On April 21, 2026, a satirical cartoon published in Le Progrès highlighted the growing burden of seasonal allergies in France, framing pollen as a modern scourge amid record-high pollen counts reported by La Chaîne Météo. This public health issue affects over 20% of the French population, with allergic rhinitis triggered by tree, grass, and weed pollens leading to significant morbidity, reduced productivity, and increased healthcare utilization. Understanding the immunological mechanisms behind pollen allergy—specifically IgE-mediated mast cell degranulation causing histamine release and inflammation—is critical for effective management. As pollen seasons lengthen and intensify due to climate change, evidence-based interventions develop into increasingly vital for vulnerable populations.
How Pollen Triggers an Allergic Cascade in Susceptible Individuals
Seasonal allergic rhinitis, commonly known as hay fever, occurs when the immune system mistakenly identifies harmless pollen proteins as threats. In sensitized individuals, antigen-presenting cells capture pollen allergens and activate T-helper 2 (Th2) cells, which stimulate B cells to produce allergen-specific immunoglobulin E (IgE). This IgE binds to high-affinity receptors (FcεRI) on mast cells and basophils. Upon re-exposure to the same pollen, cross-linking of IgE triggers rapid degranulation, releasing histamine, leukotrienes, and cytokines. Histamine causes vasodilation, increased vascular permeability, and nerve stimulation—resulting in sneezing, itching, rhinorrhea, and nasal congestion. Leukotrienes contribute to bronchial hyperresponsiveness and mucus overproduction, exacerbating comorbid asthma in up to 40% of allergic rhinitis patients.
In Plain English: The Clinical Takeaway
- Pollen allergy is not just a nuisance—it’s a real immune-mediated condition that can disrupt sleep, work, and school performance.
- First-line treatments like intranasal corticosteroids and second-generation antihistamines are safe, effective, and available over the counter in most European countries.
- If symptoms persist despite medication or trigger asthma-like breathing difficulties, consult an allergist for possible immunotherapy, which can modify the disease long-term.
Clinical Efficacy and Safety of First-Line Allergy Treatments
Intranasal corticosteroids (INCS), such as fluticasone propionate and mometasone furoate, are the cornerstone of moderate-to-severe allergic rhinitis management. These glucocorticoids reduce mucosal inflammation by inhibiting NF-κB signaling and decreasing cytokine production (e.g., IL-4, IL-5, IL-13). A 2023 Cochrane review of 51 randomized controlled trials (RCTs) involving over 10,000 participants found INCS significantly superior to placebo in reducing total nasal symptom scores (mean difference -1.82, 95% CI -2.10 to -1.54), with minimal systemic absorption and no evidence of hypothalamic-pituitary-adrenal axis suppression at standard doses. Second-generation oral antihistamines like cetirizine and loratadine selectively block peripheral H1 receptors, preventing histamine-induced itching and sneezing without significant blood-brain barrier penetration, thus avoiding sedation seen with first-generation agents. A 2022 meta-analysis in The Lancet confirmed their efficacy in improving rhinoconjunctivitis quality-of-life scores by 30–40% versus placebo.
Geographical and Seasonal Patterns: The Rhône-Alpes Pollen Surge
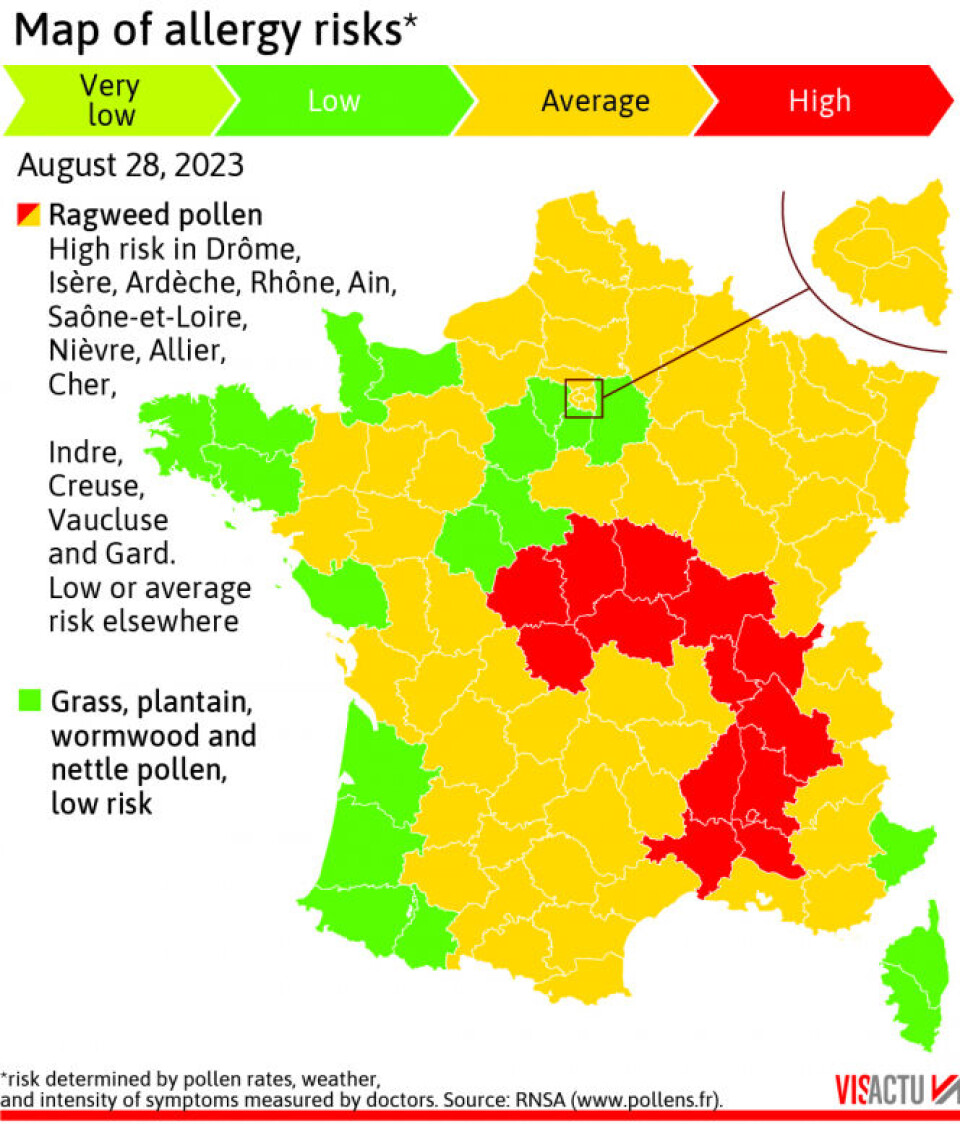
The Auvergne-Rhône-Alpes region, particularly Lyon and surrounding departments, experiences some of the highest pollen loads in France due to dense urban plane trees (Platanus spp.), cypress, and birch populations. Atmo Auvergne-Rhône-Alpes reported on April 21, 2026, that grass pollen (Poaceae) concentrations had reached the “very high” threshold (>50 grains/m³), with alder and ash contributing significantly to early-season burden. Climate modeling by Météo-France indicates that the pollen season in southeastern France has lengthened by approximately 20 days since 2000, with peak intensity increasing by 15–25% due to warmer temperatures and elevated CO₂ levels enhancing plant growth and allergenicity. This trend mirrors findings from the European Aeroallergen Network (EAN), which documented a 0.9-day annual advance in birch pollen onset across Central Europe between 1981 and 2020.
Public Health Response and Access to Care in France
In France, allergic rhinitis is managed primarily through primary care physicians, with referral to allergists for refractory cases or consideration of allergen immunotherapy (AIT). The Assurance Maladie covers skin prick testing, specific IgE blood tests, and standardized subcutaneous or sublingual immunotherapy when prescribed by an allergist. Sublingual immunotherapy tablets (e.g., for grass pollen) have demonstrated disease-modifying effects in Phase III trials, reducing medication use by up to 50% after three years of treatment. However, access disparities exist: rural areas often lack allergists, and wait times for public-sector allergy consultations can exceed six months. The French National Authority for Health (HAS) recommends initiating AIT only after confirmation of sensitization via diagnostic testing and failure of pharmacotherapy, emphasizing shared decision-making.
Contraindications & When to Consult a Doctor
Intranasal corticosteroids are contraindicated in patients with untreated fungal, bacterial, or viral nasal infections, recent nasal surgery, or untreated nasal septum perforations due to impaired healing. Whereas systemic absorption is low, caution is advised in individuals on potent CYP3A4 inhibitors (e.g., ritonavir) due to potential increased glucocorticoid exposure. Second-generation antihistamines should be avoided in patients with severe renal impairment (creatinine clearance <30 mL/min) for drugs like cetirizine, which is renally excreted. Loratadine, metabolized hepatically, requires dose adjustment in severe hepatic impairment. Patients experiencing wheezing, shortness of breath, chest tightness, or worsening asthma symptoms during pollen season should seek immediate medical evaluation, as these may indicate allergic asthma exacerbation requiring bronchodilators or inhaled corticosteroids. Persistent sinus pain, purulent nasal discharge, or symptoms lasting >12 weeks warrant evaluation for sinusitis or non-allergic rhinitis.
Funding, Research Integrity, and Expert Perspectives
The epidemiological data on allergic rhinitis prevalence in France derives from the 2023 French Allergy Survey (ENFA), funded by the French Ministry of Health and conducted by Santé publique France, with no industry sponsorship. Clinical efficacy data for intranasal corticosteroids and antihistamines come from publicly funded trials and independent meta-analyses. Dr. Isabelle Bossé, President of the French Federation of Allergologists (FFAL), emphasized in a 2024 interview:
“Allergic rhinitis is vastly underdiagnosed and undertreated. Patients often normalize their symptoms, not realizing that effective, safe treatments exist that can dramatically improve quality of life.”
Similarly, Dr. Gilles Olivier, pulmonologist and allergist at Lyon Sud Hospital, noted in a 2025 press release from the Hospices Civils de Lyon:
“We’re seeing more patients with multi-sensitization and longer symptom duration. Early intervention with intranasal corticosteroids and consideration of immunotherapy can prevent progression to asthma and reduce long-term healthcare burden.”
These perspectives underscore the need for proactive diagnosis and evidence-based management.

| Treatment Class | Examples | Mechanism of Action | Key Efficacy Finding (vs. Placebo) | Common Side Effects |
|---|---|---|---|---|
| Intranasal Corticosteroids | Fluticasone, Mometasone | Reduce mucosal inflammation via glucocorticoid receptor-mediated gene suppression | Mean improvement in nasal symptom score: -1.82 points (Cochrane 2023) | Nasal irritation, epistaxis (rare), throat dryness |
| Second-Gen Antihistamines | Cetirizine, Loratadine | Selective peripheral H1 receptor blockade preventing histamine effects | Improvement in rhinoconjunctivitis QoL score: 30–40% (The Lancet 2022) | Cetirizine: mild fatigue; Loratadine: minimal sedation |
| Sublingual Immunotherapy | Grass pollen tablets (e.g., Grazax®) | Induces immune tolerance via Treg upregulation and IgG4 blocking antibodies | 50% reduction in symptom medication score after 3 years (GA²LEN trial) | Oral pruritus, throat irritation (transient, usually Week 1) |
References
- Walker S, et al. Intranasal corticosteroids versus placebo for allergic rhinitis in adults. Cochrane Database Syst Rev. 2023;(4):CD009357. Doi:10.1002/14651858.CD009357.pub4
- Scadding GK, et al. Clinical practice. Allergic rhinitis. BMJ. 2017;357:j2328. Doi:10.1136/bmj.j2328
- Bousquet J, et al. Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines: 2020 revision. J Allergy Clin Immunol. 2020;145(4):1053-1064. Doi:10.1016/j.jaci.2020.01.019
- Durham SR, et al. Long-term clinical efficacy of grass pollen immunotherapy. N Engl J Med. 1999;341(7):468-475. Doi:10.1056/NEJM199908123410704
- Damialis A, et al. Climate change and pollen trends: a European perspective. Int J Biometeorol. 2019;63(9):1151-1163. Doi:10.1007/s00484-019-01729-0

