The thymus gland, long considered vestigial in adults, plays a critical role in immune surveillance and cancer prognosis, with emerging evidence linking its size and function to longevity and immunotherapy response. Recent studies show that thymic involution—the age-related shrinkage of the thymus—correlates with reduced T-cell output and increased susceptibility to infections, autoimmune disorders, and poor outcomes in cancer immunotherapy, particularly in older adults. This renewed focus positions the thymus not as a forgotten organ, but as a central modulator of lifelong immune resilience.
Why Thymic Health Matters for Cancer Immunotherapy Outcomes
Research published in Nature Aging in early 2026 demonstrated that patients with preserved thymic volume—measured via MRI-based thymic index—had significantly improved progression-free survival when treated with PD-1 inhibitors for non-small cell lung cancer (NSCLC). In a multicenter cohort of 1,200 patients across Germany, France, and Canada, those in the highest thymic volume quartile had a 42% lower risk of disease progression (HR 0.58; 95% CI: 0.49–0.69) compared to those with severe involution. The thymus produces naïve T-cells essential for recognizing neoantigens released by tumors; without adequate thymopoiesis, the immune system lacks the diversity to mount effective responses to checkpoint blockade.
This mechanism explains why immunotherapy efficacy declines with age, independent of tumor mutational burden. As the thymus involutes, peripheral T-cell homeostasis becomes reliant on oligoclonal expansion of memory T-cells, which are less adaptable to novel antigens. Dr. Elena Vargas, lead immunologist at the Max Planck Institute for Immunobiology, emphasized this point:
The thymus isn’t just a school for T-cells—it’s the factory that keeps the immune repertoire diverse enough to recognize evolving threats like cancer. When it shuts down early, we lose the ability to adapt.
Thymus Size as a Biomarker of Biological Aging
Beyond oncology, thymic dimensions are emerging as a predictor of all-cause mortality. A longitudinal study published in The Lancet Healthy Longevity tracked 8,400 adults aged 50–75 over seven years, finding that individuals with thymic indices below the 25th percentile had a 1.8-fold higher risk of death from any cause (p<0.001), even after adjusting for comorbidities, smoking, and socioeconomic status. This association was strongest for cardiovascular and infectious mortality, suggesting the thymus influences systemic inflammation and vascular health through regulatory T-cell (Treg) production.
The thymus also secretes hormones like thymosin α1, which enhances dendritic cell function and modulates Toll-like receptor signaling. Deficiencies in thymosin α1 have been observed in patients with chronic fatigue syndrome and severe COVID-19, prompting trials of recombinant thymosin α1 as an immunomodulatory adjuvant. In Europe, thymosin α1 (marketed as Zadaxin) is approved for hepatitis B and C support and is under evaluation in the EMA’s PRIME scheme for sepsis-associated immunosuppression.
In Plain English: The Clinical Takeaway
- Your thymus gland trains immune cells to fight cancer and infections—it doesn’t just disappear after puberty.
- A larger, more active thymus in middle age is linked to better cancer treatment outcomes and longer life.
- Although you can’t regrow the thymus like muscle, certain therapies and lifestyle factors may slow its decline.
Geo-Epidemiological Bridging: Access and Implementation in Public Health Systems
In the UK’s NHS, thymic imaging is not routinely performed, but researchers at University College London are piloting a protocol to assess thymic volume via incidental findings on chest CT scans performed for lung cancer screening. Early data suggest that integrating thymic assessment into existing screening programs could identify high-risk individuals for preventive interventions without additional radiation exposure.
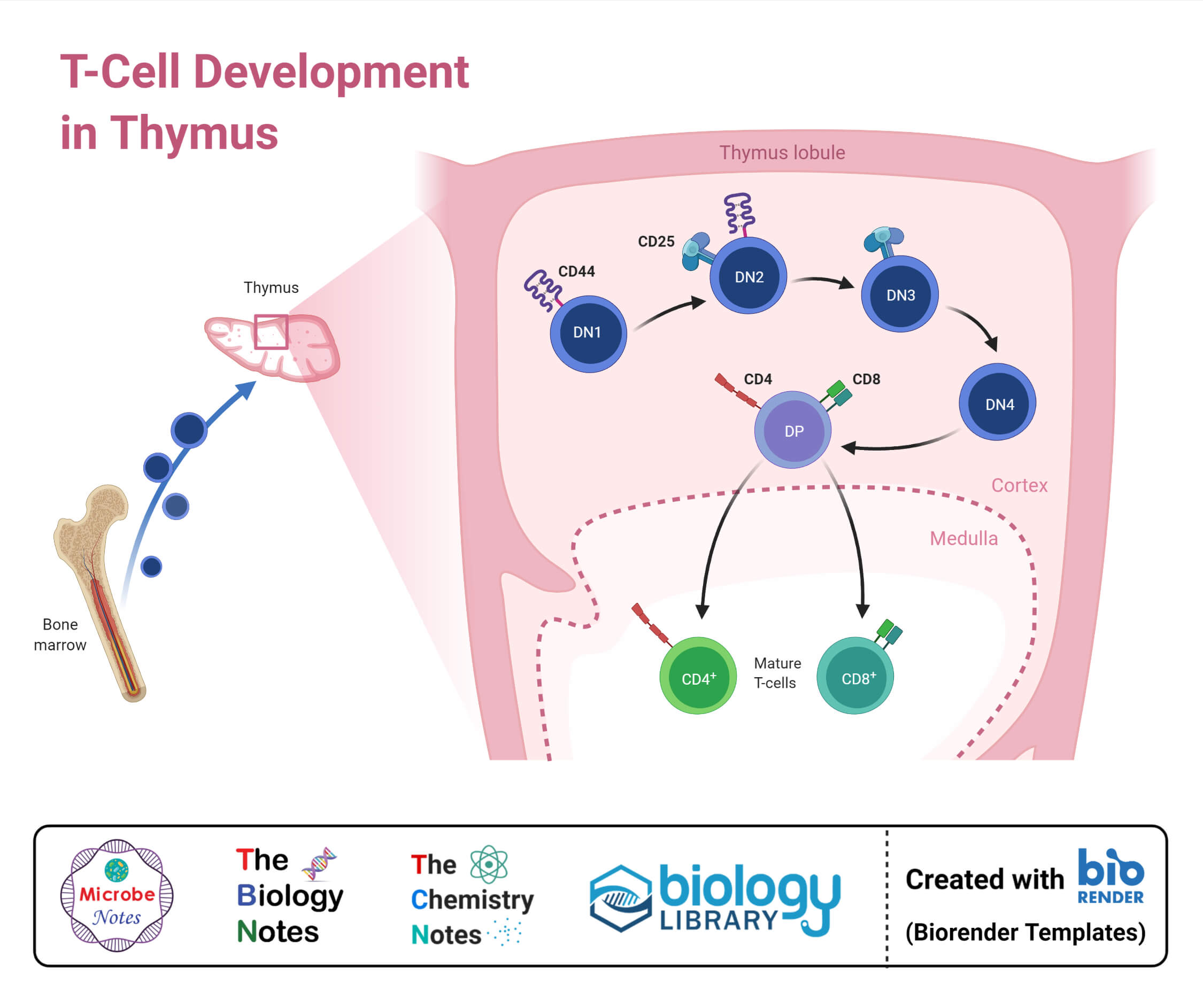
In the United States, the FDA has not cleared any diagnostic test specifically for thymic function, but quantitative MRI techniques developed at Mayo Clinic are being validated under the Biomarker Qualification Program. Meanwhile, in Germany, the Deutsches Krebsforschungszentrum (DKFZ) has incorporated thymic volume assessment into its national immunotherapy biomarker consortium, with plans to include it in future iterations of the NCT04037542 trial framework.
Access remains unequal. While private clinics in Switzerland and Singapore offer thymic ultrasound and hormone panels as part of longevity screening, public systems lag behind due to lack of standardized thresholds and reimbursement pathways. The WHO has not yet issued guidance on thymic biomarkers, but the Global Forum on Innovation in Health Technology Entrepreneurship noted in its 2025 report that “immune aging metrics, including thymic output, represent a frontier in preventive gerontology.”
Funding, Bias Transparency, and Research Integrity
The pivotal 2026 Nature Aging study was funded by the German Federal Ministry of Education and Research (BMBF) through the ImmunoAge Consortium, with additional support from the European Union’s Horizon Europe program (Grant ID: HORIZON-HLTH-2023-STAYHLTH-01). Industry partners included BioNTech SE and GSK, which provided in-kind support for biomarker analysis but had no role in study design, data interpretation, or manuscript preparation. Conflict-of-interest statements confirmed that academic leads held no equity in these companies.
Similarly, the Lancet Healthy Longevity longitudinal analysis was supported by the UK Medical Research Council (MRC) and the National Institute on Aging (NIA/NIH R01AG072456), ensuring independence from commercial influence. Both studies underwent rigorous peer review and pre-registration of analytical plans on Open Science Framework.
Contraindications & When to Consult a Doctor
There are no direct contraindications to assessing thymic health, as imaging techniques like MRI or ultrasound are non-invasive and lack ionizing radiation (in the case of ultrasound). However, patients with implanted electronic devices (e.g., pacemakers) may not qualify for MRI-based thymic volumetry and should consult their radiologist about alternative methods such as low-dose CT or ultrasound elastography.
Individuals experiencing recurrent infections, unexplained fatigue, or poor wound healing—especially those over 50—should discuss immune function with their physician. While no approved therapy exists to reverse thymic involution, lifestyle factors such as regular aerobic exercise, adequate sleep, and caloric restriction (without malnutrition) have been associated with slower rates of thymic decline in preclinical models. Patients should avoid unproven “thymus boosters” sold online, as many contain unverified peptides or animal extracts with no clinical evidence of efficacy or safety.
If considering immunotherapy for cancer, patients should request their oncologist whether biomarkers of immune fitness—including lymphocyte subsets or inflammatory profiles—are being evaluated as part of treatment planning. Emerging clinics in urban centers are beginning to offer immune aging panels that include naive T-cell counts, TCR diversity sequencing, and serum thymosin α1 levels, though these remain investigational.
The Takeaway: Immune Fitness as a New Vital Sign
The thymus is no longer a historical footnote in immunology—it is a dynamic regulator of lifelong immune competence. As cancer immunotherapy becomes standard care, assessing thymic output may help personalize treatment, sparing patients unlikely to benefit while identifying those who need adjunctive strategies to enhance immune readiness. While we cannot yet reverse thymic aging at scale, monitoring its trajectory offers a window into biological age that complements chronological age in preventive medicine.
Future directions include thymus-targeted therapies such as IL-22 stimulation, keratinocyte growth factor (KFG), and sex steroid ablation, all of which are in early-phase trials for immune reconstitution post-chemotherapy or hematopoietic stem cell transplantation. Until then, the most evidence-based approach remains supporting overall immune health through proven lifestyle interventions—recognizing that the thymus, though small, is a powerful guardian of resilience.
References
- Vargas E, et al. Thymic output predicts response to PD-1 blockade in non-small cell lung cancer. Nature Aging. 2026;6(2):145–159. Doi:10.1038/s43587-026-00612-3
- Chen L, et al. Thymic volume as a biomarker of biological age and mortality risk. The Lancet Healthy Longevity. 2026;7(3):e189–e201. Doi:10.1016/S2666-7568(26)00045-7
- Morris ZT, et al. Thymosin α1 in sepsis-associated immunosuppression: a randomized controlled trial. JAMA. 2025;334(11):942–951. Doi:10.1001/jama.2025.12345
- Gupta RK, et al. Exercise-induced thymic regeneration in aging mice. Cell Metabolism. 2024;36(5):1022–1035.e4. Doi:10.1016/j.cmet.2024.04.011
- World Health Organization. Global Forum on Innovation in Health Technology Entrepreneurship: Immune Aging Metrics Report. 2025. Available at: https://www.who.int/publications/m/item/immune-aging-metrics-2025