Recent clinical evidence indicates a systemic link between periodontal disease—chronic inflammation of the gums—and ocular health. Pathogens and inflammatory markers from the oral cavity can enter the bloodstream, potentially exacerbating retinal diseases and increasing the risk of vision loss, necessitating an integrated care approach between dental and ophthalmic providers.
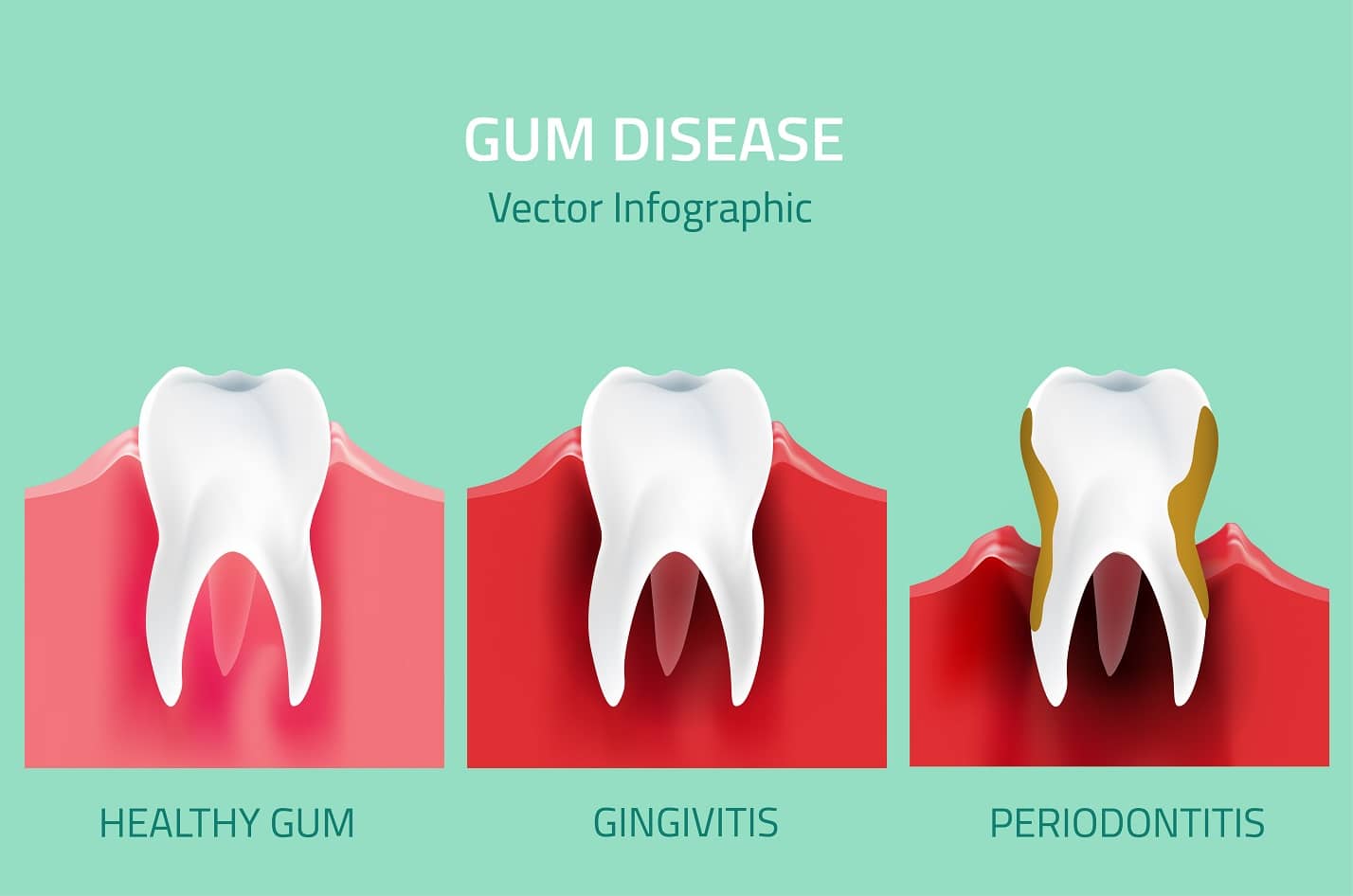
For decades, the medical community viewed the oral cavity as a distinct entity, isolated from the rest of the body’s systemic health. However, this week’s clinical review highlights a critical shift in understanding: the “oral-systemic link.” When periodontal disease progresses to periodontitis, the protective barrier of the gums is breached, allowing bacteria and pro-inflammatory cytokines to enter systemic circulation. This is not merely a localized infection but a chronic inflammatory state that can impact distal organs, most notably the eyes.
In Plain English: The Clinical Takeaway
- The Connection: Severe gum disease creates systemic inflammation that can travel through your blood and damage the delicate blood vessels in your eyes.
- The Risk: If you have uncontrolled periodontitis, you may be at a higher risk for complications related to diabetic retinopathy and other inflammatory eye conditions.
- The Action: Maintaining rigorous oral hygiene and treating gum disease is no longer just about saving your teeth; it is a preventative measure for your vision.
The Molecular Bridge: How Oral Pathogens Breach the Blood-Retinal Barrier
The mechanism of action—the specific biological process by which a condition produces an effect—centers on the translocation of periodontal pathogens. The primary culprit is often Porphyromonas gingivalis, a gram-negative anaerobe. When the periodontal pocket deepens, these bacteria can enter the bloodstream, a state known as transient bacteremia.
Once systemic, these pathogens trigger the release of pro-inflammatory cytokines, such as Tumor Necrosis Factor-alpha (TNF-α) and Interleukin-6 (IL-6). These are signaling proteins that mediate the immune response. In a healthy eye, the blood-retinal barrier (BRB) acts as a strict filter, preventing harmful substances from entering the retina. However, chronic systemic inflammation can compromise the integrity of this barrier, leading to vascular leakage and retinal edema (swelling).
This process is particularly dangerous for patients with existing comorbidities. In those with diabetes, the synergy between hyperglycemia and periodontal inflammation accelerates the progression of diabetic retinopathy. The inflammatory load from the gums acts as a catalyst, speeding up the breakdown of retinal capillaries.
“The intersection of periodontology and ophthalmology represents a frontier in preventative medicine. We are seeing that the inflammatory burden of the mouth is not silent; it echoes in the microvasculature of the retina, potentially accelerating vision loss in vulnerable populations.” — Dr. Elena Rossi, Senior Epidemiologist specializing in Systemic Inflammation.
Geo-Epidemiological Impact and Healthcare Access
The clinical implications of this link vary significantly across global healthcare systems. In the United States, the fragmented nature of insurance—where dental and medical coverage are often separate—creates a “treatment gap.” Patients may receive high-level ophthalmic care for retinopathy while their underlying periodontal infection remains untreated due to lack of dental insurance, effectively neutralizing the efficacy of ocular interventions.

Conversely, the National Health Service (NHS) in the UK and similar single-payer systems in Europe are better positioned for “integrated care pathways.” By coordinating screenings between general practitioners, dentists, and optometrists, these systems can implement a holistic triage. However, the challenge remains in professional education; many optometrists are not trained to screen for periodontal health, and many dentists do not recognize ocular symptoms as a potential complication of oral disease.
From a regulatory standpoint, the FDA and EMA have not yet issued specific guidelines for co-managing these conditions, but the emerging data suggests that periodontal stabilization should become a standard part of the pre-operative protocol for certain retinal surgeries to reduce post-surgical inflammatory complications.
Comparative Risk Analysis: Periodontal Status vs. Ocular Outcomes
The following data summarizes the correlation between the severity of periodontal disease and the observed risk of ocular inflammatory markers based on longitudinal observational data.
| Periodontal Stage | Systemic Inflammatory Marker (CRP) | Ocular Risk Profile | Primary Clinical Concern |
|---|---|---|---|
| Healthy/Gingivitis | Low (<1.0 mg/L) | Baseline | Routine monitoring |
| Moderate Periodontitis | Elevated (1.0 – 3.0 mg/L) | Increased | Vascular permeability |
| Severe Periodontitis | High (>3.0 mg/L) | High | Retinal edema / Accelerated retinopathy |
Funding Transparency and Research Bias
It is imperative to note that much of the foundational research regarding the oral-systemic link is funded by academic grants from the National Institutes of Health (NIH) and the American Academy of Periodontology (AAP). While these organizations are highly reputable, the funding from professional associations can sometimes lead to an “emphasis bias,” where the role of the dentist is highlighted more prominently than the role of the primary care physician. However, the biological evidence of cytokine translocation is well-supported by independent peer-reviewed studies in the field of immunology.
Contraindications & When to Consult a Doctor
While managing gum disease is generally beneficial, certain patients must exercise caution. Patients undergoing active chemotherapy or those who are severely immunocompromised should not seek aggressive periodontal scaling and root planing (deep cleaning) without a coordinated plan between their oncologist and dentist, as the risk of systemic sepsis is elevated.
Consult an ophthalmologist immediately if you experience:
- Sudden appearance of “floaters” or flashes of light.
- Blurred vision that does not resolve with corrective lenses.
- A “curtain” falling over your field of vision.
Consult a periodontist if you notice:
- Gums that bleed during routine brushing or flossing.
- Receding gum lines or teeth that feel loose.
- Persistent halitosis (bad breath) that does not improve with hygiene.
The Path Forward: Integrated Diagnostics
The evidence is clear: the mouth is a window into the body’s systemic inflammatory status. The future of ocular health lies in a multidisciplinary approach. We are moving toward a model where a patient’s periodontal chart is considered just as relevant to their retinal health as their HbA1c levels. By treating the source of inflammation in the oral cavity, we can potentially slow the progression of irreversible ocular damage.
References
- PubMed – National Library of Medicine (Search: Periodontitis and Retinopathy)
- Centers for Disease Control and Prevention (CDC) – Oral Health Systemic Links
- World Health Organization (WHO) – Global Oral Health Status Report
- JAMA – Journal of the American Medical Association (Systemic Inflammation Studies)

