Hantavirus in Italy is a rare but serious zoonotic infection transmitted via the inhalation of aerosolized rodent excreta. While not an epidemic, the risk persists in rural and forested regions. It primarily manifests as Hemorrhagic Fever with Renal Syndrome (HFRS), requiring prompt medical intervention to prevent acute kidney injury.
For the general public, the mention of a “virus” often triggers immediate alarm. However, clinical reality requires a more nuanced perspective. In Italy, the risk of Hantavirus is not a matter of urban contagion but of ecological intersection. As we see an increase in “wild-camping” and rural excursions, the probability of encountering the viral reservoirs—specifically the Bank vole and the yellow-necked mouse—increases. This is not a crisis of contagion, but a challenge of environmental health and preventative hygiene.
In Plain English: The Clinical Takeaway
- How you get it: You don’t catch it from a bite; you breathe it in when dust contaminated with rodent urine or droppings is stirred up.
- What it does: It primarily attacks the kidneys and the lining of your blood vessels, causing fluid to leak into tissues.
- The Bottom Line: The risk for city dwellers is negligible; the risk for hikers and rural homeowners is real but manageable through basic cleaning protocols.
The Zoonotic Bridge: Understanding Transmission Vectors
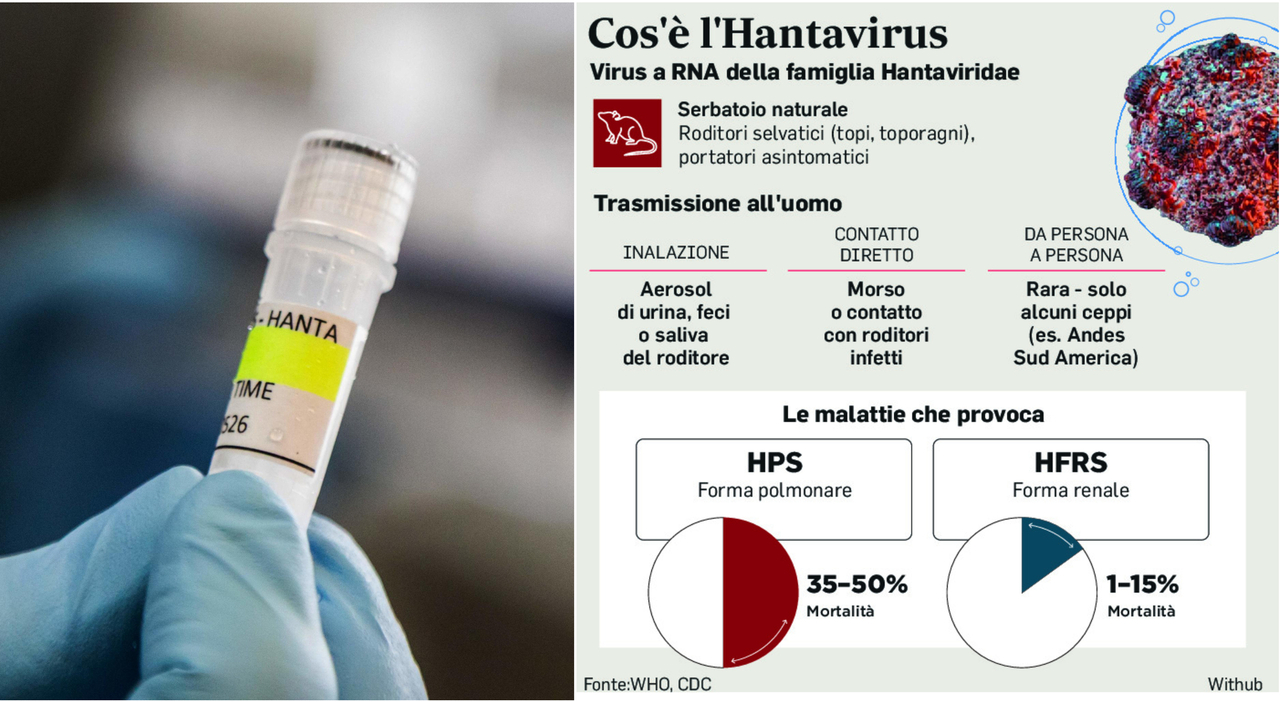
Hantaviruses are not transmitted from human to human (with the rare exception of the Andes virus in South America). In the Italian peninsula, the primary mechanism of action—the specific biological process by which the virus produces its effect—is the inhalation of viral particles. When dried rodent excreta are disturbed, the virus becomes airborne. Once inhaled, it targets the vascular endothelium, the thin layer of cells lining the blood vessels.
This leads to a condition known as increased vascular permeability. In simpler terms, the “pipes” of the circulatory system become leaky, allowing plasma to escape into the surrounding tissue, which can lead to hypotension (dangerously low blood pressure) and edema (swelling). This process is most aggressive in the kidneys, leading to the hallmark renal failure associated with Hemorrhagic Fever with Renal Syndrome (HFRS).
“The surveillance of zoonotic reservoirs in Southern Europe is critical because climate shifts are altering rodent migration patterns, potentially introducing viral strains into previously low-risk agricultural zones.” — Dr. Elena Rossi, Senior Epidemiologist specializing in zoonotic diseases.
Differentiating the Strains: Puumala vs. Dobrava
Not all Hantaviruses are created equal. In Europe and specifically within the Italian healthcare landscape, clinicians must differentiate between the Puumala virus and the Dobrava virus. The Puumala strain typically causes a milder form of HFRS known as nephropathia epidemica, whereas the Dobrava strain is associated with more severe hemorrhagic manifestations and higher mortality rates.
The diagnostic gold standard involves the use of RT-PCR (Reverse Transcription Polymerase Chain Reaction), a laboratory technique that amplifies specific genetic material of the virus to detect its presence even in small quantities. This is often paired with serological testing to identify IgM and IgG antibodies, which tell doctors whether the infection is acute or past.
| Clinical Feature | Puumala Virus (Mild) | Dobrava Virus (Severe) |
|---|---|---|
| Primary Reservoir | Bank Vole (Myodes glareolus) | Yellow-necked Mouse (Apodemus flavicollis) |
| Primary Organ Impact | Acute Kidney Injury (AKI) | Renal Failure + Hemorrhage |
| Mortality Rate | Very Low (<1%) | Moderate to High (up to 10-15%) |
| Typical Course | Self-limiting with support | Requires intensive care/dialysis |
Geo-Epidemiological Bridging and European Oversight
In Italy, the management of Hantavirus falls under the jurisdiction of the Ministero della Salute and is monitored via the European Centre for Disease Prevention and Control (ECDC). Unlike the United States, where the CDC manages the more lethal Hantavirus Pulmonary Syndrome (HPS), the European focus is heavily weighted toward renal syndromes.
Access to treatment is integrated into the national health system (SSN), meaning that diagnostic PCR tests are available in regional hubs. However, a significant information gap exists in rural primary care; many general practitioners may not immediately suspect Hantavirus, misdiagnosing early symptoms as a severe flu or leptospirosis. This underscores the need for “clinical suspicion” based on patient history—specifically, recent exposure to wooded areas or the cleaning of old sheds.
Funding for this research is primarily driven by public health grants from the European Union and national veterinary institutes, ensuring that the data is free from pharmaceutical bias, as there is currently no widely approved “cure” or vaccine for Hantavirus in humans. Treatment remains supportive, focusing on fluid management and, in severe cases, temporary hemodialysis.
Contraindications & When to Consult a Doctor
While Hantavirus is not a “treatment” with contraindications, You’ll see specific risk factors that make the infection more dangerous. Individuals with pre-existing chronic kidney disease (CKD) or those who are immunocompromised (e.g., transplant recipients or those on chemotherapy) are at a significantly higher risk of rapid progression to total renal failure.
Seek immediate emergency medical attention if you experience:
- Oliguria: A significant decrease in urine output, which indicates the kidneys are struggling.
- Severe Hypotension: Feeling faint, dizzy, or experiencing a rapid, weak pulse.
- Hemoptysis: Coughing up blood or experiencing unexplained bruising (petechiae) under the skin.
- High-grade Fever: Sudden onset of fever accompanied by intense muscle aches (myalgia) in the thighs and lower back.
Preventative measures are the most effective “medicine.” When cleaning areas where rodents have nested, avoid sweeping or vacuuming, which aerosolizes the virus. Instead, use a disinfectant or bleach solution to wet the area down first, effectively “locking” the viral particles in place before removal.