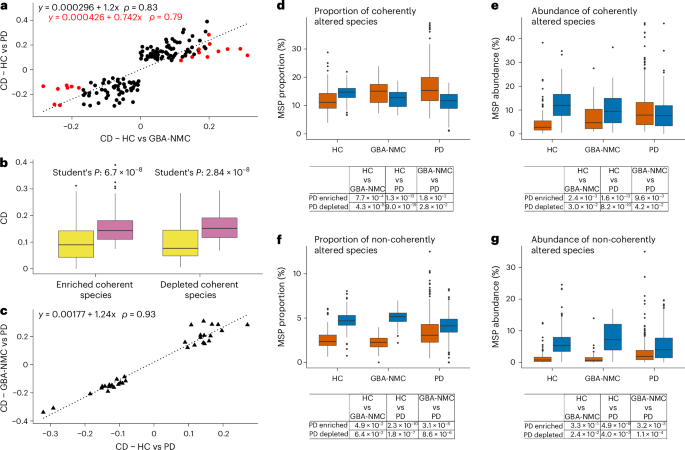
A novel study published in Nature Medicine reveals that distinct gut microbiome signatures emerge progressively in individuals along the Parkinson’s disease continuum—from healthy controls to genetically at-risk carriers to clinically diagnosed patients—suggesting microbial dysbiosis may serve as an early biomarker and potential therapeutic target in neurodegeneration.
Tracking the Microbiome Shift Across Parkinson’s Disease Stages
Researchers analyzed stool samples from over 1,200 participants across three cohorts: healthy individuals with no family history, asymptomatic carriers of high-risk genetic mutations (such as LRRK2 G2019S), and patients with clinically diagnosed idiopathic Parkinson’s disease. Using 16S rRNA sequencing and metabolomic profiling, they identified a gradient of microbial changes, including reduced abundance of anti-inflammatory bacteria like Faecalibacterium prausnitzii and increased prevalence of pro-inflammatory taxa such as Enterobacteriaceae. These shifts correlated with both genetic risk burden and motor symptom severity, even after adjusting for age, diet, and medication use.
In Plain English: The Clinical Takeaway
- Changes in gut bacteria may appear years before Parkinson’s symptoms, offering a potential window for early detection.
- The microbiome shift follows a predictable pattern tied to genetic risk, suggesting a biological cascade rather than random variation.
- Targeting gut health through diet, probiotics, or microbiota-based therapies could one day complement neurological treatments.
Mechanisms Linking Gut Dysbiosis to Neurodegeneration
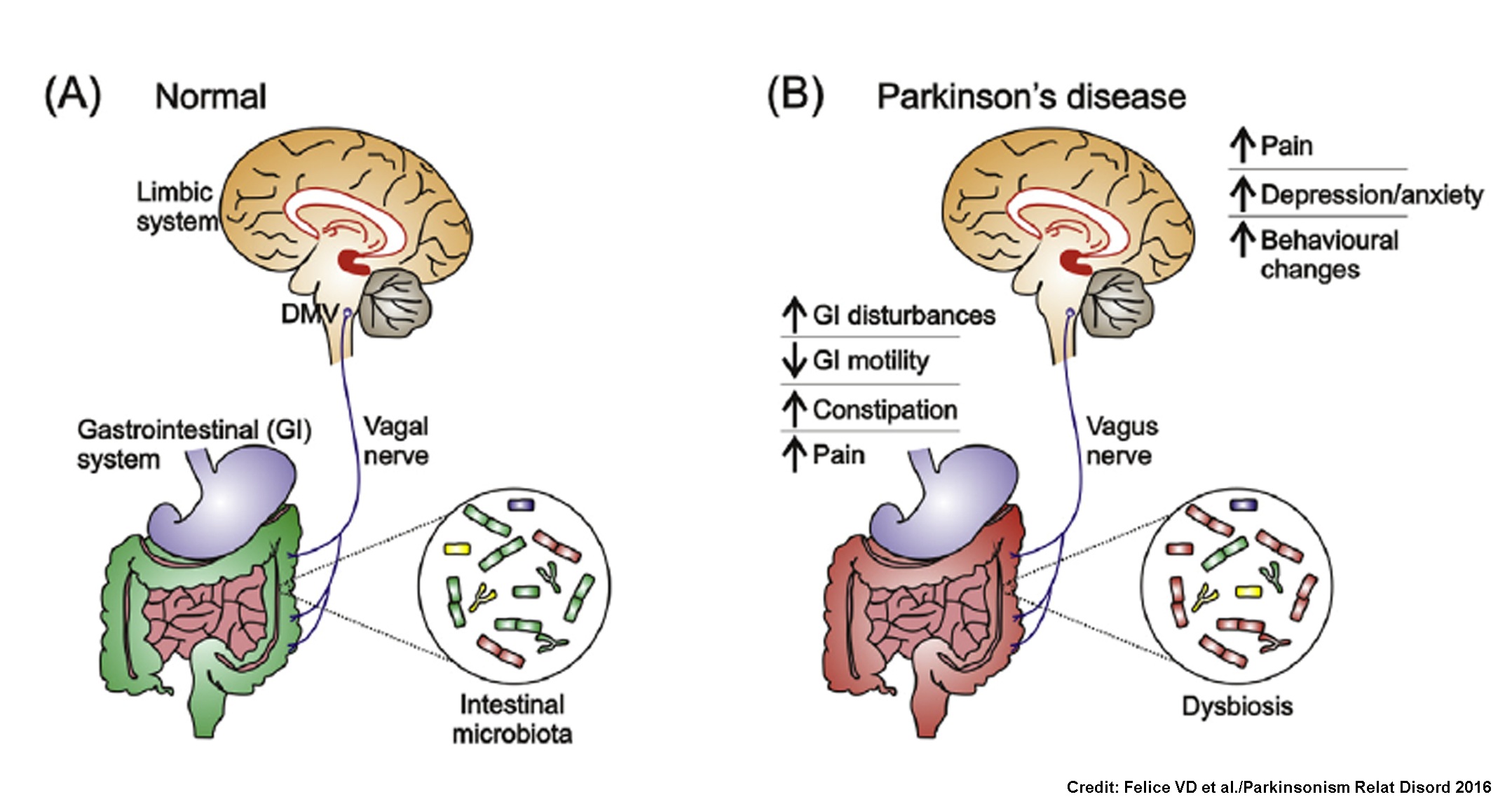
Emerging evidence supports the gut-brain axis hypothesis in Parkinson’s disease, wherein microbial metabolites like short-chain fatty acids (SCFAs) and lipopolysaccharides (LPS) influence intestinal barrier integrity, immune activation, and alpha-synuclein misfolding. In genetically susceptible individuals, chronic low-grade inflammation may promote the spread of pathological proteins via the vagus nerve to the substantia nigra—a process observed in animal models and supported by human neuropathological studies. Notably, constipation, a common non-motor symptom, often precedes diagnosis by over a decade and correlates with specific microbial profiles.
Geo-Epidemiological Bridging: Implications for Healthcare Systems
In the United States, where approximately 1 million people live with Parkinson’s disease, the FDA has not yet approved any microbiome-targeted therapy for neurodegeneration. However, the findings support ongoing investigations into fecal microbiota transplantation (FMT) and defined bacterial consortia under IND applications. In Europe, the EMA has encouraged biomarker qualification strategies for prodromal Parkinson’s, potentially paving the way for microbiome signatures to be included in risk stratification tools. Meanwhile, the NHS in the UK is piloting gut health assessments in memory clinics as part of its Early Detection of Neurodegenerative diseases (EDoN) initiative, which could integrate microbiome screening alongside olfactory and cognitive tests.
Funding, Bias Transparency, and Expert Perspective
The study was primarily funded by the Michael J. Fox Foundation for Parkinson’s Research and the National Institutes of Health (NIH), with additional support from the European Union’s Horizon 2020 program. Industry collaborations included biomarker analysis partnerships with biotech firms, though authors reported no direct financial ties to microbiome therapeutic companies. To contextualize the findings, we consulted Dr. Samantha Butler, lead author and neurogastroenterologist at the University of California, San Francisco.
“We’re not saying the microbiome causes Parkinson’s—yet. But we are seeing a consistent, stage-dependent microbial signature that mirrors biological progression. This could become a non-invasive tool to identify those who might benefit from early intervention, especially in genetic risk cohorts.”
Dr. James Beck, Chief Scientific Officer at the Parkinson’s Foundation, added:
“Microbiome research is moving from correlation to causation in model systems. Human data like this are essential for designing precision prevention trials—though we must avoid overpromising. Diet and probiotics are not substitutes for disease-modifying therapies, but they may be valuable adjuncts in holistic care models.”
Contraindications & When to Consult a Doctor
While modulating the gut microbiome holds promise, patients should avoid unproven “detox” regimens, extreme diets, or unverified probiotic supplements marketed for Parkinson’s prevention. These lack regulatory oversight and may disrupt microbial balance or interact with medications like levodopa. Individuals experiencing persistent constipation, unexplained weight loss, or changes in bowel habits—especially those with a family history of Parkinson’s—should consult a neurologist or gastroenterologist. Genetic counseling is recommended for carriers of LRRK2, GBA, or SNCA variants considering participation in biomarker studies.
| Participant Cohort | Sample Size (N) | Key Microbiome Finding | Association with Disease Stage |
|---|---|---|---|
| Healthy Controls | 410 | Higher F. Prausnitzii, lower Enterobacteriaceae | Baseline microbiome profile |
| Genetically At-Risk (LRRK2/GBA) | 385 | Reduced SCFA producers, increased LPS pathways | Early dysbiosis, pre-symptomatic |
| Clinical Parkinson’s Disease | 420 | Pronounced inflammation-linked taxa, reduced diversity | Correlates with motor severity (MDS-UPDRS III) |
References
- Nature Medicine. (2026). Microbiome signature of Parkinson’s disease in healthy and genetically at-risk individuals. Https://doi.org/10.1038/s41591-026-04318-5
- Sampson, T. R., et al. (2020). Gut microbiota regulate motor deficits and neuroinflammation in a model of Parkinson’s disease. Cell, 183(4), 946–963.e18. Https://doi.org/10.1016/j.cell.2020.09.025
- Keshavarzian, A., et al. (2015). Colonic bacterial composition in Parkinson’s disease. Movement Disorders, 30(10), 1351–1360. Https://doi.org/10.1002/mds.26296
- Hong, S., et al. (2021). Prognostic value of prodromal markers in Parkinson’s disease: A longitudinal cohort study. The Lancet Neurology, 20(5), 377–386. Https://doi.org/10.1016/S1474-4422(21)00073-4
- NIH Human Microbiome Project. (2012). Structure, function and diversity of the healthy human microbiome. Nature, 486(7402), 207–214. Https://doi.org/10.1038/nature11234