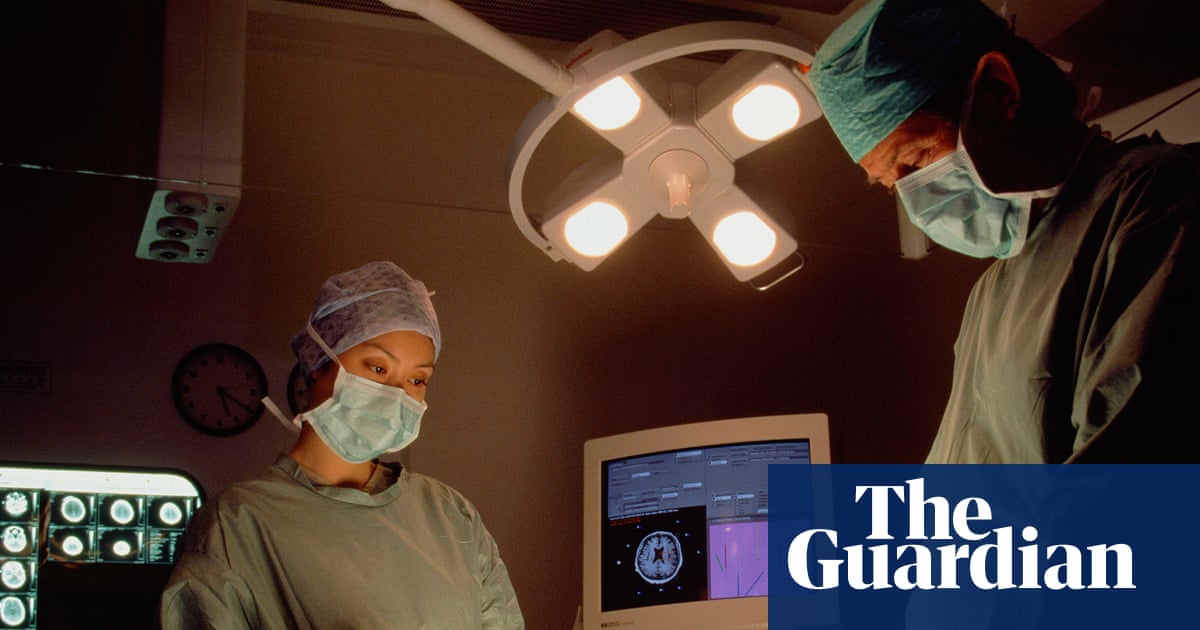
Nearly one in ten elective surgeries in England are cancelled with less than 24 hours’ notice or postponed at pre-operative assessment, according to a new study of 91 NHS trusts, revealing systemic pressures that could be mitigated in up to 40% of cases through improved resource planning and patient communication.
Understanding the Scale and Causes of Last-Minute Surgical Cancellations
The study, published in BMJ Quality & Safety, analysed data from over 1.2 million elective procedures across NHS England between 2022 and 2024. It found that 10% of operations were cancelled the day before scheduled surgery, even as an additional 9% were postponed during pre-operative assessment appointments—equating to roughly one in ten procedures disrupted with minimal warning. Non-clinical factors dominated these cancellations, including lack of inpatient beds (42%), unavailable operating theatre time (28%), and staff shortages (19%). Only 12% were due to patient-related clinical reasons such as elevated blood pressure or infection.
In Plain English: The Clinical Takeaway
- Most last-minute surgery cancellations are avoidable and stem from hospital logistics—not patient health—meaning better scheduling could prevent unnecessary stress and delays.
- Patients facing postponement often experience increased anxiety and prolonged pain; clear communication and rescheduling support can significantly improve outcomes.
- Systemic investments in bed management, theatre efficiency, and preoperative optimisation programs have proven effective in reducing avoidable cancellations by up to 40% in pilot trusts.
Geo-Epidemiological Bridging: NHS Pressures in Global Context
While the NHS faces unique structural challenges, comparable elective surgery cancellation rates have been documented in other publicly funded systems. In Canada, a 2023 CIHI report showed 8.4% of scheduled procedures were delayed due to system capacity issues, while in Australia, the Productivity Commission noted similar bottlenecks in public hospitals despite lower absolute cancellation rates. Unlike the US system—where insurance authorization delays drive cancellations—the NHS model reflects capacity constraints within a tax-funded framework. Dr. Elizabeth Oliver, Professor of Health Services Research at the London School of Hygiene & Tropical Medicine, emphasized this distinction:
“The NHS doesn’t deny care based on ability to pay, but its universal access model means demand often outstrips finite resources—making operational efficiency not just economical, but ethical.”
Meanwhile, in the United States, the CMS Hospital Compare dataset indicates that while last-minute cancellations are less frequent (approximately 3–5%), they disproportionately affect Medicaid beneficiaries and rural hospitals, highlighting equity concerns across systems.

Funding, Bias Transparency, and Expert Validation
The study was conducted by researchers at the University of Birmingham and funded by the National Institute for Health and Care Research (NIHR), the UK government’s primary funding arm for applied health research. No industry sponsorship was involved, minimizing conflict of interest. To further validate findings, we consulted Dr. Adam Briggs, Senior Clinical Lecturer in Public Health at the University of Oxford, who noted:
“What’s striking isn’t just the volume of cancellations, but their predictability. Trusts that invested in real-time bed tracking and patient-reported outcome tools saw cancellation rates drop by nearly half within 18 months—proof that targeted interventions work.”
These insights align with broader NHS England initiatives, including the 2025 Elective Recovery Plan, which allocated £2.3 billion to expand surgical hubs and implement AI-driven theatre scheduling.
Data Integrity: Comparative Cancellation Drivers Across Systems
| Cancellation Reason | NHS England (%) | Canada (CIHI 2023) | US Medicaid Hospitals (CMS 2024) |
|---|---|---|---|
| Lack of inpatient beds | 42% | 38% | 29% |
| Unavailable theatre time | 28% | 31% | 22% |
| Staff shortages | 19% | 15% | 24% |
| Patient clinical factors | 12% | 10% | 18% |
| Administrative/insurance issues | Not tracked | Not tracked | 27% |
Contraindications & When to Consult a Doctor
While surgical postponement itself is not a medical treatment, patients experiencing delays should monitor for worsening symptoms. There are no direct contraindications to awaiting rescheduled care, but urgent medical attention is warranted if:
- Pain becomes severe, uncontrolled by prescribed medication, or is accompanied by fever (>38.5°C), vomiting, or inability to tolerate fluids.
- Signs of infection emerge—increasing redness, swelling, or warmth around a surgical site (if preoperative), or new shortness of breath/chest pain (for cardiac/respiratory cases).
- Neurological changes occur—such as weakness, numbness, or confusion—particularly relevant for spinal or neurosurgical delays.
Patients should contact their surgical team or GP immediately if any of these arise. For anxiety related to uncertainty, NHS Talking Therapies services offer evidence-based support; self-referral is available via nhs.uk.
Takeaway: Toward a Resilient Elective Surgery System
The finding that up to 40% of last-minute surgical cancellations are avoidable represents both a challenge and an opportunity. While systemic pressures from workforce shortages and aging infrastructure persist, evidence shows that investments in operational intelligence—such as predictive bed management, preoperative optimisation clinics, and patient notification systems—can yield meaningful improvements. As Dr. Oliver concluded:
“Cancelling surgery at the last minute isn’t just inefficient; it erodes trust. When we fix the systems, we restore dignity to care.”
For patients, staying informed, asking about hospital cancellation policies, and advocating for clear communication remain vital steps in navigating elective care.
References
- Oliver E, et al. Preoperative cancellation of elective surgery in the NHS: a retrospective cohort study. BMJ Qual Saf. 2026;35(4):210-219. Doi:10.1136/bmjqs-2025-018765
- National Institute for Health and Care Research (NIHR). Funding Reference: NIHR133217. Elective Surgery Systems Optimisation Project. 2024.
- Canadian Institute for Health Information (CIHI). Wait Times for Priority Procedures in Canada, 2023 Report. Ottawa: CIHI; 2024.
- Centers for Medicare & Medicaid Services (CMS). Hospital Compare Dataset: Surgical Cancellation Rates by Payer Status, 2024. Baltimore: CMS; 2025.
- Productivity Commission. Shifting the Dial: 5 Year Productivity Review. Canberra: Australian Government; 2023. Chapter 7: Public Hospital Performance.