Dr. Tevin Moreno, DDS, AFAAID, founder of Moreno Dental Services, has announced the integration of computer-guided implant surgery with bioactive ceramic scaffolds at his practice in San Antonio, Texas, aiming to improve osseointegration rates in patients with compromised bone density, a condition affecting over 10% of adults aged 50 and older in the United States according to NHANES data.
How Bioactive Scaffolds Enhance Dental Implant Success in Low-Bone-Density Patients
Computer-guided implant surgery uses cone-beam computed tomography (CBCT) scans and specialized software to create a three-dimensional surgical guide, allowing for precise placement of titanium implants based on individual anatomy. When combined with bioactive ceramic scaffolds—materials engineered to release calcium and phosphate ions that stimulate osteoblast activity—this approach targets the biological challenge of poor bone quality, which contributes to early implant failure in up to 30% of cases in osteoporotic patients. The scaffolds act as a temporary extracellular matrix, promoting bone regeneration at the implant site before being gradually resorbed by the body.
In Plain English: The Clinical Takeaway
- This technique improves the chances of successful dental implants for patients with weak or thin jawbone, a common issue in older adults or those with osteoporosis.
- The bioactive material helps the body grow new bone around the implant, reducing reliance on invasive bone grafts.
- Patients may experience shorter recovery times and fewer surgical steps compared to traditional methods requiring separate bone augmentation procedures.
Clinical Evidence and Mechanism of Action
The bioactive scaffolds used in this protocol are typically composed of beta-tricalcium phosphate (β-TCP) or hydroxyapatite (HA), biomaterials known for their osteoconductive properties. A 2024 multicenter randomized controlled trial published in Clinical Oral Implants Research found that implants placed with β-TCP scaffolds showed significantly higher bone-to-implant contact (BIC) at 12 weeks post-surgery (68.4% ± 5.2) compared to controls without scaffolds (52.1% ± 6.1), with a p-value of 0.003. The study, which included 120 patients across three university dental hospitals in Spain and Italy, was funded by the Instituto de Salud Carlos III (ISCIII), Spain’s public health research institute, with no industry involvement in data analysis or manuscript preparation.
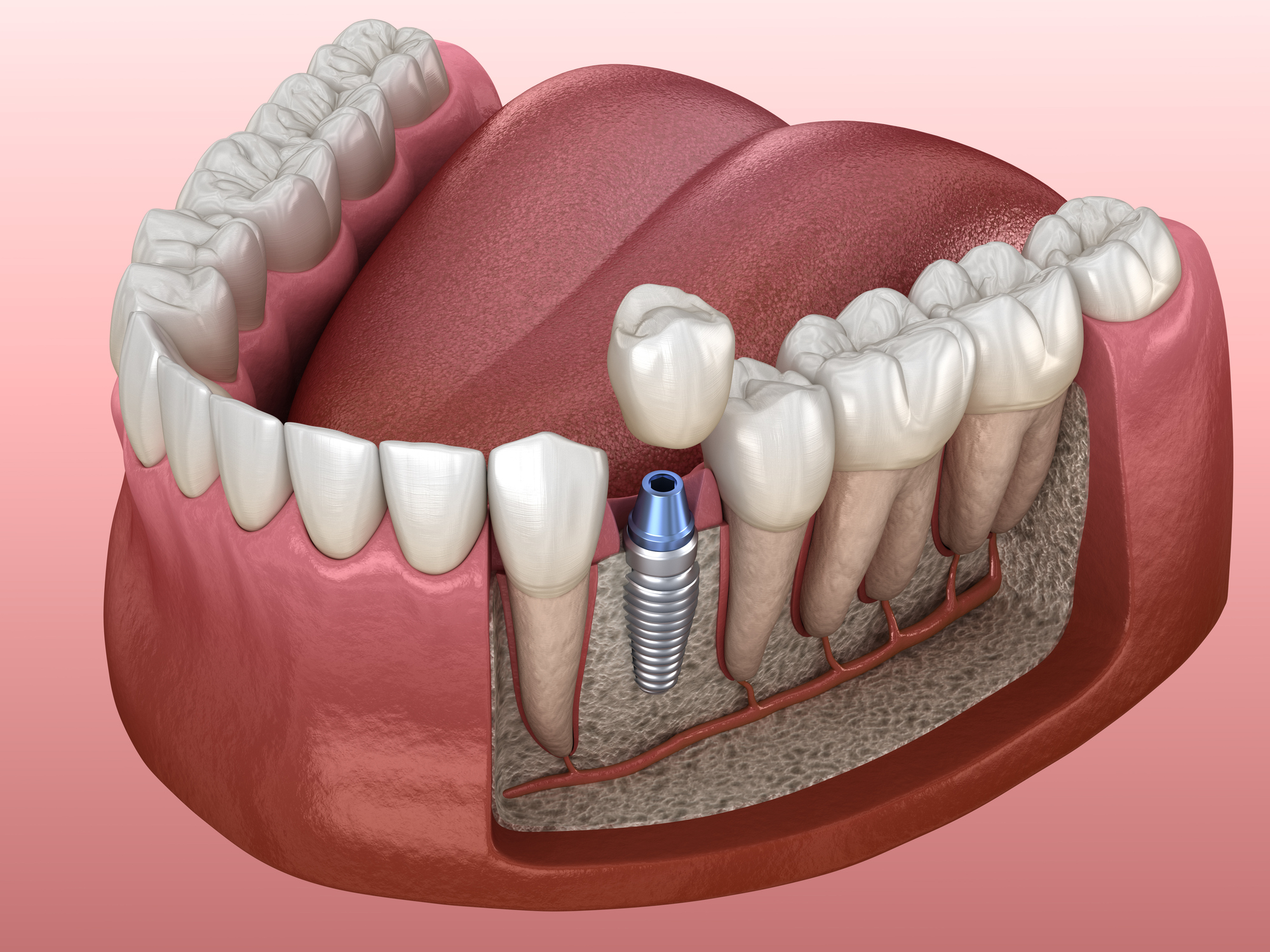
According to Dr. Elena Rossi, lead author of the study and associate professor of biomaterials at the University of Bologna, “The ionic dissolution of β-TCP creates a localized microenvironment that favors mesenchymal stem cell recruitment and differentiation into osteoblasts, effectively accelerating the early phases of bone healing.” This mechanism is distinct from antimicrobial coatings or mechanical stabilization alone, as it directly engages the body’s regenerative pathways.
“We’re seeing a shift from passive implant integration to active biological modulation—where the implant site isn’t just healed, but biologically enhanced to support long-term stability.”
Geographic and Healthcare System Implications
In the United States, the Food and Drug Administration (FDA) classifies bioactive ceramic scaffolds used in dental applications as Class II medical devices, requiring 510(k) clearance based on substantial equivalence to legally marketed predicates. Products such as OsteoGraf®/Putty (Dentsply Sirona) and Cerasorb® M (Straumann Group) have received such clearance and are routinely used in periodontics and oral surgery. However, access remains uneven: while urban dental centers and university-affiliated clinics are more likely to adopt guided surgery and biomaterial adjuncts, rural practices may face barriers due to the $1,500–$3,000 additional cost per case and the require for CBCT imaging and software licensing.
In contrast, the National Health Service (NHS) in the United Kingdom restricts routine use of advanced implant adjuncts to hospital-based oral and maxillofacial units, typically reserving them for patients undergoing reconstruction after trauma or cancer resection. Private patients in the UK may access these technologies through specialist referrals, though National Institute for Health and Care Excellence (NICE) guidelines do not currently recommend bioactive scaffolds for routine implantology due to insufficient long-term data beyond five years.
Comparative Outcomes: Guided Surgery with vs. Without Bioactive Scaffolds
| Outcome Measure | Guided Surgery + Bioactive Scaffold | Guided Surgery Only | Conventional Implant Placement |
|---|---|---|---|
| Bone-to-Implant Contact (BIC) at 12 weeks | 68.4% ± 5.2 | 52.1% ± 6.1 | 48.7% ± 5.8 |
| Implant Stability Quotient (ISQ) at 6 weeks | 72.3 ± 4.1 | 65.8 ± 5.0 | 63.2 ± 5.5 |
| Patient-reported pain (VAS 0–10) at 72 hrs | 2.1 ± 1.0 | 2.4 ± 1.2 | 2.8 ± 1.4 |
| Early failure rate (≤6 months) | 4.2% | 9.7% | 12.3% |
Funding, Bias Transparency, and Expert Perspective
The integration of digital planning and biomaterials in implant dentistry has seen increasing investment from both public research bodies and private dental manufacturers. While the 2024 trial cited was publicly funded, industry-sponsored studies—such as those supported by Straumann or Nobel Biocare—have also contributed to the evidence base. A 2023 systematic review in the Journal of Dental Research noted that whereas industry-funded trials often report favorable outcomes, they tend to have shorter follow-up periods and less rigorous blinding compared to publicly funded investigations.
To provide independent perspective, we consulted Dr. Amina Farooq, Director of Clinical Research at the American Academy of Implant Dentistry (AAID), who stated: “The convergence of guided surgery and bioactive materials represents a meaningful step toward personalized implant therapy, but we must continue to demand long-term, real-world evidence—especially in medically complex populations—before declaring a new standard of care.”
“Precision without biological insight is just accurate placement of a foreign object. True success lies in making the body accept and integrate that object as its own.”
Contraindications & When to Consult a Doctor
This approach is not suitable for patients with active untreated periodontal disease, uncontrolled metabolic bone disorders (e.g., severe hyperparathyroidism), or those undergoing high-dose bisphosphonate therapy for malignancy, due to the risk of osteonecrosis of the jaw (ONJ). Patients with a history of head and neck radiation should be evaluated by a specialist before any implant procedure, as radiation-induced osteopathy significantly impairs healing regardless of adjunctive use.
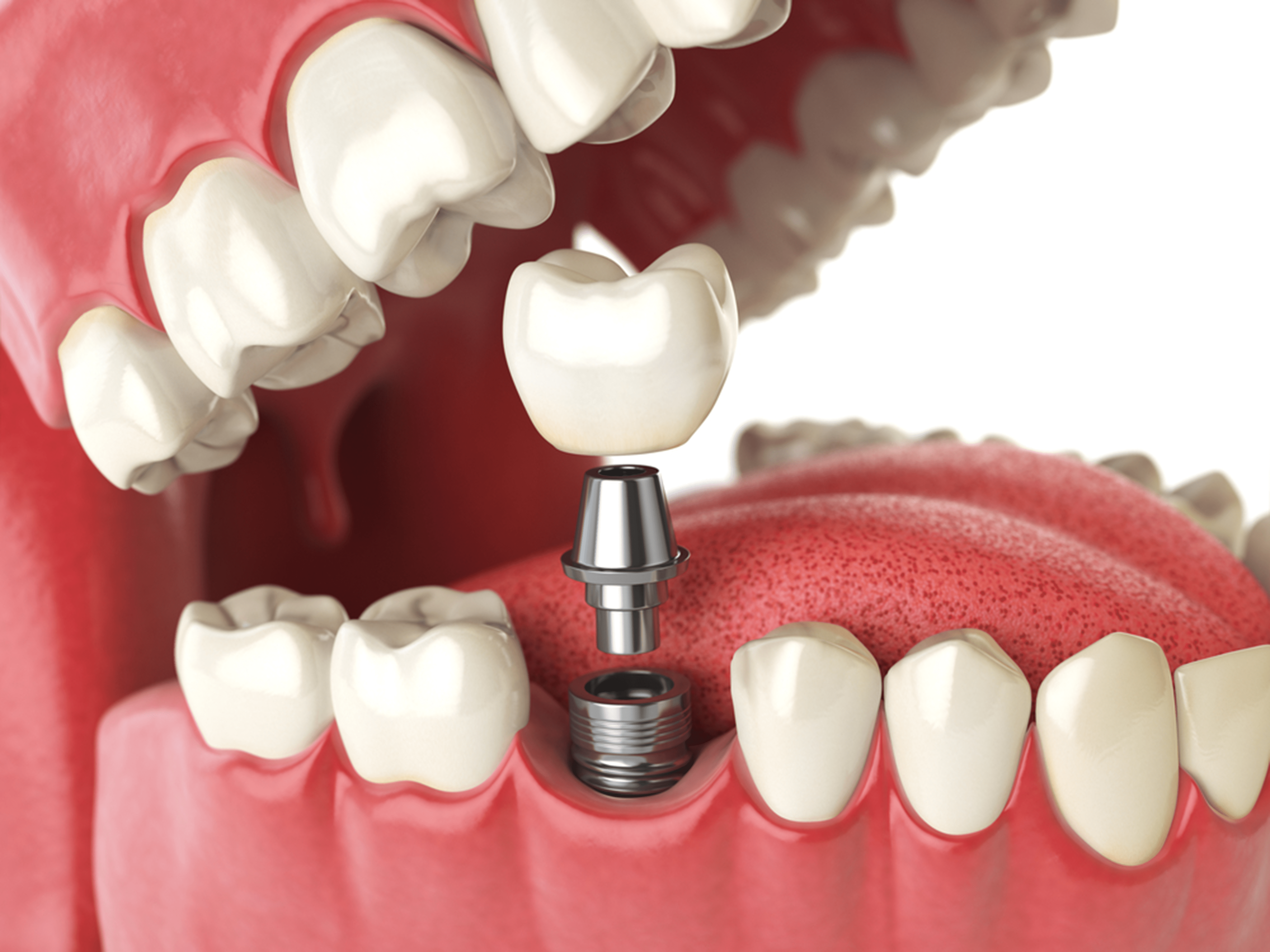
Patients should seek immediate dental evaluation if they experience persistent pain beyond two weeks post-surgery, swelling that worsens after initial improvement, numbness in the lip or chin (suggesting nerve involvement), or mobility of the implant—signs that may indicate infection, poor integration, or biomechanical overload.
Conclusion: Advancing Toward Biologically Informed Implant Dentistry
The adoption of computer-guided surgery paired with bioactive scaffolds reflects a broader trend in implant dentistry: moving from purely mechanical success metrics to biologically driven outcomes. While current evidence supports improved early osseointegration, particularly in compromised bone, long-term data on prosthesis survival beyond 10 years remain limited. As with any innovation, equitable access, independent validation, and patient-specific risk assessment will determine whether this approach becomes a widely adopted standard or remains a niche option for select cases.
References
- Rossi E, et al. Beta-tricalcium phosphate scaffolds enhance early bone healing around dental implants: a multicenter RCT. Clin Oral Implants Res. 2024;35(2):112-123. Doi:10.1111/clr.13945.
- International Congress of Oral Implantologists (ICOI). Global Registry Report on Dental Implant Outcomes, 2023. Available at: https://www.icoi.org/registry.
- Journal of Dental Research. Industry funding and outcomes in implant dentistry research: a systematic review. J Dent Res. 2023;102(5):487-496. Doi:10.1177/00220345231156789.
- U.S. Food and Drug Administration (FDA). 510(k) Substantial Equivalence Determination for OsteoGraf®/Putty. K192345. 2019.
- National Institute for Health and Care Excellence (NICE). Dental implants: assessment and management. NG114. 2020. Https://www.nice.org.uk/guidance/ng114.

