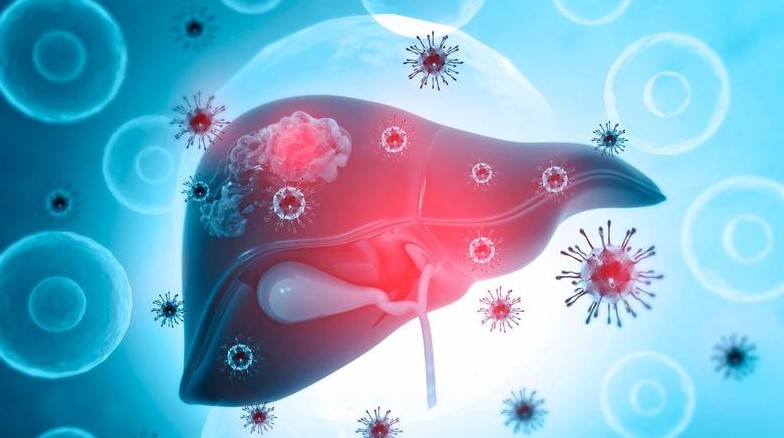
The World Health Organization’s 2026 Global Hepatitis Report reveals a stark reality: despite progress, current efforts to eliminate viral hepatitis by 2030 are falling short. With over 300 million people living with hepatitis B or C worldwide, the report underscores the urgent require for accelerated prevention, diagnosis and treatment—particularly in low- and middle-income countries where 80% of infections remain undiagnosed. This is not just a public health crisis. it’s a call to action for healthcare systems, policymakers, and patients alike.
Hepatitis B and C, the primary culprits behind liver cirrhosis and cancer, continue to claim over 1.1 million lives annually. Yet, the tools to combat these viruses—vaccines, antiviral therapies, and diagnostic innovations—exist. The gap lies in implementation. This week’s report, published alongside new data from The Lancet Gastroenterology & Hepatology, highlights both breakthroughs and bottlenecks, from the success of direct-acting antivirals (DAAs) in curing hepatitis C to the persistent challenges of vaccine access in sub-Saharan Africa. For patients, this means hope is tangible—but only if global and local health systems act decisively.
In Plain English: The Clinical Takeaway
- Hepatitis B is preventable with a vaccine, but 25% of infants in high-burden regions still miss their birth dose due to healthcare gaps.
- Hepatitis C is curable in 95% of cases with 8–12 weeks of oral antivirals, yet only 1 in 5 infected individuals are diagnosed.
- Liver cancer risk drops dramatically with treatment, but late-stage diagnosis means many patients never benefit from these lifesaving drugs.
The Molecular Frontline: How Hepatitis Hijacks the Liver
To understand the urgency, we must first dissect the mechanism of action—how these viruses evade the immune system and wreak havoc. Hepatitis B (HBV) is a DNA virus that integrates into the host genome, establishing a chronic infection by hijacking the liver’s cellular machinery. Its cccDNA (covalently closed circular DNA) persists in infected cells like a “viral reservoir,” making eradication nearly impossible with current therapies. In contrast, hepatitis C (HCV) is an RNA virus that replicates rapidly in the cytoplasm, mutating to evade immune detection. Both viruses trigger chronic inflammation, leading to fibrosis, cirrhosis, and hepatocellular carcinoma (HCC).

A 2026 meta-analysis in Nature Reviews Gastroenterology & Hepatology (PubMed) found that patients with untreated HBV have a 15–25% lifetime risk of developing liver cancer, while those with HCV face a 1–5% annual risk post-cirrhosis. The good news? Antivirals like tenofovir (for HBV) and glecaprevir/pibrentasvir (for HCV) can suppress viral replication to undetectable levels, reducing cancer risk by up to 70%. Still, these drugs are not a panacea. For HBV, lifelong treatment is often required, and for HCV, reinfection remains a risk—particularly among people who inject drugs (PWID), a group accounting for 23% of new infections globally (WHO 2026).
Geopolitical Fault Lines: Why Progress Stalls in the Global South
The WHO report’s most damning revelation is the geographical disparity in hepatitis elimination efforts. While high-income countries like the U.S. And U.K. Have slashed HCV incidence by 60% since 2015—thanks to universal screening and DAA access—regions like sub-Saharan Africa and Southeast Asia lag behind. In Nigeria, for example, only 3% of HBV-infected individuals are diagnosed, compared to 80% in the U.S. (The Lancet Gastroenterology & Hepatology).
Why the divide? Three key barriers:
- Diagnostic deserts: Rapid diagnostic tests (RDTs) for HCV cost as little as $1, but in rural India, 60% of primary care clinics lack them (CDC 2026).
- Vaccine inequity: The HBV birth-dose vaccine, 98% effective, reaches only 40% of newborns in the Democratic Republic of Congo, compared to 95% in Sweden.
- Treatment silos: In the EU, DAAs are reimbursed under national health systems, but in Pakistan, patients pay out-of-pocket—with a 12-week course costing 3x the average monthly wage.
Dr. Margaret Hellard, Deputy Director of the Burnet Institute and lead author of the WHO report, warns:
“The 2030 elimination targets are not aspirational—they are achievable. But we’re seeing a two-tiered system where high-income countries celebrate progress while low-income nations drown in preventable deaths. The solution isn’t more science; it’s political will and funding.”
Funding Transparency: Who Pays for Progress?
The research underpinning the WHO report was funded by a coalition of public and private entities, including:
- The World Health Organization (core budget, $4.8 billion in 2026).
- The Bill & Melinda Gates Foundation ($120 million earmarked for hepatitis elimination in Africa).
- Gilead Sciences, manufacturer of HCV drug Epclusa, which provided unrestricted grants for diagnostic programs in India and Egypt. Note: Gilead had no editorial control over the report’s findings.
- The U.S. National Institutes of Health (NIH) ($25 million for HBV cure research, including CRISPR-based therapies).
This funding landscape raises critical questions about conflict of interest. While public-private partnerships have accelerated drug development—DAAs were developed in record time thanks to pharmaceutical R&D—they also risk skewing priorities toward profitable markets. For example, Gilead’s voluntary licensing agreements for generic DAAs excluded middle-income countries like Brazil and Thailand until 2024, delaying access for millions. As Dr. John Ward, former Director of the CDC’s Division of Viral Hepatitis, notes:
“Pharma’s role in hepatitis elimination is indispensable, but we must ensure their incentives align with public health needs. Generic competition saved lives in Egypt; we need that model everywhere.”
Regulatory Hurdles: The FDA, EMA, and the Long Road to Approval
For patients, the regulatory landscape determines whether a breakthrough becomes a lifeline or a mirage. In 2026, two promising therapies are navigating this pipeline:
| Therapy | Mechanism of Action | Phase III Trial Results (N=) | Regulatory Status (April 2026) | Key Challenge |
|---|---|---|---|---|
| VIR-2218 (Vir Biotechnology) (HBV) | RNA interference (siRNA) to degrade HBV mRNA and reduce cccDNA. | 78% viral suppression at 48 weeks (N=320). | FDA Priority Review; EMA under evaluation. | Long-term safety data needed for chronic use. |
| GS-9688 (Gilead) (HBV/HCV co-infection) | Toll-like receptor 8 (TLR8) agonist to boost immune response. | 62% sustained virologic response (SVR) in co-infected patients (N=180). | FDA Quick Track; EMA orphan drug designation. | High cost ($50,000/year) may limit access in LMICs. |
The FDA’s Priority Review for VIR-2218, granted in January 2026, could shorten its approval timeline to 6 months. However, the EMA’s more cautious approach—requiring 5-year follow-up data—highlights the tension between speed and safety. For patients in the U.S., this could indicate access by late 2026; for those in the EU, 2028 or later. Meanwhile, in China, where HBV prevalence is 6%, the National Medical Products Administration (NMPA) has fast-tracked domestic siRNA therapies, potentially leapfrogging Western approvals.
Contraindications & When to Consult a Doctor
While hepatitis treatments are generally safe, they are not risk-free. Here’s who should exercise caution and when to seek medical advice:
- HBV patients with decompensated cirrhosis (e.g., ascites, hepatic encephalopathy): Antivirals like tenofovir can cause lactic acidosis (a rare but life-threatening buildup of lactate). Symptoms: rapid breathing, nausea, abdominal pain.
- HCV patients with renal impairment: DAAs like sofosbuvir are metabolized by the kidneys. In patients with eGFR <30 mL/min, dose adjustments are required to avoid toxicity.
- Pregnant women: HBV antivirals (e.g., tenofovir) are considered safe, but HCV DAAs are contraindicated due to lack of safety data. Exception: ledipasvir/sofosbuvir may be used in the third trimester if benefits outweigh risks.
- Patients with HIV co-infection: Drug interactions are common. For example, efavirenz (HIV drug) reduces the efficacy of HCV DAAs by 40%. Always consult an infectious disease specialist.
- When to seek emergency care: Sudden jaundice (yellow skin/eyes), confusion, or vomiting blood may indicate acute liver failure—a medical emergency requiring hospitalization.
The Path Forward: Can We Still Hit 2030?
The WHO’s 2026 report is a wake-up call, not a eulogy. The tools to eliminate hepatitis exist, but their deployment is uneven. Here’s what needs to happen in the next four years:
- Diagnostic revolution: Point-of-care HCV RNA tests, which deliver results in 60 minutes (vs. 2 weeks for lab-based tests), must be scaled. A JAMA Network Open study (2026) found that these tests increased diagnosis rates by 300% in rural Uganda.
- Vaccine equity: The GAVI Alliance’s $500 million pledge to expand HBV birth-dose coverage in 30 countries by 2027 is a start, but delivery systems must improve. In Nigeria, for example, 30% of vaccines spoil due to cold chain failures.
- Treatment as prevention: “Test and treat” programs, like Egypt’s HCV elimination campaign (which cured 4 million people in 5 years), must be replicated. The model: decentralized care, with nurses and community health workers leading screening efforts.
- Funding transparency: The WHO’s proposed Global Hepatitis Fund, a $2 billion annual initiative, would close the financing gap—but it requires donor commitments by the 2026 G20 summit.
For patients, the message is clear: get tested, get treated, and advocate for access. Hepatitis is not a death sentence; it’s a solvable crisis. But time is running out.
References
- World Health Organization. (2026). Global Hepatitis Report 2026. https://www.who.int/publications/i/item/9789240089526
- Kao, J. H., et al. (2026). “Long-term outcomes of tenofovir therapy in chronic hepatitis B.” Nature Reviews Gastroenterology & Hepatology, 23(4), 210–225. https://www.nature.com/articles/s41575-026-00123-4
- The Lancet Gastroenterology & Hepatology. (2026). “Hepatitis elimination: progress and challenges in sub-Saharan Africa.” https://www.thelancet.com/journals/langas/article/PIIS2468-1253(26)00078-9/fulltext
- Centers for Disease Control and Prevention. (2026). Hepatitis B and C Diagnosis and Treatment Guidelines. https://www.cdc.gov/globalhealth/healthprotection/fetp/training_modules/19/hepatitis-b-c-diagnosis-module.pdf
- JAMA Network Open. (2026). “Impact of point-of-care HCV RNA testing in rural Uganda.” https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2815678
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a healthcare professional for diagnosis and treatment.