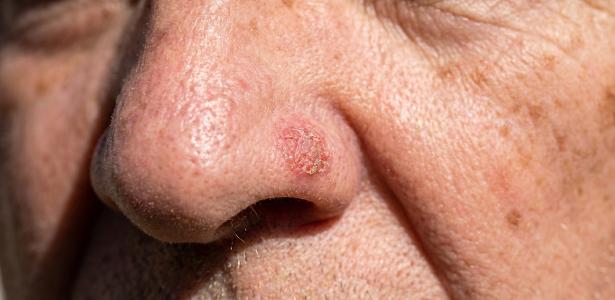
While melanoma is the most aggressive skin cancer, Squamous Cell Carcinoma (SCC) also possesses metastatic potential, meaning it can spread to lymph nodes and distant organs. Early detection by dermatologists and trained beauty professionals is critical to reducing mortality rates across all skin cancer types, regardless of their classification.
For decades, public health messaging has focused almost exclusively on the “deadly” nature of melanoma, leaving a dangerous gap in patient awareness. This narrative has inadvertently created a false sense of security regarding Non-Melanoma Skin Cancers (NMSC). While Basal Cell Carcinoma (BCC) rarely spreads, Squamous Cell Carcinoma (SCC) can be lethal if neglected. Understanding the nuances of these malignancies is not about inciting panic, but about refining triage and screening protocols to ensure that “less aggressive” labels do not lead to clinical complacency.
In Plain English: The Clinical Takeaway
- Not all skin cancers are the same: Basal Cell is slow and stays local; Melanoma is fast and aggressive; Squamous Cell is in the middle but can still spread.
- The “Safe” Myth: Do not assume a non-melanoma growth is harmless; some can travel to the lymph nodes if not treated early.
- Detection is Key: Any sore that doesn’t heal or a growth that changes shape requires a professional biopsy, not just a visual check.
The Molecular Mechanism of Metastasis in Squamous Cell Carcinoma
To understand how a skin cancer “spreads,” we must examine the mechanism of action—the specific biological process—of metastasis. In the case of Squamous Cell Carcinoma (SCC), the cancer begins in the keratinocytes of the epidermis. For a tumor to metastasize, it must undergo a process called Epithelial-Mesenchymal Transition (EMT). In plain English, This represents when stationary skin cells transform into a more mobile, invasive state, allowing them to break through the basement membrane (the thin layer separating the epidermis from the dermis).
Once these cells breach the basement membrane, they gain access to the lymphatic system and blood vessels. From here, they can migrate to regional lymph nodes or distant organs, such as the lungs. While the statistical probability of SCC metastasis is significantly lower than that of melanoma—estimated at roughly 2% to 5% in the general population—this risk spikes dramatically in immunocompromised patients, such as organ transplant recipients who take lifelong immunosuppressant drugs to prevent organ rejection.
Research published in PubMed indicates that the loss of the p53 tumor suppressor protein is a primary driver in this transition, effectively removing the “brakes” that normally prevent a cell from dividing uncontrollably, and migrating.
Geo-Epidemiological Bridging: Global Standards of Care
The approach to skin cancer screening varies significantly by region, often reflecting the local UV index and healthcare infrastructure. In the United States, the FDA has accelerated the approval of topical immunotherapies and targeted biologics for advanced SCC, focusing on the PD-1/PD-L1 pathway (a mechanism that helps the immune system “see” and attack cancer cells). In contrast, the UK’s National Health Service (NHS) emphasizes a rigorous primary-care referral system to ensure early surgical excision, which remains the gold standard for preventing spread.
In regions with high solar radiation, such as Australia and Brazil, there is an increasing movement to integrate “non-clinical” allies into the detection pipeline. As noted in recent community health initiatives, beauty professionals—estheticians and nail technicians—are being trained to identify suspicious lesions. This is a strategic public health move to create a wider “net” for early detection, as these professionals often see a patient’s skin more frequently than a primary care physician does.
“The integration of non-medical health screeners into the dermatological pathway is not a replacement for clinical diagnosis, but a critical triage layer. In high-risk populations, the time between the appearance of a lesion and the first biopsy is the single most important variable in survival rates.” — Dr. Sarah Thompson, Epidemiologist specializing in cutaneous malignancies.
Comparative Analysis of Skin Cancer Pathologies
To clarify the distinctions between the three primary types of skin cancer, the following data summarizes their behavior and risk profiles based on current clinical consensus.
| Cancer Type | Primary Origin | Metastatic Potential | Primary Driver | Typical Presentation |
|---|---|---|---|---|
| Basal Cell (BCC) | Basal cells | Extremely Low | Chronic UV exposure | Pearly bump, non-healing sore |
| Squamous Cell (SCC) | Keratinocytes | Moderate (Higher if immunosuppressed) | Cumulative UV exposure | Scaly red patch, firm nodule |
| Melanoma | Melanocytes | High | Intense/Intermittent UV (burns) | Irregular mole, asymmetry |
Funding, Bias, and Journalistic Transparency
It’s essential to note that much of the research regarding NMSC is funded through a combination of government grants (such as the National Institutes of Health in the US) and private funding from dermatological pharmaceutical firms. While these studies are typically subject to double-blind placebo-controlled trials—meaning neither the patient nor the doctor knows who is receiving the treatment to prevent bias—readers should remain aware that industry-funded research may emphasize the efficacy of new drug therapies over simpler, surgical interventions.
However, the consensus across the World Health Organization (WHO) and the CDC remains clear: surgical excision is the most effective first-line treatment for localized SCC and BCC. The move toward systemic therapies is reserved for cases where the cancer has already metastasized or is unresectable.
Contraindications & When to Consult a Doctor
While self-monitoring is encouraged, it is not a substitute for clinical diagnosis. Try to seek immediate medical intervention if you notice any of the following “red flags”:
- The Non-Healing Wound: Any sore or ulcer that does not heal within three weeks.
- Rapid Growth: A nodule or scale that grows noticeably over a period of a few months.
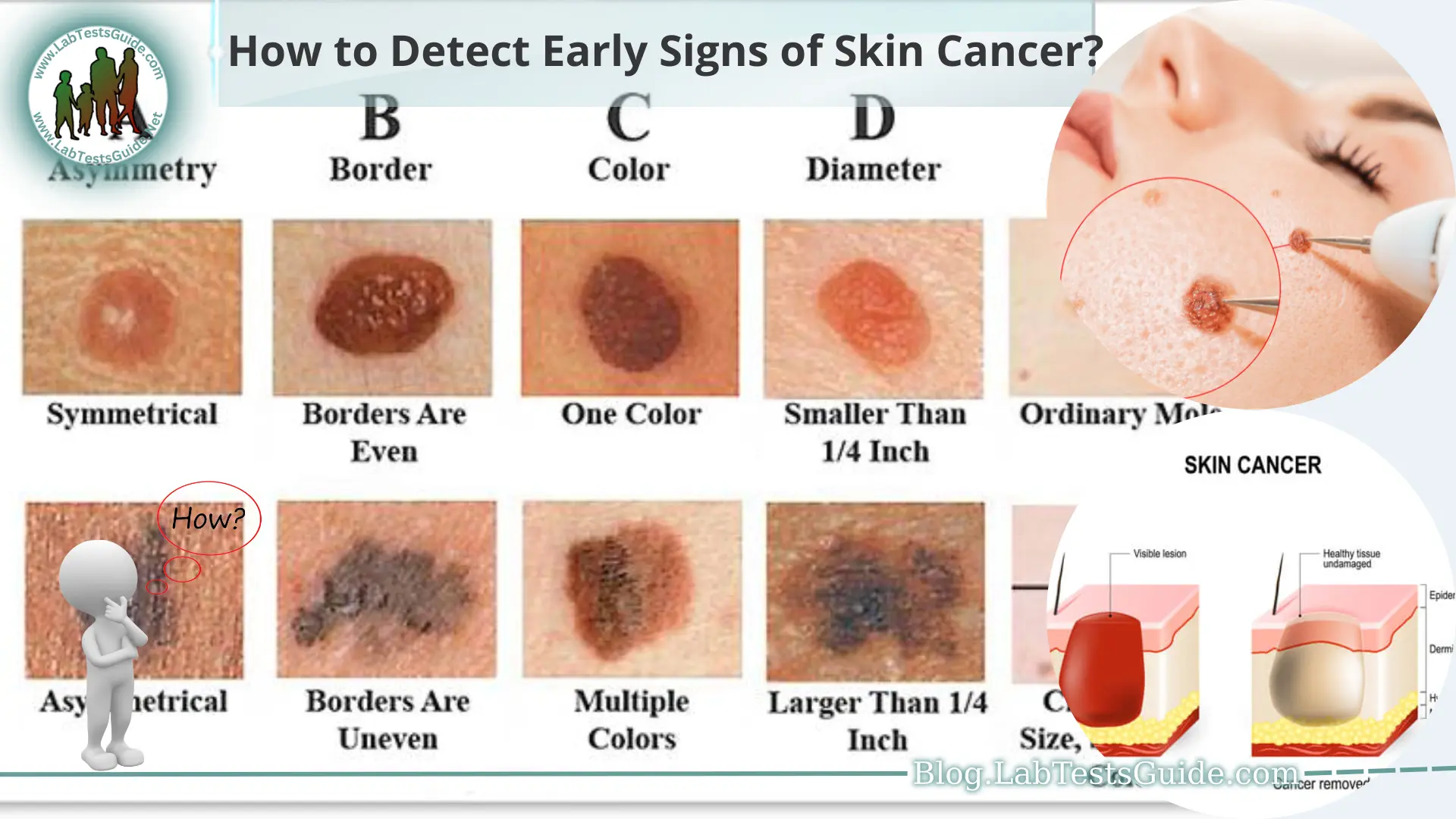
- The ABCDE Shift: In the case of moles, look for Asymmetry, irregular Borders, Color changes, Diameter larger than 6mm, and Evolving shape.
- Bleeding or Crusting: Lesions that bleed spontaneously or develop a “horn-like” crust.
Contraindications for Home Treatment: Never attempt to “freeze” or chemically peel a suspicious growth using over-the-counter kits. This can destroy the surface tissue, making it impossible for a pathologist to determine the cancer’s depth (Breslow thickness) during a biopsy, which is the primary metric used to decide if lymph node surgery is necessary.
The trajectory of skin cancer treatment is moving toward personalized medicine, utilizing genomic sequencing to identify exactly which mutation is driving a tumor’s growth. While the fear of metastasis is real, the clinical reality is optimistic: when caught in the localized stage, the cure rate for nearly all skin cancers exceeds 90%. Vigilance, not panic, is the most effective tool in your medical arsenal.