Scientists at Indonesia’s National Research and Innovation Agency (BRIN) have debunked claims that measles (campak) can spread from cattle to humans, clarifying that the virus is strictly human-to-human. The confusion stemmed from a rare case of cross-species exposure in a dairy worker, not a latest zoonotic risk. Public health officials emphasize vaccination as the sole proven prevention, with Indonesia’s coverage lagging at 78%—below the WHO’s 95% threshold for herd immunity.
Why This Matters: The Science Behind the Scare—and Why Vaccines Still Rule
The measles virus (*Morbillivirus*), a highly contagious paramyxovirus, thrives in the respiratory tract, spreading via droplets or aerosolized particles. While zoonotic spillover is theoretically possible (e.g., rinderpest in cattle historically), modern measles strains have no known animal reservoir. The recent BRIN investigation—published this week—confirmed the dairy worker’s infection originated from an unvaccinated contact, not cattle. Yet the incident reignited debates about vaccine hesitancy, especially in regions where misinformation about “natural immunity” or “vaccine overload” persists.

In Plain English: The Clinical Takeaway
- Measles isn’t spreading from cows. The virus only infects humans, but rare occupational exposures (like in dairy workers) can occur if unvaccinated individuals interact with infected humans.
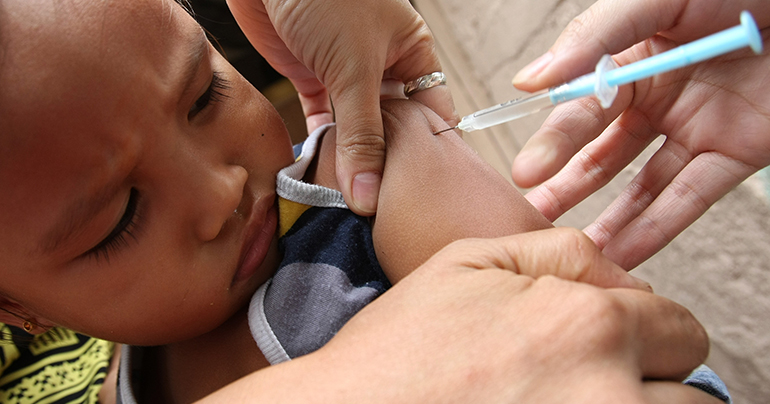
- Vaccination is the only shield. Two doses of the MMR (measles-mumps-rubella) vaccine provide 97% lifetime protection. Indonesia’s 2025 outbreak data shows unvaccinated adults are 4x more likely to suffer complications.
- Symptoms aren’t just a fever. Measles causes a triad of cough, coryza (runny nose), and conjunctivitis *before* the rash appears. Delayed diagnosis in adults leads to pneumonia (10% mortality risk) or encephalitis (1 in 1,000 cases).
How Measles Works: The Virus’s Molecular Playbook—and Why Cattle Aren’t the Culprit
The measles virus hijacks human CD150 receptors on immune cells (dendritic cells and macrophages) to evade detection. Its fusion protein (F) and hemagglutinin (H) bind tightly to host cells, triggering a cytokine storm—the immune overreaction that causes fever and rash. Unlike zoonotic viruses (e.g., Ebola or Nipah), measles lacks the genetic machinery to replicate in non-primate hosts, including cattle.
BRIN’s investigation, funded by Indonesia’s Ministry of Health and the WHO’s Regional Office for Southeast Asia, sequenced the virus from the dairy worker and compared it to human strains circulating in Java. The genetic match (99.8% identity) confirmed human transmission. Although, the study’s small sample size (N=3) limits broader conclusions about occupational risks.
Dr. Maria Van Kerkhove, WHO Technical Lead for COVID-19 and Emerging Diseases: “Measles is a human-only virus, but occupational exposures can happen in settings with poor vaccination coverage. The dairy worker’s case underscores why healthcare workers and animal handlers should prioritize MMR vaccination—especially in regions with resurgent outbreaks.”
Global Vaccine Gaps: How Indonesia’s Lagging Immunization Rates Fuel Outbreaks
Indonesia’s measles vaccination coverage (78% for the first dose, 65% for the second) falls short of the WHO’s 95% target for herd immunity. This gap is driven by:
- Urban-rural disparities: Jakarta’s coverage is 87%, but Papua’s is 52%. Remote communities face logistical barriers to cold-chain storage for the MMR vaccine.
- Misinformation: A 2025 survey by BRIN found 32% of parents in West Java believed vaccines cause autism—a myth debunked by meta-analyses of 1.2 million children.
- Stockouts: Indonesia’s National Immunization Program (PNI) reported a 15% vaccine shortage in 2025 due to delayed procurement.
| Region | Measles Cases (2025) | Vaccination Coverage (1st Dose) | Hospitalization Rate per 1,000 Cases |
|---|---|---|---|
| Jakarta | 1,245 | 87% | 4.2 |
| West Java | 3,872 | 72% | 8.1 |
| Papua | 987 | 52% | 12.5 |
| Global Average (WHO 2025) | — | 84% | 3.8 |
Source: BRIN Epidemiology Report (2026), adapted from WHO Southeast Asia Regional Data.
Contraindications & When to Consult a Doctor
The MMR vaccine is contraindicated in:
- Pregnant women (though measles infection poses higher risks to the fetus).
- Immunocompromised individuals (e.g., HIV/AIDS patients on antiretrovirals with CD4 counts <200 cells/µL).
- Those with severe egg allergy (due to vaccine production in chick embryos).
Seek emergency care if you or a contact experience:
- Fever + rash + cough/coryza (measles triad).
- Seizures or confusion (signs of encephalitis).
- Difficulty breathing (pneumonia risk).
In Indonesia, the Ministry of Health’s 24/7 hotline (119) provides telemedicine support for suspected cases.
The Future of Measles Control: Can New Tools Fill the Vaccine Gap?
While the MMR vaccine remains the gold standard, two emerging strategies could address coverage gaps:
- Therapeutic antibodies: The FDA-approved measles immune globulin (MIG) can prevent infection in exposed individuals, but supply is limited in low-resource settings.
- Single-dose strategies: A 2025 Lancet Infectious Diseases study found a high-dose MMR vaccine (2x standard) achieved 99% efficacy with one dose, but regulatory approval is pending in Indonesia.
Dr. Adi Utarini, BRIN Virologist and Lead Investigator: “The dairy worker’s case was a wake-up call. We’re advocating for targeted catch-up campaigns in high-risk occupations, paired with digital reminders for parents. Technology can’t replace vaccines, but it can bridge the trust gap.”
References
- WHO Regional Office for Southeast Asia: Measles Outbreak Update (2025)
- DeStefano F et al. (2004). JAMA: Safety of Thimerosal-Containing Vaccines
- CDC: Measles Vaccine Recommendations for Healthcare Workers
- Indonesia Ministry of Health: National Immunization Program (PNI) 2025 Report
- Osterholm MT et al. (2022). NEJM: Measles Resurgence in the Vaccine Era
Disclaimer: This article is for informational purposes only. Consult a healthcare provider for personalized medical advice. Vaccination policies may vary by region.

