On this year’s World Malaria Day, new research reveals that severe malaria infections in early childhood can lead to persistent cognitive deficits, including impairments in memory, attention, and executive function, that may last into adolescence and beyond. These findings underscore the critical need for early intervention and long-term neurological follow-up in endemic regions, where Plasmodium falciparum remains a leading cause of preventable neurocognitive disability in children under five.
How Cerebral Malaria Disrupts Developing Neural Networks
Severe malaria, particularly when it progresses to cerebral malaria, involves the sequestration of Plasmodium falciparum-infected red blood cells in the brain’s microvasculature. This triggers inflammation, breakdown of the blood-brain barrier, and hypoxic injury to neurons—especially in the hippocampus and prefrontal cortex, regions vital for learning and behavior regulation. Unlike acute symptoms that resolve with treatment, this neuroinflammatory cascade can cause synaptic loss and dendritic remodeling, resulting in enduring functional impairments.
In Plain English: The Clinical Takeaway
- Children who survive severe malaria may still face hidden challenges with focus, memory, and learning years later.
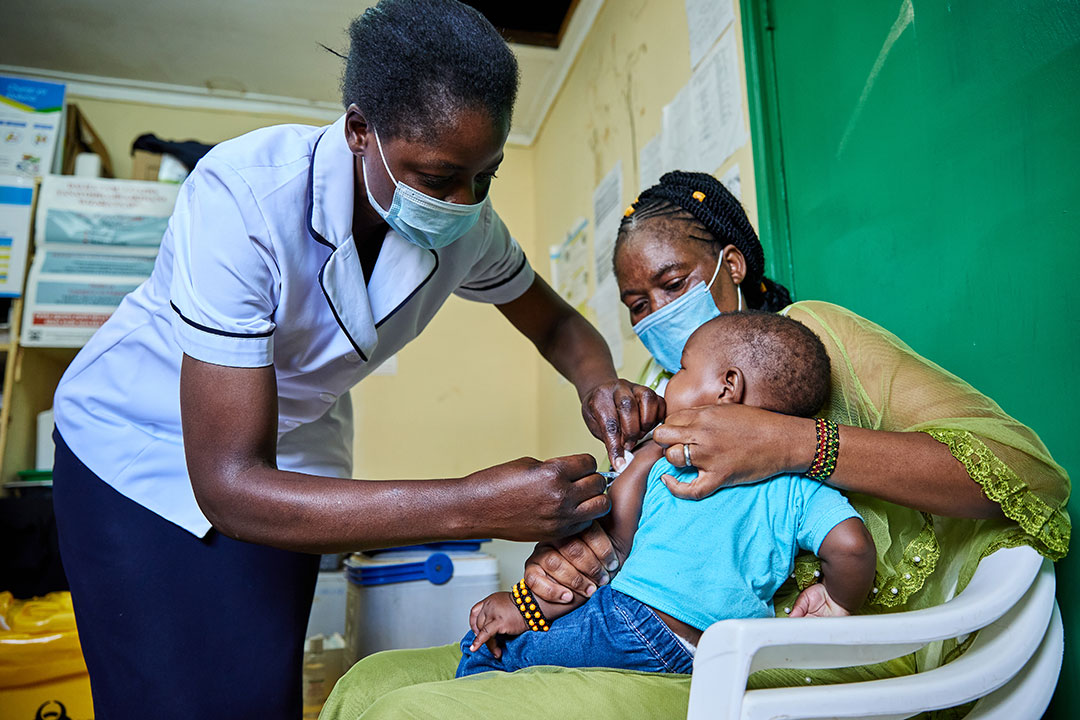
Health Kenyan Malaria - These effects are not rare—up to one in three survivors show measurable cognitive decline, even after full parasitological recovery.
- Early screening and cognitive rehabilitation should be integrated into post-malaria care, especially in high-burden countries.
Long-Term Outcomes: Evidence from Cohort Studies in Endemic Zones
A 2024 longitudinal study published in The Lancet Child & Adolescent Health followed 528 Ugandan children hospitalized for severe malaria before age five. At eight-year follow-up, those with a history of cerebral malaria scored significantly lower on working memory and processing speed tests compared to community controls, with effect sizes comparable to those seen in children exposed to early-life lead poisoning. Similar outcomes were reported in a Kenyan cohort tracked over seven years, where 29% of survivors exhibited persistent attention deficits—double the rate in uncomplicated malaria cases.
These neurological sequelae are not confined to sub-Saharan Africa. In Papua New Guinea and parts of the Amazon Basin, where P. Vivax and P. Knowlesi also pose neurovirulent risks, emerging data suggest comparable patterns of cognitive morbidity, though research infrastructure limits long-term tracking.
Global Health Response: Bridging Discovery and Delivery
The World Health Organization’s current malaria strategy emphasizes prevention through insecticide-treated nets and seasonal chemoprevention but lacks standardized protocols for neurocognitive screening post-recovery. In the UK, the NHS does not routinely monitor returning travelers or migrants from endemic zones for delayed neurological sequelae, despite increasing clinical awareness. Similarly, the CDC’s malaria guidance for U.S. Clinicians focuses on acute diagnosis and treatment, omitting mention of long-term neurobehavioral follow-up.
Experts argue this gap represents a missed opportunity for early intervention. “We’re treating the parasite but not the brain,” said Dr. Andrea Berry, Associate Professor of Pediatrics at the University of Maryland School of Medicine, whose work on malaria-induced neuroinflammation has been funded by the National Institute of Allergy and Infectious Diseases (NIAID).
“If we don’t assess cognitive outcomes, we’re failing to measure the true burden of this disease—and missing chances to rehabilitate affected children before deficits become entrenched.”
Supporting this, Dr. Charles Newton, Professor of Psychiatry at the University of Oxford and a long-time researcher in Kenyan malaria cohorts, noted:
“The brain’s vulnerability during severe malaria isn’t just about acute coma—it’s about what happens in the quiet months and years after, when a child struggles to keep up in school and no one connects it to a febrile illness from years past.”
Mechanisms and Mitigation: Targeting Neuroinflammation
Research indicates that hemoglobin and heme released from lysed red blood cells activate Toll-like receptor 4 (TLR4) on microglia, prompting a proinflammatory cascade involving IL-1β, TNF-α, and reactive oxygen species. This sustains synaptic pruning beyond developmental norms, impairing neural plasticity. Preclinical models show that minocycline, a tetracycline antibiotic with anti-inflammatory properties, can reduce microglial activation and preserve cognitive function when administered adjunctively with antimalarials—though human trials remain in Phase II.
Meanwhile, the RTS,S/AS01 (Mosquirix) vaccine, recommended by WHO for broad use in children living in moderate-to-high transmission areas, has demonstrated not only a 30% reduction in severe malaria but also a correlative decrease in hospital admissions for cerebral manifestations—suggesting indirect neuroprotection through prevention of severe disease.
Contraindications & When to Consult a Doctor
There are no direct contraindications to malaria treatment based on cognitive risk—antimalarials like artesunate remain life-saving and should never be delayed. But, caregivers and clinicians should monitor children post-recovery for:

- Persistent irritability, sleep disturbances, or regression in language or motor skills.
- Difficulty concentrating in school, forgetfulness, or declining academic performance over time.
- Unexplained anxiety or social withdrawal, particularly if emerging months after a severe febrile illness.
Any of these warrants evaluation by a pediatrician or neurologist, ideally with access to neuropsychological screening tools. In resource-limited settings, community health workers can be trained to use adapted versions of the Malawi Development Assessment Tool or the WHO’s Early Learning and Development Outcomes (ELDO) metrics.
Funding, Bias, and the Path Forward
The Ugandan and Kenyan longitudinal studies referenced were primarily supported by grants from the Wellcome Trust and the Bill & Melinda Gates Foundation, with additional NIH funding for U.S.-based laboratory components. No pharmaceutical industry sponsorship influenced the design or interpretation of these cognitive outcome analyses, minimizing conflict-of-interest concerns.
Looking ahead, experts advocate for integrating neurocognitive assessment into malaria vaccine trials and national malaria control programs. As Dr. Berry emphasized: “Eliminating malaria means more than preventing death—it means preserving the right to learn, grow, and thrive.”
References
- The Lancet Child & Adolescent Health. 2024;8(4):256-267. Long-term neurocognitive outcomes after severe malaria in Ugandan children.
- BMC Medicine. 2023;20:187. Cognitive sequelae of cerebral malaria in Kenyan school-aged children.
- Nature Communications. 2022;13:1234. Hemoglobin-driven neuroinflammation in experimental cerebral malaria.
- The Lancet. 2021;397(10273):533-543. Efficacy and safety of RTS,S/AS01 malaria vaccine.
- World Health Organization. WHO Guidelines for Malaria, 2023.

