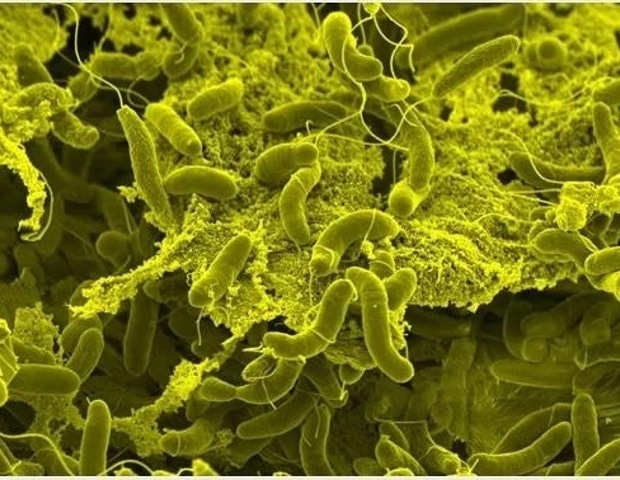
A new genomic study published in Nature reveals a dynamic evolutionary arms race between Vibrio cholerae, the bacteria causing cholera, and a virus called bacteriophage ICP1, primarily observed in the Ganges Basin. This ongoing battle influences disease severity and spread, challenging previous assumptions about cholera’s global origins and offering potential avenues for novel interventions.
Cholera remains a significant global health threat, particularly in regions with limited access to clean water and sanitation. The seventh cholera pandemic, ongoing since 1961, continues to cause an estimated 1.3 to 4 million cases and up to 143,000 deaths annually worldwide. Understanding the complex interplay between the bacteria, its viral predators, and the environment is crucial for effective prevention and control strategies.
In Plain English: The Clinical Takeaway
- Bacteria vs. Virus: Cholera bacteria are constantly evolving defenses against viruses that attack them. This fight impacts how sick people get.
- Ganges Basin is Key: The area around the Ganges River in South Asia isn’t just where cholera *starts*, but where it’s actively changing and adapting.
- Travel Matters: How people move around – not just rivers – plays a sizeable role in spreading cholera.
The Evolutionary Battlefield: Bacteriophages and Cholera Defense Systems
Researchers at the Wellcome Sanger Institute, icddr,b, and PGIMER analyzed over 2,300 V. Cholerae genomes collected across approximately 20 years in Bangladesh and North India. Their findings demonstrate that the bacteria rapidly acquire and lose genetic elements – termed defense systems – that protect them from ICP1, a bacteriophage. Bacteriophages, or phages, are viruses that specifically infect bacteria. They replicate within bacterial cells, ultimately causing their destruction. Crucially, phages are generally harmless to human cells and are a natural component of the human gut microbiome. The mechanism of action involves the phage injecting its genetic material into the bacterium, hijacking its cellular machinery to produce more phages, eventually lysing (breaking open) the bacterial cell.

This isn’t a one-sided conflict. The study reveals that ICP1, in turn, evolves “anti-defense” mechanisms to overcome the bacterial shields. This constant cycle of adaptation and counter-adaptation is a classic example of an evolutionary arms race. Previous research has established a correlation between the presence of ICP1 in the gut and reduced cholera disease severity, as the virus effectively reduces the bacterial load. However, this new research provides a deeper understanding of the *dynamics* of this interaction.
Shifting the Source: From Delta to Basin
For decades, the Ganges Delta was considered the primary global source of cholera. However, this study challenges that assumption. Genomic analysis indicates that the Ganges Basin, encompassing a wider geographical area, is the primary source of cholera strains circulating globally during the study period. This finding has significant implications for surveillance and intervention strategies.
the research highlights the limited role of river flow in bacterial spread. Instead, human travel and population density appear to be more influential factors in cholera transmission. This suggests that interventions focused on improving sanitation and hygiene in densely populated areas, coupled with monitoring travel patterns, may be more effective than solely focusing on waterborne transmission routes. This aligns with epidemiological models demonstrating the impact of human mobility on infectious disease spread, particularly in resource-limited settings.
Funding and Bias Transparency
The research was primarily funded by the Wellcome Trust, a global charitable foundation dedicated to health research. Additional funding was provided by the UK Foreign, Commonwealth & Development Office. While the Wellcome Trust has a strong commitment to global health, it’s important to acknowledge that funding sources can potentially influence research priorities and interpretations. However, the study’s rigorous methodology and peer-review process mitigate potential biases.
“This research underscores the importance of genomic surveillance in tracking the evolution of infectious diseases. By understanding how bacteria adapt to their environment and to viral predators, we can develop more effective strategies to prevent and control outbreaks.” – Dr. John J. Treanor, Professor of Medicine, University of Rochester Medical Center (Independent Expert Commentary)
Geographical Impact and Regional Healthcare Systems
The findings have direct implications for public health strategies in South Asia, particularly in Bangladesh and India. The identification of the Ganges Basin as the primary source necessitates intensified surveillance efforts in this region. This includes enhanced genomic sequencing of V. Cholerae strains to track the emergence of new defense mechanisms and identify high-risk strains. In the United States, the Centers for Disease Control and Prevention (CDC) actively monitors cholera outbreaks globally and provides guidance on prevention and treatment. The European Centre for Disease Prevention and Control (ECDC) performs a similar role within the European Union. The data generated by studies like this will inform risk assessments and potentially influence travel advisories issued by these agencies.
| Cholera Strain | Defense System Presence | ICP1 Prevalence | Disease Severity | Geographical Distribution |
|---|---|---|---|---|
| 7PET O1 (Early Samples) | Low | Low | High | Ganges Delta |
| 7PET O1 (Recent Samples) | High | High | Moderate | Ganges Basin |
| Emerging Strains (No Defense) | Absent | Variable | High | Localized Outbreaks |
Contraindications & When to Consult a Doctor
While this research doesn’t directly relate to a specific treatment, understanding cholera transmission is vital for prevention. Individuals traveling to cholera-endemic areas should prioritize consuming safe drinking water (boiled or bottled), practicing thorough hand hygiene, and avoiding raw or undercooked seafood. Individuals experiencing symptoms of cholera – profuse watery diarrhea, vomiting, and rapid dehydration – should seek immediate medical attention. Those with compromised immune systems, young children, and the elderly are particularly vulnerable to severe complications and require prompt treatment, typically involving oral or intravenous rehydration therapy and antibiotics.

The Future of Cholera Control: Harnessing the Viral Nemesis?
The discovery of the evolutionary arms race between V. Cholerae and ICP1 opens up exciting possibilities for novel cholera control strategies. Researchers are exploring the potential of harnessing bacteriophages, like ICP1, as therapeutic agents. Phage therapy, the use of viruses to kill bacteria, is gaining renewed interest as a potential alternative to antibiotics, particularly in the face of increasing antibiotic resistance. However, significant challenges remain, including the necessitate to identify phages with broad specificity and to overcome potential immune responses.
a comprehensive approach to cholera control requires a combination of improved sanitation, access to clean water, vaccination, and ongoing genomic surveillance. By understanding the complex ecological dynamics of this ancient disease, we can move closer to ending the seventh cholera pandemic and protecting vulnerable populations worldwide.
References
- Barton, A., Afrad, M. H., Taylor-Brown, A., et al. (2026). ‘Evolution of Pandemic Cholera at its Global Source’. Nature. DOI: 10.1038/s41586-026-10340-x
- World Health Organization. (2023). Cholera. https://www.who.int/news-room/fact-sheets/detail/cholera
- Centers for Disease Control and Prevention. (2023). Cholera. https://www.cdc.gov/cholera/index.html
- Goodman, A. L., et al. “Phage therapy: a review of current research and clinical applications.” *Viruses* 13.12 (2021): 2289. https://www.mdpi.com/1999-4915/13/12/2289