Researchers are targeting “super-enhancers”—overactive DNA regions that fuel cancer growth—to shut down oncogenes with high precision. This approach, currently moving from pre-clinical models to early clinical stages, aims to eliminate tumors while sparing healthy cells, offering a potent alternative to traditional, broad-spectrum chemotherapy.
For decades, oncology has focused on targeting the proteins that drive cancer. Although, proteins are often the end product of a complex assembly line. By targeting super-enhancers, scientists are effectively attacking the “master switch” that controls the entire production line. This shift from protein-centric to regulatory-centric therapy allows clinicians to target “undruggable” oncogenes—proteins that lack a binding site for traditional drugs but are driven by these hyper-active genetic regions.
In Plain English: The Clinical Takeaway
- The “Super-Switch”: Cancer cells create massive clusters of DNA called super-enhancers that force the cell to produce growth proteins at dangerous levels.
- Precision Shutdown: Instead of poisoning all fast-growing cells (like chemo), these new therapies aim to flip the “off” switch only for the cancer’s growth engine.
- Early Stages: While highly promising in mouse studies and early trials, these treatments are not yet standard care and are primarily in the research and clinical trial phases.
The Epigenetic Engine: How Super-Enhancers Drive Malignancy
To understand this breakthrough, we must look at the mechanism of action—the specific biological process by which a drug produces its effect. In a healthy cell, enhancers are short regions of DNA that support turn genes on or off. Super-enhancers (SEs) are abnormally large clusters of these enhancers, densely packed with transcription factors and co-activators like BRD4 (Bromodomain-containing protein 4).
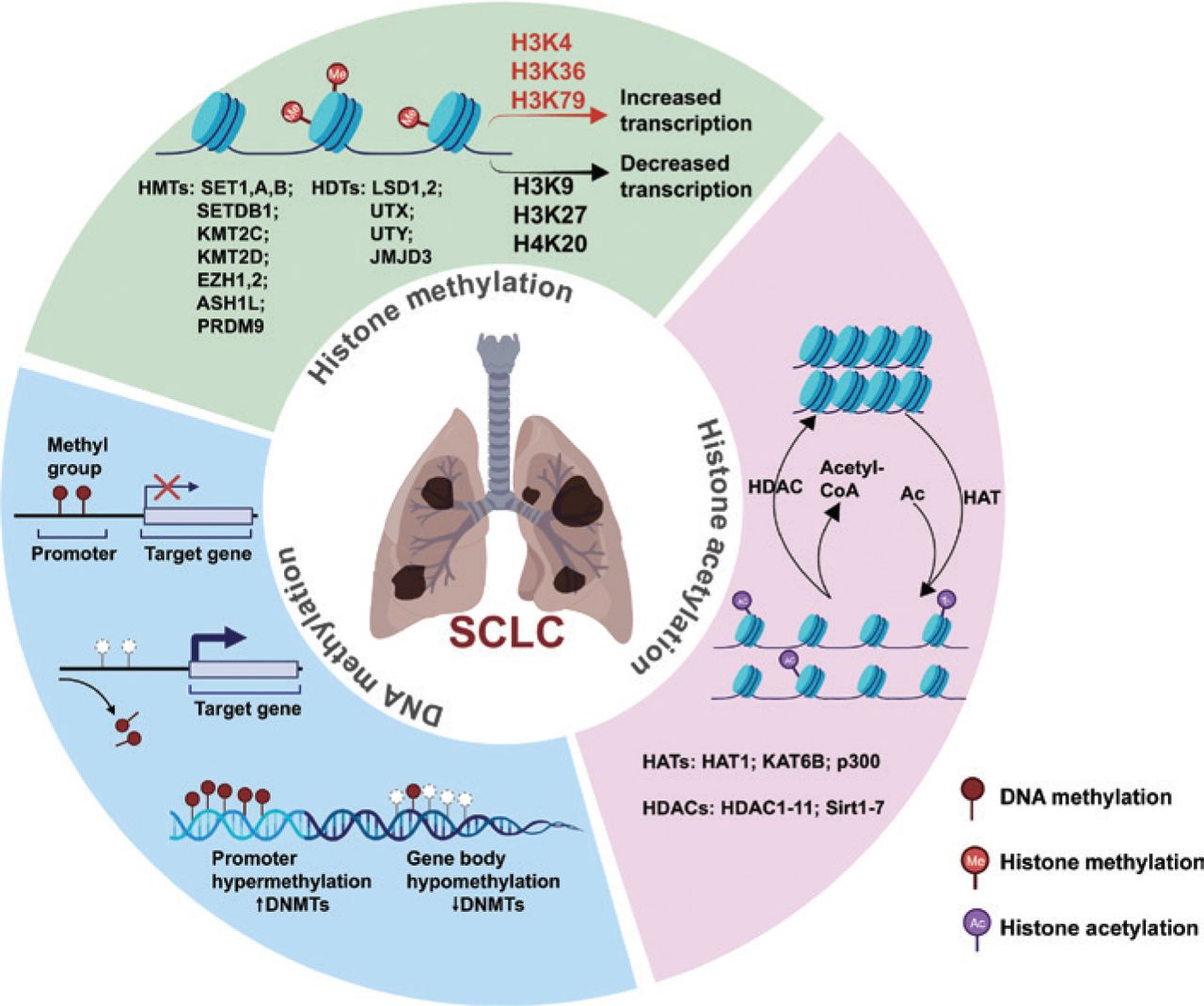
In many cancers, these SEs hijack the cell’s machinery to drive the overexpression of oncogenes, which are genes that have the potential to cause cancer. By using BET inhibitors (drugs that block the BRD4 protein), researchers can disrupt the connection between the super-enhancer and the gene it controls. This effectively “silences” the cancer’s growth signal without damaging the rest of the genome.
Recent data published this week suggests that this approach is particularly effective in hematologic malignancies (blood cancers) and certain aggressive brain tumors. By targeting the epigenetic landscape—the chemical modifications to DNA that regulate gene expression—clinicians can potentially reverse the “identity” of a cancer cell, forcing it to either stop dividing or undergo apoptosis, which is programmed cell death.
Synthetic Enhancers and the Evolution of Viral Immunotherapy
While inhibiting natural super-enhancers stops cancer, a parallel strategy involves creating synthetic super-enhancers to boost the immune system. This is a cornerstone of precision viral immunotherapy. By engineering synthetic DNA sequences that mimic super-enhancers, scientists can “supercharge” T-cells—the soldiers of the immune system—to recognize and attack tumor cells more aggressively.
This is especially critical for “cold” tumors, which are cancers that the immune system typically ignores. By inserting these synthetic enhancers via viral vectors (modified viruses used as delivery vehicles), researchers can force the expression of cytokines and receptors that make the tumor “hot” and visible to the immune system. This synergy between epigenetic silencing and immune activation represents a dual-pronged attack on tumor viability.
“The ability to precisely modulate the transcriptional output of a cell via super-enhancer manipulation allows us to move beyond simple inhibition. We are now entering an era of genomic orchestration, where You can dial down oncogenes and dial up tumor-suppressor genes simultaneously.”
Global Regulatory Pathways and Patient Access
The transition from “bench to bedside” varies significantly by region. In the United States, the FDA’s Fast Track and Orphan Drug designations are likely pathways for SE-targeting therapies, given their application in rare, aggressive cancers. In Europe, the EMA (European Medicines Agency) is expected to scrutinize the long-term genomic stability of these treatments, as altering epigenetic markers can occasionally lead to unintended gene activation.
For patients under the UK’s NHS, the primary hurdle remains cost-effectiveness. Gene therapies and precision epigenetic drugs are notoriously expensive to produce. The NICE (National Institute for Health and Care Excellence) framework will require rigorous evidence that SE-targeting extends quality-adjusted life years (QALYs) significantly more than existing standard-of-care therapies before widespread adoption.
Much of the current research, including the breakthroughs highlighted by Trogenix and various academic institutions, is funded through a mix of National Institutes of Health (NIH) grants and venture capital. This funding structure underscores the need for independent, double-blind placebo-controlled trials—studies where neither the patient nor the doctor knows who is receiving the treatment—to ensure that the observed efficacy is not skewed by corporate interest.
Comparative Analysis: Traditional vs. Super-Enhancer Therapy
| Feature | Conventional Chemotherapy | Super-Enhancer Targeting |
|---|---|---|
| Target | Rapidly dividing cells (General) | Regulatory DNA clusters (Specific) |
| Mechanism | Cytotoxic (Kills cells directly) | Epigenetic (Silences growth genes) |
| Specificity | Low (Affects healthy tissue) | High (Targets cancer-specific SEs) |
| Primary Risk | Systemic toxicity/Immunosuppression | Off-target gene silencing |
| Clinical Stage | Standard of Care | Pre-clinical / Early Phase Trials |
Contraindications & When to Consult a Doctor
Because SE-targeting therapies manipulate the fundamental way DNA is read, they are not suitable for everyone. Contraindications—conditions or factors that serve as a reason to withhold a certain medical treatment—include pregnancy, as epigenetic modifications can permanently alter fetal development. Patients with severe, pre-existing bone marrow failure may also be at higher risk due to the potential for off-target effects on hematopoietic stem cells.

Patients should consult an oncologist immediately if they experience:
- Unexplained, rapid weight loss or extreme fatigue.
- The appearance of new, hard, non-tender lumps in the breast, lymph nodes, or soft tissue.
- Persistent neurological changes, such as sudden blurred vision or loss of coordination, which may indicate tumor progression in the CNS.
The Road Ahead: Precision Oncology
The targeting of super-enhancers is not a “miracle cure,” but It’s a sophisticated evolution of cancer therapy. By moving the target from the protein to the promoter, we are gaining the ability to shut down the most aggressive drivers of malignancy with surgical precision. The next three to five years will be critical as these therapies move through Phase II and III trials to prove their safety and efficacy in diverse human populations.