
Why Sony Should Revive Their Classic Franchises
Sony is quietly reviving dormant IPs like Crash Bandicoot and Spyro—not as nostalgia bait, but as a strategic pivot toward modular game engines built on Unreal Engine 5.2’s Nanite and ... Read More
Saturday Edition
Stay updated with Archyde – your source for breaking news, global headlines, economy, entertainment, health, technology, and sports. Fresh stories daily.

Sony is quietly reviving dormant IPs like Crash Bandicoot and Spyro—not as nostalgia bait, but as a strategic pivot toward modular game engines built on Unreal Engine 5.2’s Nanite and ... Read More
Continuous Coverage

Canadian mushroom growers face U.S. Tariffs that could destabilize their market, with industry leaders warning of cascading impacts…
The night sky over Russia’s western front shimmered with a terrifying new kind of fire. At approximately 2:17…
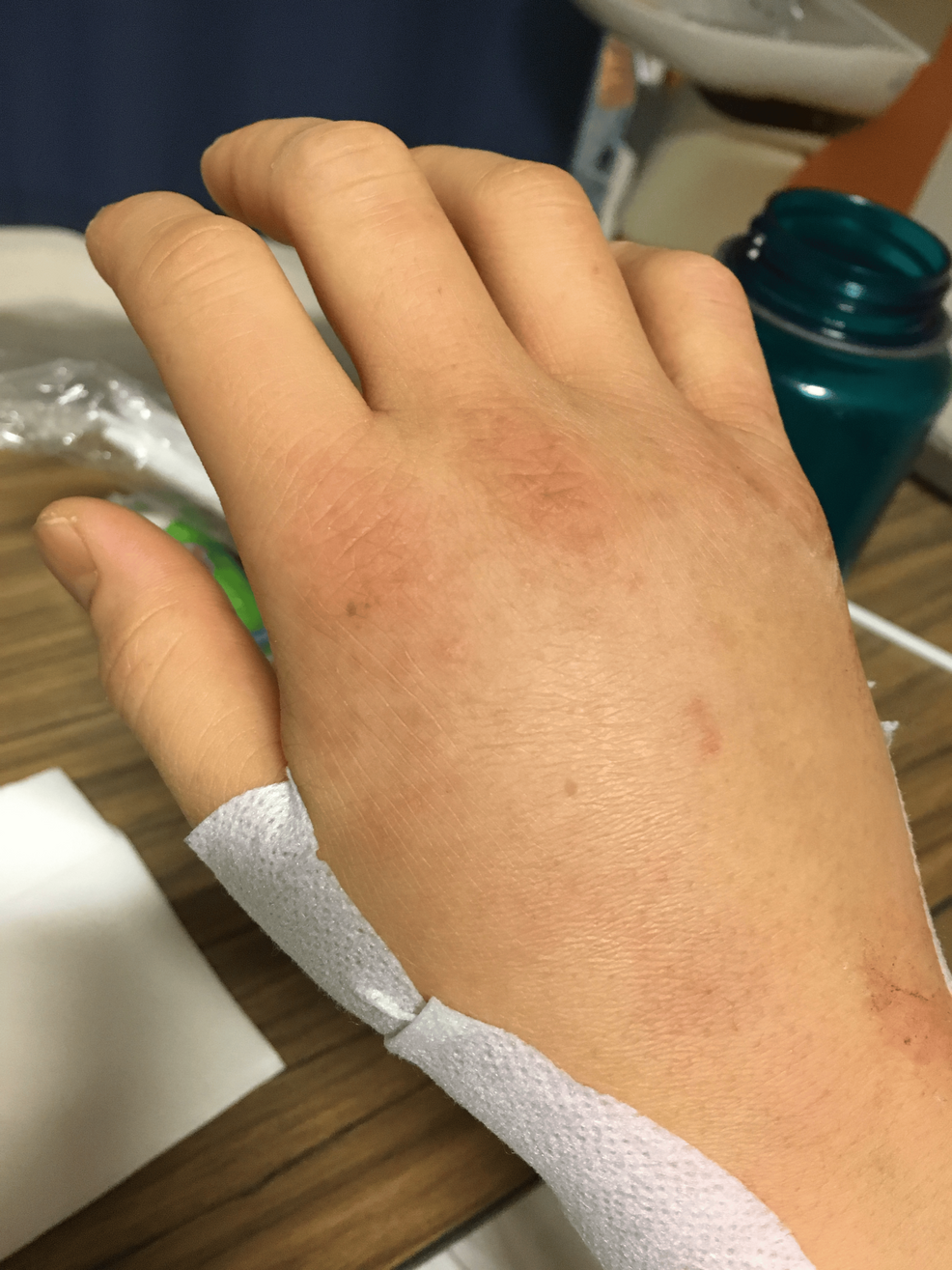
A 32-year-old postpartum woman with undiagnosed complement deficiency developed missed septic arthritis of the wrist—a rare but life-threatening…

World Triathlon Championship Series (WTCS) Yokohama 2026 delivered tactical revelations, standout performances, and strategic shifts that redefined the…

Pisces season just dropped its cosmic forecast for May 17, 2026—where Mercury retrograde’s shadow clashes with a rare…

As of May 17, 2026, the Egyptian Pound (EGP) is navigating a period of heightened volatility, reflecting a…
Global Affairs

Ukraine launched a drone strike on Moscow and Crimea on May 17, 2026, killing at least three people,…
Markets And Money

Poland’s retirement age will rise to 68—a sudden shift from 67—effective immediately, catching markets off guard. The move,…
Digital Culture

Playground Games’ Forza Horizon 6 isn’t just another open-world racer—it’s a technical marvel that’s already shattered its predecessor’s…
Science And Wellbeing

LeBron James, the NBA’s all-time leading scorer, faces a career crossroads this offseason: whether to accept a reduced…
Screen And Sound

Bulgaria’s Dara triumphed at Eurovision 2026 in Vienna, securing the country’s first victory since its 2005 debut with…
Fixtures And Form

Philip Pertl and Sebastian Röser have claimed the 2026 Austrian State Championship title in the Apfelland Triathlon, securing…