Understanding Buffalo Hump and its Connection to Health
A “buffalo hump,” clinically known as dorsal cervical fat pad, is the accumulation of fat at the base of the neck, resembling the hump of a bison. While often benign, its recent increased visibility – particularly in younger populations – is raising concerns as it can be a symptom of underlying conditions like Cushing’s syndrome, HIV-associated lipodystrophy, or, increasingly, a side effect of certain medications, notably protease inhibitors. This article will explore the causes, diagnosis, and management of this condition, providing a comprehensive overview for both patients and healthcare professionals.
The rising incidence of buffalo hump isn’t simply an aesthetic concern. It signals a potential disruption in hormonal balance or metabolic processes, demanding careful investigation. Historically, this condition was primarily associated with Cushing’s syndrome, a rare disorder caused by prolonged exposure to high levels of cortisol. However, the advent of antiretroviral therapy for HIV has introduced a new, significant association: HIV-associated lipodystrophy, where fat distribution is altered, leading to fat accumulation in the neck and abdomen. More recently, clinicians are observing a correlation with certain medications used to treat other conditions, prompting a re-evaluation of risk factors and diagnostic approaches.
In Plain English: The Clinical Takeaway
- What It’s: A buffalo hump is a noticeable fat deposit at the back of your neck. It’s not always serious, but it can be a sign of a health problem.
- Why it matters: It could indicate issues with your hormones, metabolism, or be a side effect of certain medications. Don’t ignore it – see a doctor.
- What to do: If you notice a buffalo hump developing, schedule an appointment with your physician for evaluation and potential testing.
The Pathophysiology: How and Why Buffalo Humps Develop
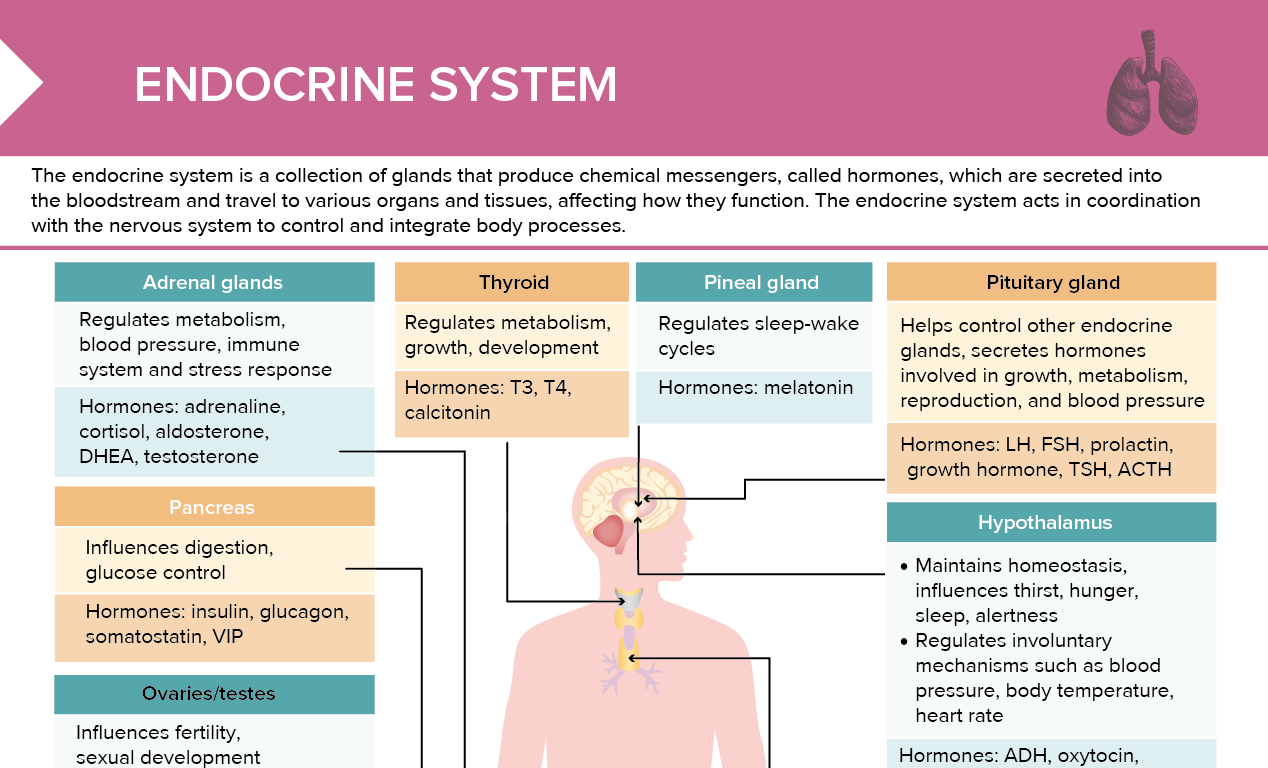
The mechanism of action behind buffalo hump formation varies depending on the underlying cause. In Cushing’s syndrome, excessive cortisol levels disrupt normal fat metabolism, promoting fat deposition in specific areas, including the dorsal cervical region. Cortisol increases lipolysis (fat breakdown) in peripheral areas but simultaneously enhances lipogenesis (fat creation) in the central abdomen and posterior neck. In HIV-associated lipodystrophy, protease inhibitors – a crucial component of HIV treatment – interfere with adipocyte (fat cell) function, leading to fat accumulation and redistribution. These drugs inhibit the enzyme protease, which is involved in the metabolism of triglycerides, ultimately altering fat storage patterns. The precise mechanisms linking other medications to buffalo hump are still under investigation, but likely involve similar disruptions in lipid metabolism and hormonal regulation.

Recent research published in the journal Endocrine Reviews highlights the role of glucocorticoid receptors in mediating the effects of cortisol on fat distribution. [1] studies on HIV-associated lipodystrophy demonstrate that protease inhibitors induce mitochondrial dysfunction in adipocytes, contributing to altered lipid metabolism. [2] The emerging link between other medications and buffalo hump suggests a broader role for drug-induced metabolic alterations in the development of this condition.
Geographical Variations and Public Health Implications
The prevalence of buffalo hump varies geographically, reflecting differences in the incidence of underlying conditions and access to healthcare. In regions with high rates of HIV infection, such as sub-Saharan Africa, HIV-associated lipodystrophy is a significant contributor to the occurrence of buffalo hump. The European Medicines Agency (EMA) has been actively monitoring reports of buffalo hump as a side effect of certain medications, particularly those used in oncology and transplantation. In the United States, the Centers for Disease Control and Prevention (CDC) is tracking trends in metabolic complications associated with HIV treatment, including lipodystrophy. Early detection and management are crucial, as untreated buffalo hump can lead to complications such as neck pain, headaches, and psychological distress.
“We are seeing a concerning rise in reports of buffalo hump, particularly in patients on long-term protease inhibitor therapy. This underscores the need for careful monitoring of metabolic parameters and proactive management strategies to mitigate the risk of this complication.” – Dr. Anthony Fauci, former Director of the National Institute of Allergy and Infectious Diseases (NIAID).
Funding and Bias Transparency
Research into HIV-associated lipodystrophy has been significantly funded by the National Institutes of Health (NIH) and pharmaceutical companies developing antiretroviral therapies. While these funding sources have facilitated important advances in understanding the condition, it’s crucial to acknowledge potential biases. Studies funded by pharmaceutical companies may be more likely to report favorable outcomes for their products. Independent research, funded by government agencies and non-profit organizations, is essential to provide a balanced and objective assessment of the risks and benefits of different treatment options.
Diagnostic Approaches and Treatment Strategies
Diagnosing buffalo hump involves a comprehensive medical evaluation, including a physical examination, review of medical history, and laboratory tests. Blood tests are used to assess cortisol levels, rule out Cushing’s syndrome, and evaluate lipid profiles. In patients with HIV, viral load and CD4 count are monitored to assess the effectiveness of antiretroviral therapy. Imaging studies, such as MRI or CT scans, may be used to visualize the fat pad and rule out other potential causes. Treatment strategies depend on the underlying cause. For Cushing’s syndrome, treatment may involve surgery, radiation therapy, or medication to reduce cortisol levels. In HIV-associated lipodystrophy, switching to alternative antiretroviral regimens or adding medications to improve lipid metabolism may be considered. Lifestyle modifications, such as diet and exercise, can also help manage fat accumulation.
| Condition | Typical Cortisol Levels (µg/dL) | Common Medications Associated | Treatment Options |
|---|---|---|---|
| Cushing’s Syndrome | >10 (late-night salivary cortisol) | Glucocorticoids, ACTH-secreting tumors | Surgery, radiation, medication (ketoconazole, metyrapone) |
| HIV-Associated Lipodystrophy | Normal | Protease Inhibitors (e.g., darunavir, atazanavir) | Switching ARV regimens, lipid-lowering drugs |
| Medication-Induced | Normal | Certain antipsychotics, immunosuppressants | Adjusting medication dosage, alternative medications |
Contraindications & When to Consult a Doctor
Individuals with a family history of Cushing’s syndrome or lipodystrophy should be particularly vigilant for the development of a buffalo hump. Patients taking medications known to be associated with fat redistribution should also be monitored closely. Consult a doctor immediately if you experience any of the following symptoms in conjunction with a developing buffalo hump: unexplained weight gain, muscle weakness, fatigue, high blood pressure, or changes in mood. Do not attempt to self-diagnose or self-treat this condition. Prompt medical attention is essential to identify the underlying cause and initiate appropriate treatment.
The emergence of buffalo hump as a potential side effect of a wider range of medications necessitates increased awareness among healthcare professionals and patients alike. Continued research is needed to elucidate the underlying mechanisms and develop more effective prevention and treatment strategies. By fostering a collaborative approach between clinicians, researchers, and patients, People can improve the management of this condition and enhance the quality of life for those affected.
References
- Glucocorticoid receptor mechanisms in metabolic disease. Endocrine Reviews. 2020 Oct 1;41(5):bbaa083.
- Mitochondrial dysfunction in HIV-associated lipodystrophy. AIDS. 2011 Dec 20;25(18):2145-55.
- Long-Term Health Conditions Associated with HIV. Centers for Disease Control and Prevention.
- Cushing’s Syndrome. National Institute of Diabetes and Digestive and Kidney Diseases.

