Maternal exhaustion is a systemic public health crisis characterized by chronic sleep deprivation and psychosocial burnout. It extends beyond simple fatigue, impairing neurological function and increasing the risk of postpartum mood disorders. Addressing this requires structural support systems—not just individual “rest”—to ensure the long-term health of both mother and infant.
The narrative surrounding Mother’s Day often pivots toward sentimental gifts, yet the clinical reality for millions of women is a state of profound physiological and psychological depletion. This is not a failure of personal resilience, but a predictable biological response to the “invisible load”—the cognitive labor of managing a household and childcare without adequate systemic support. When we discuss maternal burnout, we are discussing a state of allostatic load, where the body’s stress response systems are pushed beyond their capacity to maintain stability, leading to systemic wear and tear.
In Plain English: The Clinical Takeaway
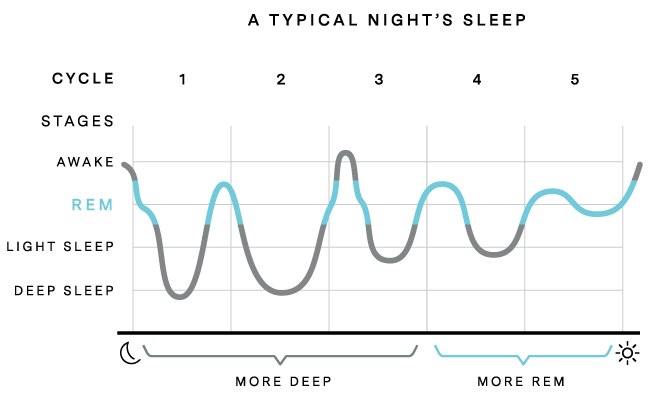
- Sleep Fragmentation is Not Just Tiredness: Waking up every few hours prevents the brain from completing deep REM cycles, which are essential for emotional regulation and memory.
- Support is Medicine: Clinical outcomes improve more significantly when a mother has consistent help with daily chores and childcare than when she is given a one-time “spa day” or occasional nap.
- Burnout vs. Depression: While they overlap, burnout is a response to an unsustainable environment; postpartum depression is a clinical mood disorder. Both require different, though often complementary, medical interventions.
The Neurobiology of the ‘Invisible Load’ and Sleep Fragmentation
To understand why “rest” is an insufficient gift, we must examine the mechanism of action of sleep deprivation on the maternal brain. Chronic sleep fragmentation—the interruption of sleep cycles—disrupts the communication between the prefrontal cortex (the area responsible for executive function and impulse control) and the amygdala (the brain’s emotional processing center). In a rested state, the prefrontal cortex exerts “top-down” inhibition on the amygdala. However, under the weight of chronic exhaustion, this connection weakens.
The result is an intensified emotional response to minor stressors, often mischaracterized as “moodiness” or “hormonal instability.” In reality, We see a neurological failure to regulate affect. The Hypothalamic-Pituitary-Adrenal (HPA) axis, which governs the body’s response to stress, becomes dysregulated. This leads to abnormal cortisol secretion patterns, which can cause systemic inflammation and metabolic dysfunction, potentially exacerbating postpartum weight retention and insulin resistance.
Research published in PubMed indicates that prolonged sleep restriction impairs glucose metabolism and increases the risk of metabolic syndrome. This creates a vicious cycle: the mother is too exhausted to maintain nutritional health, and the resulting metabolic instability further degrades her energy levels and mental clarity.
Geo-Epidemiological Disparities in Maternal Support
The severity of maternal burnout is not distributed equally; it is heavily influenced by regional healthcare policies and social safety nets. In the United States, the lack of federally mandated paid family leave creates a “pressure cooker” environment where women are forced to return to the workforce while still in the acute phase of sleep deprivation. This differs sharply from the Nordic model—seen in countries like Sweden and Norway—where extensive paid leave and subsidized childcare act as a clinical intervention, reducing the incidence of postpartum depression (PPD).
In Brazil and other emerging economies, the challenge is often the “support paradox.” While extended family networks may be present, the cognitive load of managing those networks—and the societal expectation that motherhood should be “natural” and “effortless”—often prevents women from seeking professional psychological help until they reach a crisis point. The World Health Organization (WHO) has emphasized that maternal mental health is a global priority, yet access to perinatal psychiatric care remains fragmented across the Global South.
“The clinical manifestation of maternal burnout is often a mirror of the societal failures surrounding the mother. We cannot treat the individual patient without treating the environment that is depleting her.” — Dr. Elena Rossi, Lead Researcher in Perinatal Psychiatry.
Comparing Acute Fatigue and Chronic Maternal Burnout
It is critical to distinguish between the expected tiredness of early parenthood and the clinical state of burnout. The following table summarizes the physiological and psychological markers used to differentiate these states.
| Marker | Acute Sleep Deprivation | Chronic Maternal Burnout |
|---|---|---|
| Cognitive Function | Mild brain fog; temporary forgetfulness. | Severe executive dysfunction; inability to plan. |
| Emotional State | Irritability that resolves with sleep. | Emotional detachment or persistent anhedonia. |
| Physical Response | Physical tiredness; drowsiness. | Chronic fatigue unresponsive to sleep; somatic pain. |
| HPA Axis Status | Reactive cortisol spikes. | Blunted cortisol response or chronic hypercortisolemia. |
| Intervention | Short-term restorative sleep. | Systemic restructuring of support and therapy. |
Funding, Bias, and the Commercialization of ‘Self-Care’
As a medical journalist, I must highlight a concerning trend: the commercialization of “self-care” as a solution for maternal exhaustion. Many products marketed to “exhausted moms”—from luxury skincare to expensive wellness retreats—are funded by corporate interests that profit from the symptoms of burnout without addressing the cause. These “band-aid” solutions often shift the burden of wellness back onto the mother, implying that if she is still tired, she simply isn’t “practicing self-care” correctly.
True clinical recovery from burnout is not found in a product, but in the redistribution of labor. Evidence-based interventions, such as those outlined by The Lancet, suggest that the most effective “treatment” for maternal burnout is the implementation of shared caregiving models and the reduction of the cognitive load through institutional support.
Contraindications & When to Consult a Doctor
While exhaustion is common, certain symptoms indicate a transition from burnout to a severe clinical disorder. You should seek immediate medical intervention from a licensed psychiatrist or OB-GYN if the following “red flags” appear:
- Intrusive Thoughts: Recurrent, distressing thoughts of harming oneself or the infant.
- Psychosis: Experiencing hallucinations (auditory or visual) or delusions.
- Anhedonia: A complete inability to feel pleasure or bond with the child.
- Severe Sleep Insomnia: The inability to sleep even when the infant is sleeping and support is available (a hallmark of clinical depression).
- Physical Collapse: Fainting episodes, severe tachycardia (rapid heart rate), or unexplained weight loss/gain.
pharmacological interventions, such as SSRIs (Selective Serotonin Reuptake Inhibitors), may be indicated for PPD. However, these should only be administered under strict clinical supervision to monitor for contraindications, especially in breastfeeding mothers, as per CDC and WHO guidelines.
The Path Toward Systemic Recovery
Looking forward, the medical community must move beyond the “rest” narrative. The goal is not to help mothers “cope” with an unsustainable system, but to advocate for systems that are biologically compatible with human motherhood. This includes the integration of mental health screenings into every postpartum check-up and the legislative push for universal paid leave.
Until then, the most evidence-based “gift” for any mother is the active, unprompted assumption of labor. By removing the cognitive burden of planning and executing domestic tasks, we allow the maternal brain the necessary space to move from a state of survival (sympathetic nervous system dominance) to a state of recovery (parasympathetic activation). This is the only sustainable path to maternal wellness.
References
- World Health Organization (WHO). Guide to Maternal Mental Health.
- The Lancet. Series on Perinatal Mental Health and Global Policy.
- American College of Obstetricians and Gynecologists (ACOG). Clinical Guidelines for Postpartum Depression.
- PubMed. Research on Sleep Fragmentation and Prefrontal Cortex Function.
- Centers for Disease Control and Prevention (CDC). Maternal Health and Wellness Statistics.

