
Super Furry Animals Reunite After Decade: Live Tour Kicks Off in Ireland
The first time Gruff Rhys took the stage in Dublin tonight, the air in the venue crackled like a live wire. Ten years of silence had turned the Super Furry ... Read More

Saturday Edition
Stay updated with Archyde – your source for breaking news, global headlines, economy, entertainment, health, technology, and sports. Fresh stories daily.

The first time Gruff Rhys took the stage in Dublin tonight, the air in the venue crackled like a live wire. Ten years of silence had turned the Super Furry ... Read More
Continuous Coverage

A recent legislative debate in the South Korean National Assembly regarding constitutional amendments has reignited critical discussions on…

The US administration has declared the conflict in Iran concluded to preempt a constitutional challenge from Congress regarding…

Germany’s rail operator Deutsche Bahn (DB) is slashing last-minute train fares to a record low of €6.99 for…

The air inside Madison Square Garden during a playoff series doesn’t just vibrate; it bruises. We see a…
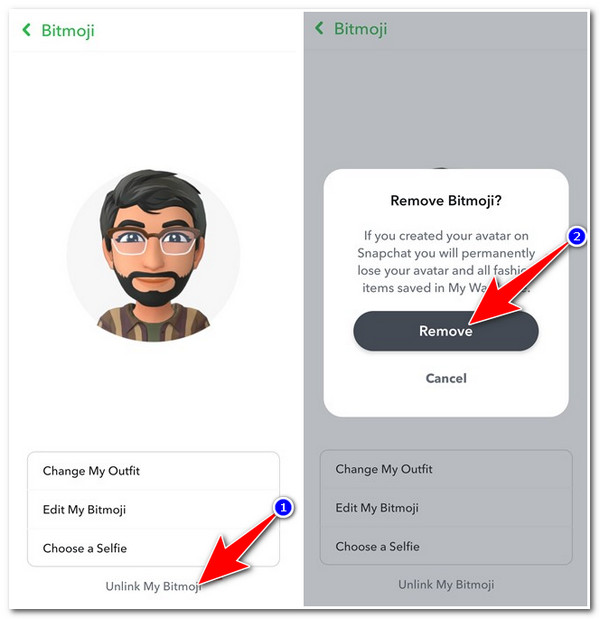
Snapchat quietly rolled out a hidden toggle for Bitmoji removal in its latest beta—just as regulators scrutinize user…

Bonnie Tyler is currently recuperating following an emergency intestinal surgery. While specific clinical details remain private, emergency bowel…
Global Affairs

As Iran awaits a formal response to a U.S. Proposal delivered late Tuesday, Tehran has denied involvement in…
Markets And Money

OpenAI co-founder Greg Brockman revealed in a BBC interview that Elon Musk’s 2018 decision to exit the company’s…
Digital Culture

NASA’s Perseverance rover has identified the “Crocodile Bridge,” a distinct, eroded rock formation on the Jezero Crater rim.…
Science And Wellbeing

New research reveals that specific inflammatory genes act as a molecular bridge between metabolic diseases, such as Type…
Screen And Sound
Alibaba has launched the Wan 2.2 Turbo Infinite Image-to-Video API via Atlas Cloud, enabling creators to transform static…
Fixtures And Form

Dayanara Campos, Georgetown’s senior guard, has been named First Team All-BIG EAST after a breakout 2026 campaign that…