Porcelain veneers fail primarily due to improper bonding techniques, excessive tooth reduction, or patient-specific factors like bruxism. These failures manifest as chipping, debonding, or recurrent decay, typically stemming from a breach in the adhesive seal or mechanical stress that exceeds the material’s structural limits.
The democratization of aesthetic dentistry, fueled by social media trends, has created a precarious gap between consumer expectation and clinical reality. Whereas the desire for a “perfect smile” is universal, the biological cost of achieving it is often understated. When a veneer fails, it is rarely a failure of the porcelain itself, but rather a failure of the interface between the synthetic material and the living tooth structure.
In Plain English: The Clinical Takeaway
- Veneers are not permanent: They are long-term restorations that typically require replacement every 10 to 15 years.
- The “Bond” is everything: If the adhesive seal is compromised, bacteria enter the gap, leading to rapid tooth decay under the porcelain.
- Biology wins: If you grind your teeth (bruxism), no amount of high-grade porcelain can prevent eventual fractures without a protective night guard.
The Bio-Mechanical Failure: Why the Bond Breaks
At the heart of every veneer failure is the compromise of the adhesive interface. The process of bonding involves “etching” the enamel—using a mild acid to create microscopic pores—which allows the resin cement to lock into the tooth. What we have is known as the mechanism of action for micromechanical retention. When this process is rushed or contaminated by saliva during placement, the bond strength is diminished.
One of the most critical clinical failures is marginal leakage. This occurs when a microscopic gap forms at the edge (margin) of the veneer. Once the marginal integrity is lost, oral fluids and bacteria infiltrate the space, leading to secondary caries—cavities that form underneath the restoration. Because the porcelain hides the tooth, these cavities often go undetected until the veneer falls off or the tooth becomes abscessed.
the issue of polymerization shrinkage—the slight contraction of the bonding resin as it hardens under a curing light—can create internal stresses. If the clinician does not manage this shrinkage, it can lead to “micro-cracks” in the porcelain or the enamel, predisposed to failure under the pressure of mastication (chewing).
The Conflict Between “No-Prep” Trends and Longevity
A significant trend in 2026 is the rise of “no-prep” veneers, marketed as a conservative alternative. However, clinical data suggests a complex trade-off. By adding porcelain on top of existing enamel without removing any tooth structure, the resulting tooth profile becomes “over-contoured.” This increases the bulk of the tooth, which alters the occlusion—how the upper and lower teeth meet.
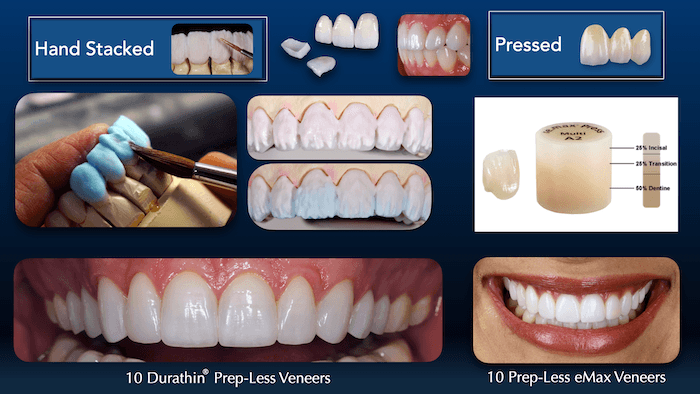
When the occlusion is disrupted, the veneer is subjected to lateral forces it wasn’t designed to handle. This often results in “shear failure,” where the veneer is literally snapped off the tooth surface. Conversely, aggressive “over-preparation” removes too much enamel, reaching the dentin. Since resin bonds significantly weaker to dentin than to enamel, the long-term stability of the restoration is compromised.
| Veneer Type | Tooth Reduction | Primary Failure Mode | Estimated Lifespan |
|---|---|---|---|
| Traditional Porcelain | 0.3mm – 0.7mm | Marginal Leakage/Chipping | 10-15 Years |
| No-Prep/Minimal Prep | 0mm – 0.3mm | Debonding/Over-contouring | 5-10 Years |
| Composite Resin | Minimal | Staining/Wear/Fracture | 3-7 Years |
Global Regulatory Disparities and the Danger of Dental Tourism
The surge in veneer failures is closely linked to the rise of dental tourism, particularly in regions where regulatory oversight of materials is lax. In the United States, the FDA regulates the biocompatibility of dental resins and ceramics. In Europe, the EMA provides similar frameworks. However, in many “discount” dental hubs, materials may lack these certifications, leading to higher rates of gingival inflammation and allergic reactions to unapproved monomers.
the lack of continuity of care is a systemic risk. A veneer placed in another country without a local follow-up protocol means that minor chipping or marginal gaps are not caught during routine check-ups. By the time a patient in the UK or US notices a problem, the underlying tooth may have suffered extensive decay.
“The biological cost of a ‘perfect’ smile is often paid in the loss of healthy enamel. Once we remove that tissue, we are managing a chronic condition, not providing a permanent cure.” — Dr. Julian Thorne, Lead Researcher in Biomaterials and Prosthodontics.
It is essential to note that much of the research promoting specific “ultra-strong” porcelain brands is funded by the manufacturers themselves, such as Ivoclar or 3M. While the materials are clinically sound, the marketing often obscures the fact that the clinician’s technique—not the material’s strength—is the primary determinant of success.
The Role of Bruxism and Parafunctional Habits
Even a perfectly placed veneer can fail if the patient suffers from bruxism (chronic teeth grinding). The forces generated during nocturnal grinding can exceed 250 pounds per square inch, far surpassing the compressive strength of dental porcelain. This leads to “fatigue failure,” where the material develops microscopic stress fractures over time until it catastrophically fails.
To mitigate this, evidence-based protocols now mandate the apply of a hard occlusal guard (night guard) for all veneer patients. Without this, the statistical probability of failure increases by nearly 40% within the first five years. Research available via PubMed indicates that longitudinal success rates are significantly higher in patients who maintain a strict nocturnal protection regimen.
Contraindications & When to Consult a Doctor
Veneers are not suitable for every patient. You should avoid this procedure or seek a second opinion if you have:
- Severe Bruxism: If you wake up with a sore jaw or worn-down teeth, veneers may fail rapidly.
- Active Periodontal Disease: Gum disease compromises the “biological width,” making it impossible to achieve a stable marginal seal.
- Severe Malocclusion: If your teeth are significantly misaligned, orthodontic treatment (braces/aligners) must precede veneers to avoid unnatural tooth shaping.
Consult a professional immediately if you experience: A sudden “rough” edge on a veneer, a dark line appearing at the gumline (indicating leakage), or localized sensitivity to hot and cold, which may signal a crack in the porcelain or underlying decay.
the longevity of porcelain veneers depends on a synergy between high-precision clinical execution and patient compliance. As we move further into 2026, the shift is moving away from “maximum aesthetics” toward “biomimetic dentistry”—the practice of mimicking the natural tooth’s structure and function to ensure the restoration lasts a lifetime, rather than a decade.
References
- The Journal of the American Dental Association (JADA) – Clinical guidelines on adhesive dentistry.
- National Center for Biotechnology Information (NCBI) – Longitudinal studies on porcelain veneer survival rates.
- World Health Organization (WHO) – Global reports on oral health and dental material safety.
- American Dental Association (ADA) – Standards for cosmetic restorative procedures.

