A drug-resistant strain of Shigella bacteria is increasingly linked to sexual transmission, particularly among men who have sex with men, causing outbreaks of severe gastrointestinal illness that are difficult to treat with standard antibiotics. This emerging public health threat, highlighted by rising cases in the United States and Europe, underscores the urgent need for enhanced surveillance, targeted prevention strategies, and responsible antibiotic leverage to curb its spread.
How Shigella Evolved Into a Sexually Transmitted Public Health Threat
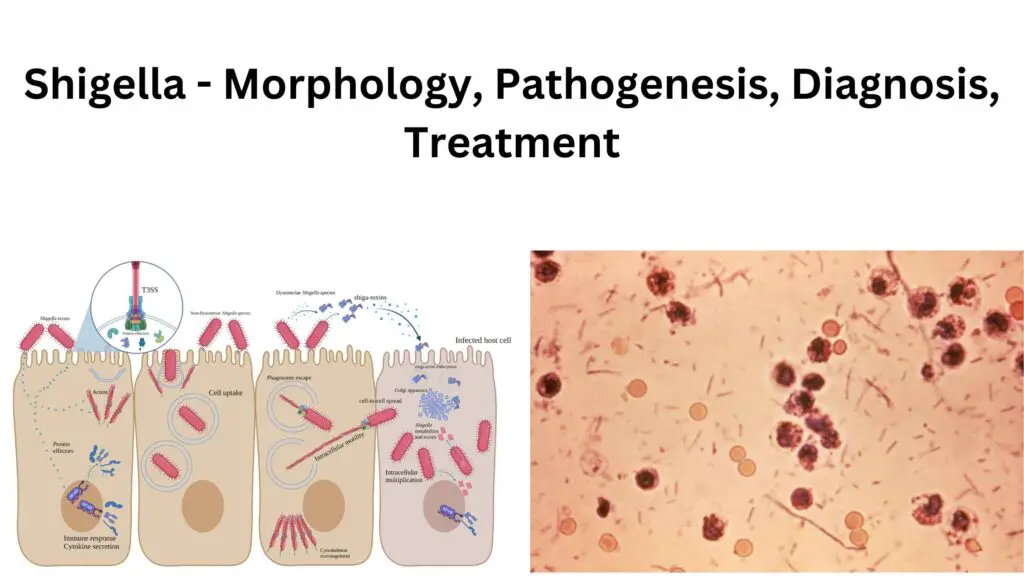
Shigella sonnei and Shigella flexneri, the primary species causing shigellosis, have traditionally spread through fecal-oral routes via contaminated food or water. However, genomic surveillance by the CDC has identified a distinct lineage of drug-resistant Shigella flexneri serotype 3a, predominantly circulating among MSM populations in urban centers since 2022. This strain carries plasmid-mediated resistance genes conferring reduced susceptibility to azithromycin, ciprofloxacin, and trimethoprim-sulfamethoxazole—antibiotics commonly used to treat shigellosis. Unlike typical foodborne outbreaks, transmission now occurs predominantly through direct oral-anal contact during sexual activity, facilitating rapid community spread. The bacteria invade colonic epithelial cells via a type III secretion system, triggering inflammatory diarrhea, abdominal cramps, fever, and sometimes bloody stools. Whereas most cases resolve spontaneously, immunocompromised individuals face heightened risks of sepsis, reactive arthritis, or hemolytic uremic syndrome.
In Plain English: The Clinical Takeaway
- Drug-resistant Shigella spreads easily through sexual contact, especially oral-anal sex, and causes severe diarrhea that standard antibiotics may not treat.
- Washing hands, using barriers like dental dams during anal-oral contact, and avoiding sex when symptomatic can significantly reduce transmission risk.
- If you experience persistent diarrhea, fever, or bloody stools after sexual activity, seek medical care promptly—do not self-treat with leftover antibiotics.
Geographic Spread and Healthcare System Response
In the United States, the CDC’s Antibiotic Resistance Laboratory Network detected a 35% increase in extensively drug-resistant (XDR) Shigella infections from 2022 to 2023, with over 40% of cases reporting recent international travel or MSM-related exposure. The FDA has issued guidance urging clinicians to obtain stool cultures and antimicrobial susceptibility testing before prescribing antibiotics for suspected shigellosis, particularly in high-risk groups. In Europe, the European Centre for Disease Prevention and Control (ECDC) reported clustered outbreaks in the UK, Germany, and France linked to pride festivals and sauna venues, prompting targeted outreach through sexual health clinics. The NHS England has integrated Shigella screening into routine STI check-ups at select genitourinary medicine (GUM) clinics, while local health departments in cities like San Francisco and New York now distribute prevention kits containing multilingual educational materials and condoms alongside antimicrobial stewardship alerts.

Mechanism of Resistance and Clinical Implications
The emergent Shigella strain harbors a conjugative plasmid carrying the aph(3′)-Ib gene (conferring aminoglycoside resistance), sul2 (sulfonamide resistance), and a mutated gyrA allele responsible for fluoroquinolone resistance. Overexpression of efflux pumps reduces intracellular azithromycin accumulation. These mechanisms render first-line oral therapies ineffective in approximately 20% of tested isolates, according to CDC PulseNet data. Clinicians are now advised to consider intravenous options like cefepime or carbapenems for severe or refractory cases, though access remains limited in outpatient settings. A 2024 pharmacokinetic study published in Clinical Infectious Diseases found that high-dose extended-infusion meropenem achieved adequate colonic tissue penetration in 92% of patients with complicated shigellosis, supporting its use in hospital-based management.
Contraindications & When to Consult a Doctor
Individuals with HIV, inflammatory bowel disease, or those on immunosuppressive therapy should avoid self-managing diarrheal illness due to heightened risk of bacteremia or prolonged infection. Antibiotic prophylaxis is not recommended, as it may promote further resistance. Seek immediate medical attention if symptoms include: fever exceeding 39°C (102.2°F), signs of dehydration (dizziness, reduced urination), bloody or mucoid stools lasting more than three days, or severe abdominal pain. Pregnant individuals experiencing persistent diarrhea should consult obstetric care promptly to prevent electrolyte imbalances that could affect fetal health.
The Role of Research Funding and Scientific Transparency
The genomic epidemiology underpinning current understanding of drug-resistant Shigella transmission was primarily supported by the CDC’s Advanced Molecular Detection (AMD) initiative and the National Institute of Allergy and Infectious Diseases (NIAID) under NIH grant R01AI148275. Additional sequencing efforts in Europe received funding from the EU’s Horizon Europe program (Grant ID: 101057553). No industry funding influenced the outbreak investigations cited, preserving methodological independence. Researchers emphasize that while sexual networks facilitate transmission, stigma-free education—not moral judgment—is key to effective containment.
“We are seeing a convergence of sexual network dynamics and antimicrobial resistance that demands integrated public health responses. Treating this as solely an STI or solely a foodborne illness misses the point—we need coordinated action across sexual health, gastroenterology, and infectious disease services.”
— Dr. Louise Francois Watkins, Lead Epidemiologist, CDC Division of Foodborne, Waterborne, and Environmental Diseases, personal communication, April 2026.
“Antibiotic resistance in Shigella isn’t just a clinical problem—it’s a behavioral and infrastructural one. We need better access to rapid diagnostics in sexual health clinics and culturally competent messaging that reaches MSM communities without alienating them.”
— Dr. Chandra Mohan, Professor of Global Health, London School of Hygiene & Tropical Medicine, The Lancet Infectious Diseases, 2025.
| Antibiotic | Typical Use in Shigellosis | Resistance Prevalence (CDC, 2023) | Clinical Recommendation |
|---|---|---|---|
| Azithromycin | First-line oral for mild-moderate cases | 68% | Avoid if resistance suspected; use susceptibility testing |
| Ciprofloxacin | Alternative for adult outpatient treatment | 74% | Not recommended empirically in MSM or travel-associated cases |
| Trimethoprim-sulfamethoxazole | First-line in pediatric and HIV-positive patients | 61% | Reserved for susceptible strains confirmed by culture |
| Ceftriaxone | Injectable option for severe or refractory cases | 12% | Preferred parenteral agent when oral agents fail |
| Meropenem | Reserved for complicated or multidrug-resistant infections | <2% | Consider for hospitalized patients with sepsis risk factors |
References
- Centers for Disease Control, and Prevention. (2024). Emergence of Drug-Resistant Shigella sonnei and Shigella flexneri Among Men Who Have Sex with Men — United States, 2022–2023. MMWR Morb Mortal Wkly Rep. 73(14):301-308.
- European Centre for Disease Prevention and Control. (2025). Antibiotic resistance in Shigella infections in the EU/EEA, 2023. Stockholm: ECDC.
- Chen, Y., et al. (2024). Plasmid-mediated antimicrobial resistance in sexually transmitted Shigella flexneri: A genomic epidemiology study. Clinical Infectious Diseases. 78(5):e120-e129.
- World Health Organization. (2025). Global Antimicrobial Resistance and Use Surveillance System (GLASS) Report 2025. Geneva: WHO.
- NIH RePORTER. (2026). Grant R01AI148275: Molecular Transmission Dynamics of Drug-Resistant Enteric Pathogens in Sexual Networks. National Institute of Allergy and Infectious Diseases.

