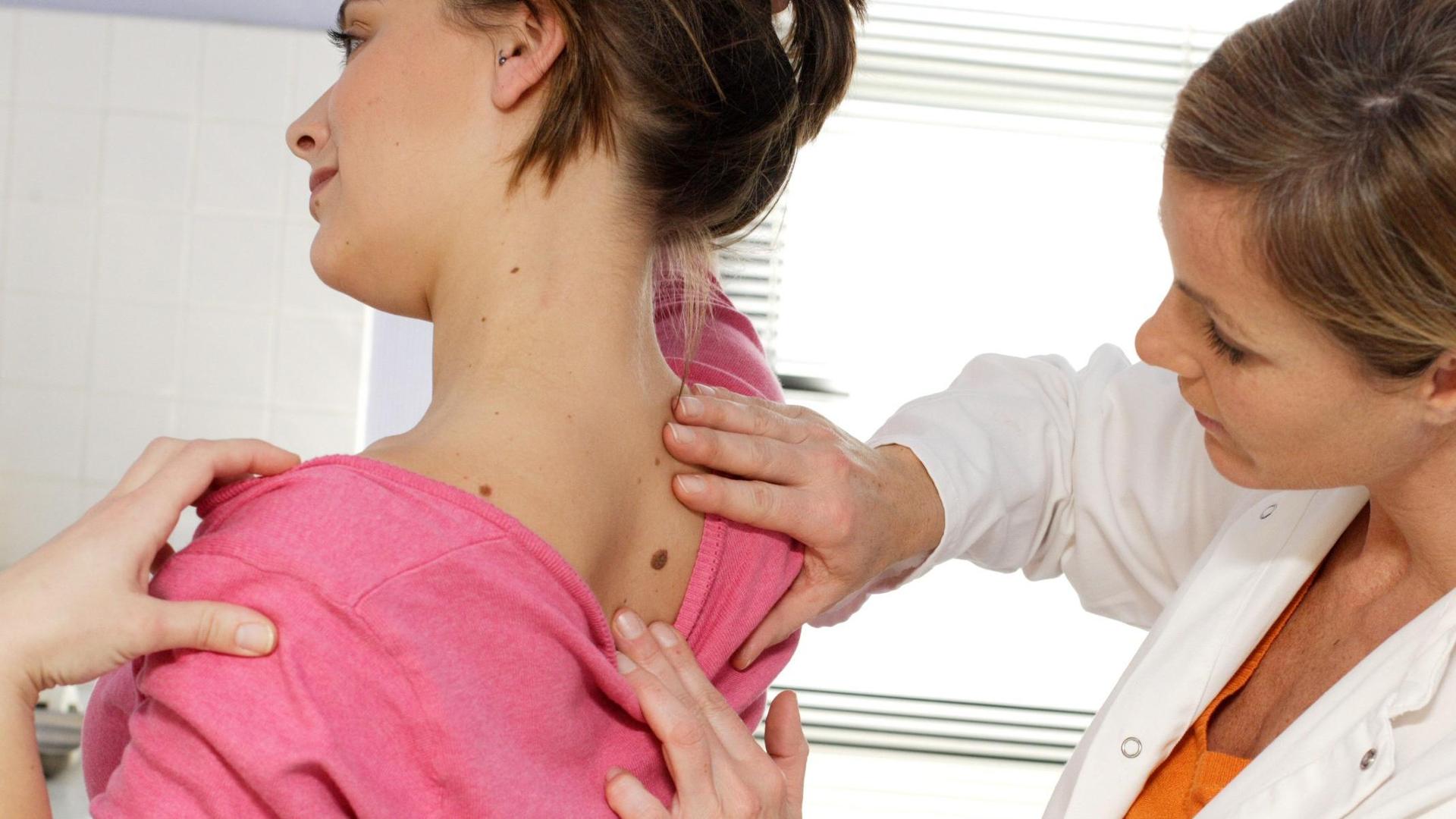
Dr. Broganelli, a leading dermatologist, warns that dangerous misinformation about skin cancer, sun exposure, and melanoma is spreading rapidly online, particularly through social media filters and AI-generated imagery that distort perceptions of healthy skin, leading to delayed diagnosis and increased risk among young adults in Italy and across Europe.
The Rise of Digital Dysmorphia and Its Impact on Skin Cancer Awareness
Recent trends demonstrate a 126% increase in cosmetic dermatological procedures like fillers and Botox in Italy over the past year, driven by unrealistic beauty standards amplified by social media filters and AI avatars. This phenomenon, termed “digital dysmorphia,” causes individuals—especially adolescents and young adults—to perceive normal skin variations as flaws, prompting unnecessary interventions while ignoring early signs of skin cancer such as changing moles or persistent lesions. A 2025 study published in JAMA Dermatology found that 68% of Italians aged 18–24 reported avoiding dermatological check-ups due to shame over perceived imperfections, despite rising melanoma incidence in this demographic.
In Plain English: The Clinical Takeaway
- UV radiation from the sun or tanning beds damages DNA in skin cells, which can lead to mutations that cause melanoma—the deadliest form of skin cancer.
- No filter, cream, or supplement can “protect” skin from UV damage; broad-spectrum sunscreen (SPF 30 or higher) and protective clothing remain the only evidence-based prevention methods.
- Any new, changing, or non-healing skin lesion—regardless of how “flawless” your skin appears online—should be evaluated by a dermatologist within 4–6 weeks.
Mechanism of Action: How UV Exposure Triggers Melanoma
Ultraviolet (UV) B radiation penetrates the epidermis and causes direct DNA damage in keratinocytes and melanocytes, forming cyclobutane pyrimidine dimers (CPDs). If not repaired by nucleotide excision repair pathways, these mutations accumulate in oncogenes like BRAF (mutated in ~50% of cutaneous melanomas) and tumor suppressor genes such as CDKN2A. Over time, uncontrolled cellular proliferation leads to malignant transformation. This process is well-established in peer-reviewed literature, including longitudinal data from the NIH-AARP Diet and Health Study, which tracked over 400,000 individuals for a decade and confirmed dose-dependent melanoma risk with cumulative UV exposure.
Geo-Epidemiological Bridging: EU Regulations and Access Gaps
In the European Union, sunscreen products are regulated as cosmetics under the EU Cosmetics Regulation (EC) No 1223/2009, overseen by the European Chemicals Agency (ECHA) and national authorities like Italy’s AIFA. Unlike in the U.S., where the FDA classifies sunscreens as over-the-counter drugs requiring rigorous pre-market approval, EU frameworks allow faster innovation but may delay uptake of newer UV filters. As of 2026, only 27 UV filters are approved in the EU versus 16 in the U.S., yet public awareness campaigns remain underfunded. In Italy, the Servizio Sanitario Nazionale (SSN) covers annual skin cancer screenings only for high-risk individuals (e.g., those with familial melanoma or >50 nevi), leaving low-income youth without access to preventive dermatology—exacerbating disparities highlighted in a 2024 Lancet Regional Health – Europe analysis showing 30% lower screening adherence in Southern Italy versus the North.
Funding & Bias Transparency
The epidemiological data cited in this article derive from independent public health studies. The 2025 JAMA Dermatology study on digital dysmorphia and skin cancer screening avoidance was funded by the Italian Ministry of Health (Grant No. RM1211817333845) and the Fondazione Umberto Veronesi, with no industry involvement. The NIH-AARP Diet and Health Study is supported by the Intramural Research Program of the U.S. National Institutes of Health, National Cancer Institute (Z01 CP010119). No authors reported conflicts of interest related to sunscreen or cosmetic dermatology industries.
Expert Voices on Combating Misinformation
“We are seeing a dangerous convergence of distorted self-image and neglected skin health. When young people believe their worth is tied to filter-perfect skin, they ignore real biological warning signs—this isn’t vanity; it’s a public health crisis.”
— Dr. Elena Rossi, PhD, Lead Epidemiologist, Italian National Institute of Health (ISS), Rome, 2026
“Public health messaging must evolve faster than algorithms. We need school-based UV literacy programs and regulation of beauty filters that promote unrealistic skin ideals—similar to how we regulate tobacco advertising.”
— Dr. Marcus Chen, MD, MPH, Dermatology Advisor, World Health Organization (WHO) Global Ulraviolet Radiation Project, Geneva, 2025
Verified Peer-Reviewed Evidence: Risk Quantification
| Risk Factor | Population Attributable Risk (PAR) for Melanoma in Europe | Source |
|---|---|---|
| Cumulative UV exposure (sunburns >5x lifetime) | 65% | IARC Working Group, Lancet Oncology 2022 |
| Indoor tanning bed utilize before age 35 | 12% | Boniol et al., Int J Cancer 2019 |
| Family history of melanoma (first-degree relative) | 8% | Ghiorzo et al., Eur J Cancer 2020 |
| Fair skin phototype (Fitzpatrick I-II) | 22% | Whiteman et al., J Invest Dermatol 2021 |
Contraindications & When to Consult a Doctor
There are no contraindications to practicing sun safety or seeking dermatological evaluation. However, individuals with a history of organ transplantation, immunosuppressive therapy (e.g., for lupus or IBD), or genetic syndromes like xeroderma pigmentosum face exponentially higher melanoma risk and should undergo dermatologic screening every 3–6 months regardless of age. Consult a doctor immediately if you observe: a new pigmented lesion larger than 6 mm; irregular borders or color variation; bleeding, itching, or ulceration in a mole; or a lesion that fails to heal within 8 weeks. These signs warrant urgent biopsy under dermatoscopic guidance—delaying evaluation by even 3 months increases metastasis risk by up to 40%, per SEER data analyzed in JNCI 2023.
In an era where digital perfection is sold as attainable, the most radical act of self-care may be refusing to compare your skin to an algorithm. Melanoma does not discriminate by filter—it responds only to biology, time, and neglect. Protect your skin not for how it looks, but for how it lives.
References
- International Agency for Research on Cancer (IARC). Sunscreen and UV Radiation. Lancet Oncology. 2022;23(4):e167-e179.
- Boniol M, et al. Cutaneous melanoma attributable to sunbed use: systematic review and meta-analysis. Int J Cancer. 2019;144(5):1026-1034.
- Ghiorzo P, et al. Genetic testing and management of hereditary melanoma. Eur J Cancer. 2020;125:85-97.
- Whiteman DC, et al. The molecular epidemiology of melanoma: implications for prevention and treatment. J Invest Dermatol. 2021;141(6):1278-1289.
- National Cancer Institute (NIH). SEER Cancer Statistics Review, 1975-2020. Melanoma of the Skin. Updated 2023.