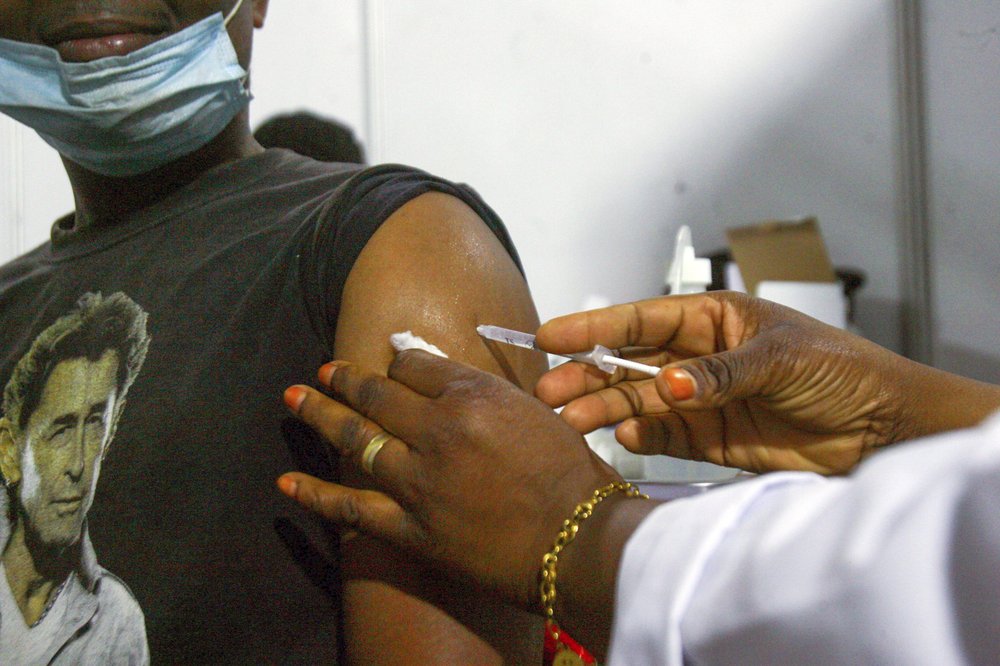
As of April 2026, the Pan American Health Organization (PAHO) is urgently urging intensified vaccination efforts across the Americas after measles cases surged by over 300% compared to the same period in 2025, with outbreaks reported in Brazil, Venezuela, and several Caribbean nations, driven primarily by declining immunization coverage in vulnerable communities.
Why Measles Is Resurging Despite a Safe, Effective Vaccine
Measles, caused by the measles morbillivirus, is one of the most contagious pathogens known, with an basic reproduction number (R0) of 12–18, meaning one infected person can transmit the virus to up to 18 susceptible individuals in an unvaccinated population. The measles, mumps, and rubella (MMR) vaccine, which uses live attenuated viruses to stimulate long-lasting humoral and cell-mediated immunity, is approximately 97% effective after two doses. However, vaccine hesitancy, disrupted routine immunization during the COVID-19 pandemic, and uneven healthcare access have left pockets of susceptibility, allowing the virus to exploit gaps in herd immunity—typically requiring 95% coverage to prevent sustained transmission.
In Plain English: The Clinical Takeaway
- Measles is not just a rash; it can cause severe complications like pneumonia and encephalitis, especially in young children and immunocompromised individuals.
- Two doses of the MMR vaccine provide lifelong protection for most people and are the most effective tool we have to stop outbreaks.
- Even if you were vaccinated as a child, checking your immunization status is wise—particularly if you live in or travel to areas with active transmission.
Epidemiological Surge and Regional Vulnerabilities
According to PAHO’s weekly epidemiological update released in mid-April 2026, over 8,400 confirmed measles cases have been reported across the Americas since January 2026, compared to just under 2,100 in the same period last year. Brazil accounts for nearly 60% of cases, with significant clusters in Amazonas and Roraima states, where indigenous populations and migrant communities face barriers to healthcare access. In the Caribbean, Jamaica and Guyana have reported localized outbreaks linked to imported cases from South America, exacerbated by vaccine coverage dropping below 85% in some parishes—well under the 95% threshold needed for herd immunity.

This resurgence contrasts sharply with the region’s progress toward measles elimination, which was verified in 2016. The reversal underscores how fragile disease control gains can be when vaccination systems falter. Unlike tetanus or hepatitis B, measles has no animal reservoir and relies entirely on human-to-human transmission, making it eradicable—but only if immunity is uniformly high.
How the MMR Vaccine Works: Mechanism and Safety
The MMR vaccine contains weakened forms of the measles, mumps, and rubella viruses. Upon injection, these attenuated viruses replicate minimally in the body, triggering an adaptive immune response without causing disease in healthy individuals. This process activates B cells to produce neutralizing antibodies against the viral hemagglutinin protein and stimulates cytotoxic T cells to eliminate infected cells. The immune system then retains memory cells capable of mounting a rapid response upon future exposure.
Extensive safety monitoring confirms the MMR vaccine’s strong risk-benefit profile. Febrile seizures occur in approximately 1 in 3,000 to 4,000 doses—typically benign and self-limiting. Thrombocytopenia is rare (about 1 case per 30,000 doses). No credible evidence links the MMR vaccine to autism; this myth originated from a retracted and fraudulent 1998 study and has been repeatedly debunked by large-scale cohort studies involving over 1.2 million children.
Contraindications & When to Consult a Doctor
The MMR vaccine is contraindicated in individuals with severe immunodeficiency (e.g., from chemotherapy, congenital disorders like SCID, or high-dose immunosuppressants) and those who have experienced a life-threatening allergic reaction (anaphylaxis) to a prior dose or vaccine component such as gelatin or neomycin. Pregnant individuals should avoid the MMR vaccine due to theoretical fetal risk, though no cases of congenital rubella syndrome have been linked to inadvertent vaccination; nonetheless, it is administered postpartum if needed.
Seek medical attention if you or a child develops symptoms suggestive of measles: high fever (>101°F), cough, coryza (runny nose), conjunctivitis (red eyes), and a maculopapular rash that begins at the hairline and spreads downward. Koplik spots—tiny white lesions on the buccal mucosa—are pathognomonic but transient. Complications such as difficulty breathing, persistent vomiting, lethargy, or seizures require urgent evaluation, as they may indicate pneumonia or encephalitis.
Funding, Transparency, and Global Coordination
PAHO’s measles response is supported by funding from the U.S. Centers for Disease Control and Prevention (CDC), the Canadian Immunization Initiative, and the GAVI Alliance, which provides vaccine procurement support to low- and middle-income countries in the region. The underlying research on MMR vaccine efficacy and safety draws from decades of peer-reviewed studies, including pivotal Phase III trials conducted in the 1970s–80s involving over 15,000 children across multiple continents, with long-term follow-up confirming durability of immunity.

No single pharmaceutical company funds PAHO’s current advocacy; the organization operates as an independent public health agency under the World Health Organization (WHO). Vaccine procurement for national programs is managed through the PAHO Revolving Fund, which negotiates pooled pricing to ensure equitable access.
“We have the tools to eliminate measles again—but only if we act now to close immunity gaps. Every missed vaccine is a crack in our collective defense.”
“Measles is a litmus test for the strength of immunization systems. When coverage drops, it’s the first disease to come back—and it hits the most vulnerable hardest.”
| Metric | Value | Source |
|---|---|---|
| Measles vaccine effectiveness (2 doses) | 97% | CDC |
| Herd immunity threshold for measles | 95% | WHO |
| Confirmed measles cases in the Americas, Jan–Apr 2026 | 8,400+ | PAHO |
| Febrile seizure risk post-MMR | 1 in 3,000–4,000 | Vaccine Safety Datalink |
| Autism risk linked to MMR | No causal association | Miller et al., JAMA Pediatrics, 2019 |
References
- Centers for Disease Control and Prevention. Measles (Rubeola) Vaccination. https://www.cdc.gov/vaccines/vpd/mmr/public/index.html
- World Health Organization. Measles Fact Sheet. https://www.who.int/news-room/fact-sheets/detail/measles
- Pan American Health Organization. Epidemiological Updates on Measles in the Americas. https://www.paho.org/en/topics/measles
- Miller et al. Association Between Measles-Mumps-Rubella Vaccination and Autism Spectrum Disorder Among Children. JAMA Pediatrics. 2019;173(4):346–353. https://doi.org/10.1001/jamapediatrics.2018.4410
- Gastañaduy et al. Measles Outbreak in a Highly Vaccinated Population — Israel, 2017–2019. Clinical Infectious Diseases. 2020;71(11):2865–2872. https://doi.org/10.1093/cid/ciaa1155