As of mid-May 2026, public health monitoring systems are distinguishing between norovirus, COVID-19, and hantavirus—three distinct pathogens with vastly different transmission vectors and clinical outcomes. Understanding these differences is critical for patient triage, as diagnostic precision prevents the misuse of antivirals and ensures appropriate supportive care for patients.
In Plain English: The Clinical Takeaway
- Norovirus: Primarily a foodborne and contact-based gastrointestinal pathogen. Focus on aggressive fluid replacement to manage dehydration.
- COVID-19: A respiratory virus requiring monitoring for systemic inflammatory responses and potential pulmonary involvement.
- Hantavirus: A zoonotic infection contracted via aerosolized rodent excreta; it presents as a severe cardiopulmonary syndrome requiring urgent intensive care.
Differential Pathophysiology: Mechanisms of Infection
To differentiate these pathogens, we must look at their mechanism of action. Norovirus is a non-enveloped, single-stranded RNA virus that causes acute gastroenteritis by binding to histo-blood group antigens (HBGAs) on the intestinal epithelium, leading to rapid viral shedding. Conversely, SARS-CoV-2 utilizes the angiotensin-converting enzyme 2 (ACE2) receptor to enter host cells, primarily in the respiratory tract, triggering a localized cytokine storm that can escalate into systemic vasculitis.
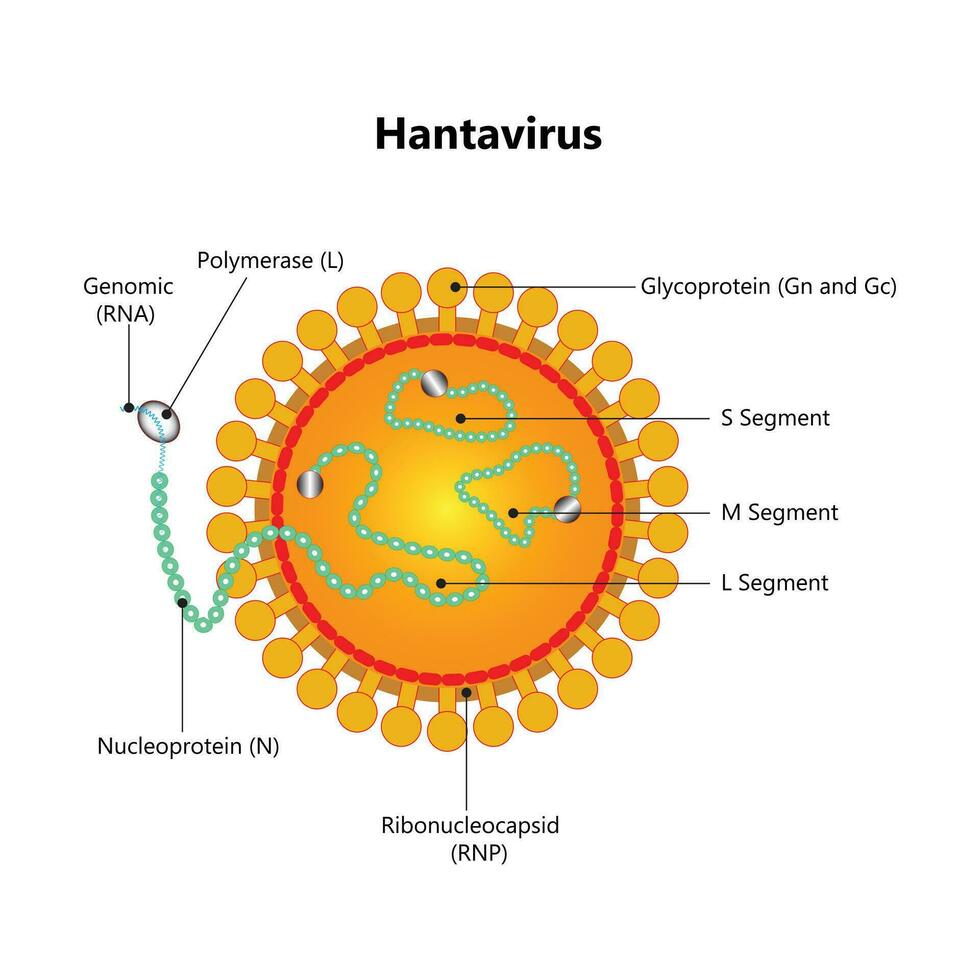
Hantavirus (specifically New World species like Sin Nombre) operates through a different modality. Upon inhalation of aerosolized virus from infected rodent urine or feces, the virus targets vascular endothelial cells. This leads to increased capillary permeability—essentially “leaky” blood vessels—which causes the hallmark pulmonary edema (fluid in the lungs) and hypotension seen in Hantavirus Pulmonary Syndrome (HPS).
“The critical challenge with emerging zoonotic threats like hantavirus is the overlap in early febrile symptoms with more common respiratory viruses. Clinicians must maintain a high index of suspicion based on patient history, particularly exposure to rodent-infested environments, rather than relying on standard viral panels alone.” — Dr. Elena Rossi, Senior Epidemiologist, Institute for Tropical Medicine.
Clinical Comparison: Transmission and Symptomology
| Pathogen | Primary Transmission | Clinical Hallmark | Incubation Period |
|---|---|---|---|
| Norovirus | Fecal-oral / Contaminated surfaces | Explosive emesis / Diarrhea | 12–48 hours |
| COVID-19 | Aerosol / Droplets | Cough / Fever / Dyspnea | 2–14 days |
| Hantavirus | Aerosolized rodent excreta | Rapid onset pulmonary edema | 1–8 weeks |
Geo-Epidemiological Bridging and Regulatory Oversight
In the United States, the FDA and CDC maintain strict surveillance protocols for Hantavirus, classifying it as a nationally notifiable condition. Unlike COVID-19, which has a robust global diagnostic infrastructure, hantavirus testing is often centralized in state public health laboratories due to the specialized biosafety level (BSL-3) required to handle the virus. For patients, Which means that while a COVID-19 test is accessible at a local pharmacy, a hantavirus diagnosis requires a high degree of clinical suspicion and coordination with regional public health authorities.

Recent research indicates that climate-driven shifts in rodent migration patterns are altering the geographic footprint of hantavirus, making it a growing concern for rural health systems that may have previously classified such cases as atypical pneumonia. Transparency in research funding remains vital; much of the ongoing surveillance data for hantavirus is federally funded through the National Institutes of Health (NIH), ensuring that findings remain in the public domain rather than being influenced by commercial pharmaceutical interests.
For further reading on current transmission trends and diagnostic criteria, clinicians and patients are encouraged to review the latest guidance from the CDC Hantavirus Resource Center and the Lancet Infectious Diseases archives regarding zoonotic spillover events.
Contraindications & When to Consult a Doctor
Patients should distinguish between self-limiting symptoms and acute distress. If you experience persistent vomiting with an inability to keep fluids down (norovirus risk), you must seek medical attention to prevent electrolyte imbalance. For respiratory symptoms, monitor your oxygen saturation via pulse oximetry. If you experience shortness of breath, chest tightness, or a sudden drop in blood pressure, this is a medical emergency requiring immediate hospitalization.
Contraindications for home management include:
- Immunocompromised status: Patients on biologicals or chemotherapy must consult their primary specialist at the first sign of fever.
- Underlying cardiovascular disease: Increased fluid burden or respiratory stress can precipitate cardiac events.
- Neurological deficits: Confusion or altered mental status is a red flag for systemic infection and requires immediate emergency department triage.
The Future of Viral Surveillance
The convergence of these distinct viral threats highlights the necessity of a “One Health” approach—an integrated effort that considers the health of humans, animals, and the environment. As weather patterns become more volatile, the spillover risk for zoonotic diseases like hantavirus is expected to fluctuate. By maintaining rigorous diagnostic standards and fostering collaboration between regional health departments and academic researchers, the medical community can better mitigate the impact of these diverse pathogens.
References
- National Center for Biotechnology Information (NCBI): Molecular Pathogenesis of Hantavirus
- World Health Organization (WHO): Norovirus Fact Sheet
- JAMA: Clinical Management of SARS-CoV-2 and its Variants
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.

