Recent clinical data reveals that screening-detected atrial fibrillation (AFib) triples the risk of heart failure. As wearables integrate advanced PPG and ECG sensors, the industry is shifting from simple detection to predictive diagnostics, turning consumer gadgets into clinical-grade early warning systems for cardiovascular collapse and chronic disease management.
For years, the “health” aspect of the smartwatch was largely performative—counting steps, tracking sleep cycles, and giving us a vague sense of “wellness.” But we have hit a critical inflection point. The latest findings regarding the link between screening-detected AFib and heart failure aren’t just medical news; they are a technical mandate for the next generation of wearable silicon. We are moving from reactive alerts (telling you that you are in AFib) to predictive modeling (telling you that you are trending toward heart failure).
This is the transition from a fitness tracker to a medical-grade sentinel.
From PPG Noise to Clinical Signal: The Hardware Hurdle
To understand how we get to a “threefold risk” prediction, we have to gaze at the sensor stack. Most wearables rely on Photoplethysmography (PPG)—those green LEDs on the back of your watch that measure blood volume changes by bouncing light off your skin. While efficient, PPG is notoriously noisy. Motion artifacts—the simple act of waving your arm—can create “false positives” that mimic the irregular rhythm of AFib.

The real heavy lifting now happens at the edge. Modern wearables are deploying dedicated NPUs (Neural Processing Units) to handle the signal processing locally. Instead of sending raw data to the cloud, the device uses on-device inference to filter out the noise in real-time. This allows the watch to distinguish between a genuine arrhythmia and a vigorous workout. When this is paired with a single-lead ECG (Electrocardiogram) for verification, the device transforms from a gadget into a diagnostic tool.
The engineering challenge is power efficiency. Running a continuous heart-rate variability (HRV) monitor requires a delicate balance of ARM-based low-power cores and high-performance bursts for analysis. If the SoC (System on a Chip) drains the battery in six hours, the longitudinal data—the history of your heart’s behavior over months—is lost. And in cardiology, the trend is more important than the snapshot.
The Predictive Pivot: Why Detection Isn’t Enough
Detection is binary: you have AFib or you don’t. Prediction is probabilistic. The recent link between screening-detected AFib and a surge in heart failure risk suggests that the “silent” nature of these episodes is the primary danger. Many patients are asymptomatic until the heart’s left ventricle begins to fail.
This is where the “Information Gap” lies. The industry is currently obsessed with detection, but the value is in prognosis. By analyzing the duration, frequency, and morphology of AFib episodes, AI models can now identify patterns that correlate with heart failure long before a patient feels short of breath. This involves analyzing “parameter scaling” within Large Language Models (LLMs) and specialized medical AI that can ingest millions of hours of ECG data to find the subtle signatures of myocardial stress.
“The shift we’re seeing is the move from ‘snapshot diagnostics’ to ‘continuous surveillance.’ The goal isn’t to tell a user they have an irregular heartbeat today, but to identify the subtle degradation of cardiac efficiency over a six-month window.” — Dr. Aris Thorne, Lead Systems Architect at BioDigital Health.
This predictive capability effectively turns the wearable into a remote triage system. Instead of a patient arriving at the ER in full heart failure, the system triggers a clinical intervention when the risk probability hits a specific threshold.
The Health Moat: Platform Lock-in via Longitudinal Data
Beyond the medicine, there is a brutal market dynamic at play. We are witnessing the construction of the ultimate “Health Moat.” When your Apple Watch or Samsung Galaxy Watch holds five years of your cardiac history, the switching cost to a competitor becomes astronomical. You aren’t just switching hardware; you are deleting your medical baseline.
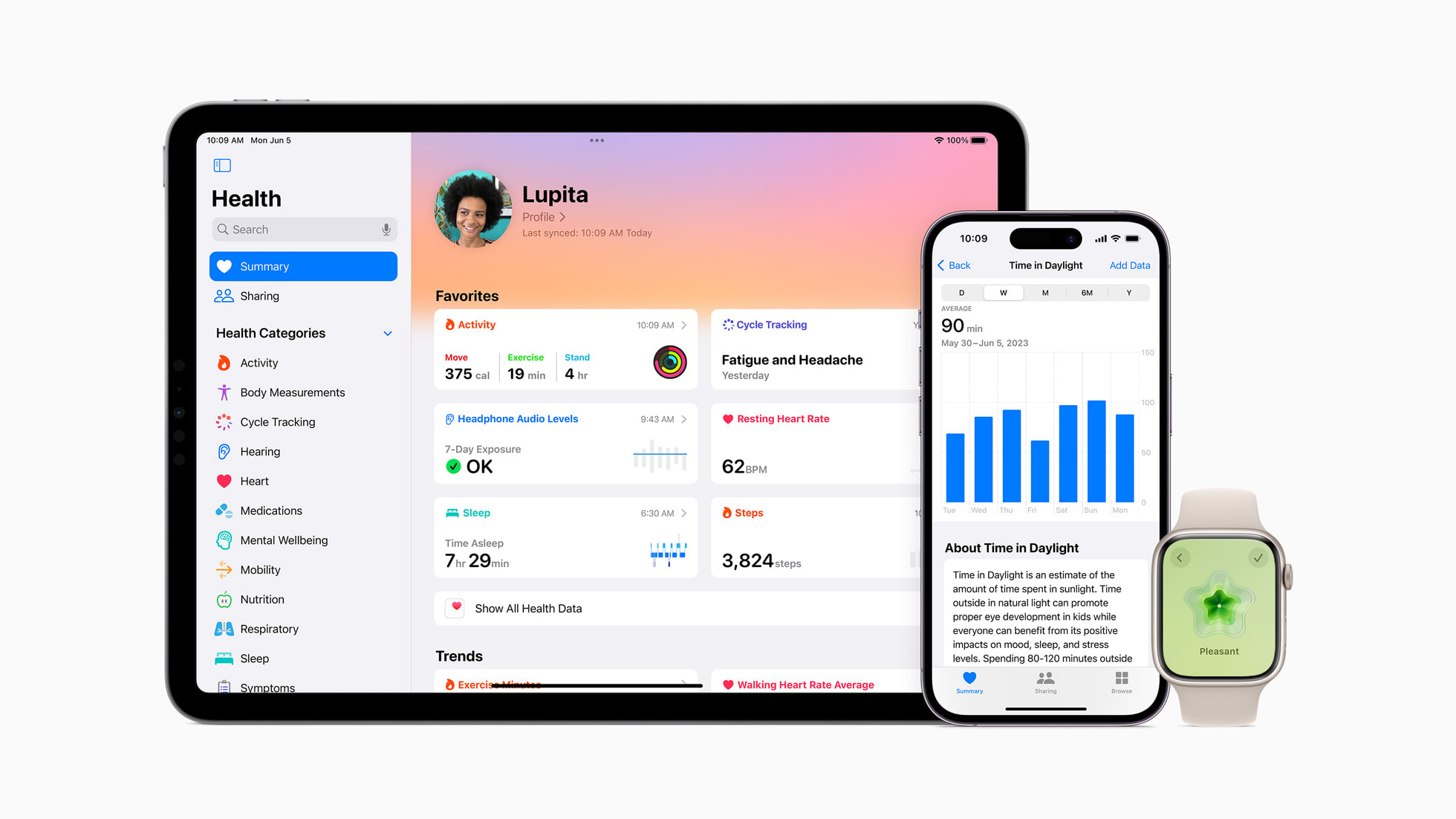
This creates a closed-loop ecosystem. Apple, Google (via Fitbit), and Samsung are racing to integrate this data into a broader “Health OS.” By owning the data pipeline—from the PPG sensor to the encrypted cloud storage—these companies are positioning themselves as the primary interface between the patient and the physician.
- Data Siloing: Proprietary formats make it tricky to export high-resolution ECG data to third-party researchers.
- API Restrictions: While Apple HealthKit and Google Health Connect provide some access, the most granular “raw” sensor data remains locked.
- Regulatory Capture: By securing FDA clearances for specific features, big tech creates a barrier to entry for smaller startups that cannot afford the multi-million dollar clinical trial process.
The 30-Second Verdict for the Tech-Savvy
The “threefold risk” finding validates the move toward continuous monitoring. For the user, this means more accurate warnings. For the industry, it means the transition of wearables from “accessories” to “essential medical infrastructure.” Expect future SoC updates to prioritize NPU performance specifically for bio-signal processing.
The Signal-to-Noise Crisis in Digital Triage
However, we must address the “Cyber-Medical” risk. As these devices become more sensitive, the risk of “over-diagnosis” increases. If a watch flags a minor irregularity as a high risk for heart failure, we risk flooding cardiology clinics with the “worried well,” creating a bottleneck in healthcare delivery.
the security of this data is paramount. Heart failure risk profiles are the ultimate piece of PII (Personally Identifiable Information). If leaked, this data could theoretically be used by insurance providers to adjust premiums dynamically—a dystopian scenario where your hardware betrays your biology to your underwriter.
To mitigate this, we are seeing a push toward end-to-end encryption (E2EE) for health data and the implementation of IEEE standards for medical device interoperability. The goal is to ensure that while the AI can analyze the data, the raw biological markers remain under the user’s control.
The future of cardiology isn’t in the clinic; it’s on the wrist. But as we bridge the gap between consumer electronics and life-saving diagnostics, the industry must prioritize data transparency over platform lock-in. The tech is finally here—now we just need the ethics to match the engineering.

