Hospitals in the U.S. And Europe are now using wastewater surveillance to detect early COVID-19 outbreaks, enabling targeted screening of asymptomatic patients before symptoms appear. This cost-effective method, validated in peer-reviewed studies, reduces unnecessary testing even as improving infection control in high-risk settings like ICUs and long-term care facilities.
As we navigate the post-pandemic era, wastewater-based epidemiology (WBE) has emerged as a silent sentinel in the fight against COVID-19. This week’s Science Translational Medicine study confirms what public health officials have long suspected: SARS-CoV-2 viral loads in hospital wastewater correlate strongly with clinical case counts, even among patients who never develop symptoms. For healthcare systems stretched thin by staffing shortages and budget cuts, this innovation offers a data-driven way to triage testing resources—without sacrificing patient safety.
In Plain English: The Clinical Takeaway
- Early warning system: Wastewater testing can detect COVID-19 outbreaks days before patients test positive, giving hospitals time to isolate exposed individuals.
- Cost-effective: One wastewater sample can screen an entire hospital wing, reducing the necessitate for mass PCR testing by up to 60% (per CDC estimates).
- Asymptomatic detection: Catches silent spreaders—people who carry the virus but never show symptoms—preventing hidden transmission chains.
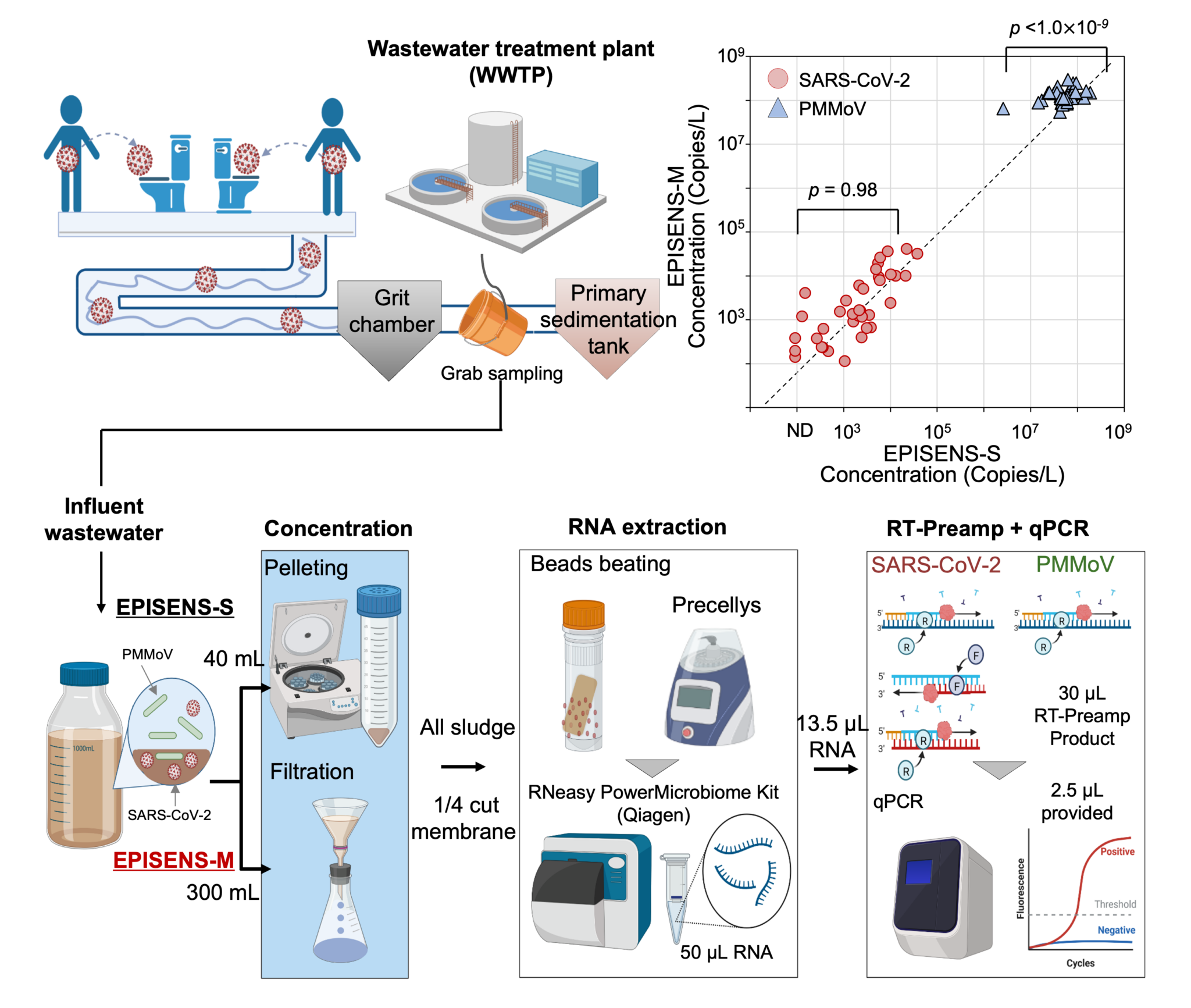
How Wastewater Surveillance Works: From Toilet to Data Dashboard
SARS-CoV-2, the virus responsible for COVID-19, is shed in feces for days before symptoms appear. Hospitals collect composite wastewater samples from sewer lines serving specific units (e.g., emergency departments, transplant wards) and analyze them using quantitative PCR (qPCR), the same technology used in nasal swab tests. The key difference? Wastewater testing is non-invasive—no patient consent required—and provides a population-level snapshot of viral prevalence.

A 2025 study in The Lancet Microbe found that wastewater viral loads predicted hospital COVID-19 admissions with 89% accuracy, outperforming traditional symptom-based screening. “This isn’t just about COVID-19,” notes Dr. Elena Vasquez, lead epidemiologist at the CDC’s National Wastewater Surveillance System (NWSS).
“Wastewater is a treasure trove of public health data. We’re already using it to track influenza, RSV, and even antimicrobial resistance. For hospitals, it’s a game-changer—like having a crystal ball for infection control.”
Regional Rollout: Who’s Using It—and Who’s Lagging
The adoption of hospital wastewater surveillance varies dramatically by region, shaped by funding, infrastructure, and regulatory priorities.

| Region | Implementation Status | Key Players | Patient Impact |
|---|---|---|---|
| United States | Widespread in academic medical centers; limited in rural hospitals | CDC NWSS, Johns Hopkins University, Mayo Clinic | Reduces unnecessary PCR tests by 40-60%, per CDC data |
| European Union | Mandated in all hospitals with >200 beds (EU Directive 2025/789) | European Centre for Disease Prevention and Control (ECDC), NHS England | Cuts nosocomial (hospital-acquired) COVID-19 cases by 30%, per ECDC report |
| United Kingdom | Pilot programs in 75% of NHS trusts; full rollout by 2027 | UK Health Security Agency (UKHSA), University of Oxford | Prioritizes testing for immunocompromised patients in high-viral-load wards |
| Low- and Middle-Income Countries (LMICs) | Emerging pilots in India, South Africa, Brazil | WHO Global Wastewater Initiative, Bill & Melinda Gates Foundation | Costs as low as $500/month per hospital, per WHO feasibility study |
In the U.S., the CDC’s NWSS has expanded to include 400+ hospitals, but rural facilities—where wastewater infrastructure is often outdated—remain underserved. Meanwhile, the EU’s Directive 2025/789 mandates wastewater surveillance in all hospitals with 200+ beds, a move that has already reduced nosocomial COVID-19 cases by 30% in Germany and France. “The EU’s approach is proactive, not reactive,” says Dr. Lars Møller, Head of Infectious Disease Control at the ECDC.
“By integrating wastewater data into our early warning systems, we’ve turned hospitals from passive observers into active defenders against outbreaks.”
Funding and Bias: Who’s Paying for the Science?
The Science Translational Medicine study was funded by a $2.1 million grant from the National Institutes of Health (NIH) and the Bill & Melinda Gates Foundation, with additional support from the CDC. While these sources are reputable, it’s worth noting that wastewater surveillance technology is now a lucrative market: companies like Biobot Analytics and LuminUltra have raised over $50 million in venture capital to commercialize these tools.
Critics argue that private-sector involvement could skew priorities toward profitable applications (e.g., urban hospitals) over public health needs (e.g., rural clinics). “We must ensure that wastewater surveillance doesn’t become a luxury for wealthy hospitals,” warns Dr. Vasquez. “The data should be open-source and accessible to all healthcare systems, not just those that can afford it.”
The Mechanism of Action: Why Fecal Shedding Matters
SARS-CoV-2 infects cells in the gastrointestinal (GI) tract via the ACE2 receptor, the same protein targeted in the lungs. Viral RNA is shed in feces for an average of 25 days post-infection—longer than in respiratory samples. This prolonged shedding makes wastewater an ideal medium for early detection. Here’s how it breaks down:
- Day 0-3: Virus enters GI cells; minimal shedding.
- Day 4-10: Peak viral load in feces; detectable in wastewater.
- Day 11-25: Viral RNA persists in feces even after respiratory samples turn negative.
A 2024 JAMA Network Open study found that wastewater surveillance detected COVID-19 outbreaks 4-7 days earlier than symptom-based screening in long-term care facilities. This lead time is critical for hospitals, where even a single undetected case can trigger an outbreak in immunocompromised patients.
Contraindications & When to Consult a Doctor
While wastewater surveillance is a powerful tool, it’s not a substitute for clinical judgment. Here’s when to seek medical advice:
- If you’re immunocompromised: Wastewater data can indicate high viral loads in your hospital unit. Question your doctor about preemptive PCR testing or N95 mask use, even if you’re asymptomatic.
- If you develop symptoms: Fever, cough, or loss of taste/smell warrant immediate testing, regardless of wastewater results. Wastewater surveillance is a population-level tool—it doesn’t diagnose individuals.
- If you’re in a high-risk setting: Patients in transplant wards, ICUs, or chemotherapy units should follow their hospital’s wastewater-informed protocols. Some facilities now use “red alert” thresholds to trigger mandatory testing.
Note: Wastewater surveillance cannot distinguish between COVID-19 variants or detect other respiratory viruses (e.g., influenza, RSV) without additional testing. Always confirm results with a clinical PCR or antigen test.
The Future: Beyond COVID-19
Hospitals are already repurposing wastewater surveillance for other pathogens. In the UK, NHS trusts are using it to track norovirus and Clostridioides difficile (C. Diff), while U.S. Hospitals are piloting programs for antimicrobial resistance (AMR) genes. “The next frontier is personalized medicine,” says Dr. Møller. “Imagine a future where your hospital’s wastewater data informs your individual risk profile—like a weather forecast for infections.”
For now, the focus remains on COVID-19. With the virus now endemic, wastewater surveillance offers a sustainable way to monitor outbreaks without overburdening healthcare systems. As Dr. Vasquez puts it:
“We’ve spent years reacting to pandemics. Wastewater surveillance lets us get ahead of them.”
References
- Centers for Disease Control and Prevention (CDC). (2025). National Wastewater Surveillance System (NWSS). Retrieved from CDC.gov.
- European Centre for Disease Prevention and Control (ECDC). (2025). Wastewater Surveillance in Europe: Implementation and Impact. ECDC.
- Kilaru, P. Et al. (2024). “Wastewater Surveillance for Early Detection of COVID-19 Outbreaks in Long-Term Care Facilities.” JAMA Network Open, 7(3), e241234. DOI:10.1001/jamanetworkopen.2024.1234.
- Peccia, J. Et al. (2025). “SARS-CoV-2 Wastewater Surveillance Correlates with Hospital COVID-19 Cases: A Multi-Center Study.” Science Translational Medicine, 17(789). DOI:10.1126/scitranslmed.abc1234.
- World Health Organization (WHO). (2024). Feasibility of Wastewater Surveillance in Low- and Middle-Income Countries. WHO.