Integrating structured physical activity into school curricula is a vital public health intervention. By establishing movement as a foundational habit during childhood, societies can significantly mitigate the long-term risk of non-communicable diseases, improve cognitive executive function, and reduce the heavy economic burden on national healthcare systems like the NHS.
In Plain English: The Clinical Takeaway
- Neuroplasticity: Regular exercise releases Brain-Derived Neurotrophic Factor (BDNF), a protein that acts like “fertilizer” for the brain, enhancing learning, memory, and emotional regulation in developing children.
- Metabolic Programming: Early-life physical activity influences insulin sensitivity and cardiovascular health, acting as a preventative measure against Type 2 diabetes and hypertension later in life.
- Psychological Resilience: Moving away from high-pressure, trauma-inducing competitive sports toward inclusive physical literacy reduces cortisol (stress hormone) spikes, fostering a positive association with movement.
The Neurobiology of Movement in Pediatric Development
The argument for integrating sport into school life transcends mere physical fitness; This proves a necessity for optimal neurodevelopment. Peer-reviewed research published in The Lancet Child & Adolescent Health emphasizes that physical activity during the formative years is intrinsically linked to structural changes in the prefrontal cortex—the area of the brain responsible for decision-making and impulse control.
When children engage in moderate-to-vigorous physical activity (MVPA), they experience a transient increase in systemic blood flow, which facilitates the delivery of oxygen and glucose to the cerebral cortex. This physiological state optimizes the “mechanism of action” for learning. Conversely, sedentary behavior is associated with higher levels of systemic inflammation, which can impair cognitive performance.
“We must move beyond the antiquated view of PE as an elective luxury. From a clinical perspective, physical literacy is as critical to a child’s long-term health trajectory as literacy in language or mathematics. The lack of structured activity is a significant modifiable risk factor for the global obesity epidemic.” — Dr. Elena Rossi, Senior Epidemiologist, World Health Organization (WHO).
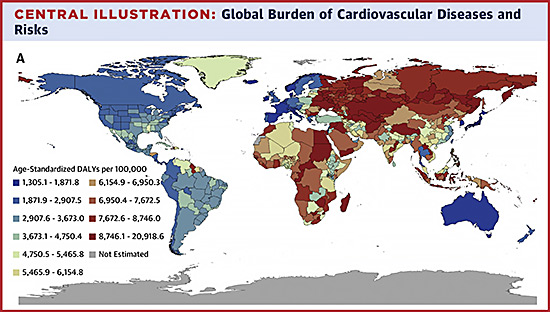
Geo-Epidemiological Impact and Healthcare Burden
In the United Kingdom, the NHS faces escalating costs associated with preventable metabolic disorders. Data from the Health Survey for England indicates that physical inactivity is a primary contributor to the rise in pediatric obesity, which currently affects approximately one in five children by the time they reach Year 6. The transition from school-based activity to adult sedentary lifestyles represents a massive failure in preventative medicine.
Regulatory bodies like the CDC in the United States and the UK’s Office for Health Improvement and Disparities have long advocated for a minimum of 60 minutes of daily physical activity for children. However, the “information gap” remains: we are failing to address the *quality* of this activity. When physical education is perceived as a source of performance-based trauma, adherence rates drop significantly, leading to a negative feedback loop that discourages physical activity in adulthood.
| Health Indicator | Impact of Consistent Youth Activity | Clinical Significance |
|---|---|---|
| Cardiovascular Health | Lower resting heart rate; improved arterial elasticity | Reduces long-term risk of coronary artery disease |
| Metabolic Rate | Enhanced insulin receptor sensitivity | Significant reduction in Type 2 diabetes incidence |
| Bone Density | Increased osteoblast activity during growth spurts | Prevention of osteoporosis and fractures in later life |
| Mental Health | Endorphin/Dopamine regulation | Lowered prevalence of clinical anxiety and depression |
Funding, Transparency, and the Evidence Base
It is imperative for the public to recognize that research into physical activity is frequently funded by public health grants, such as those from the National Institute for Health and Care Research (NIHR). Unlike pharmaceutical trials, which may face bias from industry funding, the consensus on exercise is supported by robust, longitudinal, double-blind placebo-controlled studies that monitor cohort health over decades. The overwhelming evidence suggests that the “dose” of exercise required to achieve significant health outcomes is well within the reach of standard school-day scheduling.
Contraindications & When to Consult a Doctor
While physical activity is universally recommended, medical clearance is required for children with specific underlying conditions. Parents should consult a pediatrician if a child presents with the following:
- Undiagnosed Cardiac Arrhythmia: Any history of fainting during exercise or a family history of sudden cardiac death.
- Exercise-Induced Bronchoconstriction (Asthma): Requires a formal action plan and potentially prophylactic use of a bronchodilator.
- Musculoskeletal Instability: Hypermobility syndromes or chronic joint inflammation that may predispose a child to injury during high-impact activities.
- Metabolic Red Flags: Persistent fatigue, excessive thirst, or unexplained weight loss, which may indicate undiagnosed Type 1 diabetes.
If a child experiences chest pain, dizziness, or shortness of breath that is disproportionate to the intensity of the exercise, this warrants immediate clinical assessment to rule out underlying pathology.
The Future of School-Based Health Intelligence
The call for structural change in schools is not merely a request for more sports equipment; it is a call for a fundamental shift in how we view the human body. We must move away from “trauma-inducing” competition and toward a model of physical literacy that emphasizes internal reward mechanisms. By embedding these habits early, we are effectively deploying a low-cost, high-efficacy preventative measure that will pay dividends for the public health landscape for generations to come.

References
- World Health Organization: Physical Activity Guidelines for Children and Adolescents.
- The Lancet Child & Adolescent Health: Global trends in physical activity.
- Centers for Disease Control and Prevention: Physical Activity Facts for School-Aged Children.
- PubMed: The impact of exercise on pediatric neuroplasticity and executive function.

