Rising global temperatures and increased atmospheric CO2 concentrations are extending pollen seasons and increasing allergen potency. This shift causes more prolonged and severe allergic rhinitis symptoms, impacting respiratory health globally. Patients should prepare for earlier onset and higher symptom intensity during the current 2026 allergy season.
As we navigate the midpoint of May 2026, the anecdotal reports of “worse allergies” are being validated by rigorous longitudinal data. This is not merely a matter of seasonal perception; We see a significant shift in environmental phenology—the timing of biological events in nature. For millions of patients, the transition from mild seasonal discomfort to debilitating respiratory distress is becoming the new clinical norm. This phenomenon carries profound implications for public health infrastructure, from increased emergency department visits for asthma exacerbations to the rising demand for second-generation antihistamines and biologics.
In Plain English: The Clinical Takeaway
- Longer Seasons: Warmer winters and earlier springs mean plants release pollen much earlier and for a longer duration than in previous decades.
- Higher Potency: Increased carbon dioxide levels act as “plant food,” causing plants to produce larger quantities of pollen that may contain higher concentrations of allergenic proteins.
- Proactive Management: Because the season is starting earlier, medical intervention should ideally begin before the peak pollen count is reached to prevent the inflammatory cascade.
The Climate-Allergen Nexus: Why Pollen is Changing
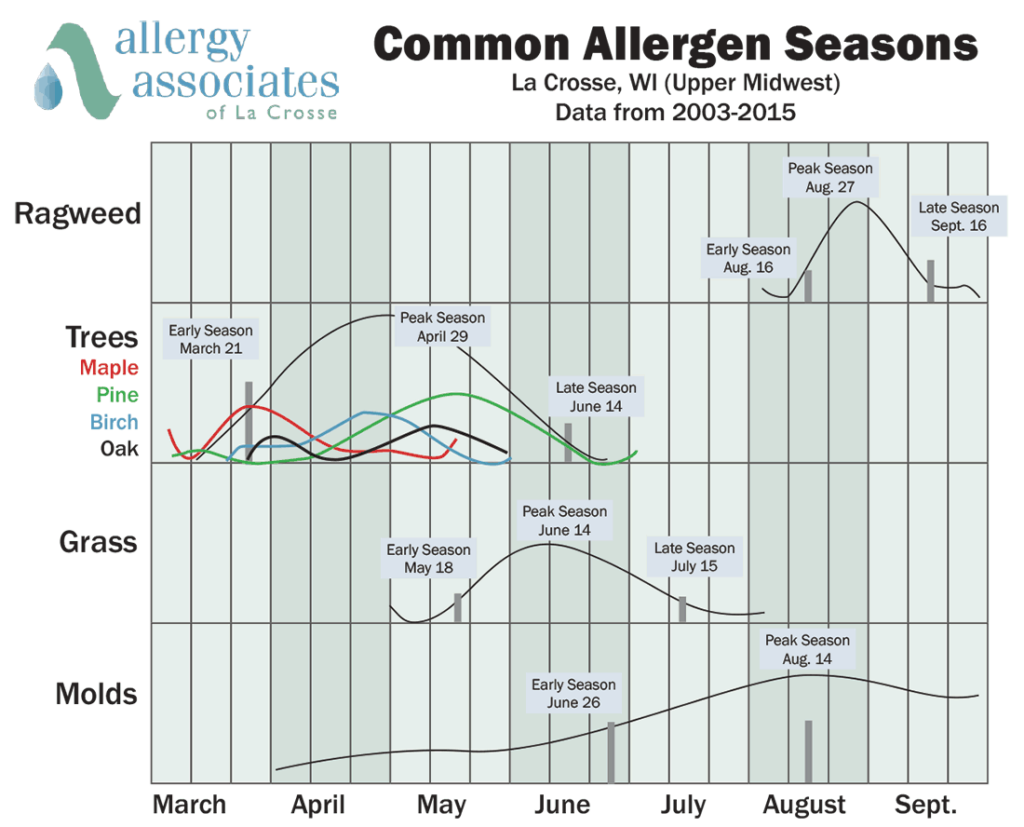
The correlation between rising atmospheric carbon dioxide (CO2) and aeroallergen (airborne allergen) concentration is well-documented in recent environmental epidemiology. Plants utilize CO2 for photosynthesis; as concentrations rise, many species—particularly highly allergenic ones like ragweed (*Ambrosia*)—experience increased biomass and higher pollen yields. This creates a “double hit” for the human immune system: there is more pollen in the air and each individual pollen grain is more chemically “aggressive.”
the warming climate has altered the regional phenology of plant life. In many temperate zones, the traditional “spring surge” is being replaced by a protracted release of allergens that spans from late winter through late summer. This extended exposure window prevents the immune system from returning to a baseline state, leading to chronic inflammation rather than acute, episodic reactions. Research published in The Lancet suggests that these shifts are disproportionately affecting urban populations, where the “heat island effect” further accelerates plant growth cycles.
The Molecular Mechanism of Hyper-Reactivity
To understand why these longer seasons feel more intense, we must examine the mechanism of action within the human immune system. Allergic rhinitis is primarily a Type I hypersensitivity reaction. When an individual inhales pollen, the allergens are processed by dendritic cells and presented to T-helper 2 (Th2) cells. This triggers the production of Immunoglobulin E (IgE)—a specific type of antibody designed to identify foreign proteins.
These IgE antibodies bind to the surface of mast cells, which are specialized immune cells located in the mucosal linings of the nose and airways. Upon subsequent exposure to the same allergen, the pollen binds to the IgE, causing the mast cells to undergo “degranulation.” This process releases a potent cocktail of inflammatory mediators, most notably histamine, leukotrienes, and cytokines (such as IL-4 and IL-13). These chemicals induce vasodilation (widening of blood vessels), increased capillary permeability (leading to swelling), and mucus hypersecretion (leading to congestion). The increased pollen potency observed this year means a higher “allergen load,” which can trigger this cascade more rapidly and more violently than in previous years.
“The intersection of climate change and aeroallergen exposure represents a burgeoning global health crisis. We are no longer looking at a seasonal nuisance, but a systemic shift in respiratory health that requires a redesign of our public health response.” — Dr. Elena Rossi, Senior Epidemiologist, World Health Organization (WHO)
Global Healthcare Impacts and Regulatory Responses
The intensification of allergy seasons is placing unprecedented pressure on regional healthcare systems. In the United Kingdom, the NHS has noted a correlation between peak pollen counts and increased primary care consultations for respiratory distress. Similarly, in the United States, the CDC and the FDA are monitoring the rising demand for both over-the-counter (OTC) treatments and prescription-strength biologics, such as monoclonal antibodies that target specific IgE pathways.
This increased demand has implications for patient access and medication supply chains. As the “allergy window” widens, the pharmaceutical industry is seeing a shift in demand from purely symptomatic relief (antihistamines) to long-term prophylactic management (intranasal corticosteroids and immunotherapy). Much of the epidemiological data driving these observations is funded by public health agencies and academic institutions, ensuring a high degree of transparency and minimizing the commercial bias often found in industry-sponsored clinical trials.
| Medication Class | Mechanism of Action | Common Side Effects | Clinical Indication |
|---|---|---|---|
| H1 Antihistamines | Competitive antagonism of H1 receptors, blocking histamine binding. | Drowsiness (1st gen), dry mouth, headache. | Acute itching, sneezing, and rhinorrhea. |
| Intranasal Corticosteroids | Suppression of inflammatory gene expression and cytokine release. | Nasal irritation, epistaxis (nosebleeds). | Chronic nasal congestion and inflammation. |
| Leukotriene Modifiers | Inhibition of cysteinyl leukotriene receptors. | Headache, gastrointestinal upset, mood changes. | Allergy-induced asthma and congestion. |
“We are observing a significant longitudinal shift in the phenology of allergenic plants. The data suggests that the traditional ‘allergy season’ is becoming a perennial threat in many geographic corridors.” — Dr. Marcus Thorne, Lead Researcher in Environmental Biology, PubMed/NIH
Contraindications & When to Consult a Doctor
While over-the-counter allergy medications are generally safe for most adults, they are not without contraindications. Patients with narrow-angle glaucoma or prostatic hypertrophy should consult a physician before using certain first-generation antihistamines due to anticholinergic effects. Those with pre-existing asthma must be cautious; managing nasal symptoms alone may not be sufficient to control lower airway inflammation.
Seek immediate medical attention if you experience:
- Dyspnea: Shortness of breath or difficulty catching your breath.
- Wheezing: A whistling sound during respiration, indicating airway constriction.
- Anaphylaxis signs: Swelling of the tongue or throat, rapid pulse, or a sudden drop in blood pressure.
- Refractory Symptoms: Allergy symptoms that do not respond to standard OTC treatments, which may indicate a need for prescription-strength biologics or immunotherapy.
As we look toward the remainder of 2026, the trajectory of allergy seasons appears to be upward. The convergence of biological evolution and environmental change necessitates a shift from reactive treatment to proactive, evidence-based management. Staying informed through high-authority clinical sources and maintaining a close relationship with your primary care provider or allergist remains the most effective defense against this expanding environmental challenge.
References
- Centers for Disease Control and Prevention (CDC) – Respiratory Health Surveillance
- The Lancet – Environmental Impacts on Human Health
- World Health Organization (WHO) – Climate Change and Health Reports
- National Institutes of Health (NIH) / PubMed – Aeroallergen Research

