Bi-portal endoscopic spine surgery (BESS) is an emerging minimally invasive technique used to treat lumbar disc herniation and spinal stenosis. By utilizing two small incisions for simultaneous viewing and instrumentation, surgeons can precisely remove compressive tissue, reducing recovery times and muscle trauma compared to traditional open-back surgeries.
For millions suffering from chronic lower back pain, the choice between conservative management and invasive surgery often feels like a gamble. The shift toward bi-portal endoscopy represents a critical evolution in neurosurgery, moving away from the “maximal exposure” philosophy toward a targeted, tissue-preserving approach. This transition is not merely about smaller scars; it is about preserving the structural integrity of the multifidus muscles and reducing the incidence of post-operative scarring, which can lead to permanent stiffness.
In Plain English: The Clinical Takeaway
- Less Damage: Instead of one large cut, doctors use two tiny holes to fix the spine, meaning less muscle cutting and faster healing.
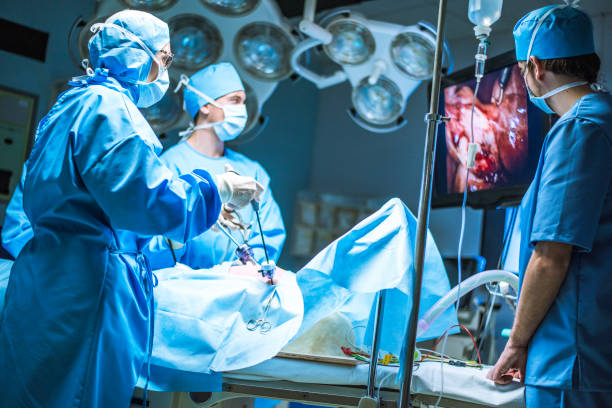
- Better View: Surgeons use a high-definition camera to spot the nerves clearly, making the removal of “slipped discs” more precise.
- Faster Return: Most patients experience a quicker return to daily activities and less immediate post-operative pain.
The Mechanism of Action: How Bi-Portal Endoscopy Differs from Traditional Laminectomy
To understand the clinical advantage of BESS, one must first understand the traditional laminectomy—a procedure where a surgeon removes the lamina (the back part of the vertebra) to create space for the spinal cord. While effective, this often requires stripping muscles away from the bone, which can trigger significant inflammation and long-term instability.
BESS operates on a different principle: the bi-portal approach. One portal serves as the “eye” (the endoscope), providing a continuous, high-resolution view of the surgical field. The second portal serves as the “hand,” allowing the surgeon to insert micro-instruments to perform the decompression. This separation of visualization and instrumentation allows for a wider range of motion and a more comprehensive removal of the pathology without the need for extensive tissue retraction.
The mechanism of action here is the minimization of the “surgical footprint.” By avoiding the massive retraction of the paraspinal muscles, BESS reduces the risk of iatrogenic injury—damage caused by the medical intervention itself—and lowers the probability of postoperative epidural fibrosis, where scar tissue binds to the nerve roots.
Comparing Surgical Outcomes: BESS vs. Conventional Microdiscectomy
Clinical data suggests that while both BESS and traditional microdiscectomy are effective at relieving leg pain (radiculopathy), the recovery trajectory differs. In a series of comparative analyses, BESS has demonstrated a statistically significant reduction in hospital stay duration and a lower requirement for opioid analgesics in the first 48 hours post-operation.

| Metric | Conventional Microdiscectomy | Bi-Portal Endoscopy (BESS) |
|---|---|---|
| Incision Size | Approx. 2–5 cm | Two portals (<1 cm each) |
| Muscle Trauma | Moderate (Retraction required) | Minimal (Tunnelling approach) |
| Recovery Time | Weeks to Months | Days to Weeks |
| Blood Loss | Low to Moderate | Incredibly Low |
The efficacy of these procedures is often measured using the Oswestry Disability Index (ODI), a gold-standard tool for quantifying permanent functional disability in spinal patients. Research indexed in PubMed indicates that BESS achieves similar long-term ODI improvement scores as open surgery but with a steeper initial recovery curve, meaning patients return to baseline function faster.
Global Access and Regulatory Landscapes
While BESS is gaining rapid traction in East Asia—particularly in South Korea and Japan—its adoption in Western healthcare systems like the NHS in the UK or through US-based providers is more gradual. This is largely due to the steep learning curve associated with the technique. Unlike open surgery, BESS requires a high degree of spatial awareness and coordination between the two portals.
In the United States, the FDA regulates the endoscopic equipment used in these procedures. While the technique itself is not a “drug” requiring a trial, the devices must meet strict safety standards. The primary barrier to global ubiquity is not the lack of efficacy, but the requirement for specialized training. Surgeons must undergo extensive cadaveric labs and proctored cases to avoid dural tears—accidental punctures of the spinal sac.
Regarding funding and bias, much of the early pioneering data on BESS has emerged from university hospitals in Seoul. While these institutions are world-class, many early studies were observational rather than double-blind placebo-controlled (which is impossible in surgery). However, the consistency of results across multiple independent centers suggests a genuine clinical benefit.
“The transition to bi-portal endoscopy represents a paradigm shift in how we approach spinal decompression. We are no longer just removing bone; we are navigating the anatomy with a precision that was previously unattainable in minimally invasive settings.” Dr. Jung-Hwan Choi, Spinal Surgery Specialist
Contraindications & When to Consult a Doctor
BESS is not a universal solution. We find specific contraindications—medical reasons why a patient should not undergo this specific procedure. Patients with severe spinal instability (spondylolisthesis) may require a fusion surgery, which cannot be performed via a simple endoscopic decompression.
Consider seek immediate medical intervention if you experience the following “red flag” symptoms:
- Saddle Anesthesia: Numbness in the groin or buttocks.
- Bowel or Bladder Dysfunction: Sudden loss of control or inability to urinate.
- Progressive Neurological Deficit: Sudden weakness in the legs that prevents walking (Foot drop).
These symptoms may indicate Cauda Equina Syndrome, a surgical emergency that requires immediate decompression regardless of the technique used.
The Future Trajectory of Spinal Intervention
As we move further into 2026, the integration of augmented reality (AR) and real-time robotic guidance is expected to flatten the learning curve for BESS. By overlaying a patient’s MRI directly onto the endoscopic view, surgeons can navigate the spinal canal with millimeter precision, further reducing the risk of nerve root injury.
The objective for the medical community is to move toward “personalized decompression,” where the choice between BESS and traditional methods is dictated by the patient’s specific anatomy and the precise location of the stenosis. For the average patient, the promise of BESS is a return to a pain-free life without the grueling recovery associated with the surgeries of the previous decade.

