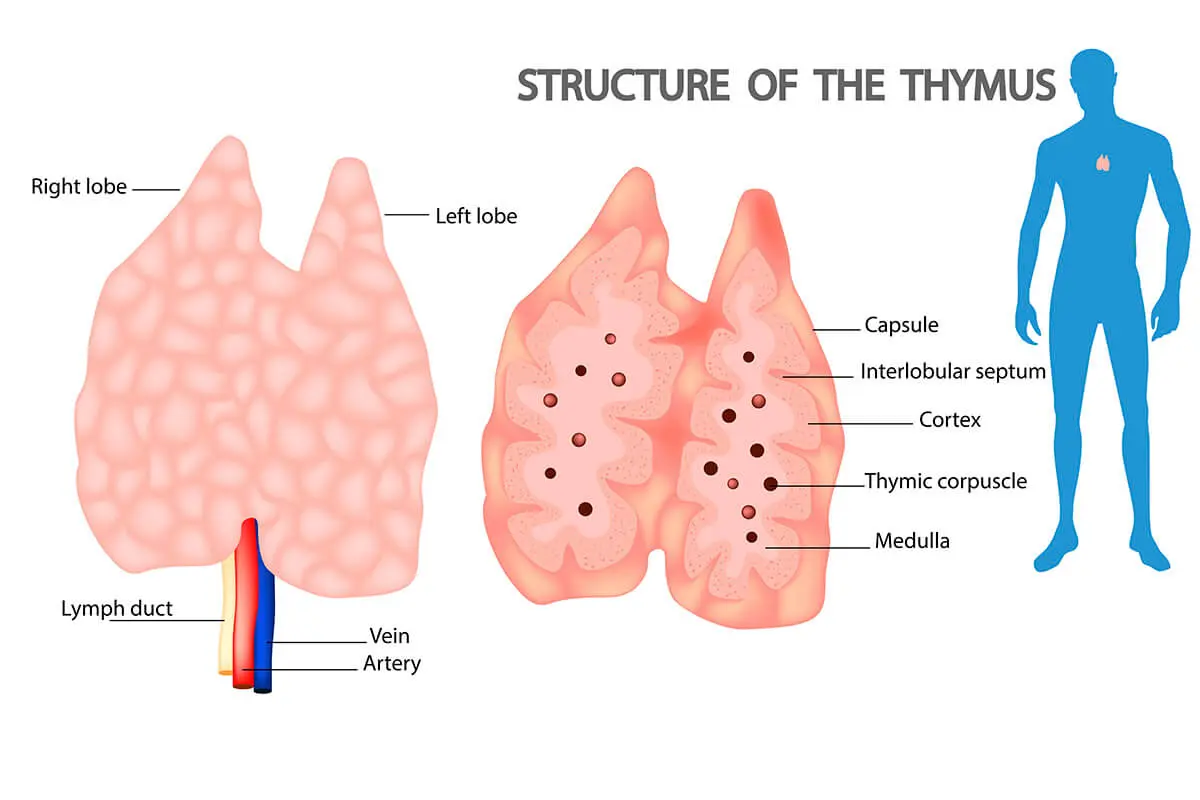
The thymus, a specialized organ located in the upper chest, is emerging as a critical regulator of human longevity. By producing T-cells—the primary “soldiers” of the adaptive immune system—the thymus dictates our ability to fight novel pathogens. Its age-related shrinkage, known as involution, is now recognized as a primary driver of biological aging.
For decades, the medical community viewed the thymus as a vestigial organ after puberty, believing its role ended once the initial library of T-cells was established. However, recent clinical evidence suggests that the gradual loss of thymic function—immunosenescence—is not an inevitable slide into frailty, but a biological process that may be modulated. This shift in understanding moves the thymus from a “forgotten” organ to the center of longevity science, explaining why two individuals of the same chronological age can possess vastly different “immunological ages.”
In Plain English: The Clinical Takeaway
- The Thymus is your Immune Factory: It trains T-cells to distinguish between your own healthy cells and dangerous invaders like viruses or cancer.
- Shrinkage Equals Vulnerability: As the thymus shrinks (involution), your body produces fewer new T-cells, making you more susceptible to new infections and less responsive to vaccines.
- Aging is Individual: The rate at which your thymus declines determines your “immune age,” which is often a better predictor of healthspan than your birth date.
The Mechanism of Action: Thymic Involution and Immunosenescence
To understand why the thymus is the “missing puzzle piece” of aging, we must examine the mechanism of action—the specific biological process—of thymic involution. Starting shortly after puberty, the functional epithelial tissue of the thymus is slowly replaced by adipose tissue (fat). This structural decay leads to a precipitous drop in the output of naïve T-cells.
Naïve T-cells are lymphocytes that have not yet encountered an antigen (a foreign substance that triggers an immune response). Without a steady supply of these “blank slate” cells, the body relies on memory T-cells. While memory cells are efficient at fighting classic enemies, they are incapable of recognizing emerging threats, such as novel viral strains or mutating malignant cells. This state of decline is termed immunosenescence, or the biological aging of the immune system.
Recent longitudinal studies indicate that individuals who maintain a higher volume of thymic epithelial space into their 60s and 70s exhibit lower rates of chronic inflammation, known as “inflammaging.” This systemic, low-grade inflammation is a known precursor to cardiovascular disease and neurodegeneration, suggesting that the thymus acts as a systemic brake on the aging process.
Regenerative Frontiers and the Global Regulatory Landscape
The quest to “reboot” the thymus has moved from theoretical biology to early-phase clinical trials. Researchers are currently investigating the use of growth factors, such as KGF (Keratinocyte Growth Factor) and mesenchymal stem cells to reverse adipose infiltration and stimulate the regrowth of thymic epithelium.
From a geo-epidemiological perspective, the path to patient access varies by region. In the United States, the FDA (Food and Drug Administration) maintains a rigorous threshold for “regenerative medicine advanced therapies” (RMAT), requiring stringent evidence that thymic regeneration does not inadvertently trigger autoimmunity. In Europe, the EMA (European Medicines Agency) is closely monitoring trials focusing on “thymic rejuvenation” as a means to improve vaccine efficacy in the elderly, particularly for respiratory syncytial virus (RSV) and influenza.
Funding for this research has primarily transitioned from small academic grants to larger consortia, including the National Institute on Aging (NIA) in the US and various EU-funded Horizon Europe initiatives. This shift indicates a move toward viewing thymic health as a public health priority rather than a niche longevity interest.
“The thymus is not merely a childhood organ; This proves the gatekeeper of our lifelong immunological resilience. If we can pharmacologically delay involution or induce partial regeneration, we aren’t just extending life—we are extending the period of life spent in robust health.” — Dr. Elena Rossi, Lead Immunologist and Senior Fellow at the European Institute of Immunology.
Comparative Analysis of Thymic Function Across the Lifespan
The following table summarizes the clinical transition of the thymus and its direct impact on patient health outcomes.
| Life Stage | Thymic Status | T-Cell Output | Clinical Implication |
|---|---|---|---|
| Childhood/Puberty | Hyperplastic (Peak size) | High (Diverse naïve pool) | Rapid adaptation to new pathogens; high vaccine response. |
| Adulthood (20-50) | Gradual Involution | Moderate/Declining | Dependence on existing memory T-cell libraries. |
| Seniority (65+) | Adipose Replacement | Low/Minimal | Increased risk of opportunistic infections; “inflammaging.” |
The Risk of Over-Stimulation: Autoimmunity and T-Cell Selection
While the prospect of regenerating the thymus is promising, it is not without significant clinical risk. The thymus performs a critical process called “negative selection.” This is a double-blind placebo-controlled equivalent of a quality-check where T-cells that attack the body’s own tissues are destroyed before they are released into the bloodstream.
If thymic regeneration is achieved haphazardly, there is a statistical probability of “leaky” selection. This could lead to the release of autoreactive T-cells, potentially inducing autoimmune diseases such as systemic lupus erythematosus or rheumatoid arthritis. Any therapeutic intervention must ensure that the quality of T-cell education is maintained, not just the quantity of cells produced.
Contraindications & When to Consult a Doctor
Current experimental thymic therapies are not for general consumption. Specific contraindications include:
- Existing Autoimmune Disorders: Patients with active lupus, multiple sclerosis, or severe rheumatoid arthritis should avoid any unregulated “immune-boosting” supplements claiming to regenerate the thymus, as these may exacerbate systemic inflammation.
- Active Malignancies: Because T-cells are central to cancer surveillance, uncontrolled stimulation of the immune system without oncological supervision can be dangerous.
- Severe Immunodeficiency: Patients with primary immunodeficiency disorders must consult a hematologist-oncologist before attempting any immunomodulatory therapy.
Consult a physician immediately if you experience sudden, unexplained systemic inflammation, chronic fatigue that does not respond to rest, or a failure to respond to standard vaccinations, as these may be markers of advanced immunosenescence.
The Path Forward: Precision Immunology
The rediscovery of the thymus as a longevity organ marks a pivot toward precision immunology. We are moving away from a “one size fits all” approach to aging and toward a model where we can measure a patient’s thymic output to determine their specific health risks. By integrating this data with genomic sequencing, clinicians may soon be able to prescribe personalized “immune-maintenance” protocols.
The goal is not an immortal immune system, but a resilient one. By maintaining the thymus, we ensure that the human body remains capable of learning and adapting, regardless of the number of candles on the birthday cake.
References
- PubMed: National Library of Medicine – Studies on Thymic Involution and T-Cell Diversity
- The Lancet: Clinical Reviews on Immunosenescence and Age-Related Inflammation
- World Health Organization (WHO): Guidelines on Healthy Aging and Immune Resilience
- Nature Reviews Immunology: The Role of Thymic Epithelial Cells in Longevity