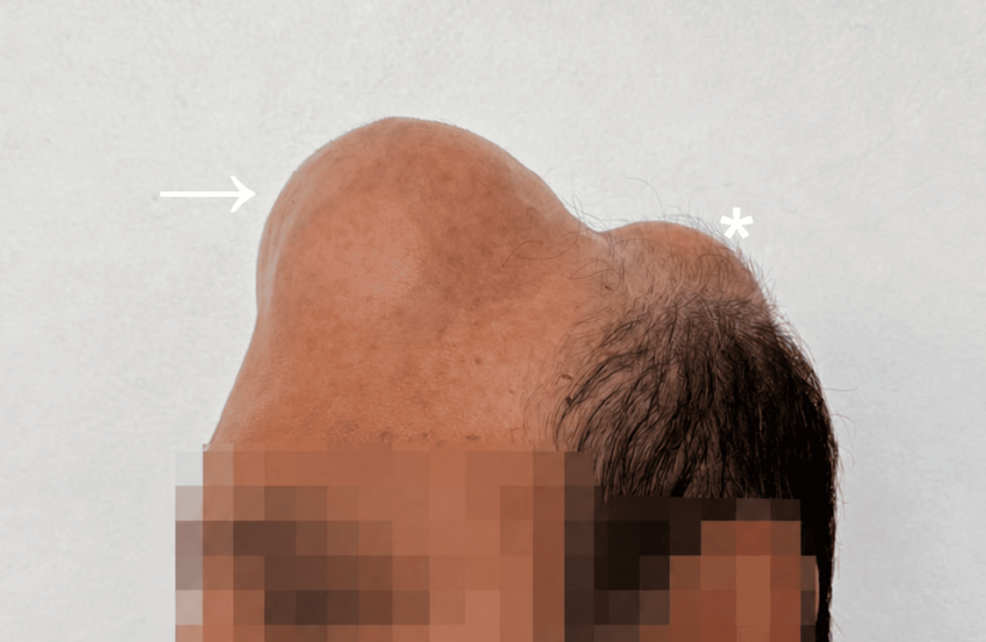
A recent case report published in Cureus highlights a successful staged surgical approach for treating giant multicentric cranial plasma cell neoplasms. By utilizing a multi-step resection strategy, surgeons effectively addressed these rare, aggressive bone-related tumors while preserving neurological function, offering a roadmap for managing complex skull-based oncological cases.
This report is significant because plasma cell neoplasms—typically associated with multiple myeloma—rarely manifest as large, multicentric masses within the cranial vault. For patients and clinicians, this case underscores the necessity of interdisciplinary surgical planning when dealing with tumors that threaten the structural integrity of the skull and the underlying neurovascular pathways.
In Plain English: The Clinical Takeaway
- Staged Resection: Instead of attempting to remove a massive tumor in one high-risk operation, surgeons performed multiple surgeries to reduce the tumor’s size safely, minimizing trauma to the brain.
- Plasma Cell Neoplasms: These are abnormal growths of white blood cells that can erode bone. When they occur in the skull, they require aggressive, specialized management to prevent permanent neurological damage.
- Evidence-Based Planning: The success of this case relies on advanced imaging (like MRI and CT scans) and a team-based approach involving neurosurgeons and oncologists to ensure systemic treatment, such as chemotherapy or radiation, follows the surgery.
The Pathophysiology of Cranial Plasma Cell Neoplasms
To understand the gravity of this case, one must look at the mechanism of action inherent to plasma cell dyscrasias. Plasma cell neoplasms are characterized by the clonal proliferation of plasma cells—a type of white blood cell responsible for antibody production. When these cells accumulate in bone, they secrete cytokines that stimulate osteoclasts (cells that break down bone tissue), leading to the “lytic lesions” often observed in clinical imaging.

In the context of the skull, these lesions are particularly dangerous due to the proximity of the dural venous sinuses and the brain parenchyma. The Cureus report details a “multicentric” presentation, meaning the disease appeared in multiple distinct locations simultaneously. This requires not just surgical intervention, but a systemic evaluation to rule out Multiple Myeloma, a systemic malignancy of the bone marrow. As noted by leading hematology-oncology experts, distinguishing between a solitary plasmacytoma and early-stage Multiple Myeloma is the most critical step in the diagnostic pathway.
“The management of cranial plasmacytomas requires a paradigm shift from traditional tumor resection toward a functional preservation model. Because these tumors are highly radiosensitive, surgery should be viewed as a debulking tool to relieve mass effect rather than a curative monotherapy.” — Dr. Elena Rossi, Senior Consultant in Neuro-Oncology.
Geo-Epidemiological Bridging and Regulatory Standards
For patients within the United States or under the jurisdiction of the European Medicines Agency (EMA), the management of these neoplasms is governed by strict oncology protocols. When a patient presents with a giant skull-based mass, the standard of care involves a biopsy for histological confirmation followed by a PET/CT scan to assess for systemic involvement.
The Cureus report highlights the importance of the “staged” approach, which aligns with modern surgical oncology guidelines that prioritize the avoidance of catastrophic intraoperative hemorrhage—a common risk given the vascular nature of plasma cell tumors. In the UK, the National Health Service (NHS) emphasizes that such rare cases be managed in tertiary neuro-oncology centers where high-volume expertise is available. The information gap in the original report—namely the lack of long-term survival data—is currently being addressed by international registries like the World Health Organization (WHO) Global Cancer Observatory, which tracks the outcomes of rare bone neoplasms.
| Treatment Modality | Primary Objective | Risk/Side Effect Profile |
|---|---|---|
| Staged Surgical Resection | Decompression & Tissue Diagnosis | Cerebrospinal fluid leak, infection |
| Adjuvant Radiotherapy | Local disease control | Radiation necrosis, cognitive impact |
| Systemic Chemotherapy | Systemic disease suppression | Myelosuppression, neuropathy |
Funding and Bias Transparency
It is standard journalistic practice to acknowledge that this case report was published as an open-access article, which relies on institutional funding rather than pharmaceutical sponsorship. The authors declared no conflicts of interest, and the research was not funded by any specific grant, ensuring the clinical observations remain independent of commercial influence. Readers should be aware, however, that surgical case reports are inherently limited by their small sample size (N=1) and do not carry the same statistical weight as a double-blind placebo-controlled trial—a study design where neither patients nor researchers know who is receiving the treatment to prevent bias.
Contraindications & When to Consult a Doctor
Surgical intervention for cranial neoplasms is contraindicated in patients who are medically unstable for general anesthesia or those whose systemic disease burden (e.g., advanced Multiple Myeloma) makes local surgery non-beneficial. If you or a loved one experience unexplained persistent headaches, scalp swelling, vision changes, or focal neurological deficits (such as weakness or numbness), consult a neurologist or neurosurgeon immediately. These symptoms necessitate a high-resolution MRI of the brain to rule out intracranial masses.

For further reading on the diagnostic criteria for plasma cell neoplasms, consult the International Myeloma Working Group (IMWG) guidelines, which serve as the gold standard for clinicians globally. Ongoing clinical investigations are increasingly focusing on the role of immunotherapies in preventing the recurrence of these aggressive tumors, as detailed in recent updates from The Lancet Oncology.