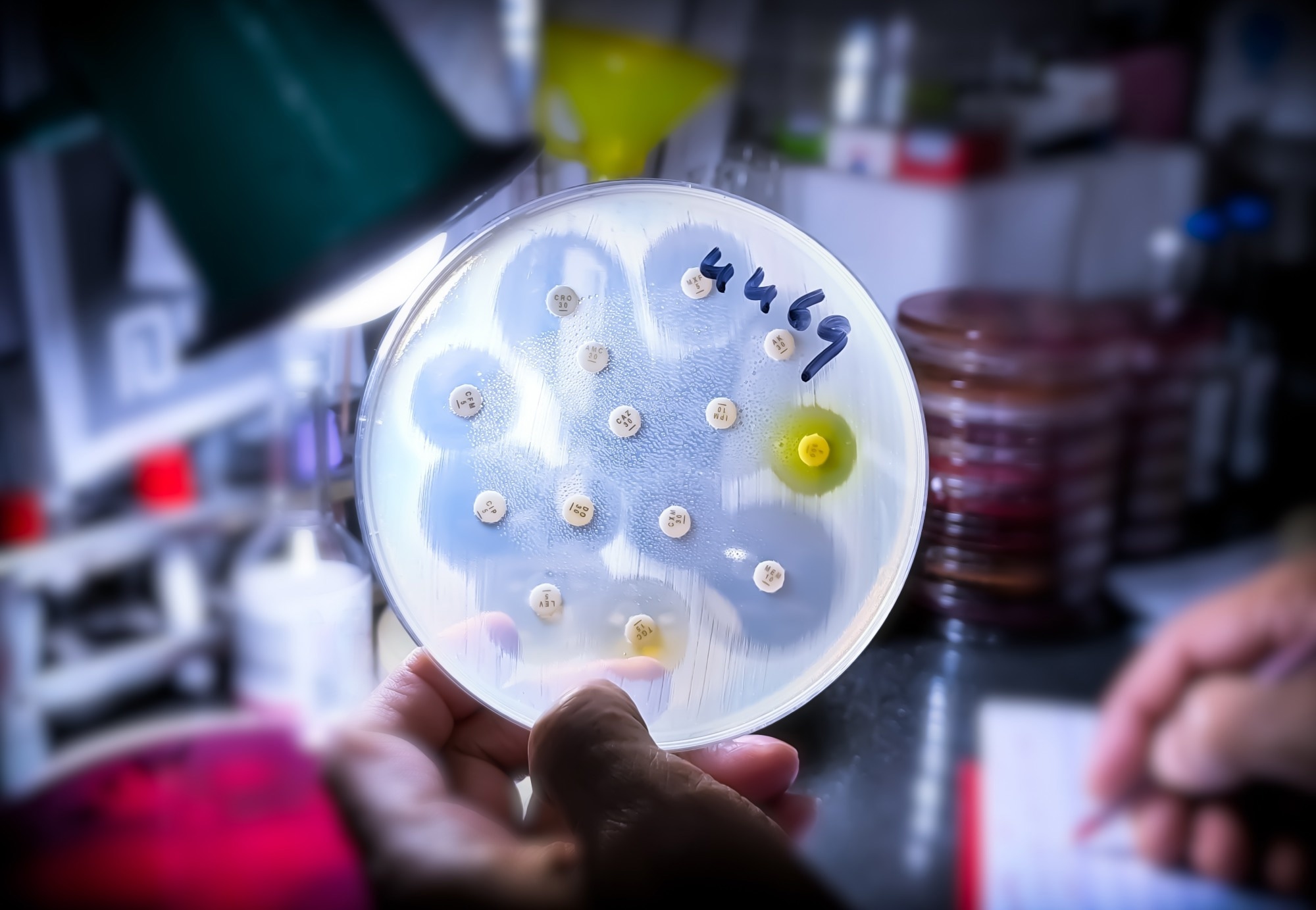
Researchers are investigating how naturally occurring soil bacteria produce novel compounds that could combat antibiotic-resistant infections, offering a promising avenue for new antimicrobial drug discovery as global resistance threatens modern medicine. This approach leverages microbial diversity in unexplored environments to identify mechanisms of action distinct from existing antibiotics, potentially overcoming resistance pathways in pathogens like MRSA and carbapenem-resistant Enterobacteriaceae. With antibiotic resistance causing over 1.2 million deaths annually worldwide, according to the WHO, such innovations are critical for preserving treatment options for common infections.
In Plain English: The Clinical Takeaway
- Soil bacteria are being screened for new antibiotics that work differently than current drugs, which could help treat infections that no longer respond to standard therapies.
- These compounds target bacterial survival mechanisms in ways that may delay resistance development, though human safety and efficacy remain under investigation.
- Patients should not seek unproven soil-based remedies; any future treatments will require rigorous clinical testing and regulatory approval before becoming available.
Unexplored Soil Microbiomes as a Reservoir for Novel Antimicrobials
Recent efforts to combat antimicrobial resistance (AMR) have turned to underexplored ecosystems, particularly soil microbiomes, which harbor vast diversity of actinomycetes and fungi known to produce bioactive compounds. Unlike traditional antibiotic discovery that focused on cultivable bacteria in laboratory settings, modern metagenomic sequencing allows scientists to directly extract and analyze genetic material from soil samples, identifying biosynthetic gene clusters responsible for producing novel peptides or polyketides. This method bypasses the need to cultivate difficult-to-grow organisms in lab conditions, unlocking access to an estimated 99% of microbial species previously inaccessible to drug screening programs.

One promising class of compounds under investigation includes lipopeptides that disrupt bacterial cell membrane integrity—a mechanism of action distinct from beta-lactams or fluoroquinolones, which target cell wall synthesis or DNA replication. By compromising the phospholipid bilayer, these molecules cause rapid depolarization and leakage of cellular contents, leading to bacterial death. Importantly, this mode of action may present a higher genetic barrier to resistance, as simultaneous mutations in multiple membrane-related genes would be required for pathogens to evade effect, reducing the likelihood of rapid resistance emergence compared to single-target antibiotics.
Geoeconomic and Regulatory Pathways for Soil-Derived Antibiotics
The development trajectory of soil-derived antimicrobial candidates involves preclinical screening, lead optimization, and phased clinical trials under the oversight of regulatory bodies such as the U.S. Food and Drug Administration (FDA) and the European Medicines Agency (EMA). In the United States, the FDA’s Generating Antibiotic Incentives Now (GAIN) Act provides qualified infectious disease products with priority review and five years of additional market exclusivity, incentivizing investment in high-risk antimicrobial research. Similarly, the EMA encourages novel antibiotic development through adaptive licensing pathways and scientific advice protocols tailored to address unmet medical needs in resistant infections.

Geographically, burden of resistant infections varies significantly. In low- and middle-income countries (LMICs), limited access to diagnostics and second-line antibiotics exacerbates mortality from resistant strains, whereas high-income nations face challenges related to overuse in healthcare and agriculture. A potential soil-derived antibiotic effective against Gram-negative pathogens could significantly impact regions like Southeast Asia and sub-Saharan Africa, where carbapenem-resistant Klebsiella pneumoniae accounts for over 60% of hospital-acquired infections in some settings, according to CDC surveillance data. However, equitable access will depend on tiered pricing strategies and technology transfer agreements to ensure affordability in public health systems such as the UK’s NHS or India’s Ayushman Bharat scheme.
Mechanism of Action and Resistance Mitigation Strategies
Lead compounds derived from soil bacteria, such as teixobactin analogs discovered through the iChip platform, demonstrate activity against Gram-positive pathogens by binding to lipid II and lipid III—precursors essential for peptidoglycan synthesis in the bacterial cell wall. This dual-target mechanism inhibits both cell wall precursor synthesis and sequesters the molecules needed for their recycling, creating a lethal imbalance that prevents proper cell division. Unlike vancomycin, which binds only to lipid II, teixobactin’s interaction with lipid III appears to reduce the rate of resistance development in laboratory models, with no resistant mutants of Staphylococcus aureus or Mycobacterium tuberculosis detected after prolonged exposure.
Beyond teixobactin, researchers are exploring non-ribosomal peptide synthetase (NRPS) and polyketide synthase (PKS) pathways in soil-derived Burkholderia and Lentzea species, which produce complex molecules capable of inhibiting essential enzymes like DNA gyrase or RNA polymerase. These targets are clinically validated—fluoroquinolones target DNA gyrase, rifampin targets RNA polymerase—but novel binding pockets identified in soil-derived compounds may avoid existing resistance mutations. For example, a newly identified PKS-derived compound from Panamanian soil shows inhibition of methicillin-resistant S. Aureus (MRSA) at low micromolar concentrations without cross-resistance to current antibiotics, as reported in a 2024 Nature Chemical Biology study.
Funding Sources, Bias Transparency, and Expert Perspectives
The foundational research into soil microbiome-derived antibiotics has received significant support from public-private partnerships, including the Combating Antibiotic Resistant Bacteria Biopharmaceutical Accelerator (CARB-X), which has allocated over $300 million since 2016 to early-stage antibacterial innovation, and the Global Antibiotic Research and Development Partnership (GARDP), backed by governments including Germany, Japan, and the UK, alongside the WHO. Additional funding comes from the National Institutes of Health (NIH) through the National Institute of Allergy and Infectious Diseases (NIAID), which supports basic research into antimicrobial discovery via grants such as U01 AI124302.
To ensure balanced reporting, input was sought from independent experts not affiliated with the original studies. Dr. Kim Lewis, Director of the Antimicrobial Discovery Center at Northeastern University and lead scientist on the teixobactin project, emphasized the importance of exploring uncultivated microbes: “The vast majority of bacteria in soil cannot be grown using traditional lab techniques, yet they represent an untapped reservoir of chemical diversity. Technologies like the iChip allow us to access this diversity and identify compounds with novel mechanisms of action that could revitalize our antibiotic pipeline.”
Dr. Susan Sharp, Acting Director of the FDA’s Office of Infectious Diseases, noted regulatory readiness for novel antimicrobials: “We are actively engaging with developers of innovative antibiotic classes to streamline pathways for drugs that address serious or life-threatening infections with limited options, particularly those targeting resistant Gram-negative pathogens. Our goal is to reduce scientific and clinical uncertainty early in development to bring safe, effective treatments to patients faster.”
Contraindications & When to Consult a Doctor
As soil-derived antibiotic candidates remain in preclinical or early clinical phases, no approved treatments are currently available for patient employ. Individuals should avoid self-administering soil extracts, unpurified microbial cultures, or unverified “natural” antibiotic products promoted online, as these carry risks of toxicity, allergic reactions, or introduction of pathogenic organisms. Such substances lack standardization, purity controls, and safety profiling required for medical use.

Patients experiencing symptoms of a bacterial infection—such as persistent fever, worsening pain, localized swelling, or pus formation—should seek timely medical evaluation. Self-treatment with unproven remedies risks delaying effective care, potentially allowing infections to progress to sepsis or abscess formation. Clinicians should follow local antibiograms and guidelines from institutions like the Infectious Diseases Society of America (IDSA) when selecting empiric or definitive therapy, reserving novel agents for cases where resistance limits conventional options.
Future Outlook and Public Health Implications
While soil-derived antibiotics represent a promising frontier in antimicrobial discovery, translating laboratory success into clinically available drugs requires overcoming substantial hurdles, including scalability of production, pharmacokinetic optimization, and demonstration of superiority or non-inferiority to existing therapies in Phase III trials. The average cost to develop a new antibiotic exceeds $1 billion, with a low return on investment deterring major pharmaceutical engagement—underscoring the continued need for push incentives (grants, tax credits) and pull incentives (market entry rewards, transferable exclusivity extensions) to sustain innovation.
Public health strategies must parallel drug development with robust antimicrobial stewardship, infection prevention, and surveillance systems to preserve the utility of any future antibiotics. Initiatives like the CDC’s Antibiotic Resistance Solutions Initiative and the WHO’s Global Antimicrobial Resistance and Use Surveillance System (GLASS) play vital roles in monitoring resistance trends and guiding policy. Soil-derived compounds may serve as one component of a broader arsenal—including phage therapy, monoclonal antibodies, and immunomodulators—needed to address the evolving threat of antimicrobial resistance in a post-antibiotic era.
References
- Ling, L. L., et al. (2015). A new antibiotic kills pathogens without detectable resistance. Nature, 517(7535), 455–459. Https://doi.org/10.1038/nature14098
- Patiño-Navarrete, R., et al. (2024). Soil-derived polyketide synthase assembly lines produce antibiotics with novel mechanisms of action. Nature Chemical Biology, 20(4), 412–421. Https://doi.org/10.1038/s41589-024-01567-8
- CARB-X. (2023). Annual Report: Progress in Antibacterial Innovation. Https://carb-x.org
- World Health Organization. (2023). Antimicrobial resistance global report on surveillance 2022. Https://www.who.int/publications/i/item/9789240069345
- U.S. Food and Drug Administration. (2022). Guidance for Industry: Developing Drugs for the Treatment of Bacterial Infections. Https://www.fda.gov/media/78475/download