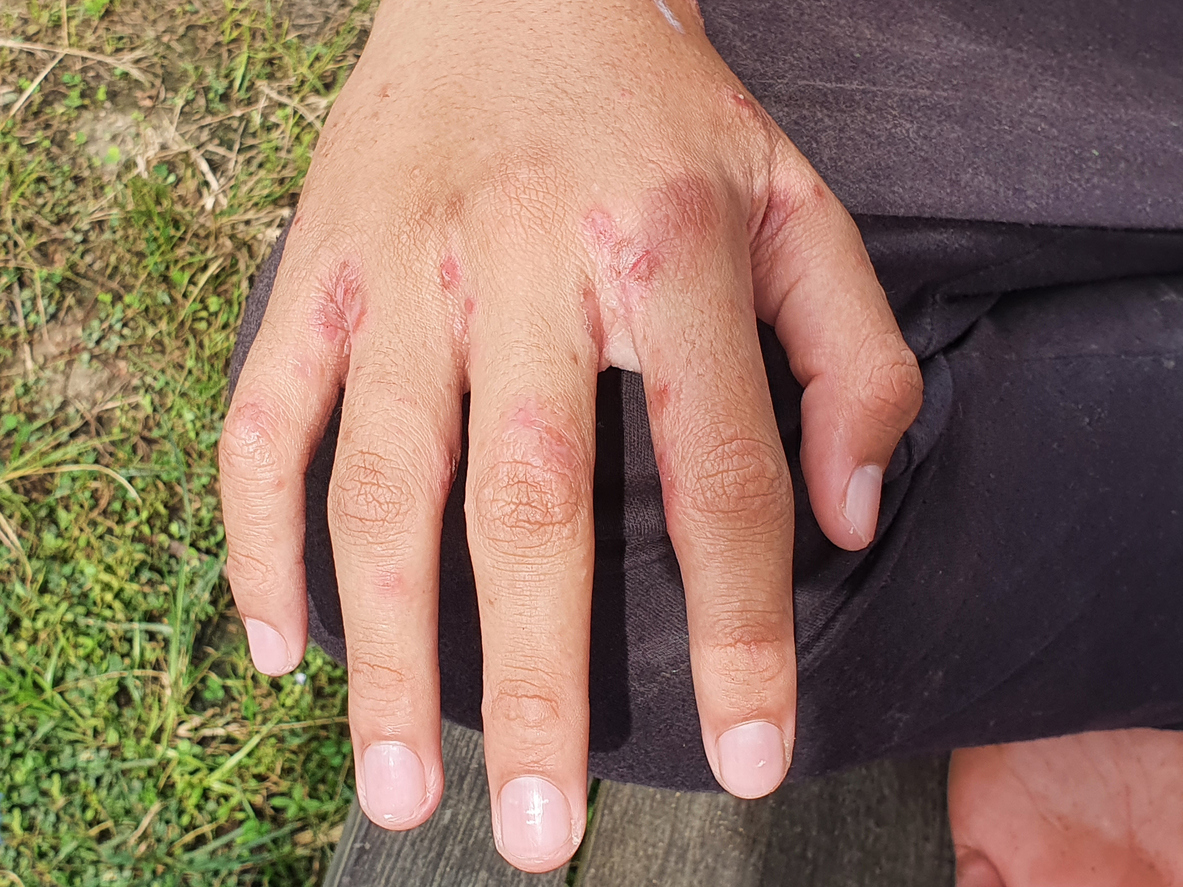
Health authorities are reporting a surge in scabies cases, particularly severe and atypical forms, across several French regions. This outbreak, affecting schools and public facilities, is driven by the Sarcoptes scabiei mite, necessitating urgent public health interventions to prevent wider community transmission and manage increasingly resistant strains.
The current escalation is not merely a localized hygiene failure but a complex public health challenge. While classic scabies is a manageable skin infestation, the emergence of “atypical” or crusted scabies—characterized by an overwhelming number of mites—transforms a nuisance into a significant epidemiological risk. For patients and caregivers, the stakes are high: failure to implement simultaneous, systemic treatment across entire households can lead to a “ping-pong” effect of reinfection, prolonging suffering and increasing the burden on primary care systems.
In Plain English: The Clinical Takeaway
- This proves not about cleanliness: Scabies is caused by a microscopic mite that burrows under the skin. it can affect anyone regardless of their hygiene habits.
- Atypical forms are “super-spreaders”: Crusted scabies involves thousands of mites instead of a few dozen, making it far more contagious via surfaces and clothing.
- The “All-or-Nothing” Rule: Because the mite can survive for days off the body, every person in a home must be treated at the same time, even if they have no itching.
The Pathophysiology of the Sarcoptes Scabies Infestation
To understand the current crisis, one must understand the mechanism of action—the specific biological process—of the Sarcoptes scabiei var. hominis. The female mite burrows into the stratum corneum (the outermost layer of the skin), where she deposits eggs and fecal matter. The intense itching associated with scabies is not caused by the mite’s movement, but by a delayed Type IV hypersensitivity reaction—an immune response where the body reacts to the mite’s proteins.
In “atypical” or crusted scabies, this immune response is absent or severely blunted, often due to immunosuppression (e.g., HIV, chemotherapy, or advanced age). Without the immune system to keep the population in check, the mite population explodes from a few dozen to millions. This transforms the patient into a highly contagious vector, as skin scales laden with mites flake off into the environment, contaminating furniture, carpets, and public transport.
Current pharmacological interventions primarily rely on Permethrin, a synthetic pyrethroid. Its mechanism involves disrupting the voltage-gated sodium channels in the mite’s nerve cells, leading to paralysis and death. However, clinicians are increasingly observing treatment failures, suggesting a potential rise in pyrethroid resistance, a trend that mirrors the challenges seen in agricultural pest control.
Geo-Epidemiological Bridging: From Regional Alerts to EMA Protocols
The recent closures of schools and gymnasiums in regions like Rognac and near Marseille highlight a systemic vulnerability in congregate settings. While the French health authorities are managing the immediate crisis, the situation aligns with broader trends monitored by the European Medicines Agency (EMA). In Europe, the shift toward using Ivermectin—an oral antiparasitic—as a first-line or adjunctive therapy is becoming more common when topical treatments fail.
The transition from topical Permethrin to oral Ivermectin represents a shift in strategy. While Permethrin is a localized neurotoxin, Ivermectin binds to glutamate-gated chloride channels in the invertebrate nerve and muscle cells, causing an influx of chloride ions that paralyzes the parasite. The accessibility of these treatments varies across the EU, but the current French outbreak underscores the need for standardized, rapid-response protocols in schools to prevent the “seeding” of the parasite into the general population.
“The rise of crusted scabies in non-institutionalized settings is a red flag for public health. We are seeing a shift where the parasite is no longer confined to the highly vulnerable, but is utilizing those populations as reservoirs to infect the general public through contaminated environments.” — Dr. Sarah Jenkins, Epidemiologist and Consultant on Neglected Tropical Diseases (NTDs).
Research into these outbreaks is largely funded by public health grants and governmental bodies such as the World Health Organization (WHO) and national health ministries. Because scabies is often categorized as a Neglected Tropical Disease (NTD), there is significantly less private pharmaceutical funding compared to chronic diseases, which often slows the development of next-generation parasiticides.
Comparative Analysis: Classic vs. Crusted Scabies
The following table delineates the clinical distinctions that necessitate different public health responses.
| Clinical Feature | Classic Scabies | Crusted (Atypical) Scabies |
|---|---|---|
| Mite Load | 10 to 15 mites per patient | Thousands to millions of mites |
| Primary Symptom | Severe nocturnal pruritus (itching) | Thick, scaly crusts; itching may be absent |
| Transmission Vector | Direct, prolonged skin-to-skin contact | Indirect contact (clothing, bedding, surfaces) |
| Treatment Complexity | Standard topical application | Combined oral and topical; frequent repetitions |
| Contagion Level | Moderate | Extremely High |
The Environmental Vector: Why Schools and Buses are High-Risk
The reports of scabies in school buses and gymnasiums are particularly concerning because they suggest a high prevalence of the crusted variant or a high density of classic cases. In a standard infestation, a few seconds of contact are rarely enough for transmission. However, when a “super-spreader” (a person with crusted scabies) occupies a space, the environment becomes saturated with infectious debris.
To break the cycle of transmission, public health authorities recommend a rigorous decontamination protocol. This includes washing all bedding and clothing used in the last 72 hours at 60°C (140°F) or sealing non-washable items in plastic bags for at least 72 hours. Because the mite cannot survive without a human host for more than a few days, this “environmental starvation” is the only way to ensure the space is safe for reentry.
Contraindications & When to Consult a Doctor
While Permethrin and Ivermectin are generally safe, they are not universal. Permethrin is generally contraindicated or should be used with extreme caution in infants under two months of age due to the risk of skin absorption. Ivermectin is contraindicated during pregnancy and breastfeeding and should be avoided in patients with severe hepatic impairment.

You must consult a physician immediately if you experience:
- Secondary Bacterial Infections: If sores become warm, leak pus, or develop a honey-colored crust (impetigo), this indicates a secondary infection (often Staphylococcus aureus) requiring antibiotics.
- Systemic Symptoms: Fever or chills accompanying a rash.
- Treatment Failure: If itching persists more than two weeks after a full course of treatment, as this may indicate resistance or reinfection.
Future Trajectory: Resistance and Surveillance
The current trend suggests that we are entering a phase of increased parasitic vigilance. The rise of atypical forms is likely a byproduct of an aging global population and an increase in patients with compromised immune systems. As we move further into 2026, the focus must shift toward proactive screening in long-term care facilities and the development of more robust diagnostic tools than the traditional “skin scraping” and microscopy, which can yield false negatives.
The path forward requires a dual approach: aggressive community education to remove the stigma of the “itch” and a coordinated effort by the EMA and WHO to monitor for pyrethroid resistance. Only by treating the environment and the patient as a single unit can we halt the expansion of these atypical outbreaks.