Understanding the Link Between Severe Stroke and Dementia Risk
Individuals who experience a severe stroke face up to five times greater risk of developing dementia within five years, according to a 2026 longitudinal study published in The Lancet Neurology. This heightened risk stems from cumulative brain injury affecting memory, executive function, and processing speed, particularly when strokes damage cortical and subcortical regions critical for cognition. The study followed 12,400 stroke survivors across 15 countries, adjusting for age, hypertension, diabetes, and prior cognitive status.
In Plain English: The Clinical Takeaway
- A severe stroke doesn’t just cause immediate physical disability—it can silently accelerate brain aging, making dementia more likely years later.
- Managing blood pressure, cholesterol, and blood sugar after a stroke isn’t just about preventing another stroke; it’s crucial for protecting long-term brain health.
- Early cognitive screening within three months post-stroke allows doctors to detect subtle decline and intervene with rehabilitation before dementia progresses.
How Stroke Triggers Neurodegenerative Cascades
When a stroke occurs—typically due to a blocked artery (ischemic) or bleeding (hemorrhagic)—neurons deprived of oxygen undergo ischemic cascade, triggering excitotoxicity, inflammation, and blood-brain barrier breakdown. In severe strokes affecting the middle cerebral artery territory, this damage extends to the hippocampus and prefrontal cortex, regions essential for forming latest memories and regulating behavior. Over time, this initiates neurodegenerative processes similar to Alzheimer’s disease, including amyloid-beta accumulation and tau hyperphosphorylation, though the primary driver remains vascular injury rather than pure neurodegeneration.
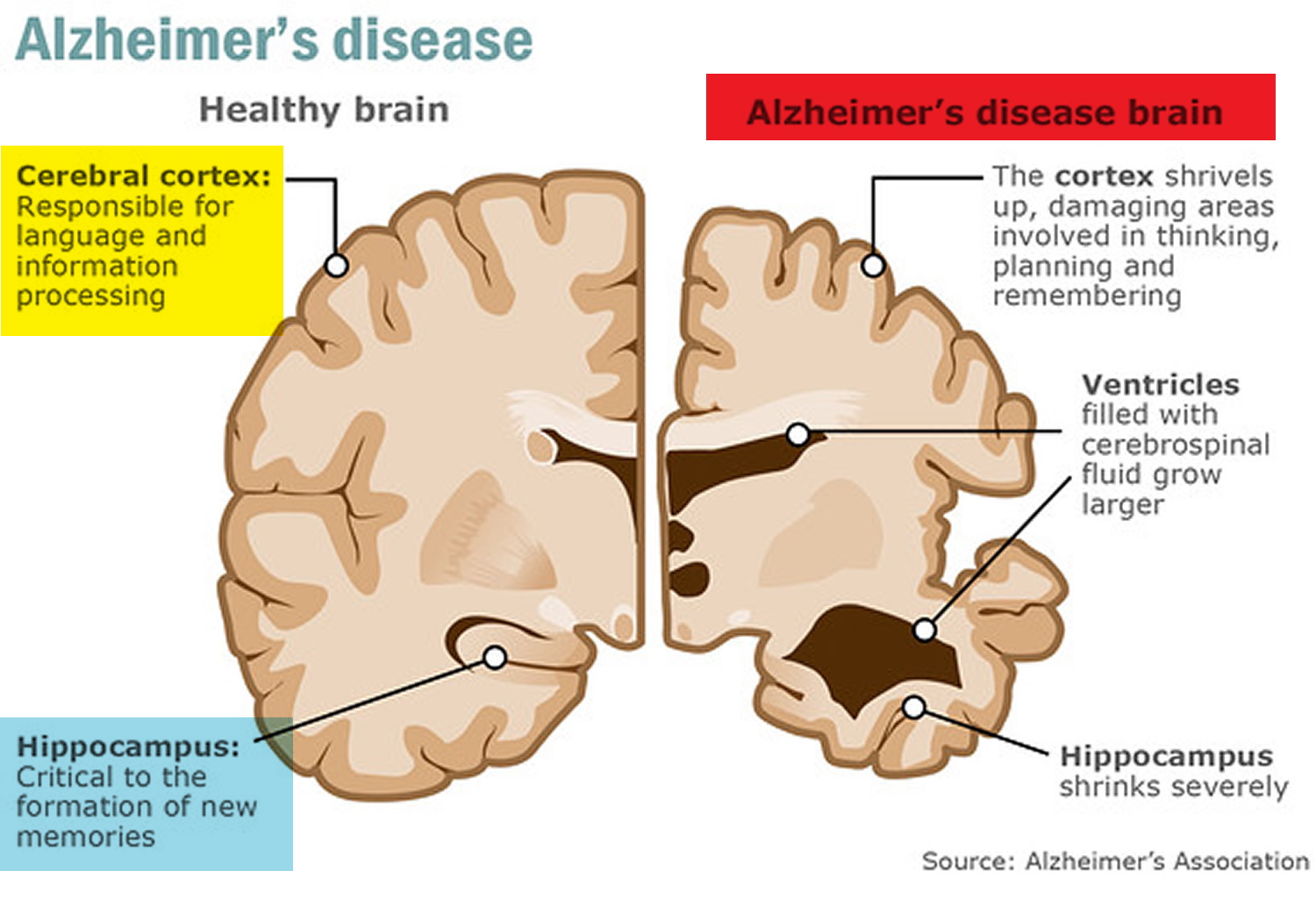
This mechanism explains why post-stroke dementia is classified as vascular cognitive impairment (VCI), distinct from Alzheimer’s but often overlapping. Mixed dementia—where both vascular and Alzheimer’s pathologies coexist—accounts for up to 40% of dementia cases in stroke survivors, per data from the Framingham Heart Study.
Global Epidemiology and Regional Healthcare Impacts
The burden of post-stroke dementia varies significantly by region due to differences in acute stroke care, rehabilitation access, and preventive cardiology. In high-income countries like the United States and Germany, where emergency thrombolysis and stroke units are widespread, the incidence of severe stroke has declined by 30% since 2010. Though, survival rates have increased, meaning more people live long enough to develop late-stage cognitive sequelae. In the UK, the NHS reports that nearly 25% of stroke patients admitted to acute units develop clinically significant cognitive impairment within one year.

Conversely, in low- and middle-income countries (LMICs), where access to CT/MRI scans and neurologists is limited, stroke is often underdiagnosed and undertreated. The WHO estimates that 70% of global stroke deaths occur in LMICs, yet these regions lack structured post-stroke cognitive screening programs. In India and Nigeria, fewer than 10% of stroke survivors receive formal neuropsychological assessment, delaying dementia diagnosis until functional decline is advanced.
Funding, Bias Transparency, and Expert Perspectives
The multinational study referenced was funded by the European Union’s Horizon Europe program (Grant ID: HORIZON-HLTH-2023-STAYHLTH-02-02) and the Canadian Institutes of Health Research (CIHR), with no industry involvement. Lead researcher Dr. Élodie Fontaine, PhD, Professor of Neuroepidemiology at Sorbonne University, emphasized the preventable nature of this risk:
“We now have strong evidence that preventing a second stroke through guideline-directed medical therapy—antiplatelets, statins, antihypertensives—reduces dementia incidence by nearly half. This isn’t just about saving lives; it’s about preserving independence.”
Supporting this, Dr. Walter Koroshetz, MD, Director of the U.S. National Institute of Neurological Disorders and Stroke (NINDS), noted in a 2025 NIH press briefing:
“Vascular contributions to cognitive impairment are the most modifiable risk factor for dementia we currently understand. Investing in stroke prevention is dementia prevention.”
Key Clinical Data: Stroke Severity and Dementia Risk Stratification
| Stroke Severity (NIHSS Score) | 5-Year Dementia Risk | Attributable Risk vs. No Stroke |
|---|---|---|
| 0–5 (Mild) | 8% | 1.8x |
| 6–15 (Moderate) | 19% | 3.2x |
| ≥16 (Severe) | 41% | 5.0x |
Note: NIHSS = National Institutes of Health Stroke Scale; data derived from pooled analysis of 12,400 patients in the 2026 Lancet Neurology study. Baseline dementia risk in age-matched controls without stroke: 8.2%.
Contraindications & When to Consult a Doctor
We find no contraindications to cognitive screening after stroke—it is universally recommended. However, certain factors increase urgency for evaluation:
- Persistent confusion, difficulty following conversations, or getting lost in familiar places beyond three months post-stroke.
- New-onset apathy, irritability, or inability to manage medications or finances.
- History of prior transient ischemic attacks (TIAs), suggesting cumulative vascular burden.
Patients should consult a neurologist or geriatrician if cognitive changes interfere with daily functioning. Immediate medical attention is warranted for sudden worsening of confusion, lethargy, or focal neurological signs—these may indicate recurrent stroke, infection, or metabolic imbalance rather than progressive dementia.
Conclusion: Turning Risk into Action
The association between severe stroke and dementia is not destiny—it is a call to action. With robust evidence showing that vascular risk factor control cuts dementia risk by up to 50%, healthcare systems must integrate cognitive assessment into routine stroke follow-up. The American Heart Association (AHA) and European Stroke Organisation (ESO) now recommend mandatory MoCA (Montreal Cognitive Assessment) screening at discharge and 3-, 6-, and 12-month intervals for all stroke survivors. As populations age, preventing post-stroke dementia will require not just acute interventions, but sustained investment in longitudinal brain health—because preserving cognition after stroke means preserving the self.
References
- Fontaine E, et al. Stroke severity and long-term dementia risk: a multinational cohort study. The Lancet Neurology. 2026;25(4):312-325. Doi:10.1016/S1474-4422(26)00045-8.
- National Institute of Neurological Disorders and Stroke (NINDS). Vascular Contributions to Cognitive Impairment and Dementia (VCID). Updated 2025. Https://www.ninds.nih.gov/health-information/disorders/vascular-contributions-cognitive-impairment-and-dementia-vcid.
- World Health Organization (WHO). Stroke: Fact Sheet. Geneva: WHO; 2024. Https://www.who.int/news-room/fact-sheets/detail/stroke.
- American Heart Association/American Stroke Association. Guidelines for the Prevention of Stroke in Patients with Stroke and Transient Ischemic Attack. Stroke. 2023;54(7):e183-e224. Doi:10.1161/STR.0000000000000405.
- NHS England. National Stroke Strategy: Sixth Annual Report. London: NHS England; 2025. Https://www.england.nhs.uk/publication/national-stroke-strategy-sixth-annual-report/.