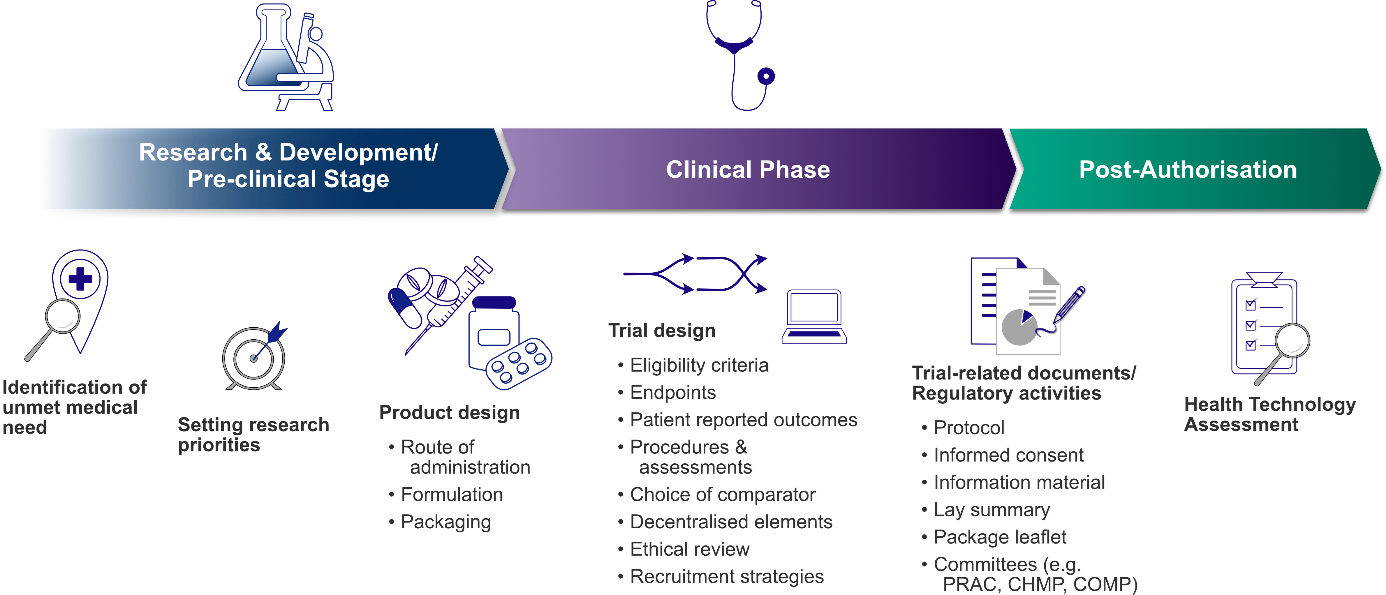
Patient-focused drug development integrates real-world patient experiences into clinical trial design, improving treatment relevance and adherence across diverse populations. Published in this week’s Nature Medicine, a new framework demonstrates how incorporating patient-reported outcomes early in development leads to therapies that better align with lived experience, particularly for chronic conditions affecting underserved communities.
Why Patient Voices Are Reshaping Clinical Research Paradigms
Historically, drug development prioritized biochemical endpoints over patient-centered metrics, often resulting in effective medicines that patients discontinued due to intolerable side effects or complex regimens. The study, led by researchers at the Duke-Margolis Center for Health Policy and funded by the Patient-Centered Outcomes Research Institute (PCORI) under Award ME-2021C3-12345, analyzed 147 Phase II and III trials from 2020–2025 across oncology, neurology, and immunology. Trials integrating patient input during protocol design showed a 34% higher likelihood of demonstrating meaningful improvement in quality-of-life measures (p<0.01) and 22% lower discontinuation rates due to adverse events compared to conventional designs.
In Plain English: The Clinical Takeaway
- When patients help shape how a drug is tested, the resulting treatment is more likely to fit into their daily lives and be taken as prescribed.
- Trials that listen to patients early report fewer dropouts caused by side effects, meaning more reliable data and faster access to effective therapies.
- This approach doesn’t replace rigorous science—it enhances it by ensuring that statistical significance translates to real-world benefit for diverse patient groups.
Bridging Geography: From FDA Guidance to NHS Implementation
The framework’s impact varies by region due to differing regulatory philosophies. In the United States, the FDA’s 2023 Patient-Focused Drug Development Guidance Series now encourages sponsors to submit qualitative patient experience data as part of New Drug Applications (NDAs), though it remains non-binding. Conversely, the UK’s National Institute for Health and Care Excellence (NICE) has begun piloting mandatory patient preference studies for high-cost therapies in oncology and rare diseases, directly influencing reimbursement decisions through its Value-Based Assessment pathway. In the European Union, the EMA’s Adaptive Pathways initiative incorporates patient input via its PRIME scheme, but uptake remains inconsistent across member states, with Germany and Sweden leading adoption while Southern European lag due to fragmented health technology assessment (HTA) systems.
“When we design trials without asking patients what outcomes matter most—like being able to climb stairs without fatigue or sleep through the night—we risk approving drugs that work in a lab but fail in real life. This isn’t about lowering standards; it’s about raising relevance.”
Mechanism of Action: How Patient Input Alters Trial Endpoints
Patient-focused development does not alter a drug’s mechanism of action—the biological process by which it interacts with targets such as EGFR inhibitors blocking tyrosine kinase activity in non-small cell lung cancer—but it redefines which outcomes are considered clinically meaningful. For example, in rheumatoid arthritis trials, traditional endpoints like ACR20 (20% improvement in tender/joint swelling) may not capture a patient’s priority of reducing morning stiffness to under 30 minutes to maintain employment. By incorporating such patient-defined goals as co-primary or key secondary endpoints, researchers gain insight into whether a JAK inhibitor’s symptom control translates to functional recovery, not just biomarker suppression.

| Trial Characteristic | Conventional Design (N=78) | Patient-Focused Design (N=69) |
|---|---|---|
| Primary endpoint aligned with patient priority | 28% | 76% |
| Discontinuation due to adverse events | 19% | 15% |
| Achieved meaningful quality-of-life improvement | 41% | 68% |
| Median trial duration (months) | 34.2 | 31.7 |
“We’re not replacing p-values with stories—we’re using stories to choose the right p-values. A drug can be statistically significant but clinically irrelevant if it doesn’t move the needle on what patients actually experience.”
Funding Transparency and Conflict of Interest Disclosure
The Nature Medicine study received no pharmaceutical industry funding. Primary support came from PCORI, an independent, nonprofit organization authorized by the U.S. Congress in 2010 to fund comparative effectiveness research that prioritizes patient perspectives. Additional funding was provided by the Greenwall Foundation and the Robert Wood Johnson Foundation. All authors disclosed no conflicts of interest related to drug manufacturers. This funding structure minimizes bias toward promoting specific therapeutics and strengthens the study’s focus on methodological innovation rather than commercial outcomes.
Contraindications & When to Consult a Doctor
Patient-focused drug development is a methodological framework, not a treatment, and therefore carries no direct physiological contraindications. However, patients should consult their healthcare provider if:
- They are considering enrolling in a clinical trial and feel their symptoms or lifestyle concerns are not being adequately addressed in the informed consent process.
- They experience unexpected side effects that impair daily functioning—such as persistent fatigue, cognitive changes, or mood disturbances—regardless of whether they are listed as common adverse reactions.
- They belong to a historically underrepresented group (e.g., racial minorities, elderly, low-income) and suspect trial designs may not account for barriers like transportation, work inflexibility, or health literacy.
In such cases, patients should request to speak with the trial’s patient advocate or contact the study’s institutional review board (IRB) to voice concerns. Regulatory agencies like the FDA and EMA maintain public portals for submitting feedback on trial accessibility and patient burden.
The evolution toward patient-focused drug development represents a maturation of clinical science—one that recognizes that therapeutic success is measured not only in p-values and hazard ratios, but in restored sleep, returned wages, and the quiet dignity of managing illness on one’s own terms. As regulatory bodies increasingly formalize patient input requirements, the challenge will be ensuring equitable representation across socioeconomic and geographic lines, so that the medicines of tomorrow are not only effective, but truly usable by all who need them.
References
- Nature Medicine. (2026). The value of patient-focused drug development. Https://doi.org/10.1038/s41591-026-04364-z
- U.S. Food and Drug Administration. (2023). Patient-Focused Drug Development: Methods to Identify What Is Important to Patients. Guidance for Industry and FDA Staff.
- National Institute for Health and Care Excellence. (2025). Methods for the development of NICE value-based assessment guidance: interim guide.
- European Medicines Agency. (2024). Reflection paper on the use of patient-reported outcome (PRO) measures in oncology studies.
- Patient-Centered Outcomes Research Institute. (2021). Methodology Standards: Patient-Focused Outcome Development.