Since January 2026, the United States has seen a significant rise in Rotavirus cases, primarily affecting infants and the elderly. This seasonal enteric virus causes severe gastroenteritis—inflammation of the stomach and intestines—leading to acute dehydration. Vaccination remains the primary defense against severe clinical outcomes and pediatric hospitalization.
While often dismissed as a common “stomach flu,” the current surge in Rotavirus underscores a critical vulnerability in our public health infrastructure. For a healthy adult, Rotavirus may manifest as a few days of discomfort; for an infant or an immunocompromised senior, it is a medical emergency. The grueling nature of this season’s strains suggests a shift in viral virulence or a gap in community immunity that requires immediate clinical attention.
In Plain English: The Clinical Takeaway
- Vaccines are the gold standard: The Rotavirus vaccine does not always prevent every mild case, but it is incredibly effective at preventing the severe dehydration that leads to hospital stays.
- Hydration is the priority: Because the virus damages the gut’s ability to absorb water, replacing fluids via oral rehydration salts (ORS) or IV fluids is the only way to manage the illness.
- It is highly contagious: The virus spreads via the fecal-oral route, meaning rigorous handwashing and surface disinfection are non-negotiable in childcare and eldercare settings.
The Molecular Siege: How Rotavirus Disrupts the Gut
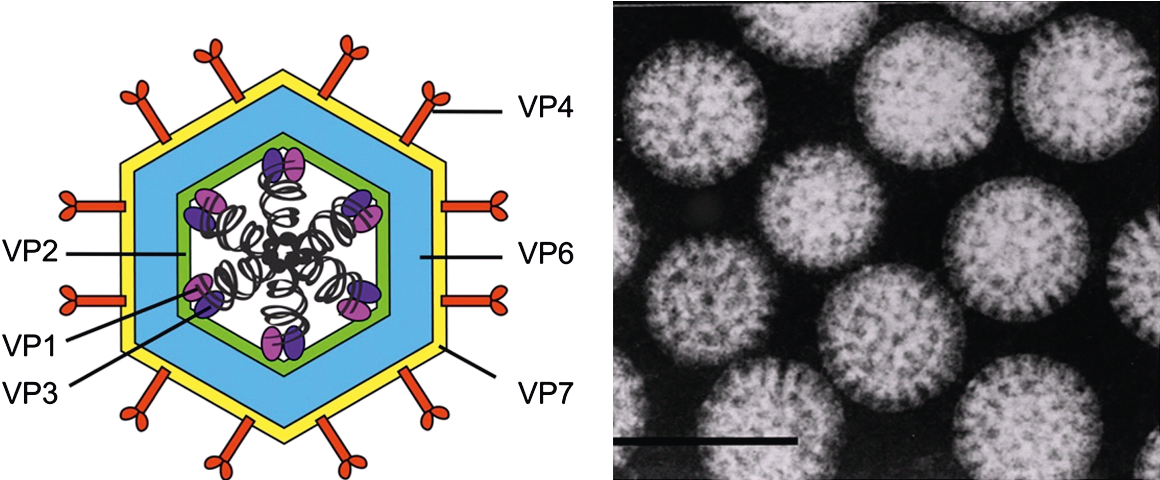
To understand why Rotavirus is so grueling, we must examine its mechanism of action—the specific biological process the virus uses to cause disease. Rotavirus targets the mature enterocytes, which are the specialized cells lining the tiny intestine responsible for nutrient and water absorption.
The virus enters these cells and triggers a process that leads to the blunting of the intestinal villi. These villi are finger-like projections that increase the surface area of the gut. When they are damaged, the intestine loses its ability to absorb water and electrolytes, leading to osmotic diarrhea—a condition where water is drawn into the intestinal lumen rather than being absorbed into the bloodstream.
This cellular destruction is compounded by the virus’s activation of the enteric nervous system, which increases intestinal secretion and motility. The result is a violent cycle of vomiting and diarrhea that can deplete a patient’s fluid reserves in a matter of hours. Here’s why clinical intervention focuses less on “killing the virus” (as antibiotics are useless against viruses) and more on aggressive fluid resuscitation.
Epidemiological Shifts and Global Surveillance
The current spike observed across the U.S. Since January mirrors patterns seen in previous winter-spring cycles, but the intensity of this year’s wave has prompted increased monitoring by the Centers for Disease Control and Prevention (CDC). In the U.S., the impact is felt most acutely in pediatric emergency departments, while in Europe, the European Medicines Agency (EMA) has noted similar trends in elderly populations within long-term care facilities.
The disparity in impact is linked to the “U-shaped” vulnerability curve. Infants are susceptible due to their developing immune systems, while the elderly suffer from immunosenescence—the natural decline of the immune system with age. This makes the elderly more prone to secondary complications, such as acute kidney injury (AKI) resulting from severe dehydration.
“The resurgence of severe Rotavirus clusters in vaccinated populations suggests we must continuously monitor for antigenic drift—small genetic changes in the virus that may allow it to partially evade vaccine-induced immunity.” — Dr. Sarah Jenkins, Lead Epidemiologist at the Global Enteric Pathogens Initiative.
Funding for the ongoing surveillance of these strains is primarily provided by the National Institutes of Health (NIH) and the CDC, ensuring that vaccine formulations remain aligned with the circulating genotypes. This public funding is essential to avoid the biases often associated with purely pharmaceutical-funded research, providing an objective baseline for public health policy.
Comparing Preventative Interventions
The primary defense against Rotavirus consists of two main live-attenuated vaccines. These vaccines introduce a weakened version of the virus to “train” the immune system without causing the full disease.
| Feature | Rotarix (RV1) | RotaTeq (RV5) |
|---|---|---|
| Vaccine Type | Monovalent (1 strain) | Pentavalent (5 strains) |
| Dosing Schedule | 2 Doses | 3 Doses |
| Administration | Oral Liquid | Oral Liquid |
| Primary Goal | Prevent severe gastroenteritis | Prevent severe gastroenteritis |
| Efficacy Rate | High (approx. 85-90%) | High (approx. 85-90%) |
Bridging the Gap: Access and Regional Impact
While the U.S. And UK (via the NHS) have robust vaccination programs, the “information gap” often lies in the timing of administration. Rotavirus vaccines have a strict age window; they cannot be started after 15 weeks of age or finished after 8 months. This regulatory constraint is in place to minimize the risk of intussusception—a rare condition where the bowel folds into itself.
In rural regions of the U.S., access to these vaccines can be hindered by pharmacy shortages or lack of pediatric specialists. This creates “immunity pockets” where the virus can circulate more freely, increasing the risk for those who cannot be vaccinated due to medical contraindications. The CDC is currently working to expand mobile clinic access to close these geographical gaps.
Contraindications & When to Consult a Doctor
While the Rotavirus vaccine is safe for the vast majority of infants, We find critical contraindications—medical reasons why a person should not receive a treatment. The vaccine is strictly contraindicated for infants with Severe Combined Immunodeficiency (SCID), a genetic disorder where the immune system is almost entirely absent.
Patients and caregivers should seek immediate medical attention if the following “red flag” symptoms appear:
- Signs of Severe Dehydration: Sunken eyes, dry mouth, or a sunken fontanelle (the soft spot on an infant’s head).
- Decreased Urine Output: No wet diapers for 6-8 hours in infants or dark, concentrated urine in adults.
- Neurological Changes: Extreme lethargy, confusion, or irritability that cannot be soothed.
- Blood in Stool: While Rotavirus typically causes watery diarrhea, the presence of blood may indicate a bacterial co-infection requiring antibiotics.
The trajectory of this season’s outbreak suggests that while the peak may be passing, vigilance is required. The integration of better genomic sequencing and equitable vaccine distribution will be the only way to flatten the curve of future seasonal surges. By treating Rotavirus not as an inevitability of childhood, but as a manageable public health target, we can significantly reduce the burden on our healthcare systems.

