This week’s essay on golf and human connection highlights an often-overlooked health intersection: how recreational activities like golf can both reveal and influence underlying medical conditions, particularly sleep disturbances and mood changes commonly reported during midlife transitions. For individuals experiencing new-onset insomnia, persistent fatigue, or urinary symptoms such as frequent nighttime urination, these may not simply be signs of aging but could indicate treatable conditions like obstructive sleep apnea, depression, or benign prostatic hyperplasia (BPH)—a non-cancerous enlargement of the prostate gland that affects urinary flow. Recognizing these patterns early allows for timely intervention, improving quality of life and preventing long-term complications.
In Plain English: The Clinical Takeaway
- Poor sleep and low mood during midlife are not inevitable parts of aging—they may signal medical conditions that respond well to treatment.
- Frequent nighttime urination in men over 50 should prompt evaluation for BPH, which is highly manageable with medication or minimally invasive procedures.
- Engaging in regular, moderate activities like golf supports cardiovascular and mental health, but persistent symptoms warrant medical assessment rather than being dismissed as stress or age-related change.
Connecting Lifestyle Clues to Hidden Health Signals
The anecdotal observation in the Korean economic essay—that conversations on the golf course often turn to personal health struggles—mirrors broader clinical patterns. Midlife adults, particularly those aged 45 to 65, frequently report clusters of symptoms including disrupted sleep, low energy, irritability, and urinary changes. While these are often attributed to stress or “getting older,” they frequently represent identifiable medical conditions. For example, obstructive sleep apnea (OSA), characterized by repeated pauses in breathing during sleep due to airway collapse, affects an estimated 22 million Americans and is strongly linked to hypertension, atrial fibrillation, and depression. Its hallmark symptom—non-restorative sleep despite adequate duration—often presents as fatigue and poor concentration, which patients may misattribute to lifestyle.
Similarly, benign prostatic hyperplasia (BPH) affects approximately 50% of men by age 60 and up to 90% by age 85. It occurs when the prostate gland enlarges, compressing the urethra and causing symptoms like hesitancy, weak stream, nocturia (waking two or more times at night to urinate), and urgency. These symptoms directly interfere with sleep quality and daily comfort, potentially explaining why golfers in their 50s and 60s frequently mention urinary inconvenience during rounds. Importantly, BPH is not cancer, nor does it increase cancer risk, but it significantly impacts quality of life if left unmanaged.
Geopolitical and Systemic Access to Diagnosis and Care
In the United States, the U.S. Food and Drug Administration (FDA) has approved several classes of medication for BPH, including alpha-blockers (e.g., tamsulosin) that relax prostate and bladder neck muscles, and 5-alpha-reductase inhibitors (e.g., finasteride) that reduce prostate size by blocking hormonal conversion of testosterone to dihydrotestosterone (DHT). For moderate to severe cases, minimally invasive procedures such as UroLift or Rezum vapor therapy are now widely covered by Medicare and private insurers when medical therapy fails. In the UK, the National Health Service (NHS) follows NICE guidelines recommending alpha-blockers as first-line therapy, with surgical options like transurethral resection of the prostate (TURP) available for refractory cases.
In South Korea, where the original essay originates, the Ministry of Food and Drug Safety (MFDS) regulates BPH treatments, and national health insurance covers both diagnostic evaluations (including prostate-specific antigen [PSA] testing and uroflowmetry) and standard medications. Still, access to newer minimally invasive therapies varies by region, with urban centers like Seoul offering broader options than rural areas. A 2023 study in The Korean Journal of Urology found that while 78% of Korean men over 60 reported BPH symptoms, only 41% sought medical care—often due to stigma or normalization of symptoms.
Mechanisms, Evidence, and Transparent Origins of Knowledge
The understanding of BPH pathophysiology centers on androgen sensitivity: the prostate gland relies on dihydrotestosterone (DHT), a potent metabolite of testosterone, for growth. In BPH, epithelial and stromal cells in the transition zone of the prostate proliferate under DHT stimulation, leading to nodules that encroach on the urethra. This is why 5-alpha-reductase inhibitors—which block the enzyme converting testosterone to DHT—can reduce prostate volume by approximately 20–30% over 6–12 months, as demonstrated in the landmark MTOPS trial (Medical Therapy of Prostatic Symptoms), a randomized, double-blind, placebo-controlled study involving over 3,000 men across North America and Europe.
Funding for the MTOPS trial came from the U.S. National Institutes of Health (NIH), specifically the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), ensuring independence from pharmaceutical influence. Similarly, large-scale epidemiological data on sleep apnea prevalence cited here derives from the Wisconsin Sleep Cohort Study, a longitudinal project funded by the National Heart, Lung, and Blood Institute (NHLBI) and published in peer-reviewed journals like Sleep and American Journal of Respiratory and Critical Care Medicine. These studies exemplify how public investment generates generalizable knowledge free from commercial bias.
“Sleep disruption and nocturia are rarely isolated symptoms—they often cluster as part of a broader physiological shift in midlife that warrants holistic evaluation, not piecemeal treatment.”
— Dr. Susan Redline, MD, MPH, Professor of Sleep Medicine, Harvard Medical School and Senior Physician, Brigham and Women’s Hospital
“Benign prostatic hyperplasia is incredibly common, but it’s also highly treatable. The danger lies not in the condition itself, but in delaying care until complications like urinary retention or bladder damage occur.”
— Dr. Gerald Andriole Jr., MD, Chief of Urology, Washington University School of Medicine in St. Louis
Putting Risk in Context: Who Should Be Cautious and When to Act
Contraindications & When to Consult a Doctor
While lifestyle activities like golf are universally beneficial for cardiovascular and mental health, certain symptoms should prompt medical evaluation rather than being attributed to stress or aging. Men over 50 who experience nocturia (waking to urinate twice or more per night), a weak or intermittent urinary stream, difficulty starting urination, or a feeling of incomplete bladder emptying should consult a primary care physician or urologist. These are hallmark signs of BPH that, if ignored, can lead to complications such as urinary tract infections, bladder stones, or acute urinary retention—a sudden inability to urinate requiring catheterization.
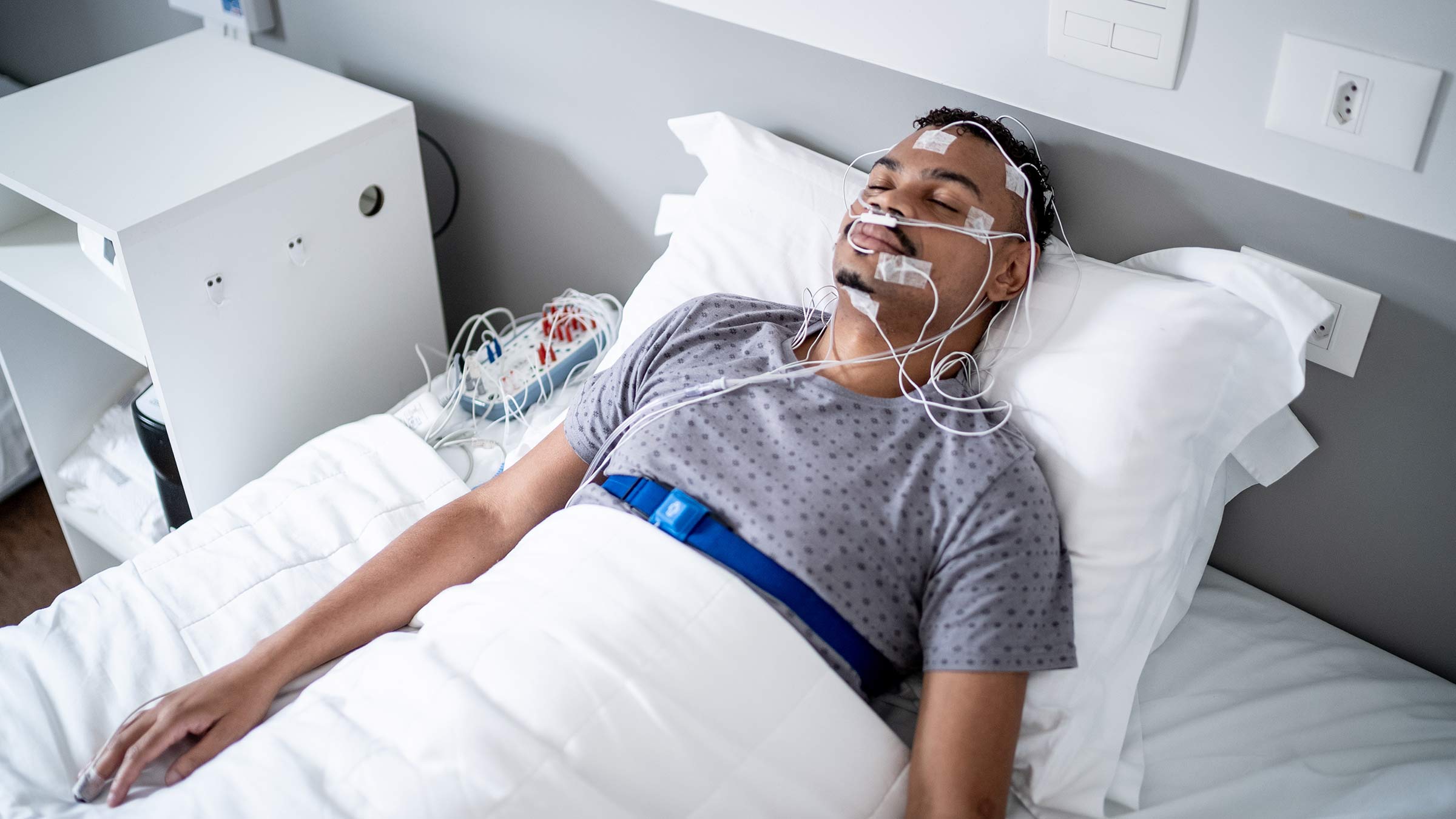
Similarly, persistent insomnia accompanied by loud snoring, gasping during sleep, or daytime fatigue despite adequate time in bed may indicate obstructive sleep apnea. Left untreated, OSA increases the risk of stroke by up to threefold and is associated with resistant hypertension. Individuals with diagnosed OSA should avoid sedatives, alcohol before bedtime, and sleeping in the supine position, as these can worsen airway collapse. Weight management and positional therapy are first-line recommendations, with continuous positive airway pressure (CPAP) remaining the gold standard for moderate to severe cases.
Importantly, PSA testing—often used alongside BPH evaluation—must be interpreted cautiously. Elevated PSA can reflect BPH, prostatitis, urinary retention, or, less commonly, prostate cancer. We see not diagnostic on its own and should never trigger alarm without further context, such as free-to-total PSA ratio, prostate MRI, or urology referral. Patients should be informed that BPH does not cause cancer, and having BPH does not increase cancer risk—though both conditions become more prevalent with age.
Toward Proactive, Compassionate Midlife Health
The conversations sparked on the golf course reveal a valuable truth: shared activities create spaces where health concerns surface naturally. Rather than dismissing these moments as mere complaints, they offer opportunities for early detection and compassionate dialogue. Clinically, addressing sleep disruption, mood changes, and urinary symptoms is not about chasing youth—it’s about preserving function, independence, and well-being through evidence-based care.
Public health systems in the U.S., Europe, and increasingly in parts of Asia are structured to support timely intervention for conditions like BPH and OSA. The key lies in normalizing help-seeking behavior, dismantling the myth that suffering in silence is a sign of strength, and recognizing that seeking care is an act of resilience—not vulnerability.
References
- Roehrborn CG, et al. Medical Therapy of Prostatic Symptoms (MTOPS) Trial. J Urol. 2001;166(5):1651-7. PMID: 11238302
- Young T, et al. Sleep-disordered breathing and mortality: eighteen-year follow-up of the Wisconsin Sleep Cohort. Sleep. 2008;31(8):1071-8. PMID: 18714778
- Barry MJ, et al. Benign prostatic hyperplasia-specific health status measures in clinical research: how much change in the American Urological Association Symptom Index and Benign Prostatic Hyperplasia Impact Index is perceptible to patients? J Urol. 1995;154(5):1770-6. PMID: 7500465
- Redline S, et al. Epidemiology, genetics, and consequences of obstructive sleep apnea. J Allergy Clin Immunol. 2010;125(3):440-50. PMID: 20226764
- Kim SW, et al. Prevalence and associated factors of lower urinary tract symptoms in Korean men: results from the Korean Longitudinal Study on Aging (KLoSA). Korean J Urol. 2013;54(12):825-32. PMID: 24363655

