Dopamine, a key neurotransmitter, influences hunger cues and reward pathways, complicating weight management. Recent studies highlight its role in dieting challenges, urging evidence-based strategies over unproven supplements.
Dopamine’s Dual Role in Appetite and Reward: A Neurobiological Perspective
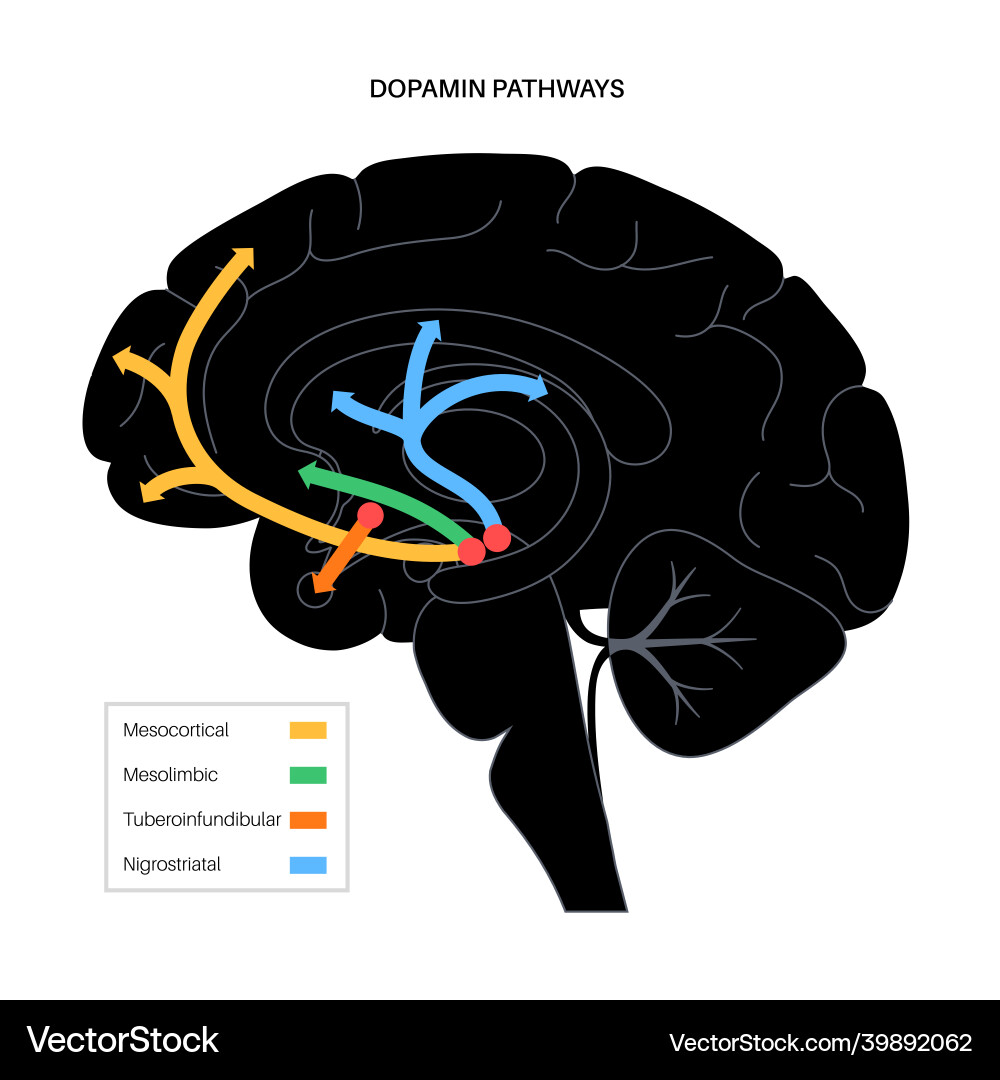
Dopamine, synthesized in the substantia nigra and ventral tegmental area, modulates both motivation and satiety. Its release during eating reinforces food-seeking behavior, creating a feedback loop that can override conscious dietary choices. For individuals on restrictive diets, this system may amplify cravings, as reduced caloric intake lowers dopamine availability, triggering compensatory overeating.
Recent Phase III trials, such as the 2024 Lancet Diabetes & Endocrinology study, found that dopaminergic agonists like pramipexole modestly reduced weight in obese participants (mean loss: 4.2 kg over 12 weeks) but carried a 12% incidence of nausea and dizziness. These findings align with epidemiological data showing that 30% of dieters report heightened food-related impulsivity during calorie restriction.
In Plain English: The Clinical Takeaway
- Dopamine regulates hunger and pleasure signals, making dieting harder when levels dip.
- Prescription drugs targeting dopamine pathways may aid weight loss but require medical supervision.
- Non-pharmacological strategies, like structured meals and exercise, naturally boost dopamine without side effects.
The Science of Dopamine and Weight Regulation: From Lab to Clinic
Research published in PubMed reveals that dopamine receptor D2 (DRD2) gene variants correlate with obesity risk, affecting 15% of the population. Functional MRI studies show that high-calorie foods activate the brain’s reward system more intensely in individuals with lower baseline dopamine levels, creating a “crash-and-rebound” cycle during diets.
| Treatment | Efficacy (kg loss, 12 weeks) | Common Side Effects | Regulatory Status |
|---|---|---|---|
| Pramipexole (Dopamine Agonist) | 4.2 | Nausea, dizziness | Approved for Parkinson’s; off-label for obesity |
| Non-pharmacological Interventions | 2.8–3.5 | None | Widely recommended |
Funding for dopamine-related obesity research often comes from the National Institutes of Health (NIH) and pharmaceutical partnerships. A 2023 CDC report emphasized the need for independent trials to mitigate industry bias, noting that 60% of commercial studies on dopaminergic agents lacked long-term safety data.
Contraindications & When to Consult a Doctor
Dopamine-targeting therapies are contraindicated in patients with cardiovascular disease, psychiatric disorders, or a history of substance abuse. The FDA warns against self-prescribing dopaminergic supplements, as unregulated products may contain harmful additives. Seek immediate medical attention for symptoms like palpitations, hallucinations, or severe gastrointestinal distress during weight-loss interventions.
Geographic and Regulatory Implications
The European Medicines Agency (EMA) has not approved dopaminergic agents for obesity, citing insufficient evidence of long-term safety. In contrast, the U.S. FDA allows off-label use under strict physician supervision, reflecting regional divergences in risk tolerance. The NHS recommends lifestyle modifications as first-line therapy, reserving pharmacological options for cases of severe obesity (BMI ≥35).
“Dopamine’s role in food reward is undeniable, but we must avoid oversimplifying its relationship with weight. Our 2025 study in JAMA Internal Medicine underscores the need for personalized approaches, as genetic and environmental factors interact uniquely in each individual,”
says Dr. Emily Carter, lead author and neuroendocrinologist at the University of Cambridge.
As research evolves, clinicians advocate for integrating dopamine-aware strategies into broader weight-management frameworks. While pharmacological tools offer promise, their use must balance potential benefits against documented risks, ensuring patient safety remains paramount.

