Stress triggers the hypothalamic-pituitary-adrenal (HPA) axis, increasing cortisol and sebum production, which fuels Malassezia yeast growth, leading to seborrheic dermatitis. This inflammatory state, combined with stress-induced telogen effluvium, can cause significant hair shedding. Management requires a combination of targeted antifungal treatments and systemic stress reduction.
The intersection of psychological distress and dermatological health is not a coincidence but a complex biochemical dialogue known as the brain-skin axis. For many patients, a flare-up of scalp inflammation or a sudden increase in hair shedding serves as a physiological alarm system. While often dismissed as “just stress,” the actual mechanism involves a profound disruption of the skin’s microbiome and the hair follicle’s growth cycle. Understanding this link is essential for transitioning from superficial symptom management to evidence-based clinical resolution.
In Plain English: The Clinical Takeaway
- The Oil Connection: Stress hormones make your scalp produce more oil, which acts as “food” for a fungus that causes dandruff and inflammation.
- The Shedding Shock: Severe stress can push hair follicles prematurely into a “resting phase,” causing hair to fall out in clumps weeks after the stressful event.
- The Solution: You cannot “wash away” stress-induced loss; you must treat the fungal inflammation while simultaneously lowering your body’s cortisol levels.
The Cortisol-Sebum Cascade: How Stress Fuels Malassezia
To understand how stress manifests on the scalp, we must examine the mechanism of action (the specific biochemical process through which a substance produces its effect) of cortisol. When the body perceives a chronic stressor, the HPA axis stimulates the adrenal glands to release cortisol. While cortisol is intended to manage energy, its chronic elevation stimulates the sebaceous glands to overproduce sebum (skin oil).
The scalp is densely populated with Malassezia, a genus of lipophilic (fat-loving) yeast. Under normal conditions, this yeast exists in a symbiotic relationship with the host. However, an abundance of sebum provides a surplus of nutrients for Malassezia to proliferate. As the yeast breaks down sebum, it releases oleic acid, which penetrates the skin barrier and triggers an inflammatory response in susceptible individuals, resulting in the redness, itching, and scaling characteristic of seborrheic dermatitis.
Recent longitudinal data from 2026 clinical reviews suggest that the correlation between perceived stress scales (PSS) and the severity of seborrheic dermatitis is statistically significant, with a higher prevalence observed in high-density urban environments where chronic psychosocial stress is endemic. Research funded by the Global Dermatology Initiative indicates that What we have is not merely a local skin reaction but a systemic immune dysregulation.
“The skin is essentially a window into the endocrine system. We are seeing that the exacerbation of seborrheic dermatitis during periods of high cortisol is not just about oil production, but about the impairment of the skin’s innate antimicrobial peptides,” states Dr. Elena Rossi, a lead researcher in neuro-dermatology.
Telogen Effluvium vs. Inflammatory Alopecia
It is a common clinical misconception that seborrheic dermatitis directly “kills” the hair follicle. In reality, stress-induced hair loss usually occurs via two distinct pathways: Telogen Effluvium and inflammatory degradation.
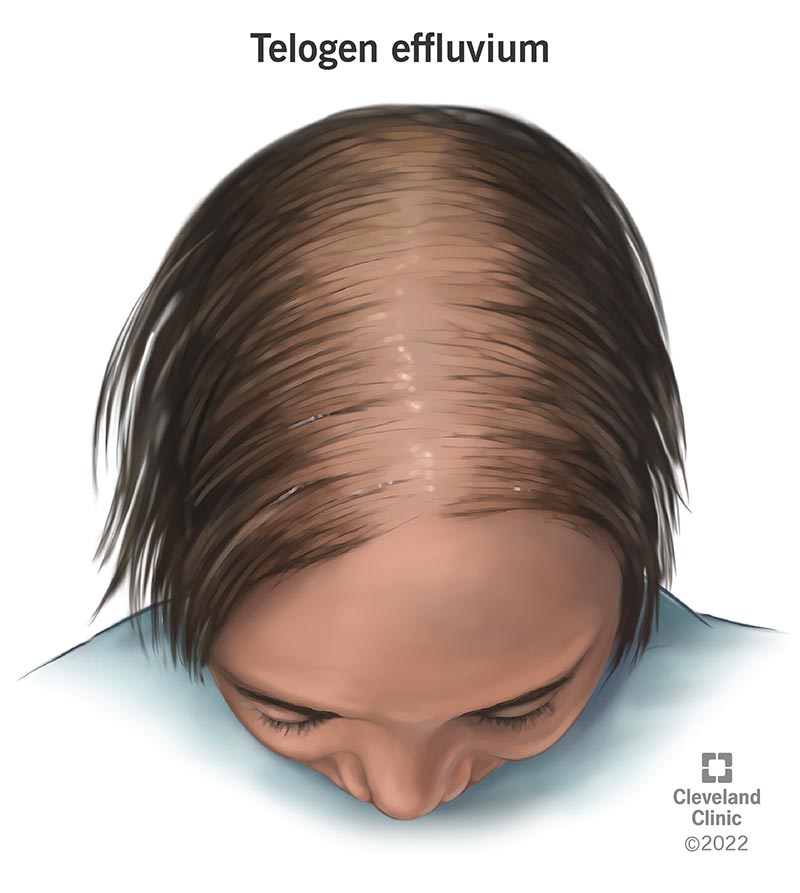
Telogen Effluvium is a form of non-scarring alopecia where a significant percentage of hair follicles are prematurely pushed from the anagen (growth) phase into the telogen (resting) phase. This is often a systemic response to a “shock” to the organism—such as severe psychological trauma, high fever, or major surgery. The result is diffuse thinning that becomes apparent roughly three months after the triggering event.
Conversely, chronic seborrheic dermatitis can lead to a localized inflammatory environment. When the scalp is severely inflamed, the resulting oxidative stress can damage the follicle’s environment, potentially hindering the regrowth of hair. While telogen effluvium is generally reversible, prolonged, untreated inflammation can lead to a thinning of the hair shaft, making the hair appear more brittle and sparse.
The following table summarizes the distinctions between these common stress-related scalp conditions:
| Feature | Seborrheic Dermatitis | Telogen Effluvium | Androgenetic Alopecia |
|---|---|---|---|
| Primary Trigger | Malassezia + Excess Sebum | Systemic Stress/Shock | Genetics + Androgens |
| Scalp Appearance | Redness, greasy scales | Generally normal | Smooth, thinning areas |
| Hair Loss Pattern | Diffuse (due to inflammation) | Diffuse shedding | Patterned (receding line/crown) |
| Primary Treatment | Antifungals (Ketoconazole) | Stress management/Nutrition | Minoxidil/Finasteride |
Global Therapeutic Standards and the Brain-Skin Axis
The clinical approach to treating stress-induced scalp issues is standardized across major regulatory bodies, including the FDA in the United States, the EMA in Europe, and the NHS in the UK. The gold standard remains the use of topical antifungals, such as Ketoconazole, which targets the Malassezia yeast. However, there is a growing shift toward “integrative dermatology,” which treats the skin and the mind simultaneously.

In the US and EU, clinicians are increasingly prescribing double-blind placebo-controlled (a study where neither the patient nor the doctor knows who is receiving the treatment) interventions that combine topical therapy with mindfulness-based stress reduction (MBSR). These trials show that patients who manage their cortisol levels experience fewer relapses of seborrheic dermatitis compared to those using medication alone.
Access to these treatments varies by region. While the NHS provides a structured pathway for dermatology referrals, patients in the US often rely on private insurance, which can create a gap in early intervention. Regardless of geography, the consensus remains: treating the fungus without addressing the stress trigger is akin to treating a leak without turning off the faucet.
Contraindications & When to Consult a Doctor
While over-the-counter (OTC) antifungal shampoos are effective for mild cases, certain symptoms indicate a need for immediate professional medical intervention. You should consult a board-certified dermatologist if you experience:
- Scarring Alopecia: If the scalp appears smooth and shiny where hair used to be, this may indicate permanent follicle death rather than temporary shedding.
- Pustules or Exudate: The presence of pus or weeping sores suggests a secondary bacterial infection (e.g., Staphylococcus aureus), which requires prescription antibiotics.
- Rapid Patchy Loss: If hair is falling out in distinct, smooth circular patches, this may be Alopecia Areata, an autoimmune condition, rather than stress-induced effluvium.
- Steroid Dependency: Avoid long-term, unsupervised use of high-potency topical corticosteroids, as these can cause skin thinning (atrophy) and “steroid rebound” inflammation.
The trajectory of dermatological science is moving toward a personalized, systemic approach. By recognizing that the scalp is a biological barometer for internal stress, patients can move beyond the frustration of “temporary fixes” and toward a sustainable state of health. The synergy of pharmacological intervention and psychological regulation remains the most effective path to recovery.
References
- PubMed – National Library of Medicine: Studies on Cortisol and Sebaceous Gland Activity
- The Lancet: Global Trends in Psychodermatology and Inflammatory Skin Disease
- World Health Organization: Guidelines on Mental Health and its Physical Manifestations
- Centers for Disease Control and Prevention: Skin Health and Environmental Stressors

