Chronic stress is emerging as a primary “lifestyle disease,” acting as a systemic catalyst for hypertension, type 2 diabetes, and cardiovascular decay. Unlike acute stress, chronic activation of the HPA axis creates a state of permanent physiological arousal, fundamentally altering metabolic and neurological health for millions of adults globally.
For decades, the medical community focused on diabetes and obesity as the twin pillars of lifestyle-driven illness. However, recent clinical data suggests these are often the end-stage manifestations of a more insidious driver: chronic stress. When the body remains in a state of perpetual “fight or flight,” the resulting biochemical imbalance doesn’t just affect mood; it physically remodels the architecture of the heart, the sensitivity of insulin receptors, and the integrity of the spinal column.
In Plain English: The Clinical Takeaway
- Stress is a Physical Toxin: Prolonged stress floods the body with cortisol, which, over time, acts like a slow-acting poison to your arteries and organs.
- The Metabolic Domino Effect: Chronic stress triggers insulin resistance, meaning your body can’t manage blood sugar, leading to diabetes even in people with a healthy diet.
- Neurological Rewiring: Constant connectivity and digital overload keep the brain in a state of hyper-vigilance, which shrinks the prefrontal cortex (the area responsible for decision-making).
The HPA Axis and the Pathology of Allostatic Load
To understand why stress is now classified as a lifestyle disease, we must examine the Hypothalamic-Pituitary-Adrenal (HPA) axis—the complex feedback system that governs our response to danger. In a healthy system, the hypothalamus signals the pituitary gland, which then prompts the adrenal glands to release cortisol. Once the threat passes, the system resets.
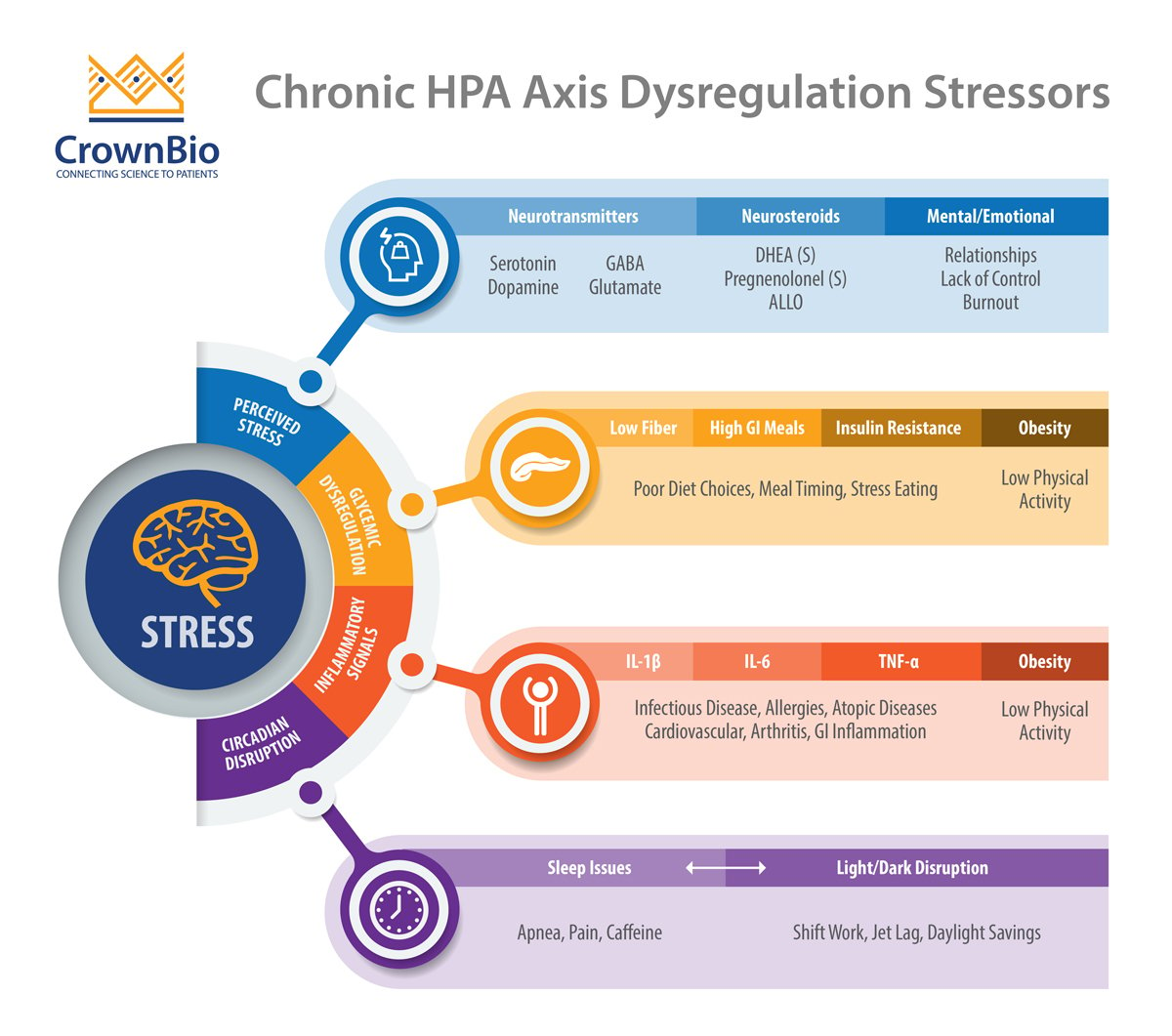
In the modern era of constant connectivity, this “off switch” is rarely flipped. This leads to allostatic load, a clinical term referring to the cumulative wear and tear on the body when exposed to repeated or chronic stress. When allostatic load becomes excessive, the body loses its ability to maintain homeostasis (internal stability), leading to systemic organ failure.
The mechanism of action is straightforward but devastating. Chronic cortisol elevation inhibits the production of insulin-like growth factor 1 (IGF-1) and promotes gluconeogenesis—the process by which the liver creates glucose from non-carbohydrate sources. This keeps blood sugar levels chronically elevated, forcing the pancreas to overproduce insulin, which eventually leads to the insulin resistance characteristic of Type 2 Diabetes.
“The global burden of mental health disorders, specifically those driven by chronic psychosocial stress, is no longer a secondary concern; it is a primary driver of non-communicable diseases that threaten to overwhelm healthcare systems from New Delhi to New York.” — Representative guidance from the World Health Organization (WHO) on Mental Health Action Plans.
Cardiovascular Erosion and the “Connectivity Tax”
The relationship between stress and the heart is not merely about “feeling anxious.” It is about hemodynamic instability—the fluctuation of blood pressure and flow. Chronic stress triggers a persistent release of catecholamines (epinephrine and norepinephrine), which causes systemic vasoconstriction (the narrowing of blood vessels).
Over time, this constant pressure creates micro-tears in the endothelium, the thin inner lining of the blood vessels. These tears become sites for plaque accumulation, accelerating atherosclerosis (hardening of the arteries). This is why patients with high-stress professional lives often present with cardiovascular events despite having “optimal” cholesterol levels.
From a geo-epidemiological perspective, this is creating a crisis in urban hubs. In cities like Bengaluru and London, the “always-on” work culture is resulting in a spike of early-onset hypertension. Although the NHS in the UK has begun integrating “social prescribing” to combat this, the US healthcare system remains largely reactive, treating the resulting hypertension with beta-blockers rather than addressing the HPA axis dysfunction at the root.
| Physiological Marker | Acute Stress Response (Normal) | Chronic Stress Pathology (Disease) | Long-term Clinical Outcome |
|---|---|---|---|
| Cortisol Levels | Brief spike, then rapid decline | Persistently elevated (Hypercortisolemia) | Muscle wasting, immune suppression |
| Blood Pressure | Temporary rise to increase oxygen | Chronic hypertension | Left ventricular hypertrophy (Heart failure) |
| Glucose Metabolism | Rapid energy release for action | Chronic hyperglycemia | Type 2 Diabetes Mellitus |
| Neurological State | Heightened alertness | Cognitive fatigue / Brain fog | Hippocampal atrophy (Memory loss) |
Funding Transparency and the Evidence Gap
It is critical to note that much of the research linking chronic stress to systemic disease is funded by public health entities such as the National Institutes of Health (NIH) and university-led longitudinal studies. Unlike pharmaceutical trials for obesity or diabetes drugs, there is less commercial incentive to “cure” stress, which means the data is generally less biased toward a specific product and more focused on public health outcomes.
However, an information gap exists regarding the “spine damage” mentioned in recent reports. The clinical link is likely cortisol-induced bone resorption. High levels of cortisol inhibit osteoblast (bone-building cell) activity and increase osteoclast (bone-breaking cell) activity. In high-stress populations, this can lead to decreased bone mineral density, making the spine more susceptible to degenerative disc disease, especially when coupled with the sedentary posture of corporate work.
Contraindications & When to Consult a Doctor
While lifestyle modifications—such as mindfulness, sleep hygiene, and digital detoxing—are evidence-based, they are not substitutes for clinical intervention in severe cases. It is vital to distinguish between “lifestyle stress” and clinical pathologies.

Seek immediate medical attention if you experience:
- Chest Pain or Palpitations: This may indicate that chronic stress has progressed to unstable angina or arrhythmia.
- Severe Insomnia: When sleep deprivation lasts more than two weeks, it can trigger a feedback loop that exacerbates HPA axis dysfunction.
- Anhedonia: The total loss of interest in previously enjoyed activities, which may signal that chronic stress has transitioned into Major Depressive Disorder (MDD).
- Unexplained Weight Gain: Specifically “central obesity” (weight gain around the abdomen), which is a hallmark of Cushingoid responses to chronic cortisol.
Patients currently taking corticosteroids or those with existing adrenal insufficiency must consult an endocrinologist before attempting aggressive “stress-reduction” protocols that involve significant dietary changes or supplements, as these can interfere with hormone replacement therapy.
The Future of Preventative Medicine
We are moving toward a paradigm where “stress management” is no longer viewed as a wellness luxury but as a clinical imperative. The integration of biomarkers—such as measuring salivary cortisol or heart rate variability (HRV)—will likely become standard in annual physicals, allowing physicians to intervene before allostatic load triggers a permanent metabolic shift.
The goal is a shift from reactive medicine (treating the diabetes) to translational medicine (treating the stress that caused the diabetes). Only by addressing the neurological and hormonal roots of the modern lifestyle can we hope to bend the curve of the global chronic disease epidemic.
References
- PubMed Central: Studies on Allostatic Load and Cardiovascular Disease
- World Health Organization: Global Report on Mental Health and Non-Communicable Diseases
- The Lancet: Longitudinal Analysis of Psychosocial Stress and Metabolic Syndrome
- JAMA: The Impact of Occupational Burnout on Patient Safety and Provider Health
- Centers for Disease Control and Prevention (CDC): Hypertension and Stress Correlation Data

