
Vivien Leigh: Life and Legacy of a British Icon
We have all seen the image: the porcelain skin, the arched brows, and that defiant, emerald-eyed gaze that defined an entire era of cinema. Vivien Leigh was the ultimate “English ... Read More

Saturday Edition
Stay updated with Archyde – your source for breaking news, global headlines, economy, entertainment, health, technology, and sports. Fresh stories daily.

We have all seen the image: the porcelain skin, the arched brows, and that defiant, emerald-eyed gaze that defined an entire era of cinema. Vivien Leigh was the ultimate “English ... Read More
Continuous Coverage

Netflix’s Man on Fire remake, arriving this April 2026, revitalizes the protector-thriller genre by blending gritty realism with…
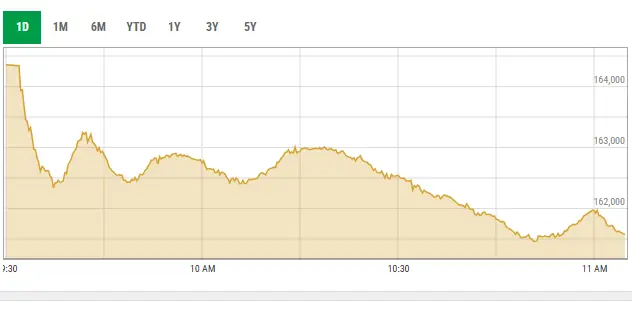
The KSE-100 index of the Pakistan Stock Exchange (PSX: KSE100) declined 3,449.98 points (2.08%) on Thursday, closing at…

Imagine a world where the morning commute doesn’t involve a steering wheel or a subway ticket, but a…

Google is integrating an AI-driven Speech Practice feature into Google Translate to celebrate its 20th anniversary. This update…

England captain Leah Williamson has officially signed a contract extension with Arsenal, securing her future at the Emirates.…

Daniel Blake’s death in Daredevil: Born Again Season 2 serves as a stark clinical illustration of hemorrhagic shock…
Global Affairs

BYD has signaled a bold pivot into the ultra-luxury market by selling the Yangwang U9 Xtreme for over…
Markets And Money

Quebec grocery retailers are implementing aggressive price cuts on proteins and dairy as of late April 2026. This…
Digital Culture

TikTok’s recommendation engine is fueling a migration crisis by amplifying fraudulent “guides” through engagement-biased algorithms. By prioritizing high-retention…
Science And Wellbeing

Long Covid, clinically termed Post-Acute Sequelae of SARS-CoV-2 (PASC), remains a global health challenge six years after the…
Screen And Sound

Kyotographie is an annual international photography festival in Kyoto, Japan, transforming historic sites into immersive galleries. The 2026…
Fixtures And Form

Commandment has emerged as the definitive favorite for the 2026 Kentucky Derby following a dominant 6 ¾ length…