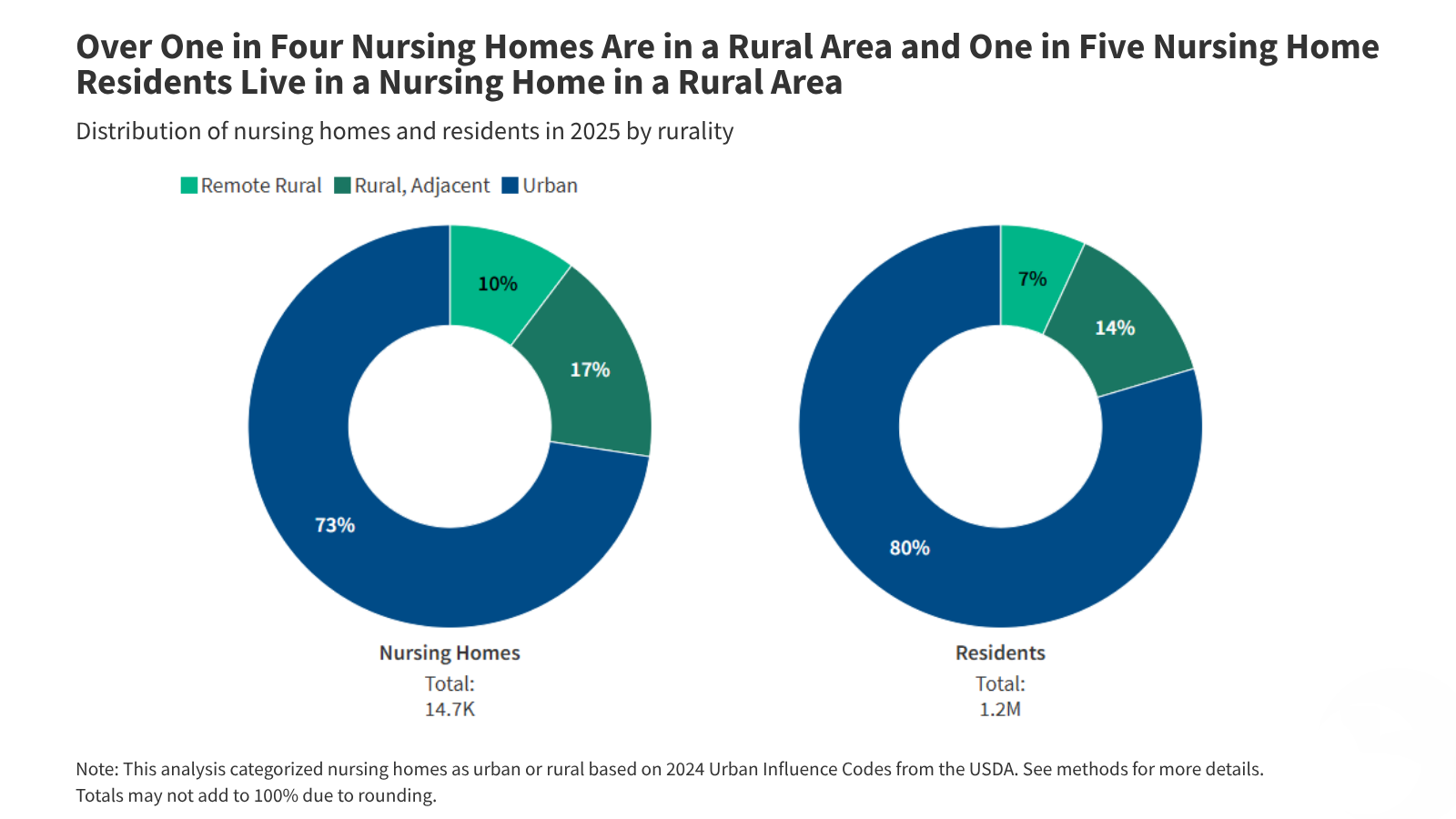
A recent analysis of Nursing Home Compare data reveals significant disparities in quality of care between rural and urban nursing homes across the United States. Rural facilities consistently report lower staffing levels, fewer services, and poorer health inspection results, impacting the approximately 1.3 million Americans residing in these long-term care settings. This analysis underscores the urgent need for targeted interventions to improve care quality and access for vulnerable populations in rural communities.
In Plain English: The Clinical Takeaway
- Lower Staffing = Less Attention: Rural nursing homes often have fewer nurses and aides per resident, meaning residents may not get the help they need as quickly.
- Fewer Services Mean Limited Care: Access to specialized care like physical therapy or mental health services is often reduced in rural areas.
- Inspection Scores Matter: Lower inspection scores indicate potential problems with safety and quality of care, and rural facilities tend to have lower scores.
The Rural Nursing Home Landscape: A Growing Crisis
The challenges facing rural nursing homes are multifaceted and deeply rooted in systemic issues. Declining rural populations, coupled with an aging demographic, are increasing the demand for long-term care services in areas already struggling with limited resources. This demographic shift exacerbates existing financial pressures on these facilities, often leading to staffing shortages and reduced investment in infrastructure, and services. The financial viability of rural nursing homes is increasingly precarious, with many operating on thin margins or facing closure. This creates a cascade effect, limiting access to care for residents and impacting local economies.

The Impact of Staffing Ratios and Quality Metrics
Staffing ratios are a critical determinant of quality of care in nursing homes. Lower staffing levels are directly correlated with increased rates of pressure ulcers (bedsores), urinary tract infections, and falls – all preventable adverse events. Data from the Centers for Medicare & Medicaid Services (CMS) consistently demonstrates a strong association between Registered Nurse (RN) hours per resident day and improved clinical outcomes. Rural facilities, on average, provide significantly fewer RN hours per resident compared to their urban counterparts. This disparity is further compounded by difficulties in recruiting and retaining qualified healthcare professionals in rural areas. The mechanism of action here isn’t complex: fewer staff mean less time for individualized care, monitoring, and preventative interventions.
Geographic Disparities and Access to Specialized Care
Beyond staffing, access to specialized medical care is significantly limited in rural areas. Residents of rural nursing homes are less likely to have access to geriatricians, specialists in the care of older adults, and other essential healthcare providers. This lack of specialized expertise can lead to delayed diagnoses, inadequate treatment of complex medical conditions, and increased hospital readmission rates. The geographic isolation likewise presents challenges for emergency medical services, potentially delaying critical care in time-sensitive situations. The FDA is currently reviewing proposals for telehealth expansion to address these access issues, but regulatory hurdles and reimbursement policies remain significant barriers.
Funding, Bias, and the Role of Research
Much of the data informing this analysis originates from the Nursing Home Compare database, a publicly funded resource maintained by CMS. However, it’s crucial to acknowledge potential biases inherent in self-reported data. Facilities are incentivized to present a favorable picture of their performance, potentially underreporting deficiencies. Independent research, such as a 2023 study funded by the Agency for Healthcare Research and Quality (AHRQ), has corroborated the findings of lower quality of care in rural facilities, utilizing a combination of publicly available data and on-site inspections.
“The persistent disparities in rural nursing home quality are a clear indication of systemic failures in our long-term care system. We need to move beyond simply identifying the problem and focus on implementing evidence-based solutions that address the unique challenges faced by rural communities.” – Dr. Emily Carter, Epidemiologist, AHRQ.
A Comparative Look: Rural vs. Urban Nursing Home Characteristics (2025 Data)
| Characteristic | Rural Nursing Homes (Average) | Urban Nursing Homes (Average) |
|---|---|---|
| Total Number of Residents | 45 | 112 |
| RN Hours per Resident Day | 2.8 | 3.9 |
| Overall Health Inspection Rating (5-star scale) | 3.1 | 3.8 |
| Percentage of Residents with Pressure Ulcers | 8.2% | 4.5% |
| Percentage of Residents Receiving Antipsychotics | 18.5% | 14.2% |
The Role of Telehealth and Innovative Care Models
Telehealth offers a promising avenue for improving access to specialized care in rural nursing homes. Remote monitoring technologies, virtual consultations with geriatricians, and telehealth-delivered physical therapy can help bridge the gap in access to essential services. However, successful implementation requires addressing challenges related to broadband access, digital literacy among residents and staff, and reimbursement policies. Innovative care models, such as the “Hospital at Home” program, which provides acute-level care in a patient’s home, are also being explored as potential solutions for reducing hospital readmissions and improving patient outcomes. These models rely on a multidisciplinary team of healthcare professionals and advanced remote monitoring technologies.

Contraindications & When to Consult a Doctor
While advocating for improved rural nursing home care is paramount, it’s crucial to recognize situations requiring immediate medical attention. Residents experiencing unexplained falls, sudden changes in mental status, signs of infection (fever, redness, swelling), or severe pain should be evaluated by a physician immediately. Families should be actively involved in monitoring their loved ones’ care and advocating for their needs. Individuals with pre-existing conditions, such as dementia or heart failure, may be particularly vulnerable to complications and require closer monitoring. If you suspect neglect or abuse, contact your local Adult Protective Services agency.
Looking Ahead: Policy Implications and Future Research
Addressing the challenges facing rural nursing homes requires a comprehensive and coordinated approach involving policymakers, healthcare providers, and community stakeholders. Increased funding for rural healthcare infrastructure, incentives for recruiting and retaining healthcare professionals in rural areas, and regulatory reforms to promote innovative care models are all essential steps. Further research is needed to evaluate the effectiveness of different interventions and identify best practices for improving quality of care in rural long-term care settings. The World Health Organization (WHO) emphasizes the importance of integrated care systems that prioritize the needs of vulnerable populations, including those residing in rural areas.
“Investing in rural healthcare is not just a matter of equity; it’s a matter of public health. A strong rural healthcare system is essential for ensuring the health and well-being of all Americans.” – Dr. Maria Rodriguez, Senior Advisor, CDC.
References
- “Rural-Urban Differences in Nursing Home Quality and the Role of Workforce Availability.” *Health Affairs*.
- Nursing Home Compare. Centers for Medicare & Medicaid Services.
- Agency for Healthcare Research and Quality (AHRQ).
- World Health Organization – Ageing and Health.
- Centers for Disease Control and Prevention – Aging.