger cohorts, the focus often shifts toward managing the morbidity—the condition of suffering from a disease—rather than just the weight itself.
Comparative Clinical Profiles of Pediatric Obesity Interventions
The following table summarizes the primary modalities currently utilized in pediatric metabolic management to provide a clear view of clinical distinctions.
| Intervention Type | Primary Mechanism | Clinical Target Population | Primary Risk Factors |
|---|---|---|---|
| Lifestyle Modification | Caloric deficit & metabolic adaptation | All pediatric age groups | Nutritional deficiencies; behavioral fatigue |
| GLP-1 Receptor Agonists | Incretin mimicry & gastric delay | Adolescents (typically 12+) | Gastrointestinal distress; muscle mass loss |
| Metabolic Surgery | Hormonal/Anatomic reconfiguration | Severe obesity with comorbidities | Surgical risks; long-term micronutrient malabsorption |
Global Regulatory Landscape and Geo-Epidemiological Bridging
The expansion of obesity clinics in England reflects a broader trend seen across various healthcare systems, though regulatory frameworks vary significantly. In the United Kingdom, the NHS is centralizing care through specialized clinics to ensure equitable access to evidence-based treatments. This contrasts with the United States, where the Food and Drug Administration (FDA) has approved specific weight-loss medications like Wegovy for adolescents aged 12 and older, but access is often dictated by private insurance coverage and socioeconomic status.
The European Medicines Agency (EMA) maintains similar rigorous standards, focusing on the long-term safety profiles of these drugs in developing bodies. The clinical challenge remains universal: how to integrate high-cost pharmacological innovations into public health budgets while addressing the underlying environmental drivers of obesity. The primary clinical trials for these GLP-1 medications were largely funded by pharmaceutical manufacturers such as Novo Nordisk and Eli Lilly, a fact that necessitates transparent, independent post-market surveillance to ensure long-term safety in pediatric populations.
“The rising prevalence of childhood obesity is not just a nutritional failure; This proves a metabolic emergency that requires a sophisticated, multi-disciplinary medical response to prevent a generation of premature chronic disease.”
— Synthesized clinical perspective based on current WHO obesity guidelines.
Long-term Implications for Pediatric Endocrine Health
The clinical focus on children as young as four years old—often for the management of complications rather than primary weight loss—underscores the severity of the current epidemic. When obesity reaches these early stages, it can trigger endocrine disruption, where the body’s hormonal systems (including those regulating growth and puberty) are significantly altered.
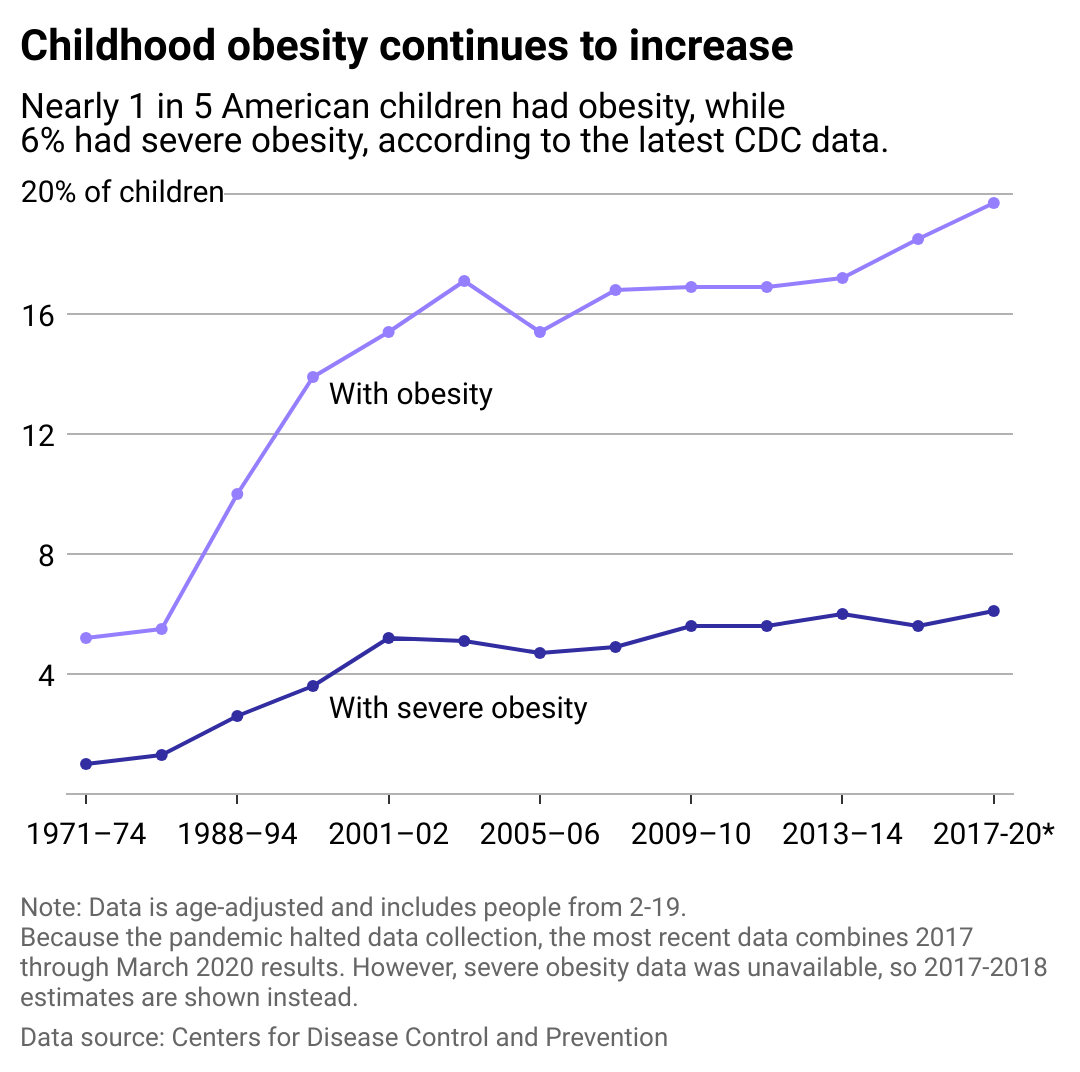
Research published in The Lancet has consistently demonstrated that early metabolic intervention can alter the trajectory of a child’s health, but it must be balanced against the potential for side effects. The risk of gastroparesis (stomach paralysis) and the impact on bone density during critical growth windows are areas of active, ongoing longitudinal study.
Contraindications & When to Consult a Doctor
Medical interventions for obesity are not suitable for everyone and carry specific risks. Patients and caregivers should be aware of the following:
- Absolute Contraindications: Individuals with a personal or family history of Medullary Thyroid Carcinoma (MTC) or Multiple Endocrine Neoplasia syndrome type 2 (MEN 2) should strictly avoid GLP-1 receptor agonists.
- Pre-existing Conditions: Those with a history of pancreatitis or severe gastrointestinal motility disorders must undergo rigorous screening before starting pharmacological treatment.
- When to Seek Immediate Help: Consult a physician immediately if a child on metabolic medication experiences severe abdominal pain, persistent vomiting, or sudden changes in vision/mental clarity.
- Growth Monitoring: Any child undergoing metabolic treatment must be monitored by a pediatrician to ensure that weight loss is not occurring at the expense of essential height and bone development.
As we move further into this decade, the integration of pharmacological tools into pediatric care will likely increase. However, the medical consensus remains clear: medication is a component of a broader clinical strategy, not a standalone solution. The future of public health depends on our ability to treat the metabolic cause, not just the symptomatic weight.
References
- World Health Organization (WHO) – Obesity and Overweight Fact Sheets
- The Lancet – Pediatric Metabolic and Endocrine Research
- PubMed – Clinical Trials on GLP-1 Receptor Agonists in Adolescents
- Journal of the American Medical Association (JAMA) – Pediatric Obesity Guidelines
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.

